Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

AI in healthcare is everywhere right now - in headlines, vendor pitches, and product demos. But for most healthcare providers and decision-makers, the real questions are much more practical:
Most content doesn’t answer these questions clearly. It either stays too high-level or dives too deep into technical detail without addressing real-world decisions.
This guide takes a different approach.
This is a comprehensive AI in healthcare FAQ, built as a structured collection of AI in healthcare questions and answers based on how people actually search, ask, and evaluate solutions today.
From healthcare AI basics questions and answers to advanced implementation and vendor selection, this guide brings together:
Everything is designed to help you move from understanding to decision-making without jumping between multiple resources.
This guide functions as both a beginner guide to AI in healthcare with questions and answers and a detailed FAQ on artificial intelligence in the healthcare industry.
You’ll find answers to:
If you’ve been searching for AI in healthcare explained with real-world questions or looking for medical AI questions explained simply, this guide is designed to give you clear, connected answers.
This guide is built for:
Whether you’re just starting or actively evaluating solutions, this resource acts as a central hub of healthcare AI explained questions and answers tailored to real-world needs.
You don’t need to read everything in order.
Each section is structured as a set of AI healthcare guide questions, so you can quickly find what matters most to you.
There’s no shortage of content on artificial intelligence in healthcare. What’s missing is clarity. This guide brings together:
All in one place - explained clearly, without hype, and focused on real-world application.
Let’s start with the fundamentals.
AI in healthcare sounds straightforward on the surface, but most people searching for it are not looking for definitions alone. They are trying to understand what it actually means in practice, how it differs from traditional systems, and whether it’s something they should take seriously right now.
This section answers those foundational questions.
If you’ve been looking for healthcare AI basics questions and answers, or trying to make sense of AI healthcare concepts explained simply, this is where you start. These are the kinds of medical AI questions explained clearly that help you build a solid understanding before moving into real-world use cases and implementation.
AI in healthcare refers to the use of technologies such as machine learning, natural language processing, and computer vision to analyze medical data, assist in diagnosis, automate workflows, and improve patient outcomes.
Unlike traditional systems that follow fixed rules, these technologies learn from data and improve over time. This allows them to detect patterns in patient histories, interpret imaging data, and extract insights from clinical documentation with increasing accuracy.
In practice, artificial intelligence is embedded into tools healthcare providers already use, such as EHR systems, radiology software, and patient management platforms, rather than being introduced as a completely separate system.
Across hospitals and clinics, AI is already being applied in both clinical and operational areas, from diagnosis to administrative workflows.
Common applications include:
Most organizations start with operational use cases such as documentation or scheduling, since they are easier to implement and deliver quick efficiency gains.
The importance of artificial intelligence in healthcare comes from its ability to address structural challenges such as increasing patient demand, limited staff, and rising costs.
AI helps improve diagnostic accuracy, reduce time spent on administrative work, and enable earlier intervention by identifying risks before they become critical. This shifts healthcare delivery from reactive treatment to more proactive care.
For organizations, this is less about adopting a new technology and more about improving how existing systems use data to support better decisions.
Real-world AI applications can be seen across both patient care and hospital operations.
Some widely adopted examples include:
For example, many hospitals use predictive systems to detect early signs of sepsis, allowing intervention hours earlier than traditional methods.
AI helps solve several key challenges in healthcare, including delayed diagnosis, administrative inefficiencies, rising costs, and the underuse of medical data.
Some of the most important problems it addresses include:
This is why adoption often begins with workflow optimization before expanding into clinical decision support.
At a system level, AI improves how decisions are made, how resources are used, and how early interventions happen.
It enables healthcare providers to identify risks sooner, reduce inefficiencies in operations, and allocate time more effectively. Instead of reacting to issues after they occur, organizations can anticipate and prevent them.
The biggest impact is seen when multiple applications, such as predictive analytics and automation, are used together rather than in isolation.
The main types of AI applications in healthcare can be grouped into predictive, diagnostic, generative, and automation-focused systems.
In practice, these include:
Healthcare organizations typically evaluate these as solutions tied to outcomes rather than underlying technologies.
Machine learning enables systems to learn from medical data and improve predictions over time.
It is widely used to identify risk patterns, recommend treatment options, and optimize workflows. As models are exposed to more data, their ability to detect meaningful patterns improves.
For example, hospitals use machine learning to identify patients at high risk of readmission, allowing earlier and more targeted intervention.
Deep learning is an advanced approach designed to handle complex data such as medical images and large datasets.
It plays a major role in imaging-based diagnosis, where it can detect subtle abnormalities that might not be obvious to the human eye. It is also used in genomics and advanced research.
This makes it particularly valuable in areas where early and accurate detection is critical.
The difference lies in how systems use data.
Traditional software follows predefined rules and is mainly used for storing and retrieving information. AI-driven systems analyze data, identify patterns, and generate insights that support decision-making.
For example, instead of simply flagging abnormal lab results, AI can assess multiple variables together to predict potential health risks.
AI is not replacing doctors but is being used to support them by improving efficiency, accuracy, and decision-making.
While these systems can analyze data and assist in diagnosis, they cannot replace human judgment, empathy, and clinical experience. Doctors remain essential for interpreting results and providing care.
In practice, this leads to better efficiency rather than reduced human involvement.
AI can assist in diagnosing diseases by analyzing medical data, but it is typically used alongside healthcare professionals.
It can process imaging data, lab results, and patient histories to identify patterns associated with specific conditions. In some cases, it has shown high accuracy in detecting diseases.
However, diagnosis requires context and judgment, which is why these systems are used as decision-support tools.
AI can be highly accurate, especially in areas like medical imaging and pattern recognition, but its performance depends on data quality and implementation.
Some systems have demonstrated accuracy comparable to human experts in controlled settings. However, real-world performance can vary.
