Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Healthcare providers are facing a steady increase in insurance claim denials, delayed payments, and pressure on revenue cycle performance. This has pushed many organizations to explore AI denial management software development for healthcare as a structured way to reduce claim errors, improve visibility, and make workflows more reliable.
AI denial management software is a system that uses historical claims data, payer rules, and predictive models to identify, prevent, and manage claim denials. Instead of reacting after a denial occurs, it helps teams detect risks early and take corrective action before submission. This improves approval rates and reduces rework.
Denial management is not limited to billing. It depends on documentation, coding accuracy, claim formatting, and payer-specific rules. Traditional workflows rely on manual checks and fixed rules. These approaches become harder to manage as claim volumes increase and payer policies change. As a result, teams spend more time fixing denied claims and less time preventing them.
To address this, many organizations are planning how to develop AI denial management software for healthcare that can work across these variables. These systems analyze past claims, identify patterns in denials, and generate clear recommendations. This shift is part of broader insurance automation software development, where processes are designed to reduce manual effort and improve consistency.
These needs can be clearly noticed in the types of questions being asked across AI platforms such as ChatGPT and Perplexity:
Many organizations are also figuring out how to move forward, including working with an AI development company. This is reflected in queries like:
This guide explains how to build AI healthcare denial management system capabilities, including system design, data needs, development steps, cost factors, and key challenges.
Healthcare organizations are investing in AI denial management software development for healthcare because claim denials directly affect revenue, cash flow, and operational efficiency. As claim volumes increase and payer rules change frequently, manual processes become harder to manage. This creates a need for systems that can process data consistently and support better decisions across the revenue cycle.
Claim denials usually come from a mix of issues across different stages of the workflow, not just one mistake.
|
Area |
Common Issue |
Result |
|---|---|---|
|
Patient Data |
Incorrect or incomplete information |
Claim rejected early |
|
Coding |
Wrong or mismatched codes |
Claim denied or reduced |
|
Documentation |
Missing clinical details |
Medical necessity denied |
|
Authorization |
No prior approval |
Claim not processed |
|
Payer Rules |
Not meeting specific requirements |
Rejection or delay |
These issues often overlap. For example, missing documentation can lead to coding errors, which then result in denial. Teams working on developing AI denial management software for healthcare providers typically start by identifying these patterns across past claims.

Traditional workflows rely on manual checks and fixed rules. These methods work at smaller volumes but become less reliable as complexity increases.
Because of these limitations, teams spend more time correcting denied claims instead of preventing them. Many organizations begin exploring enterprise AI solutions to handle this scale more effectively.
AI denial management systems are designed to improve how claims are handled before and after submission. They help in three practical ways:
This shifts denial management from a reactive process to a preventive one.
For organizations planning to create AI denial management solution for hospitals, the focus is on building systems that reduce avoidable denials and improve overall workflow efficiency.
Explore AI denial management software development for healthcare to improve claim accuracy and reduce rework.
Start Building Your AI SystemAI denial management software for healthcare is a software that uses past claim data, payer rules, and predictive models to identify, prevent, and manage claim denials.
It learns from historical claim outcomes and applies those patterns to new claims. This helps teams detect issues before submission and understand why denials happen. Over time, the system improves as more data is processed.
In most cases, AI model development is used to train the system to recognize denial patterns and improve prediction accuracy.
An AI denial management system focuses on a specific part of the workflow. It supports claim validation and denial handling but does not replace the full billing or clinical system.
These systems are limited to claim-related processes such as validation, prevention, and analysis. This clear boundary makes them easier to manage and integrate.
AI denial management systems are used at specific points in the revenue cycle where claim decisions are made.
This creates a cycle where each claim outcome improves the next one.
For organizations planning to make AI healthcare denial management software, understanding this placement helps ensure smooth integration with existing billing and revenue workflows.
