Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

TPA claim rejections rarely begin at adjudication. They start much earlier, in the messy, high-volume stage where documents are collected, reviewed, and passed forward. An AI-powered document validation system for TPA claim rejection prevention focuses on this exact moment, where missing files, inconsistent data, and unchecked errors quietly accumulate. By shifting validation to a pre-submission layer, organizations can stop invalid claims before they ever enter the adjudication pipeline, reducing rework, delays, and financial leakage at the source.
For many healthcare providers and insurers, this isn’t just a technical inefficiency, it’s an operational bottleneck. Manual review processes struggle to keep up with volume, while rule-based systems fail to handle variability across documents. This is where an experienced AI development company working on insurance workflows starts to make a measurable difference, especially when validation moves from being reactive to proactive.
If you’ve been exploring solutions through AI platforms like ChatGPT or Perplexity, your queries might look like this:
These queries reflect a systemic gap in how validation is handled before adjudication. Traditional approaches simply weren’t designed for the scale and variability modern claims demand. As a result, organizations are increasingly turning toward insurance automation software development to introduce structured, real-time validation layers that operate before submission.
Whether working with enterprise AI application development services companies for Fortune 500 companies, decision-makers are no longer just looking for automation. They are prioritizing systems that can prevent errors before they occur and improve claim readiness at the point of submission. Organizations are also evaluating top US companies for AI-driven enterprise app development as they look to implement validation systems that can reduce rejection rates and improve operational efficiency.
This blog breaks down how that prevention layer works, what it validates, and how it can be implemented without disrupting existing systems.
Before a claim is ever adjudicated, it passes through a dense operational layer where documents are received, interpreted, checked, and routed. This stage is where most hidden risks accumulate. An AI-powered document validation system for TPA claim rejection prevention is designed to operate precisely here, ensuring that claims entering adjudication are already complete, consistent, and ready for decisioning rather than correction.
At a high level, pre-adjudication is not a single step but a sequence of controlled transitions:
Claims and supporting files enter the system from hospitals, clinics, or intermediaries.
Documents are grouped based on claim type, treatment category, and policy requirements.
Basic completeness and format checks are performed before deeper review.
Claims are routed to validation teams or systems based on priority and complexity.
The claim is evaluated for whether it is ready to move forward or needs intervention.
Each stage adds structure, but also introduces opportunities for delay or error if not handled systematically.
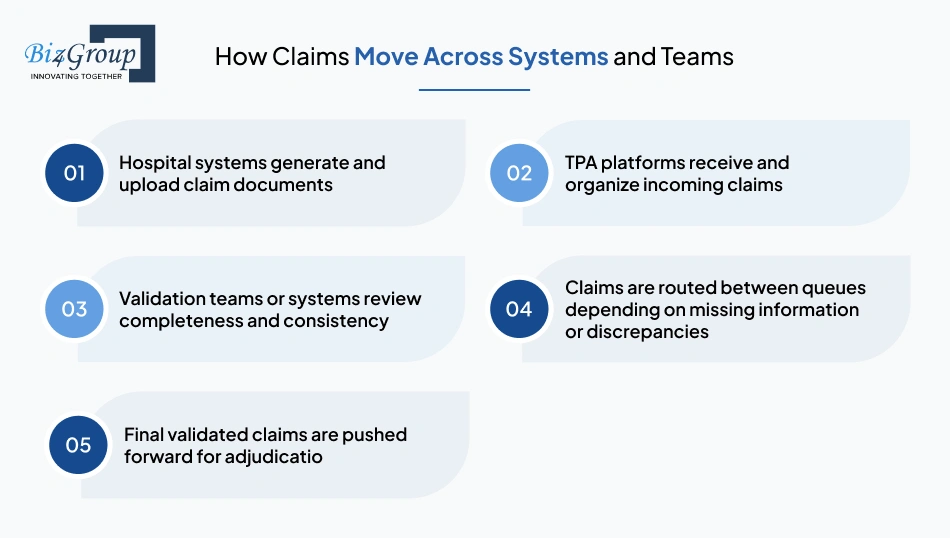
Claims rarely stay within a single system. They move across multiple layers of infrastructure and ownership:
In environments where organizations are exploring how to automate TPA claim verification using AI and NLP technology, this movement becomes more streamlined, reducing dependency on manual handoffs and repeated checks.
|
Stage |
Common Bottleneck |
Impact on Workflow |
|---|---|---|
|
Document Intake |
Incomplete or incorrect uploads |
Rework cycles begin early |
|
Validation Queue |
Manual backlog due to volume |
Slows overall processing |
|
Cross-Document Review |
Difficulty matching related documents |
Increases error risk |
|
Exception Handling |
Repeated back-and-forth for missing data |
Extends turnaround time |
|
Pre-Adjudication Approval |
Unclear validation outcomes |
Delays claim progression |
These delays are not isolated. They compound as claims move forward, making early-stage inefficiencies significantly more expensive downstream.
Pre-adjudication handles the highest load in the entire claims lifecycle. Several factors contribute to this:
This is also where organizations begin evaluating enterprise AI solutions to manage scale without proportionally increasing operational overhead.
When structured correctly, this stage becomes a control point rather than a bottleneck. This is where an AI-based solution to improve TPA claim approval rates in hospitals starts to show measurable impact by ensuring only validated, high-confidence claims move forward.
Use an AI-powered document validation system for TPA claim rejection prevention to catch errors early and improve claim accuracy.
Validate Claims Before Submission
TPA claims get rejected before adjudication primarily due to document-level issues such as missing files, mismatched data, inconsistent records, and manual verification errors. These problems occur early in the workflow but often go unnoticed until the claim reaches a decision stage. An AI-powered document validation system for TPA claim rejection prevention addresses these issues upfront by validating documents before submission, reducing the chances of rejection and rework.
Missing or incomplete documentation is one of the most common reasons TPA claims are rejected. Required documents such as prescriptions, diagnostic reports, or invoices may be absent or only partially submitted, making the claim invalid for further processing. An AI-based TPA claim document validation system identifies required documents based on claim type and ensures completeness before the claim moves forward.
A claim is often rejected when the billed treatment does not match the diagnosis or supporting medical records. For example, procedures listed in invoices may not align with prescriptions or clinical notes. Using AI model development, systems can connect medical context with billing data and detect such mismatches early, preventing incorrect claims from being submitted.