Healthcare organizations must validate these systems carefully to ensure reliability and safety.
AI offers several benefits across both clinical outcomes and operational efficiency. Key advantages include:
These benefits are driving adoption across healthcare systems.
AI also comes with risks that organizations need to consider. Some key risks include:
Managing these risks requires strong governance, compliance, and human oversight.
At its core, AI in healthcare is about improving how data is used to support better decisions, reduce inefficiencies, and enable earlier intervention.
With the fundamentals in place, the next step is to explore how these capabilities translate into real-world healthcare use cases.
Explore practical solutions built around AI in healthcare questions and answers to move from learning to implementation.
Start Your AI Healthcare Journey
Understanding the fundamentals is important, but most healthcare providers and decision-makers are really trying to answer one thing: where does this actually work in practice, and what should we prioritize first?
This section breaks down AI healthcare use cases explained in real-world terms, focusing on where AI is already delivering value across hospitals, clinics, and healthcare organizations. If you’re evaluating adoption, these are the applications that matter most.
AI is used in medical diagnosis to analyze patient data and detect patterns that enable earlier and more accurate disease identification. It is commonly applied in imaging, lab analysis, and risk prediction, where early detection directly improves outcomes.
By processing large datasets quickly, AI helps clinicians identify conditions that might otherwise be missed or detected later. In practice, it acts as a decision-support layer that enhances diagnostic confidence and speed.
AI helps in radiology by analyzing medical images to detect abnormalities and prioritize critical cases. It is widely used in interpreting X-rays, CT scans, and MRIs, where speed and accuracy are essential.
In high-volume environments, AI reduces reporting delays by flagging urgent findings first. This allows radiologists to focus on complex cases, improving both efficiency and consistency in diagnosis.
AI can detect certain cancers early by identifying subtle patterns in imaging and clinical data that may not be immediately visible. It is especially effective in screening workflows, such as breast and lung cancer detection.
Early identification allows for faster intervention, which significantly improves survival rates. However, AI is used alongside clinical validation to confirm diagnosis and guide treatment decisions.
AI is used in drug discovery to analyze biological and chemical data, helping identify viable treatment candidates faster. It reduces reliance on trial-and-error by predicting how compounds will behave.
This shortens early research cycles and lowers development costs. It is particularly valuable in complex areas like genomics and rare diseases, where traditional methods are time-intensive.
AI enables personalized medicine by tailoring treatments based on individual patient data, including genetics, medical history, and lifestyle factors.
This allows healthcare providers to move away from one-size-fits-all approaches and deliver more targeted therapies. The impact is most visible in areas like oncology, where treatment response varies significantly between patients.
AI is used in surgery to improve planning, precision, and intraoperative support. It helps analyze patient data before procedures and, in some cases, guides robotic-assisted systems.
This leads to greater accuracy and reduced risk of complications. In practice, AI enhances surgical capabilities while leaving decision-making fully in the hands of clinicians.
AI in remote patient monitoring refers to analyzing real-time patient data from wearable devices and sensors to detect health risks early.
It is commonly used for chronic disease management, where continuous monitoring can identify subtle changes before they escalate. This reduces hospital visits and enables more proactive care.
AI improves hospital operations by optimizing workflows, resource allocation, and patient flow. It is often used to predict demand, manage bed availability, and streamline scheduling.
These improvements reduce bottlenecks and increase efficiency, allowing hospitals to handle more patients without compromising care quality.
Hospitals use AI across clinical and operational functions to improve outcomes and efficiency simultaneously. On the clinical side, it supports diagnosis and monitoring; on the operational side, it automates workflows and optimizes resources.
This combined approach allows healthcare systems to deliver better care while controlling costs and improving overall performance.
AI is used in mental healthcare to support early detection, monitoring, and patient engagement. It can analyze speech, behavior, and patient inputs to identify patterns associated with conditions like depression or anxiety.
Digital tools also provide continuous support between clinical visits, improving access to care. However, treatment decisions still rely heavily on human professionals.
AI can predict the likelihood of certain diseases by analyzing patterns in patient data before symptoms develop. It uses historical records, biomarkers, and behavioral data to identify risk factors.
This enables earlier intervention, which can prevent or delay disease progression. Predictive capabilities are one of the most valuable aspects of AI in long-term care management.
AI is used in pathology to analyze tissue samples and detect disease-related patterns with high precision. It is particularly effective in identifying cancerous cells in digital pathology slides.
By reducing manual review time, AI allows pathologists to focus on complex cases while improving diagnostic consistency.
AI supports clinical decision-making by analyzing patient data and providing recommendations based on patterns and clinical knowledge.
It can highlight risks, suggest treatment options, and flag inconsistencies. This is especially useful in complex cases where multiple variables must be considered quickly.
AI in medical imaging refers to the use of algorithms to analyze visual data and assist in diagnosis. It improves accuracy, reduces interpretation time, and helps detect abnormalities earlier.
Because it integrates directly into existing workflows, it is one of the most widely adopted applications in modern healthcare systems.
AI is used in emergency care to identify high-risk patients quickly and support triage decisions. It analyzes incoming data in real time to prioritize cases based on severity.
This improves response time and ensures that critical patients receive immediate attention, which can be life-saving in urgent situations.
Get expert support to solve real AI healthcare implementation questions and deploy solutions that actually work in clinical environments.
Build Your AI Healthcare SolutionAI reduces hospital readmissions by identifying patients at high risk before discharge. It analyzes medical history, treatment plans, and recovery trends to predict complications.
This allows healthcare providers to intervene early through follow-ups or care adjustments, improving outcomes and reducing costs.
AI is used in healthcare administration to automate repetitive processes and improve operational efficiency.