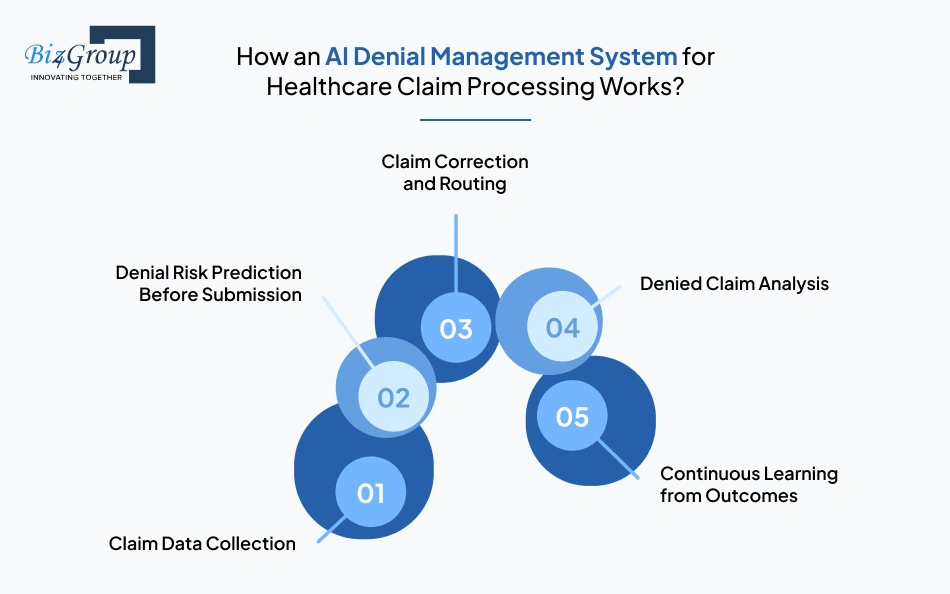
An AI denial management system works as a step-by-step process that checks claims, identifies risks, guides corrections, and learns from outcomes. In AI denial management software development for healthcare, this flow is designed to reduce errors before submission and improve how denied claims are handled after submission.
|
Stage in Claim Workflow |
What the System Does |
Result on Claim Processing |
|---|---|---|
|
Claim Data Collection |
Collects claim data from EHR, billing systems, and payer inputs, including patient details, codes, and documentation |
Creates a clean and structured dataset for review |
|
Denial Risk Prediction Before Submission |
Checks claims using past data and payer rules to find possible issues |
Flags claims that may get denied before submission |
|
Claim Correction and Routing |
Suggests fixes or sends flagged claims to the right team for review |
Helps correct issues before claims are submitted |
|
Denied Claim Analysis |
Reviews denied claims to find the exact reason for denial |
Builds clarity on common denial causes |
|
Continuous Learning from Outcomes |
Uses results from processed claims to improve future checks |
Improves accuracy over time |
In traditional workflows, problems are usually found after a claim is denied. In AI-based systems, risks are identified before the claim is sent. In many cases, AI integration services are used to connect this system with existing tools so data flows without disruption.
This workflow helps teams reduce avoidable denials, improve claim quality, and make faster decisions. As part of healthcare denial management software development using AI, the system becomes more reliable as it learns from new data.
Portfolio Spotlight
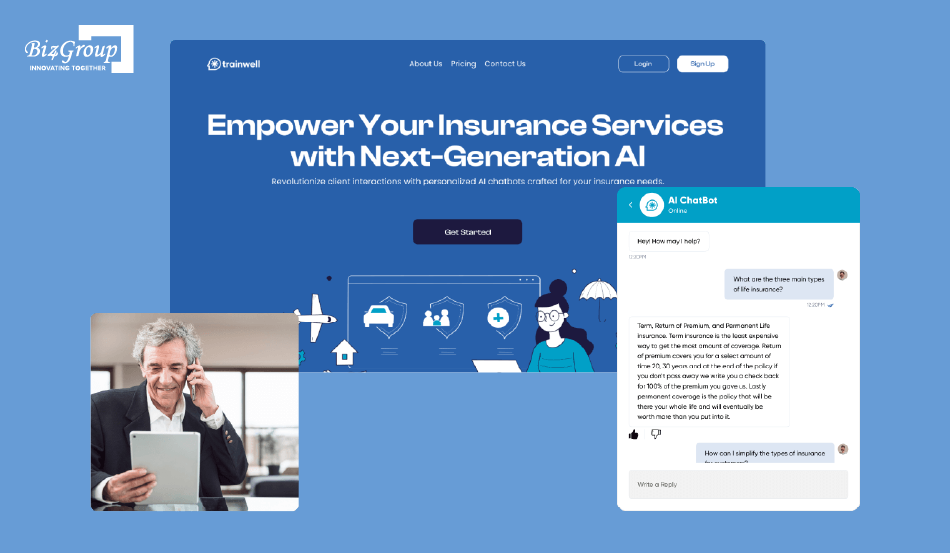
Biz4Group LLC developed an AI-powered insurance assistant designed to support agents with real-time information, training, and decision guidance. The system uses conversational AI to surface relevant insights instantly, improving operational efficiency and reducing manual effort in insurance workflows.