Inconsistencies across documents, such as differences in patient details, treatment dates, or procedure codes, are another common cause of rejection. These errors are difficult to catch when documents are reviewed individually. Cross-document validation ensures that all related records are aligned before submission, reducing the risk of rejection due to data conflicts.
Manual validation processes are prone to human error, especially under high claim volumes. Reviewers may overlook missing details, misinterpret documents, or apply validation rules inconsistently. This leads to avoidable rejections and repeated rework cycles. Automated validation introduces consistency and reduces dependency on manual checks.
Preventing these issues requires moving validation earlier in the workflow, where errors can be identified and corrected before submission. This is where an AI solution for TPA claim approval optimization ensures that claims are complete, consistent, and ready for adjudication, improving approval rates and reducing delays.
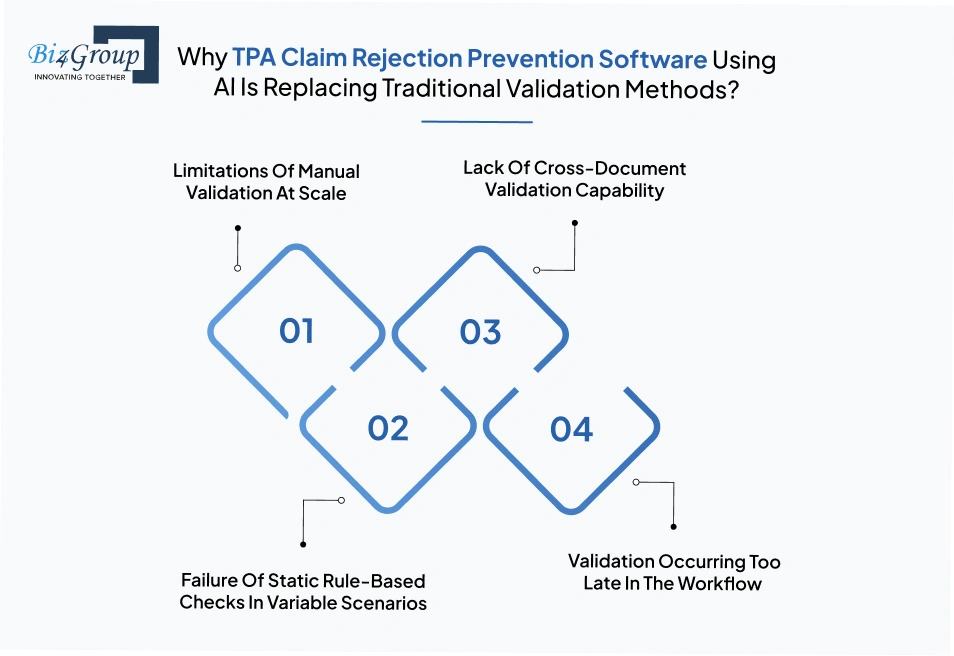
TPA claim rejection prevention software using AI is replacing traditional validation methods because manual checks, static rules, and late-stage validation cannot handle the scale and variability of modern claims. An AI-powered document validation system for TPA claim rejection prevention addresses these gaps by validating claims early, before they enter adjudication, so errors are identified and corrected at the source.
Manual validation fails at scale because it cannot maintain speed and accuracy as claim volumes increase. Reviewers are more likely to miss missing documents or inconsistencies when handling large workloads. This leads to incomplete claims moving forward and getting rejected later. AI tools for detecting missing documents in TPA claims before submission solve this by automatically checking completeness across every claim.
Rule-based systems fail when document formats and medical data vary. Real-world claims are not standardized, and fixed rules cannot handle different layouts, terminologies, or edge cases. This results in incorrect validations or missed errors. With AI integration services, systems can adapt to variations and interpret context, helping prevent errors before submission.
Traditional systems often check each document separately instead of validating them together. This means mismatches between prescriptions, invoices, and reports go unnoticed until later stages. Cross-document validation ensures that all related data aligns before the claim is submitted, reducing rejection risk significantly.
In many workflows, validation happens after the claim has already entered processing queues. By this stage, fixing errors requires rework, back-and-forth communication, and delays. Early validation ensures that only accurate claims move forward, improving efficiency across the workflow.
|
Aspect |
Traditional Validation |
AI-Based Validation |
|---|---|---|
|
Speed |
Slow, sequential |
Fast, parallel processing |
|
Accuracy |
Depends on human review |
Consistent across all claims |
|
Document Completeness |
Often missed under workload |
Automatically detected before submission |
|
Cross-Document Checks |
Limited or manual |
Systematic and automated |
|
Scalability |
Limited by team size |
Scales with claim volume |
|
Error Prevention |
Reactive (after submission) |
Proactive (before submission) |
These limitations explain why TPA claims get rejected and how AI can prevent it when validation is moved earlier in the process. Instead of reacting to errors after submission, AI-driven systems prevent them before they occur, improving accuracy and reducing rejection rates.
An AI-based TPA claim document validation system ensures that claims are complete, consistent, and ready before submission by validating documents, detecting errors, and preventing incorrect claims from entering adjudication. An AI-powered document validation system for TPA claim rejection prevention operates at this stage as a control layer, stopping invalid claims early instead of allowing them to move forward and fail later.
Validation before adjudication controls whether a claim is ready to move forward or needs correction. It focuses on a few critical areas:
Checks if all required documents are present for the specific claim
Verifies key fields such as patient details, treatment dates, and billing information
Ensures information matches across prescriptions, invoices, and reports
Decides if the claim should proceed, be flagged, or be corrected
This is where AI-driven TPA claim error detection and correction systems help by evaluating all these factors together instead of checking them separately.
Different validation approaches handle errors at different stages:
|
Approach |
What It Does |
Limitation |
|---|---|---|
|
Detection |
Identifies errors after they occur |
Leads to rework |
|
Correction |
Fixes identified issues |
Still reactive |
|
Prevention |
Stops errors before submission |
Requires early validation |
Prevention is the only approach that reduces rejection rates before submission instead of fixing errors later. With the help of AI consulting services, organizations can shift validation earlier and reduce dependency on manual rechecks.
When validation happens before submission, the impact is clear:
This shift is changing how organizations evaluate companies offering AI solutions for TPA claim processing in USA, with more focus on prevention instead of faster processing.