Common applications include scheduling, billing, claims processing, and documentation. These improvements reduce manual workload and allow staff to focus more on patient care.
AI automates workflows by handling routine tasks that would otherwise require manual effort.
For example, it can generate clinical documentation, process insurance claims, and manage scheduling. This reduces administrative burden and improves overall efficiency across departments.
Computer vision is used to analyze medical images and detect patterns that support diagnosis and treatment. Key applications include:
These applications improve both speed and accuracy, particularly in data-intensive clinical areas.
Natural language processing (NLP) is used to extract insights from unstructured clinical text such as doctor’s notes and reports.
It converts this data into structured information that can support decision-making and analytics. This is critical because a large portion of healthcare data is not stored in structured formats.
AI improves patient engagement by making communication more timely, accessible, and personalized.
Tools like chatbots, automated reminders, and digital assistants help patients stay informed and adhere to treatment plans. This leads to better outcomes and fewer missed appointments.
AI is used for predictive analytics to identify risks and trends in patient data, enabling earlier intervention.
It helps forecast disease progression, detect complications, and support preventive care strategies. This shifts healthcare from reactive treatment to proactive management.
AI helps scale healthcare services by improving efficiency and enabling better use of resources.
By automating processes and supporting decision-making, healthcare providers can manage higher patient volumes without compromising care quality. This is essential as demand continues to grow.
Real-world adoption of AI in healthcare is driven by practical applications that deliver measurable outcomes across diagnosis, operations, and patient care.
This section reflects some of the most important AI in healthcare FAQs, helping connect real-world use cases with actionable understanding.

Once use cases are clear, the next step is understanding what tools actually power them. This section addresses key AI healthcare guide questions, helping healthcare providers evaluate the technologies behind AI in healthcare and how they are used in practice.
The most popular AI tools in healthcare are those that directly support diagnosis, automation, and patient interaction.
These typically include:
These tools are widely adopted because they integrate easily into existing workflows and deliver measurable results quickly.
The best AI tools for healthcare providers are those that solve specific problems while fitting seamlessly into existing systems.
In practice, providers tend to prioritize tools that reduce administrative burden, improve diagnostic accuracy, or enhance patient engagement. The right choice depends less on features and more on how well the tool aligns with daily workflows and clinical needs.
Generative AI in healthcare refers to systems that create content such as clinical notes, summaries, and patient communication.
It is primarily used to automate documentation and reduce time spent on repetitive writing tasks. For example, clinicians can generate structured notes directly from conversations or patient data.
This is one of the fastest-growing areas because it delivers immediate efficiency gains without major workflow changes.
ChatGPT is used in healthcare workflows mainly for documentation, communication, and internal knowledge support.
Common use cases include:
Its value comes from reducing time spent on text-heavy tasks while improving consistency in communication.
Clinical decision support systems are tools that analyze patient data and provide recommendations to assist clinicians.
They compare patient information with clinical guidelines and historical data to highlight risks or suggest next steps. These systems are especially useful in complex cases where multiple variables need to be evaluated quickly.
Natural language processing (NLP) is used to analyze unstructured clinical text and convert it into usable data.
It processes sources such as doctor’s notes, discharge summaries, and reports, making this information accessible for analytics and decision-making. This is critical because much of healthcare data exists in text form.
Computer vision is used to analyze visual data such as medical images and identify patterns relevant to diagnosis and treatment. It is most commonly applied in:
This improves both diagnostic accuracy and speed, especially in data-intensive clinical areas.
AI-powered EHR systems enhance traditional records by adding intelligence and automation.
They can summarize patient histories, highlight critical information, and provide contextual insights during clinical workflows. This allows healthcare providers to make faster, more informed decisions without replacing existing systems.
Predictive analytics uses AI to analyze historical and real-time data to forecast future outcomes.
It is commonly used to identify high-risk patients, predict disease progression, and anticipate resource needs. This enables earlier intervention and helps shift healthcare from reactive to proactive care.
AI medical chatbots are tools that interact with patients to handle routine communication and support tasks.
They are typically used for:
These tools improve accessibility while reducing the workload on administrative teams.
AI tools that assist doctors focus on analyzing patient data and providing actionable insights.
These include clinical decision support systems, imaging analysis tools, and predictive models. Together, they help clinicians make faster, more accurate decisions, especially in complex or high-risk cases.
Ambient clinical intelligence refers to AI systems that capture and process clinical interactions automatically in the background.
For example, these systems can listen to doctor-patient conversations and generate structured notes without manual input. This reduces documentation burden and allows clinicians to focus more on patient care.
Leverage proven AI in healthcare solutions to automate workflows, optimize operations, and enhance patient outcomes at scale.
See What AI Can Do for Your OrganizationAI scribes are tools that automatically generate clinical documentation from conversations.
They use speech recognition and language processing to capture interactions in real time and convert them into structured notes. This significantly reduces time spent on documentation and improves workflow efficiency.
AI-powered triage systems assess patient symptoms and determine the level of urgency for care.
They are commonly used in emergency settings and digital health platforms to guide patients toward the appropriate level of care. This helps prioritize critical cases and improves overall efficiency.
FDA-approved AI tools are systems that have been validated for safety and effectiveness in clinical use.
They are most commonly found in areas such as imaging and diagnostics, where regulatory approval is required. This ensures that the tools meet specific standards before being used in patient care.
Healthcare SaaS solutions powered by AI are cloud-based platforms that deliver AI capabilities without requiring on-site infrastructure.
They typically offer:
These solutions are preferred because they are scalable, easier to deploy, and more cost-effective than traditional systems.
Understanding the tools behind AI in healthcare is essential for moving from exploration to execution.
This section addresses some of the most common questions about AI in healthcare, helping organizations evaluate which technologies to prioritize and how to approach adoption in a practical, results-driven way.