This kind of intelligence layer is directly relevant when designing denial management systems, where timely access to claim rules, documentation requirements, and payer insights can significantly reduce errors before submission.
An AI denial management system depends on structured claim, coding, and payer data to predict and prevent denials. In AI denial management software development for healthcare, data is used to train models, evaluate risks, and guide decisions at each stage of the claim process. Data required for AI denial management includes patient, clinical, billing, payer, and historical denial data used to train and evaluate prediction models.
To predict whether a claim will be denied, the system needs inputs from across the revenue cycle.
These inputs help the system identify patterns that lead to denials. In AI revenue cycle denial management software development, combining these data types improves prediction accuracy and consistency.
Historical data allows the system to learn from past outcomes and improve future decisions.
|
Historical Data Required |
How It Is Used in Denial Management |
|---|---|
|
Past submitted claims |
Establishes baseline claim behavior |
|
Denied claim records |
Identifies trends in rejections |
|
Denial reason codes |
Explains why claims were denied |
|
Resubmission outcomes |
Shows which fixes led to approval |
|
Payment timelines |
Highlights delays and processing gaps |
Most systems require at least 6 to 12 months of historical claims data to identify reliable denial patterns.
Payer rules directly affect whether a claim is approved or denied. Payer variation is one of the main reasons claims are rejected, making it a key factor in system design.
Because these rules are not consistent, systems need a structured way to interpret and apply them during claim evaluation. This is often where teams bring in AI consulting services early, not just for model design but to map payer logic into a usable format for the system.
Even when data is available, quality issues can reduce system accuracy. Before development, common problems need to be resolved:
Without clean and complete data, predictions become unreliable.
For teams planning how to build scalable AI denial management system for insurance claim processing, data quality and coverage directly determine how well the system can prevent claim denials.
Build AI healthcare denial management system capabilities that flag risks early and guide corrections in real time.
Explore Your AI Strategy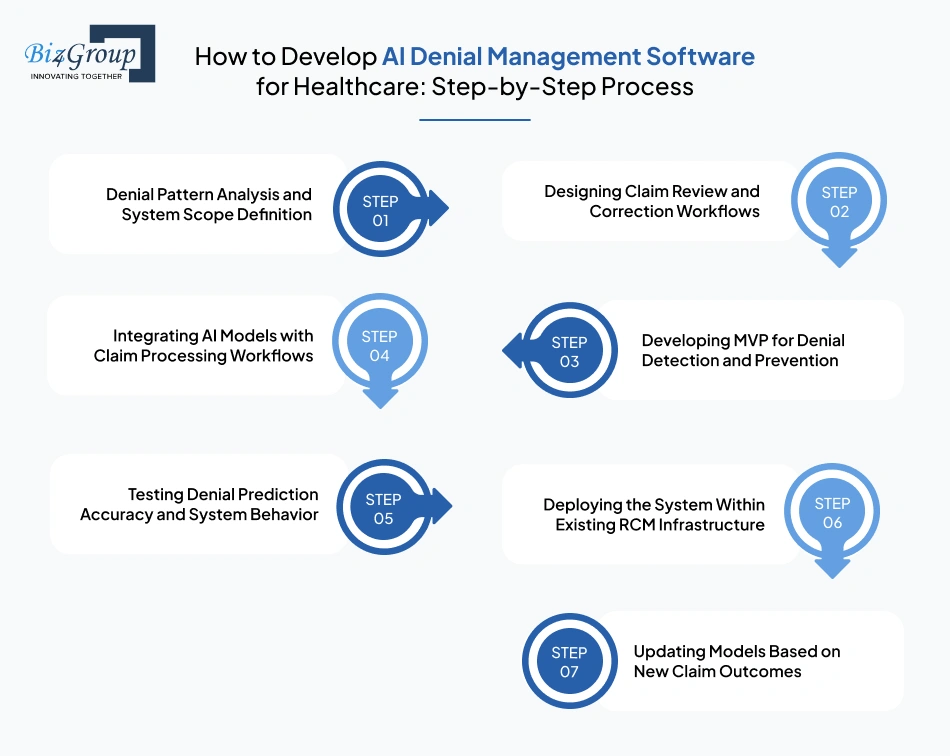
Developing an AI system for denial management is about fixing where claims fail, not just adding automation. In AI denial management software development for healthcare, each step focuses on reducing preventable denials by improving how claims are validated, corrected, and learned from over time.