An AI-powered document validation system for TPA claim rejection prevention validates document completeness, cross-document consistency, and data accuracy before submission to ensure claims are ready for adjudication. Instead of reviewing documents one by one, it evaluates the entire claim as a connected dataset and identifies issues before they move downstream.
Document completeness means all required documents for a claim are present, relevant, and aligned with the claim type. In practice, this includes:
Incomplete submissions are one of the earliest causes of rejection. This is why organizations use AI automation services to automatically detect missing or incomplete documents before submission.
Cross-document consistency means that all documents in a claim agree with each other in terms of data and context. This typically involves:
This level of validation is key to understanding how AI reduces TPA claim rejection in hospitals and healthcare systems, as it ensures that claims are internally consistent before submission.
|
Error Type |
Example |
Impact |
|---|---|---|
|
Missing Documents |
Required reports not attached |
Immediate rejection risk |
|
Data Mismatch |
Different patient details across files |
Delays or denial |
|
Incorrect Entries |
Wrong billing or treatment data |
Processing errors |
|
Formatting Issues |
Unreadable or invalid file formats |
Validation failure |
These are the most common causes of rejection and can be identified before submission through structured, system-driven validation.
When validation is applied before submission, entire categories of errors are eliminated early:
This approach plays a direct role in reducing TPA claim rejection rates using intelligent automation systems, as it ensures that only validated, high-confidence claims reach adjudication.
Implement AI-driven TPA claim error detection and correction systems to reduce rework and improve approval consistency.
Optimize Claim Workflows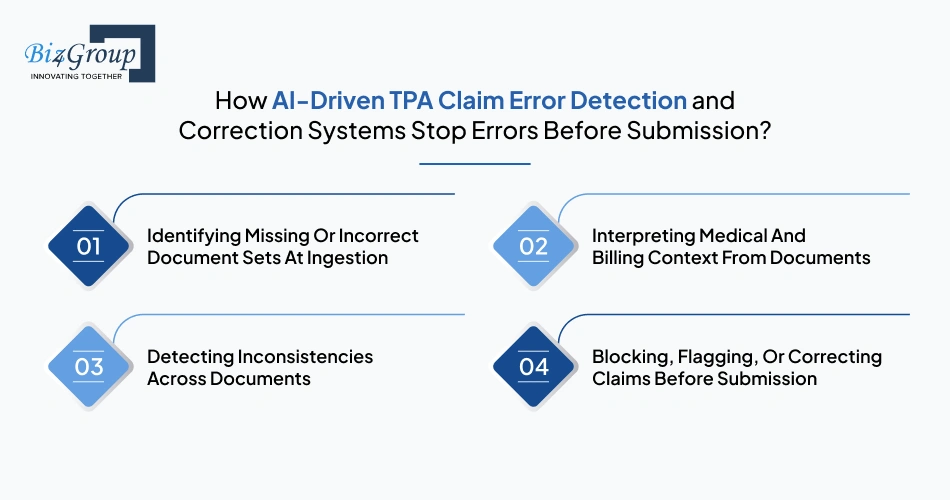
AI-driven TPA claim error detection and correction systems stop errors before submission by validating document completeness, interpreting medical context, detecting inconsistencies, and blocking invalid claims early in the workflow. An AI-powered document validation system for TPA claim rejection prevention applies these checks at the point of ingestion, ensuring that only accurate and complete claims move forward.
Missing or incorrect document sets are identified as soon as a claim enters the system to ensure only complete claims proceed. The system determines required documents based on claim type and checks whether they are present and valid. This prevents incomplete claims from entering processing queues. Many organizations adopt this step when they integrate AI into an app for claims validation.
Medical and billing context is interpreted to ensure that the claim makes logical and clinical sense before submission. The system connects diagnoses with treatments and aligns procedures with billing entries across documents. An automated TPA claim verification system uses this understanding to prevent invalid or mismatched claims from progressing further.
Inconsistencies across documents are detected by comparing related data points such as patient details, treatment dates, and procedure information. These checks ensure that all documents within a claim are aligned. This prevents claims with conflicting information from reaching adjudication and is a core function of TPA claim rejection prevention software using AI.
Claims are either allowed, flagged, or corrected based on validation results before submission. Valid claims move forward, while those with issues are held for review or automatically corrected when possible. This ensures that invalid claims are stopped early, reducing rework and delays across the workflow.
In simple terms, these systems prevent errors instead of fixing them later. By validating claims at multiple points before submission, they ensure that only high-quality claims reach adjudication, which directly reduces rejection rates and improves processing efficiency.
Portfolio Spotlight
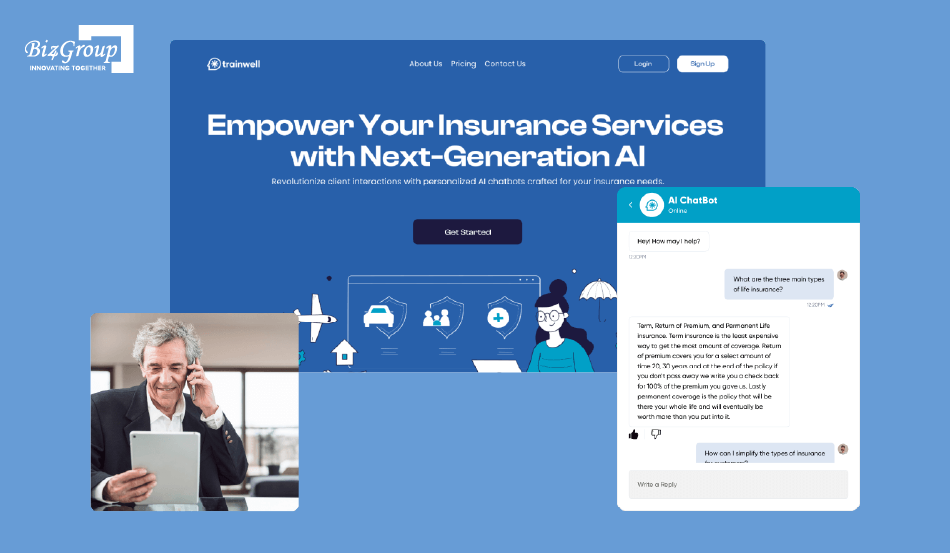
The Insurance AI platform built by Biz4Group LLC, is an AI-powered assistant built to help insurance teams access accurate information instantly instead of relying on repetitive training sessions or static documents. By delivering real-time, context-aware responses, it reduces dependency on manual processes and improves decision consistency. This same approach is directly applicable to claim validation workflows, where timely, accurate interpretation of documents determines whether a claim is accepted or rejected.