As organizations move from understanding to execution, automation becomes one of the first practical entry points. This section addresses frequently asked questions on healthcare AI, focusing on how conversational tools and automation systems are applied in real-world settings using AI in healthcare.
AI chatbots in healthcare are software applications that interact with patients and users through text or voice to provide information, support, and basic assistance.
They are commonly used to handle routine tasks such as answering questions, scheduling appointments, and guiding patients. Their main value lies in improving accessibility while reducing the workload on healthcare staff.
Healthcare chatbots work by using natural language processing and predefined workflows to understand user input and generate relevant responses.
They analyze patient queries, match them with trained data or logic, and provide responses in real time. More advanced systems can learn from interactions and improve over time.
In practice, they are often integrated with existing systems like EHRs or patient portals.
Chatbots are used across multiple areas in healthcare, especially where repetitive communication is involved.
Common use cases include:
These use cases are popular because they are easy to implement and deliver immediate efficiency gains.
Chatbots improve patient engagement by making communication faster, more consistent, and available at any time.
They provide instant responses, send reminders, and offer guidance without requiring patients to wait for human interaction. This improves accessibility and helps patients stay connected with their care plans.
As a result, adherence to treatment and appointment attendance often improve.
Healthcare chatbots can be HIPAA compliant, but compliance depends on how they are designed and deployed.
To meet requirements, they must ensure secure data handling, encryption, and controlled access to patient information. They also need to follow strict guidelines around storing and transmitting sensitive data.
Organizations must evaluate vendors carefully to ensure compliance standards are met.
The best healthcare chatbot solutions are those that integrate seamlessly with existing systems and meet compliance requirements.
Rather than focusing on brand names, organizations typically evaluate solutions based on:
The right solution depends on the specific use case and organizational needs.
The cost of building a healthcare chatbot varies depending on complexity, features, and whether it is custom-built or based on existing platforms.
Basic chatbots with limited functionality are relatively affordable, while advanced systems with integrations, AI capabilities, and compliance features require higher investment.
In most cases, cost is influenced more by AI integration services and compliance requirements than by the chatbot itself.
Conversational AI in healthcare refers to advanced systems that enable natural, human-like interactions between users and digital tools.
Unlike basic chatbots, conversational AI can understand context, manage multi-step conversations, and provide more personalized responses. It is used in patient support, virtual assistants, and automated communication systems.
Virtual healthcare assistants are AI-powered tools that support both patients and healthcare providers.
They are used to:
These assistants improve efficiency while enhancing the overall user experience.
AI is widely used to automate administrative tasks that consume time and resources.
Common solutions include tools for scheduling, billing, claims processing, and documentation. These systems reduce manual effort and improve accuracy across operations.
Automation is often the first step organizations take when adopting AI because it delivers quick and measurable results.
AI chatbots reduce operational costs by automating repetitive communication and reducing the need for manual intervention.
They handle large volumes of patient interactions without requiring additional staff, which lowers administrative expenses. They also reduce errors and improve efficiency in processes like scheduling and support.
Over time, these savings can be significant, especially in high-volume healthcare environments.
AI chatbots and automation tools represent some of the most accessible and high-impact entry points into AI in healthcare.
This section builds on core healthcare AI basics questions and answers, showing how organizations can improve efficiency, reduce costs, and enhance patient experience through practical, scalable solutions.

As organizations move from exploration to execution, choosing the right partner becomes one of the most critical decisions. This section addresses key medical AI questions explained, focusing on how to evaluate vendors, development companies, and solution providers involved in AI in healthcare.
Top AI healthcare software development companies in the USA are those with proven experience in regulated environments, strong integration capabilities, and successful deployments in hospitals or clinics.
Rather than relying on generic rankings, organizations should prioritize companies that have worked on similar use cases and can demonstrate measurable outcomes. In healthcare, domain expertise and compliance knowledge matter more than brand visibility.
The best AI healthcare software companies are those that deliver production-ready solutions, not just prototypes or demos.
They typically specialize in areas like diagnostics, predictive analytics, or automation, and have validated their solutions in real clinical settings. The key differentiator is their ability to move from concept to deployment while meeting regulatory and integration requirements.
Healthcare software development companies design, build, and maintain systems that support clinical and operational workflows.
This includes developing applications, integrating with EHR systems, ensuring compliance, and supporting deployment. More advanced firms also build AI-driven solutions such as analytics platforms and automation tools.
The real value lies in connecting these systems into a cohesive, usable workflow.
Choosing the right AI healthcare development company is less about features and more about fit.
You should evaluate:
A technically strong company without healthcare context often struggles, while a domain-focused partner can significantly reduce implementation risk.
Top AI healthcare startups are usually focused on solving one specific problem exceptionally well.
They often lead innovation in areas like diagnostics, remote monitoring, or automation. However, they may lack the maturity or scalability of larger vendors.
They are best suited for targeted use cases rather than large, system-wide implementations.
Successful AI healthcare companies are defined by real-world impact, not just technology.
They typically have:
Success in healthcare is less about innovation alone and more about reliable execution.
AI healthcare development companies offer services across the full lifecycle of implementation. These usually include:
Outsourcing is often the most practical option for organizations without in-house AI or development expertise.
It allows faster execution and access to specialized skills. However, it introduces dependency on external partners, which makes vendor selection critical.
The decision should balance speed, control, and long-term strategy.
Outsourcing provides clear advantages when done correctly.
However, these benefits only materialize when working with a partner that understands healthcare-specific requirements.
Hiring healthcare software developers requires a mix of technical and domain expertise.
Developers should understand healthcare workflows, compliance requirements, and integration challenges. In many cases, organizations rely on specialized firms or vendors to hire AI developers rather than building large in-house teams from scratch.