Before building anything, you need clarity on why claims are getting denied in your system.
Most teams initially assume coding errors are the main issue, but once data is reviewed, patterns usually point to a mix of documentation gaps, payer rule mismatches, and workflow delays.
Start by:
If your goal is to create AI system to reduce insurance claim denials in hospitals, this step defines what the system should actually solve, instead of trying to automate everything at once.
Denial management is a time-sensitive task. If the system slows teams down, it won’t be used. The UI/UX design should answer three questions instantly:
Instead of dashboards full of data, the focus should be on:
This is where many systems fail. They provide insights, but not usable actions.
Working with a strong UI/UX design helps align design with real billing workflows.
Also read: Top UI UX design companies in USA
At this stage, the focus is not scale, it’s validation. Instead of building a full platform, start with MVP development services:
Teams that successfully build AI solution for healthcare claim denial prediction and prevention usually begin with a system that can answer one question reliably:
“Will this claim be denied if submitted right now?”
Core modules to build first:
Also read: MVP software development
Once the MVP works, the system needs to move beyond rules and start learning from data. This is where most complexity comes in. Claims are not uniform. The same procedure can be accepted by one payer and denied by another. The system must learn these variations instead of applying generic logic.
Teams that develop automated AI system for healthcare claims denial management focus heavily on:
Without this layer, the system remains a rule engine, not an adaptive system.
At this point, the system is interacting with real patient and financial data. The challenge is not just protecting data, but ensuring decisions made by the system can be explained and audited. Key focus areas:
This is also where many organizations evaluate companies that develop AI denial management software for healthcare providers in USA, especially when internal teams lack healthcare-specific compliance experience.
Also Read: Software Testing Companies in USA
Deployment is where systems often fail, not because of technology, but because they don’t fit existing workflows. The system should:
Instead of a full rollout, start with:
This controlled approach helps identify issues early before scaling.
Denial patterns change constantly. Payer rules evolve, coding practices shift, and new errors appear. A static system will lose accuracy quickly.
To build scalable AI denial management system for insurance claim processing, the system must continuously:
Over time, the system becomes less dependent on manual intervention and more reliable in preventing denials before they happen.
Develop AI denial management software for healthcare to improve first-pass claim acceptance and accelerate reimbursements.
Improve Your Revenue CycleThe tech stack for an AI denial management system defines how claims are validated, risks are identified, and corrections are applied across the revenue cycle. In AI denial management software development for healthcare, the stack includes frontend, backend, API, AI, and data layers that work together to check claims before submission and improve outcomes after denial.