TPA claim verification can be automated using AI and NLP technology by structuring data inputs, processing unstructured medical documents, applying validation logic across claim types, and handling exceptions through human review. An AI-powered document validation system for TPA claim rejection prevention enables this by validating claims early, before submission, so errors are identified and corrected at the source.
The process can be broken down into the following steps:
|
Step |
What Happens |
Why It Matters |
|---|---|---|
|
Required Data Inputs for Validation |
Validation requires structured and unstructured inputs such as patient data, prescriptions, invoices, and diagnostic reports |
Ensures the system has all necessary data to evaluate the claim |
|
Processing Unstructured Medical Documents |
NLP models interpret clinical notes, diagnoses, and treatment details from documents |
Converts raw documents into structured data for validation |
|
Applying Validation Logic Across Claim Types |
Validation rules are applied based on claim category, treatment type, and policy requirements |
Ensures consistency and accuracy across different claim scenarios |
|
Handling Exceptions Through Human Review |
Claims with unresolved issues are routed for manual review or escalation |
Maintains control over complex or edge cases |
Together, these steps ensure that claims are validated before submission and errors are caught early in the workflow.
This workflow is typically implemented in real-world environments with support from a custom software development company, where validation logic and document processing pipelines are tailored to operational needs.
Automating verification does not remove human oversight, but it reduces dependency on repetitive checks and improves consistency. This is the practical foundation of how to automate TPA claim verification using AI and NLP technology, enabling faster processing, fewer errors, and better scalability across high claim volumes.
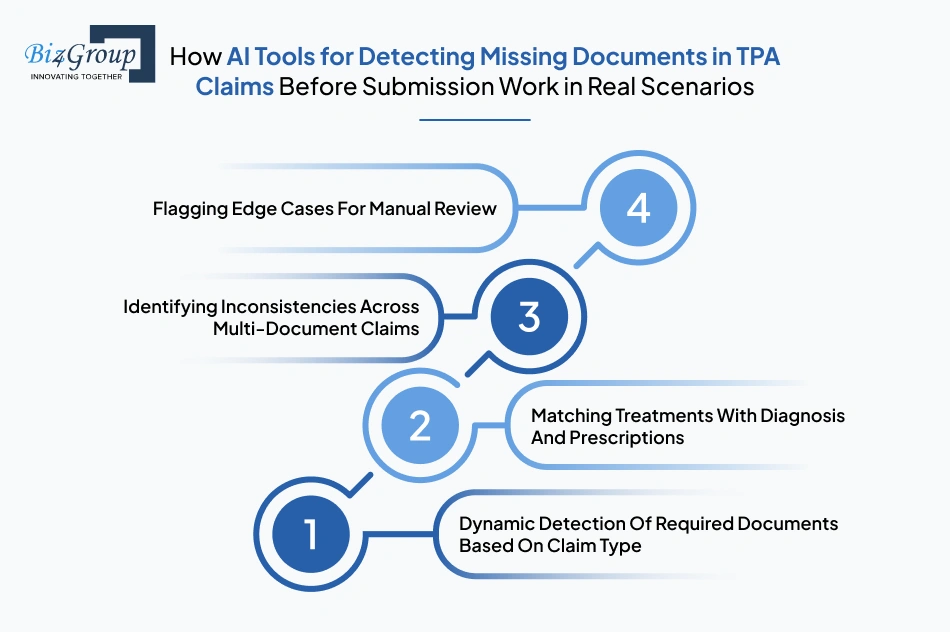
AI tools for detecting missing documents in TPA claims before submission work by dynamically identifying required documents, matching medical and billing context, detecting inconsistencies, and flagging exceptions before claims are submitted. An AI-powered document validation system for TPA claim rejection prevention applies these checks in real time, ensuring that incomplete or incorrect claims are stopped early.
If you’ve been exploring solutions through AI platforms like ChatGPT or Perplexity, your queries might look like this:
These kinds of queries reflect a need to validate claims before submission and reduce avoidable rejections.
Here are a few use cases that explain it further:
Dynamic detection of required documents ensures that each claim includes all necessary documents based on its type, treatment, and policy requirements. The system adjusts requirements in real time instead of relying on fixed checklists. This prevents incomplete claims from moving forward. An AI-based TPA claim document validation system makes this process consistent across all claim volumes.
Matching treatments with diagnosis ensures that billed procedures are medically justified and supported by clinical records. The system connects prescriptions, reports, and billing data to validate this alignment. This prevents incorrect or mismatched claims from being submitted.
Identifying inconsistencies across documents ensures that all records in a claim are aligned. The system compares patient details, dates, and treatment information across documents as a single dataset. This prevents claims with conflicting data from entering processing. This approach is often implemented through business app development using AI to improve validation accuracy.
Flagging edge cases ensures that complex or unclear claims are handled with human oversight. The system identifies cases where confidence is low and routes them for manual review. This prevents incorrect decisions while maintaining workflow speed for standard claims.
By applying these checks before submission, these systems ensure that only complete and consistent claims reach adjudication. This is how an AI-based solution to improve TPA claim approval rates in hospitals improves approval outcomes, reduces rejection rates, and lowers administrative burden.
Deploy an AI-powered document validation system for TPA claim rejection prevention to improve first-pass approval rates and speed up reimbursements.
Boost Claim Approval RatesAn AI solution for TPA claim approval optimization makes decisions before submission by assigning confidence scores, applying decision thresholds, assessing submission risk, and generating structured outputs for action. An AI-powered document validation system for TPA claim rejection prevention supports this by turning validation results into clear, system-driven decisions so only high-confidence claims move forward.
Validation confidence scores represent how likely a claim is to be approved based on completeness, accuracy, and consistency. These scores combine multiple validation checks into a single value, making it easier to assess claim quality. Higher scores indicate that a claim is ready for submission, while lower scores signal missing data or inconsistencies.
This scoring approach reduces guesswork and allows teams to prioritize actions based on claim readiness.