A strong vendor should demonstrate reliability, compliance knowledge, and the ability to integrate into existing systems.
Look for evidence of past success, clear communication, and long-term support capabilities. Vendors should also understand how their solutions will be used in real workflows, not just how they are built.
Healthcare automation companies focus on streamlining administrative and operational processes.
They build tools for scheduling, billing, documentation, and workflow management. These solutions are often the easiest entry point into AI adoption because they deliver quick efficiency gains.
Healthcare IT software companies provide the foundational systems used across healthcare organizations.
This includes EHR systems, hospital management platforms, analytics tools, and AI-enabled solutions. These companies are essential for maintaining digital infrastructure and enabling integration.
The best providers are those that consistently deliver reliable, scalable, and compliant solutions.
Rather than focusing on brand names, organizations should evaluate providers based on performance, integration capability, and long-term support. The best provider is one that fits your specific operational needs.
Companies that build custom solutions focus on tailoring AI systems to specific organizational requirements.
This is often necessary when off-the-shelf tools do not fit workflows or data structures. Custom software development companies offer flexibility but require more time, investment, and ongoing support.
End-to-end providers manage the full lifecycle of AI projects, from strategy to deployment.
They reduce complexity by handling consulting, development, integration, and scaling within a single engagement. This is particularly valuable for organizations with limited internal resources.
Vendors in this category focus on building solutions that meet regulatory standards while supporting long-term growth.
They ensure secure data handling, interoperability, and the ability to scale across systems. These factors are critical for organizations planning large-scale adoption.
Companies specializing in diagnostics and monitoring build AI software that directly impact patient outcomes.
These include imaging systems, predictive models, and remote monitoring platforms. Organizations should prioritize accuracy, validation, and clinical usability when evaluating these vendors.
Vendors focused on analytics provide tools that turn large datasets into actionable insights.
They help identify trends, predict risks, and support clinical decisions. The best vendors combine strong analytics capabilities with seamless integration into existing systems.
These companies specialize in AI conversation apps and workflow automation.
They build chatbots, virtual assistants, and automation tools that improve communication and reduce administrative workload. These solutions are often used as entry points into AI adoption.
Case studies should be evaluated based on relevance, not just results.
Look for:
A strong case study demonstrates both capability and practical impact.
Work with experts who understand AI in healthcare explained for providers with practical questions and can turn concepts into deployable systems.
Talk to Our AI ExpertsIntegration-focused companies ensure that AI tools work with existing systems such as EHRs and hospital software.
This is often one of the most critical aspects of implementation, as poor integration can limit the value of even the best AI tools.
Trusted providers are those with a consistent track record of successful deployments and strong client relationships.
They demonstrate reliability through long-term partnerships, compliance adherence, and consistent performance across projects.
Some companies provide both strategic guidance and technical execution.
They help organizations identify use cases, plan implementation, and build solutions tailored to their needs. This combination of AI consulting services is especially useful for organizations early in their AI journey.
Shortlisting should focus on alignment rather than quantity.
Organizations typically narrow down options based on experience, expertise, and proven results. A focused shortlist allows for deeper evaluation and better decision-making.
Comparing vendors requires evaluating both technical and practical factors.
The best partner is one that aligns with your long-term goals, not just immediate needs.
These companies manage the entire AI lifecycle, from planning to implementation and scaling.
They are particularly valuable for complex projects where coordination across multiple stages is required. Working with a single partner reduces fragmentation and improves overall execution.
Selecting the right partner is a strategic decision that directly impacts the success of AI in healthcare initiatives.
This section simplifies AI healthcare concepts explained simply, helping organizations move from exploration to confident vendor selection based on real-world considerations.
Understanding tools and vendors is only part of the journey. The real challenge lies in execution, where most AI initiatives either succeed or fail. This section addresses practical AI healthcare implementation questions, focusing on how organizations can realistically adopt and scale AI in healthcare without overcomplicating the process.
Hospitals implement AI systems through phased rollouts rather than large-scale deployments.
In practice, most start with a single use case, such as documentation or imaging, run a controlled pilot, and validate results before expanding. What often slows implementation is not the technology itself, but integration with existing systems and staff adoption.
The most successful hospitals treat AI as a gradual capability build, not a one-time deployment.
AI adoption follows a structured path, but execution often breaks down when steps are rushed or skipped.
A realistic sequence includes:
The biggest mistake is jumping directly to scaling without validating the initial use case.
Waiting rarely reduces complexity; it only delays learning.
Most organizations benefit from starting now with focused use cases where AI is already proven, such as automation or imaging. The real advantage of early adoption is not just ROI, but building internal experience and readiness.
Organizations that wait often struggle later because they lack both data maturity and operational familiarity.
AI fails when it forces clinicians to change how they work instead of fitting into existing processes.
Successful implementations prioritize:
If a solution adds friction, adoption drops regardless of its technical quality.
The best starting point is where value is obvious and resistance is low. Most organizations begin with:
These areas deliver quick wins and help build trust before moving into more complex use cases.
Practical use cases are those that balance impact with ease of implementation.
Automation, predictive analytics, and imaging support are commonly prioritized because they require less structural change while delivering measurable outcomes. The goal is not to start with the most advanced use case, but the most executable one.
Successful execution depends more on alignment than technology. Organizations need to align:
Implementation typically fails when one of these is overlooked, especially data quality or workflow integration.
Clinics without technical teams should avoid building from scratch. Instead, they can adopt:
These options reduce complexity and allow clinics to focus on usage rather than development.
The easiest way to start is with a single, clearly defined problem that affects daily operations.
In most cases, this is documentation or scheduling. These use cases require minimal integration, show quick results, and help organizations understand how AI fits into their workflows.
AI does not always require heavy infrastructure, especially with modern cloud-based solutions.