|
Label |
Preferred Technologies |
Why It Matters |
|---|---|---|
|
Frontend Layer (RCM Interfaces) |
React, Angular |
Displays claim risk, errors, and actions in real time; using ReactJS development helps billing teams act quickly on flagged claims |
|
Server-Side Rendering & Performance Layer |
Next.js, Nuxt.js |
Ensures fast loading of data-heavy dashboards; NextJS development improves usability during high claim volumes |
|
Backend Layer (Processing & APIs) |
Node.js, Python, Django, FastAPI |
Handles claim validation, routing, and system logic; combining services with NodeJS development and Python development supports both APIs and AI workloads |
|
API & Integration Layer (EHR, Billing, Payers) |
REST APIs, GraphQL, HL7 FHIR APIs |
Connects systems so claim data flows automatically between EHR, billing, and payer platforms without manual steps |
|
AI & Model Layer (Prediction & Learning) |
TensorFlow, Scikit-learn, PyTorch, XGBoost |
Identifies denial risks before submission and improves predictions using past claim outcomes |
|
Model Serving Layer (Real-Time Inference) |
FastAPI, TensorFlow Serving, TorchServe |
Delivers predictions instantly during claim processing so teams can act before submission |
|
Data Processing Layer (Pipelines & Streaming) |
Apache Kafka, Airflow, Spark |
Ensures claims are evaluated continuously and updated with denial outcomes for learning |
|
Data Storage Layer (Claims & AI Data) |
PostgreSQL, MongoDB, Snowflake |
Stores claim history, denial reasons, and outcomes for analysis and model training |
|
Workflow Orchestration Layer |
Camunda, Temporal, Apache Airflow |
Routes flagged claims to the right teams and manages correction and resubmission workflows |
|
Cloud Infrastructure Layer |
AWS, Azure, Google Cloud |
Supports large claim volumes and ensures system availability during peak processing periods |
|
Security & Compliance Layer |
OAuth 2.0, HIPAA-compliant services, IAM |
Protects patient and financial data and ensures all claim processing meets compliance requirements |
|
Monitoring & Observability Layer |
Prometheus, Grafana, ELK Stack |
Tracks system performance, prediction accuracy, and workflow efficiency in real time |
A well-structured tech stack ensures claims are checked before submission, denial risks are identified early, and correction workflows run without disruption. This alignment between technology and revenue cycle operations is what makes the system reliable in real-world healthcare environments.
The decision to build or buy depends on how your denial workflows operate today. In AI denial management software development for healthcare, building means creating a system tailored to your processes, while buying means adopting a ready-made solution from a vendor.
The choice usually comes down to:
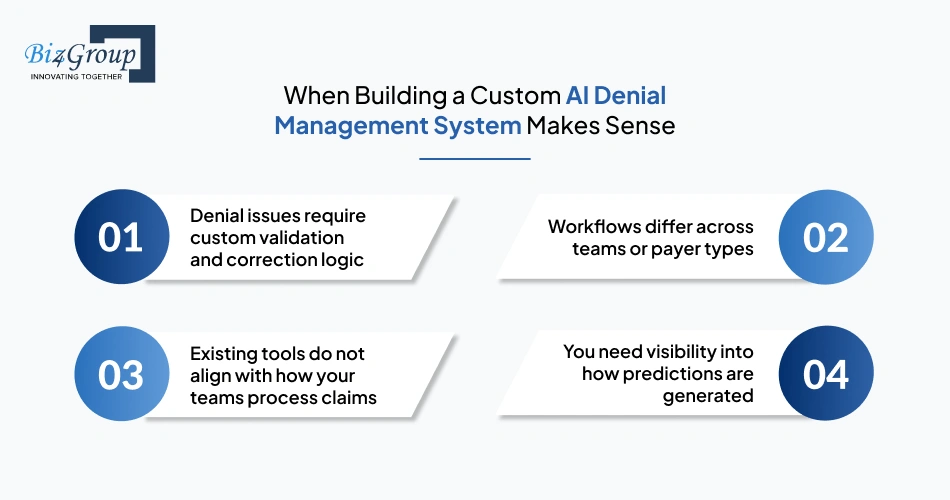
Building is a better fit when standard solutions cannot handle your workflows.
Organizations that develop AI denial management software for healthcare usually take this route when denial management directly impacts financial performance. In such cases, working with a custom software development company allows the system to fit existing operations instead of changing them.