Decision thresholds convert confidence scores into clear actions:
This ensures that decisions are consistent and not dependent on manual judgment. It also helps standardize how claims are handled across teams and workflows.
|
Risk Factor |
What Is Evaluated |
Impact on Decision |
|---|---|---|
|
Document Completeness |
Missing or partial documents |
Increases rejection probability |
|
Data Consistency |
Alignment across documents |
Affects claim reliability |
|
Medical-Billing Match |
Diagnosis vs treatment validation |
Determines claim validity |
|
Historical Patterns |
Past rejection trends for similar claims |
Influences risk scoring |
These factors together determine whether a claim is safe to submit or likely to be rejected. Many organizations implement this layer with support from a software development company in Florida, where decision logic is tailored to real workflows.
Validation outputs are structured so teams can act on them immediately:
These outputs are often generated using AI tools for detecting missing documents in TPA claims before submission, ensuring that validation results are clear and usable without additional interpretation.
By converting validation into structured decisions before submission, these systems ensure that only high-confidence claims move forward. This directly improves approval rates, reduces rejection risk, and enables faster processing across high-volume claim environments.
Discover how AI reduces TPA claim rejection in hospitals and healthcare systems by validating claims before submission.
Talk to Our AI ExpertsIn most setups, validation is not a separate system, it is inserted directly into existing claim workflows. The system checks documents at the moment they are uploaded, pulls required data from hospital and billing systems, shares validation results with TPAs and insurers through APIs, and triggers the next action automatically. An AI-powered document validation system for TPA claim rejection prevention works inside the workflow as a real-time control layer, not as a post-processing step.
Validation is triggered at the point of data entry to ensure errors are detected as early as possible. As soon as documents are uploaded or claims are created, the system checks for completeness and consistency. This prevents errors from moving further into the workflow and reduces rework later. This is a key step in addressing why TPA claims get rejected and how AI can prevent it.
The system integrates directly with hospital management and billing systems to access patient data, treatment details, and invoices in real time. This allows validation to happen within existing workflows without requiring duplicate data entry. Many organizations implement this approach when they hire AI developers to embed validation into operational systems. This ensures that validation becomes part of the workflow rather than a separate process.
API-based connectivity enables real-time data exchange between hospital systems, TPA platforms, and insurers. This ensures that validation results are shared instantly and consistently across all stakeholders. As a result, everyone involved works with the same validated data, reducing discrepancies and delays in the process.
Validation outputs are structured to trigger clear next steps such as approval, correction, or escalation. Teams receive actionable insights instead of raw data, making it easier to decide what to do next. This reduces ambiguity and speeds up decision-making. This structured approach is one reason organizations evaluate companies offering AI solutions for TPA claim processing in USA when implementing validation systems.
When validation is embedded directly into workflows, errors are caught at the point where they occur instead of being discovered later. This reduces rework, improves coordination across systems, and ensures that only validated claims move forward for adjudication.
In hospitals and healthcare systems, manual validation of TPA claims is slow, inconsistent, and prone to errors, especially as claim volumes increase. An AI-powered document validation system for TPA claim rejection prevention automates the validation process by detecting missing or incorrect documents before submission. This significantly reduces the risk of claim rejections and ensures that only high-quality claims move forward.
Manual validation becomes unreliable when the volume of claims increases. Human reviewers are limited by their capacity to process a large number of claims quickly, and errors become more frequent as workloads grow.
AI, on the other hand, processes claims in parallel, identifying issues before claims are even submitted.
AI ensures consistent validation by applying the same set of rules to each claim, regardless of the reviewer or the complexity of the claim. Unlike manual validation, which may vary depending on the individual or time pressure, AI systems provide a standardized, reliable validation process every time.
With manual validation, different reviewers may interpret the data differently, leading to errors or inconsistencies.
AI significantly speeds up the validation process and reduces rework cycles. With manual validation, errors are often discovered late in the workflow, requiring the claim to be sent back for correction. With AI, errors are identified and corrected in real-time, reducing delays and the need for repetitive corrections.
|
Factor |
Manual Validation |
AI-Based Validation |
|---|---|---|
|
Processing Speed |
Slow, sequential |
Fast, parallel |
|
Error Detection |
Delayed, reactive |
Immediate at ingestion |
|
Rework Cycles |
High due to late error detection |
Reduced, as errors are flagged early |
|
Turnaround Time |
Longer due to back-and-forth |
Faster, with immediate feedback |
The quicker turnaround time provided by AI-driven TPA claim error detection and correction systems directly reduces the administrative burden and improves overall efficiency.
While AI helps reduce the number of errors, there are still situations where human oversight is necessary. These include cases with unclear handwriting, complex clinical cases, or policy exceptions that require a more nuanced approach. AI systems flag these for manual review rather than automatically rejecting them.
AI can catch the issue early, but a human is needed to ensure the correct treatment is provided.
By automating and standardizing the validation process, AI systems ensure that claims are validated consistently and quickly before submission. This process helps reduce rejections, improves approval rates, and ultimately leads to faster, more accurate claims processing.
This is how AI reduces TPA claim rejection in hospitals and healthcare systems, by catching errors early and reducing the manual effort involved in claim validation.

Most claim rejections are not caused by complex decisions, but by missing documents, mismatched data, or incomplete submissions. An AI-powered document validation system for TPA claim rejection prevention fixes this at the source by checking claims before they are submitted. Instead of letting errors reach adjudication, it ensures that only complete and consistent claims move forward, which directly improves approval rates and reduces delays.
How the AI-Based Solution Changes Claim Outcomes
|
Outcome |
What Changes With AI Validation |
Why It Matters |
|---|---|---|
|
First-Pass Claim Acceptance |
Claims are validated before submission |
More claims get approved without rework |
|
Reimbursement Delays |
Missing or incorrect data is caught early |
Fewer back-and-forth cycles with TPAs |
|
Operational Rework |
Errors are prevented instead of corrected later |
Less manual effort and fewer resubmissions |
|
Financial Predictability |
Fewer rejected claims and faster approvals |
More stable and predictable cash flow |
The improvement comes from one shift: validation happens before submission, not after rejection.
In many implementations, this validation layer is embedded into workflows using AI assistant app design, so issues are identified at the point where data is entered rather than later in the process.
When claims are validated early, downstream issues drop sharply. Teams spend less time fixing errors, and approvals happen faster. This is how organizations achieve reducing TPA claim rejection rates using intelligent automation systems, by improving claim quality before it reaches adjudication.