At a minimum, organizations need secure data storage, access to relevant datasets, and integration capabilities. In practice, infrastructure becomes a challenge only when scaling, not during initial adoption.
AI systems rely on clean, structured, and relevant data to function effectively.
This typically includes patient records, imaging data, lab results, and clinical notes. However, the real challenge is not data availability, but data quality and consistency.
Poor data leads to poor outcomes, regardless of how advanced the model is.
Integration is one of the most critical and difficult parts of implementation.
AI tools need to connect with EHR systems so that insights are available within existing workflows. This is usually done through APIs, but real challenges often include data formatting, system compatibility, and workflow alignment.
Many projects fail not because of AI, but because integration is underestimated.
The biggest challenges are rarely technical in isolation. They typically include:
Among these, adoption and workflow fit are often the hardest to solve.
Most failures come from strategic missteps rather than technical ones. Common mistakes include:
AI adoption works best when treated as an iterative process, not a one-time rollout.
AI is highly scalable, but only after the initial foundation is stable.
Once data pipelines, integrations, and workflows are established, organizations can expand use cases across departments. Scaling too early, however, often leads to inconsistent results and operational friction.
Small clinics do not need complex AI systems, but they can benefit significantly from targeted solutions.
Even simple tools for automation or communication can improve efficiency and patient experience. The key is to match the solution to the scale of the organization.
AI implementation requires a mix of technical, clinical, and operational expertise.
This includes data handling, system integration, and understanding healthcare workflows. Most organizations rely on external partners to complement internal capabilities.
Effective use of patient data depends on structure, quality, and governance.
AI systems analyze this data to identify patterns, predict risks, and support decisions. However, without proper data preparation and compliance controls, even the best tools fail to deliver value.
Organizations should prioritize technologies that are easy to implement and deliver immediate value.
These include automation tools, predictive analytics, and imaging support. Starting here builds momentum and creates a foundation for more advanced use cases.
The key is to integrate AI into existing systems rather than layering it on top.
This involves choosing tools that align with current workflows, introducing them gradually, and ensuring that they reduce effort rather than add to it.
Adoption improves when users barely notice the transition.
Start with one clearly defined use case, not a full system overhaul.
For example, begin with diagnostic support or patient management automation, validate results, and then expand. Trying to implement multiple solutions at once usually leads to complexity and slower progress.
AI generates insights by identifying patterns across large datasets.
This requires structured data, proper integration, and tools designed for analytics. Insights can then be used to predict risks, improve decision-making, and optimize operations.
The quality of insights depends entirely on the quality of data.
Choosing the right platform depends on how well it fits your existing systems and long-term goals. Organizations should evaluate:
The best solution is not the most advanced, but the one that fits your environment and can be adopted successfully.
Implementing AI in healthcare is less about technology and more about execution discipline.
This section reflects the most common questions about AI in healthcare explained, showing that success comes from starting small, integrating carefully, and scaling based on real results rather than assumptions.
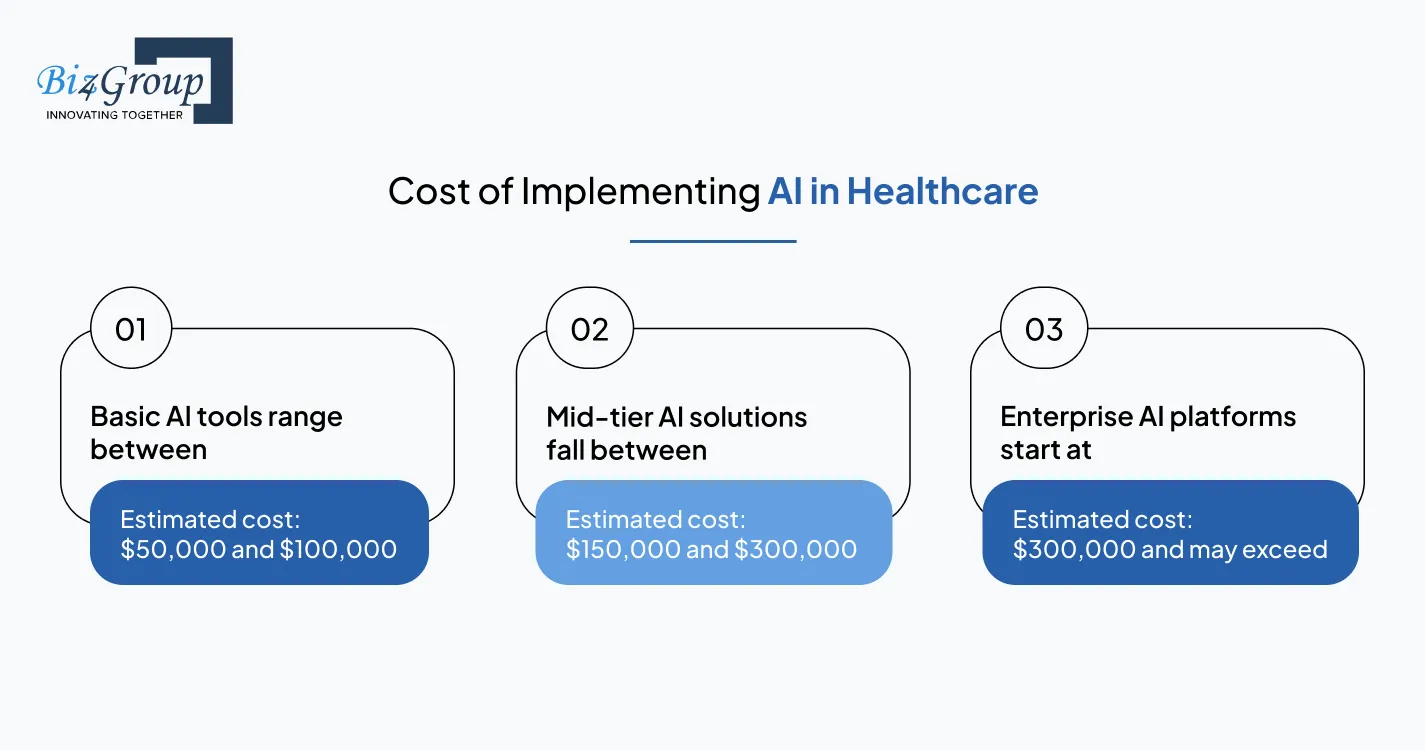
At some point, every organization evaluating AI moves past curiosity and into financial reality: what will this cost, where will the money go, and when will it pay back? This section acts as a beginner guide to AI in healthcare with questions and answers, helping decision-makers understand the real economics of adopting AI in healthcare beyond surface-level estimates.