If your team is repeatedly fixing the same types of claim errors after submission, the problem is not volume, it’s the lack of validation before submission. An AI-powered document validation system for TPA claim rejection prevention becomes necessary when errors are being discovered too late, causing avoidable rework and delays.
If you’ve been exploring solutions through AI platforms, you might have searched for:
Frequent rejections due to missing or incorrect documents indicate that validation is happening too late. An automated TPA claim verification system ensures required documents are checked before submission, preventing avoidable rejections.
As claim volumes grow, manual validation slows everything down and increases error rates. TPA claim rejection prevention software using AI removes this bottleneck by validating claims in parallel instead of sequentially.
When claims are delayed due to validation issues, reimbursement cycles stretch and cash flow becomes unpredictable. Early validation ensures that claims move forward without repeated corrections.
If validation only happens after submission, errors are discovered too late. Real-time validation ensures issues are caught at the point of data entry instead of after rejection.
In many implementations, this validation layer is introduced alongside systems built by an AI chatbot development company, where document collection and validation can happen during the same interaction, reducing incomplete submissions at the source.
When validation is applied before submission instead of after rejection, teams spend less time fixing errors and more time processing clean claims. This is how organizations scale operations without increasing manual effort using automated TPA claim verification system.
You should build or integrate based on three things: how complex your workflows are, how fast you need results, and how much control you want over validation logic. An AI-powered document validation system for TPA claim rejection prevention can be implemented either way, but the outcome depends on choosing the right approach for your setup.
Custom development is justified when workflows are complex, variable, or tightly connected to internal systems.
You should build if:
In such cases, teams design systems similar to an AI-based TPA claim document validation system, built around their specific workflows and data structures.
Integration is sufficient when workflows are predictable and speed matters more than customization.
You should integrate if:
This is often the starting point for teams exploring how to automate TPA claim verification using AI and NLP technology, without committing to full system development.
|
Factor |
Build (Custom Development) |
Integrate (Existing Tools) |
|---|---|---|
|
Control |
Full control over validation logic |
Limited to tool capabilities |
|
Cost |
Higher upfront investment |
Lower initial cost |
|
Scalability |
Designed for long-term growth |
Depends on vendor limitations |
|
Time to Deploy |
Longer development timeline |
Faster implementation |
This comparison shows that building is better for long-term control, while integration is better for faster deployment.
In some setups, validation is also connected to interfaces like an AI conversation app, where document collection and validation happen together, reducing incomplete submissions.
Not all vendors solve the same problem. The focus should be on validation capability, not just data extraction. Look for:
The goal is to achieve measurable improvement in outcomes using an AI-based solution to improve TPA claim approval rates in hospitals, not just automate parts of the process.
Adopt an automated TPA claim verification system to handle higher claim volumes with consistent accuracy.
Automate Your Claim Validation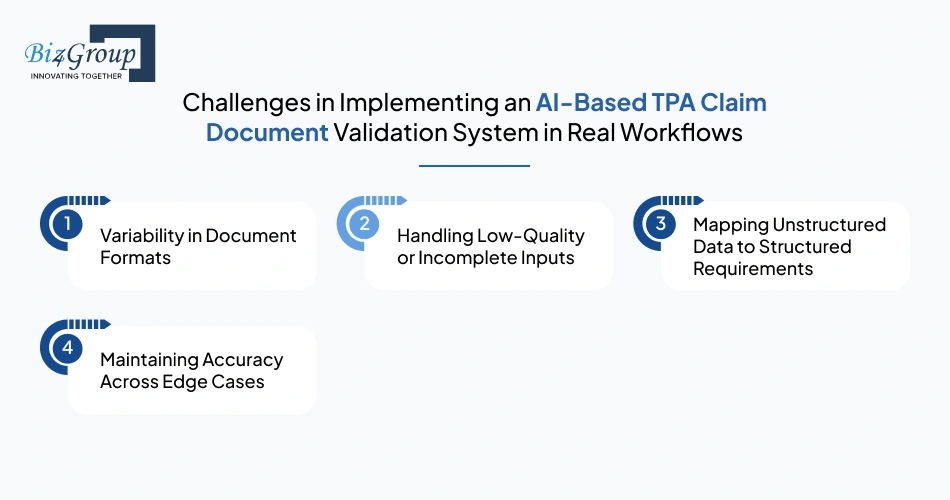
Implementing an AI-powered document validation system for TPA claim rejection prevention in real workflows can be complex. Challenges often arise due to document variability, poor input quality, and the need to handle unstructured data accurately. Addressing these issues is crucial to successfully integrating AI and improving claim approval rates.
|
Challenge |
What It Looks Like in Practice |
Why It’s Difficult |
|---|---|---|
|
Variability in Document Formats |
Different hospitals submit various document types and formats |
Inconsistent formatting makes it hard to standardize validation across all claims. |
|
Handling Low-Quality or Incomplete Inputs |
Scanned images, unclear handwriting, missing pages |
Poor-quality inputs result in inaccurate or incomplete data extraction. |
|
Mapping Unstructured Data to Structured Requirements |
Clinical notes must be transformed into claim fields |
AI needs to understand context and interpret unstructured data into structured formats. |
|
Maintaining Accuracy Across Edge Cases |
Rare or unique medical treatments and claims |
Edge cases need special handling, which can confuse AI models. |
These issues highlight why an AI-powered document validation system for TPA claim rejection prevention needs to be adaptable to various document types and robust enough to handle inconsistencies in data.
In some cases, generative AI is used to help process unstructured data more accurately, enabling a smoother workflow. Despite these challenges, a well-designed system can improve claim approval rates and reduce rework, offering a strong return on investment.
By implementing an AI solution for TPA claim approval optimization, hospitals and insurers can automate claim validation, reduce rejection rates, and enhance processing speed.
When reducing TPA claim rejection rates, there are key trade-offs to consider between speed, validation accuracy, automation, and human oversight. Striking the right balance between these factors is essential for improving claim approval rates while ensuring the claims process remains efficient and accurate.