The cost of AI in healthcare is not a single number but a combination of multiple cost layers that vary by use case. In practice, organizations spend on:
The biggest misconception is that AI itself is expensive. In reality, most cost comes from making AI usable within existing healthcare environments.
Implementation costs are typically higher than the cost of the tool itself.
Most of the budget goes into integration, data readiness, and workflow alignment rather than the AI model. This is why two organizations using the same tool can have very different total costs.
The more complex your existing systems, the higher the implementation effort.
The cost of building a healthcare app depends heavily on compliance, integrations, and data handling requirements.
Apps that require EHR integration, real-time processing, and regulatory compliance are significantly more expensive than standalone applications. Adding AI capabilities increases complexity further, especially when custom models are involved.
The real cost driver is not features, but how deeply the app connects with healthcare systems.
AI development costs are primarily driven by complexity and data. The most important cost drivers include:
Among these, data preparation is often the most underestimated and time-consuming component.
Chatbot costs vary widely based on how advanced and integrated the solution is. Basic chatbots that handle FAQs or scheduling are relatively low-cost. However, once you add:
The cost increases significantly.
Most of the cost comes from integration and ensuring secure handling of patient data.
ROI from AI in healthcare typically shows up in three areas: cost reduction, efficiency gains, and improved outcomes.
However, not all use cases deliver ROI equally. In practice:
The key is to start with use cases where ROI is both measurable and achievable within a short timeframe.
ROI timelines depend more on implementation complexity than on the AI itself.
Simple automation tools can deliver results within months because they require minimal integration. More complex systems, especially those involving predictive models or custom development, take longer due to validation and workflow alignment.
Organizations that start small tend to see faster and more reliable returns.
AI reduces costs by eliminating inefficiencies that are built into healthcare operations. This includes:
Cost reduction is rarely immediate, but it compounds over time as workflows become more efficient.
Hidden costs are one of the biggest reasons AI projects exceed budgets. The most common ones include:
Organizations that plan only for software costs often underestimate total investment significantly.
ROI calculation requires looking beyond direct cost savings. Organizations typically measure:
The challenge is that some benefits are indirect, which is why defining clear metrics early is critical.
Discover how real-world use cases from common questions about AI in healthcare can guide your next digital transformation initiative.
Explore AI Use CasesAI can be highly cost-effective for small practices when applied selectively. Instead of large-scale systems, small practices benefit most from:
These use cases require low investment but deliver immediate operational improvements.
Before investing, organizations should evaluate both financial and operational readiness. This includes:
The most successful investments are those tied to specific, measurable outcomes rather than broad experimentation.
The economics of AI in healthcare are less about upfront cost and more about where and how the investment is applied.
This section reflects a detailed FAQ on artificial intelligence in healthcare industry, helping organizations move beyond cost concerns and make informed decisions based on real-world financial impact.
As organizations move closer to deployment, regulatory and security concerns become one of the biggest decision barriers. This section addresses the top questions healthcare providers ask about AI adoption, focusing on how compliance, data protection, and risk are handled in real-world implementations of AI in healthcare.
Yes, AI in healthcare is regulated in the US, but regulation is fragmented and depends on how the system is used.
There is no single “AI law” for healthcare. Instead, different aspects are governed by different frameworks:
In practice, this means organizations must evaluate compliance based on the specific use case, not AI as a whole.
FDA approval means that an AI tool has been evaluated for safety, accuracy, and clinical reliability before being used in patient care.
This applies mainly to AI systems involved in diagnosis, imaging, or treatment recommendations. However, not all AI tools require FDA approval. Many administrative or workflow tools fall outside this category.
A common mistake is assuming all AI must be FDA-approved, when in reality it depends on whether the tool directly impacts clinical decisions.
AI systems that process patient data must meet HIPAA requirements for privacy, security, and accountability. In practice, this includes:
Most compliance issues arise not from the AI model itself, but from how data flows between systems and vendors.
AI does not “ensure” privacy on its own - privacy depends on how the system is designed and governed. Organizations typically use:
However, the biggest risk comes from integration points, where data moves between systems. This is where privacy controls must be strongest.
AI systems handle sensitive data by operating within defined regulatory and governance frameworks. This means:
In reality, compliance is not a one-time setup. It requires continuous monitoring, especially as models evolve and new data is introduced.
AI in healthcare can be highly secure, but only when security is treated as a core design requirement. Most security risks come from:
The AI itself is rarely the weak point. Instead, security depends on the surrounding infrastructure and how systems are implemented and managed.
Organizations that follow best practices can achieve security levels comparable to or better than traditional healthcare systems.
Regulation and security are not barriers to adopting AI in healthcare, but they do require careful execution and awareness of where risks actually occur.
This section reflects AI healthcare use cases explained through FAQs, helping organizations move forward with confidence by understanding how compliance and security work in real-world scenarios.
As adoption grows, it’s just as important to understand where AI falls short as it is to understand its benefits. This section addresses important questions about AI in healthcare for hospitals and clinics, focusing on the real risks, limitations, and failure points organizations encounter when implementing AI in healthcare.
The biggest risks of AI in healthcare come from poor implementation, not the technology itself. In practice, the most common risks include:
The key point is that AI amplifies both strengths and weaknesses in a system. If data and processes are flawed, AI can scale those problems.
AI in medical diagnosis is powerful, but it has clear limitations.
It relies heavily on the data it has been trained on, which means it may struggle with rare conditions, incomplete data, or cases that fall outside its training patterns. It also lacks contextual understanding that human clinicians bring, such as patient history nuances or atypical presentations.
This is why AI is used as a support tool rather than a replacement for clinical judgment.
Yes, AI can and does make mistakes in healthcare, just like any system or human. Errors usually occur due to:
What makes AI different is that mistakes can scale quickly if not monitored properly. This is why human oversight and validation are critical in any AI-driven system.
Most AI healthcare projects fail not because the technology doesn’t work, but because implementation is misaligned with reality. The most common reasons include:
Successful projects treat AI as part of a broader system change, not a standalone solution.
Understanding the risks and limitations of AI in healthcare is essential for making informed decisions and avoiding costly mistakes.
This section is part of everything you need to know about AI in healthcare Q&A guide, helping organizations approach AI adoption with realistic expectations, proper safeguards, and a clear understanding of where it works best, and where it doesn’t.
Use insights from this detailed FAQ on artificial intelligence in healthcare industry to choose the right tools, partners, and strategy.
Start Your AI Transformation TodayFor organizations that want full control, flexibility, and long-term differentiation, custom development becomes a serious consideration. This section answers AI in healthcare explained for providers with practical questions, focusing on how custom systems are actually built and deployed in real-world implementations of AI in healthcare.
Building custom AI healthcare software for diagnosis and analytics is a structured process that combines clinical understanding, data engineering, and system integration. It is not just about creating a model - it is about building a reliable, usable system that fits into real clinical workflows.
The process begins with defining a clear and narrow use case. Without this, projects quickly lose direction.
Common starting points include:
A well-defined problem ensures that both technical and clinical teams stay aligned.
The next phase is data preparation, which is often the most time-consuming part. Healthcare data is:
To make it usable, it must be:
In most real-world projects, this step takes more effort than AI model development itself. Once data is ready, teams move into model development and training. Depending on the use case, this may involve:
However, performance is not just about accuracy. The model must also handle edge cases and different patient populations reliably. After development, clinical validation becomes critical. This step ensures that:
Without proper validation, even accurate models cannot be trusted in practice. The next challenge is integration into existing systems. This is where many projects fail. The AI system must:
If the system creates friction, adoption drops immediately.
Finally, deployment and continuous improvement determine long-term success. AI systems require:
Without this, accuracy and reliability degrade over time.
In practice, successful custom AI development is less about building advanced models and more about aligning data, workflows, and clinical needs into a system that actually gets used.
By this stage, most organizations are no longer asking what AI can do. The real question is how to make it work inside an actual healthcare environment.
On paper, implementation looks linear. Define a use case, pick a solution, deploy it. In reality, execution is where things get complicated. Data is fragmented, systems don’t always integrate cleanly, and even well-built solutions struggle if they disrupt how clinicians already work.
This gap between idea and execution is where many AI initiatives stall. Experience changes how this problem is approached.
Instead of starting with the model, experienced teams focus on the environment in which that model will operate. That means thinking early about:
This shift often determines whether a system gets adopted or quietly ignored.
Companies like Biz4Group LLC , which is one of the top AI development companies in Florida, operate with this execution-first mindset.
The focus is not just on building AI systems, but on making sure those systems:
That difference between building and operationalizing is what separates working solutions from stalled projects.
You can see this more clearly through real implementations.
Solutions like Dr Ara extend AI beyond traditional clinical settings by combining performance and health data into actionable insights. The real challenge there was not just analysis, but presenting insights in a way users could actually use.
In a different context, CogniHelp focuses on supporting dementia patients in daily life. Here, simplicity and reliability mattered more than complexity, because adoption depends on how comfortably patients and caregivers can interact with the system.
At a broader system level, Truman demonstrates how AI can improve both patient interaction and operational efficiency, which requires balancing intelligence with usability and integration.
Across these examples, a consistent pattern shows up.
It’s not the sophistication of the AI that determines success. It’s how well the system fits into its environment. That usually comes down to a few things:
This is why many organizations move from experimentation to collaboration. Not because they lack capability, but because the cost of getting it wrong is high. Delays, rework, and failed adoption often outweigh the initial savings of trying to do everything internally.
Working with experienced teams doesn’t remove complexity. It changes how that complexity is handled, making execution more predictable and less risky.
Understanding AI is only the starting point. The real value comes from execution, and execution in healthcare depends on how well systems align with data, workflows, and real-world constraints.
That’s where experience makes the difference between a promising idea and an enterprise AI solution that actually works.
This guide brought together answers to 130+ real questions people ask when exploring AI in healthcare, covering everything from basics and use cases to tools, costs, implementation, risks, and choosing the right partners.
Across all of this, the issue isn’t really about understanding AI anymore. It’s about deciding where to start and how to make it work in a practical way. The organizations that move forward successfully usually keep things simple. They pick one clear problem, test a solution, and then build on what works instead of trying to do too much at once.
AI in healthcare works best when it’s approached step by step. Focus on what will create real impact in your setup, make sure it fits into your existing workflows, and then expand from there.
At this point, you already have the clarity most teams spend months trying to get. What matters now is taking that first step and doing it right.
Ready to turn insights into action? Book a consultation with our experts and start building your AI healthcare solution today.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.