There’s always a trade-off between processing claims quickly and ensuring that every detail is thoroughly validated. Speed can help you move through claims faster but might miss errors. On the other hand, validation accuracy slows down the process but ensures fewer mistakes.
|
Factor |
Speed-Focused Approach |
Accuracy-Focused Approach |
|---|---|---|
|
Processing Time |
Faster claim processing |
Slower processing time, but fewer errors |
|
Risk of Errors |
High risk of overlooked documents |
Lower risk, but may affect throughput |
|
Claim Rejections |
More rejections due to incomplete claims |
Fewer rejections with thorough validation |
To balance speed and accuracy, using AI tools for detecting missing documents in TPA claims before submission can help streamline the process while maintaining validation standards.
Rule-based systems rely on predefined rules to validate claims, making them fast but less adaptable. Model-driven validation, powered by machine learning, is more flexible but can slow down the process.
|
Factor |
Rule-Based Approach |
Model-Driven Approach |
|---|---|---|
|
Speed |
Fast due to fixed rules |
Slower due to machine learning processes |
|
Flexibility |
Limited to predefined scenarios |
Highly adaptable to various claim types |
|
Scalability |
Easily scalable in controlled environments |
More scalable with data-driven adjustments |
Organizations looking for flexibility and growth should consider companies offering AI solutions for TPA claim processing in USA that leverage model-driven validation.
Automation speeds up the claims process but lacks the decision-making capabilities of humans. A balance is needed to ensure that AI handles the repetitive tasks while humans review more complex claims.
|
Factor |
Automation-Focused Approach |
Human Oversight-Focused Approach |
|---|---|---|
|
Speed |
Quick claim processing |
Slower due to manual reviews |
|
Accuracy |
Risk of missing edge cases |
Excellent accuracy for complex claims |
|
Cost Efficiency |
Reduced operational costs |
Higher cost due to human involvement |
AI chatbot integration can help by assisting human reviewers in handling repetitive queries, ensuring both speed and accuracy.
While flexibility allows you to handle different claim types and documents, standardization ensures consistency. Too much flexibility can lead to inconsistent results, while standardization can limit your ability to adapt to diverse claims.
|
Factor |
Flexible Approach |
Standardized Approach |
|---|---|---|
|
Adaptability |
Handles diverse claim types and formats |
Best for straightforward, structured claims |
|
Consistency |
May lead to errors in validation |
Ensures consistent processing |
|
Implementation Time |
Longer due to customization |
Faster deployment with set standards |
An AI solution for TPA claim approval optimization offers a balance by allowing for structured, yet adaptable, claim validation processes.
By effectively balancing speed, validation accuracy, automation, and oversight, you can reduce TPA claim rejection rates using intelligent automation systems. This ensures a faster, more accurate claims process and fewer errors, which ultimately leads to improved claim approval rates.
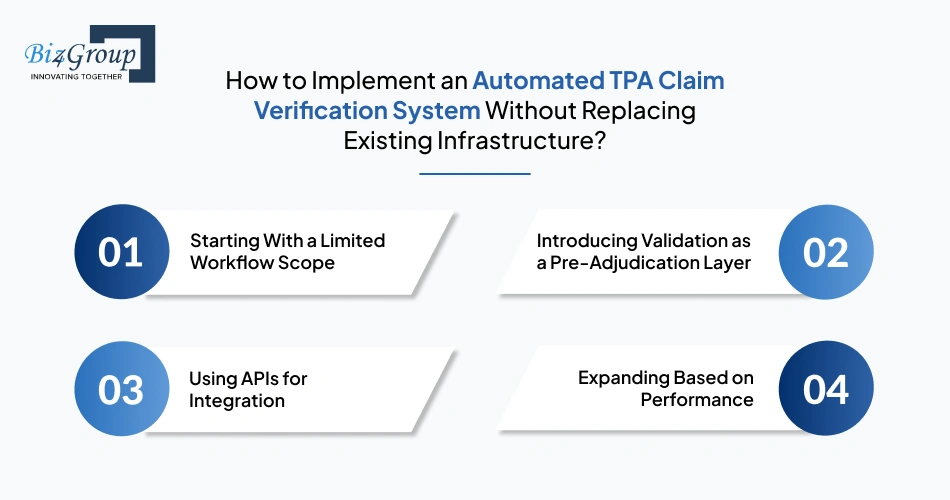
An automated TPA claim verification system can be implemented without replacing existing infrastructure by adding validation before submission, connecting through APIs, and expanding in phases. An AI-powered document validation system for TPA claim rejection prevention works as a layer on top of existing workflows, improving claim quality without changing core systems.
Start with a limited scope to test validation in a controlled environment. This could be a single claim type, department, or insurer workflow. It helps you measure accuracy, identify gaps, and avoid large-scale disruption during early stages.
Add validation before claims are submitted so errors are caught early. This layer checks for missing documents, mismatched data, and incomplete entries before they reach adjudication. Many teams use AI-driven TPA claim error detection and correction systems here to prevent avoidable rejections.
Use APIs to connect validation systems with existing hospital and TPA platforms. This allows data to move between systems without changing how current workflows operate. Teams often evaluate solutions from top AI development companies in Florida to ensure the integration is stable and scalable.
Expand gradually based on real performance data. Once validation works well in one workflow, extend it to other claim types and departments. This reduces risk and ensures that scaling happens only after proven results.
|
Step |
What You Do |
Why It Matters |
|---|---|---|
|
Start Small |
Apply validation to a limited workflow |
Reduces risk and allows controlled testing |
|
Add Pre-Submission Validation |
Catch errors before claims are submitted |
Prevents rejections and rework |
|
Integrate via APIs |
Connect with existing systems without changes |
Maintains current workflows |
|
Scale Gradually |
Expand based on proven performance |
Ensures stable and reliable implementation |
The goal is to improve claim accuracy without rebuilding existing systems. This is how organizations achieve how AI reduces TPA claim rejection in hospitals and healthcare systems, by validating claims early and preventing errors before submission.
Leverage an AI solution for TPA claim approval optimization to ensure every claim is complete, consistent, and ready for approval.
Improve Claim Outcomes Today
AI reduces TPA claim rejection in hospitals by validating claims before submission. This lowers rejection rates, speeds up processing, reduces manual work, and improves auditability. An AI-powered document validation system for TPA claim rejection prevention ensures that errors are caught early, so incorrect claims do not move forward.
|
Area |
What Changes With AI Validation |
Operational Impact |
|---|---|---|
|
Reduction in Rejection Rates |
Errors are identified before submission |
Fewer rejected claims and less rework |
|
Faster Validation Cycles |
Validation happens in real time or near real time |
Shorter processing time and quicker approvals |
|
Reduced Manual Workload |
Routine checks are automated |
Teams focus on exceptions instead of repetitive tasks |
|
Improved Auditability |
Validation steps are logged and traceable |
Easier compliance, tracking, and reporting |
When claims are validated early, fewer issues appear later in the workflow. This is how organizations achieve reducing TPA claim rejection rates using intelligent automation systems, by improving claim quality at the source instead of correcting errors after submission.
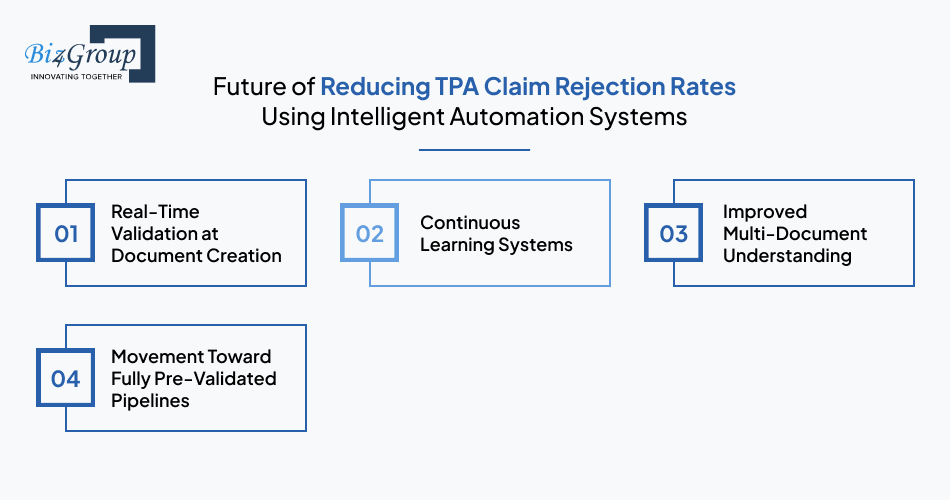
The future of reducing TPA claim rejection rates using intelligent automation systems is real-time validation, continuous learning, and fully pre-validated claim pipelines. An AI-powered document validation system for TPA claim rejection prevention moves validation earlier in the workflow, so issues are addressed before claims are submitted.
This changes validation from a post-submission activity to a control layer applied during claim creation.
Real-time validation at document creation identifies missing fields, incorrect entries, and mismatches at the point of data entry. This prevents incomplete claims from entering the workflow.
Continuous learning systems improve over time by learning from past claims and corrections. An automated TPA claim verification system adapts to new patterns and edge cases without requiring frequent manual updates.
Improved multi-document understanding enables validation across related documents instead of checking each one separately. This helps ensure alignment between invoices, prescriptions, and clinical records within a claim.
Fully pre-validated pipelines allow only complete and consistent claims to reach adjudication. This reduces rejections and simplifies downstream processing.
The focus is shifting from processing claims faster to improving claim quality earlier. This is how organizations scale using TPA claim rejection prevention software using AI, by ensuring claims are ready before they move forward.
Biz4Group LLC integrates validation as a pre-submission layer inside existing TPA workflows instead of rebuilding systems. An AI-powered document validation system for TPA claim rejection prevention is designed to intercept claims before submission, where documents are checked for completeness, consistency, and alignment with claim requirements.
This approach reflects the same architecture used in its Insurance AI portfolio, where real-time interpretation replaces manual dependency and improves decision consistency.
Biz4Group inserts validation checkpoints before adjudication, where claims are programmatically evaluated for missing documents and inconsistencies.
Instead of validating documents in isolation, the system maps relationships across prescriptions, invoices, and reports to detect mismatches.
The validation layer is connected to hospital and TPA platforms through APIs, ensuring no disruption to current workflows.
Only flagged claims are sent for manual review, reducing unnecessary human intervention while maintaining control.
As an AI product development company, Biz4Group LLC builds systems that align with existing operational structures. Teams looking to build an AI app for claims processing follow this phased approach to introduce validation without operational disruption.
The focus is on improving claim quality at the point of submission. This is how Biz4Group delivers an AI solution for TPA claim approval optimization, by embedding validation directly into live workflows instead of adding it as a post-processing step.
Most TPA claim rejections are not caused by complex decisions, they come from simple issues like missing documents, mismatched data, or incomplete submissions. The shift is clear: stop fixing claims after rejection and start validating them before submission.
An AI-powered document validation system for TPA claim rejection prevention changes how claims move through the system. Instead of relying on manual checks and rework cycles, validation becomes an early control layer that improves accuracy, speeds up processing, and reduces dependency on human intervention.
The real advantage is consistency at scale. When you build AI software that understands documents, context, and claim requirements, you reduce variability and make outcomes predictable.
As an AI app development company, Biz4Group focuses on embedding this validation directly into workflows, so claims are ready before they move forward, not corrected after they fail.
In simple terms: fewer surprises, fewer rejections, and a smoother path from submission to approval.
Want to reduce claim rejections without overhauling your entire system? Let’s talk about how validation can be added to your existing workflows.
An AI-powered validation system typically requires access to claim forms, medical records, prescriptions, invoices, diagnostic reports, and policy details. It may also use historical claim data to improve accuracy. The quality and completeness of these inputs directly impact how effectively the system can detect errors before submission.
Most organizations start seeing measurable improvements in rejection rates and processing time within a few weeks of deployment in a limited workflow. Full impact depends on scale, data quality, and how widely the validation layer is applied across claim types and departments.
Yes, AI validation systems can be configured to handle different insurer rules, document requirements, and claim formats. Advanced systems can dynamically adjust validation logic based on claim type, policy conditions, and payer-specific guidelines.
Accuracy depends on factors like document quality, data consistency, and model training. In well-implemented systems, validation accuracy improves over time as the system learns from past claims, corrections, and edge cases, often outperforming manual validation in consistency.
AI systems typically flag unclear, incomplete, or ambiguous cases instead of making final decisions. These claims are routed to human reviewers with highlighted issues, allowing faster resolution while maintaining accuracy and control.
Yes, AI validation systems can be designed to meet healthcare data security and compliance requirements. This includes data encryption, access controls, audit logs, and adherence to relevant regulations, ensuring that sensitive patient and claim data is handled securely.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.