Buying is more practical when speed and simplicity matter more than customization.
|
Scenario |
When Buying Is the Better Choice |
|---|---|
|
Limited internal technical capability |
Avoids building and maintaining systems internally |
|
Need for faster implementation |
Systems can be deployed in a shorter timeframe |
|
Common denial scenarios |
Pre-built models handle standard cases effectively |
|
Budget constraints |
Lower initial investment compared to custom builds |
Many organizations that build AI healthcare denial management system capabilities through vendors use this approach to start quickly and improve performance without long development cycles.
Each option involves trade-offs that affect how the system performs over time.
These trade-offs influence how early issues are identified and how easily workflows can be improved. Some organizations take a hybrid approach by starting with a vendor solution and extending it later using AI automation services.
Use this checklist to guide your decision:
If your goal is to create AI denial management solution for hospitals, focus on how well the system will support your workflows over time rather than just how quickly it can be implemented.
The cost of AI denial management software development for healthcare typically ranges from $10,000 to $150,000+, which should be treated as a ballpark estimate. Costs increase as the system moves from basic validation to full-scale prediction, integration, and automation.
|
Cost Tier |
Estimated Cost Range |
What It Includes |
Typical Use Case |
|---|---|---|---|
|
MVP-Level (Low Complexity) |
$10,000 – $30,000 |
Basic claim validation, limited denial prediction, simple dashboards, minimal integrations |
Testing denial prediction on a small dataset or single workflow |
|
Advanced System (Mid Complexity) |
$30,000 – $80,000 |
Expanded prediction models, payer-specific rules, integration with billing systems, improved workflows |
Reducing denials across multiple categories and departments |
|
Enterprise-Grade System (High Complexity) |
$80,000 – $150,000+ |
Real-time processing, full-scale prediction and prevention, deep EHR and payer integrations, continuous model updates |
Large providers handling high claim volumes and complex workflows |
Costs increase with data preparation, model complexity, and the number of system integrations required. Systems that require real-time validation or multi-payer support typically fall into higher cost ranges.
For organizations planning to create AI denial management solution for hospitals, understanding these cost factors helps define the right scope before moving into development decisions.
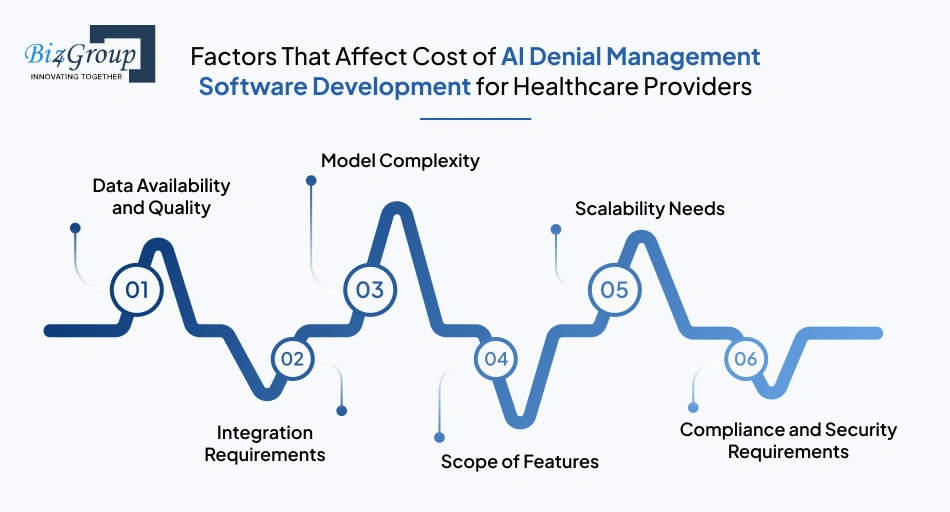
Cost is mainly affected by data quality, integrations, model complexity, feature scope, scalability, and compliance requirements. These factors determine how much time, effort, and infrastructure the system requires. In most cases, data quality and integration complexity are the biggest cost drivers.
Poor data quality increases development time and cost. Missing, inconsistent, or unstructured claim data requires additional effort for cleaning and preparation.
Connecting with EHR, billing systems, and payer platforms adds complexity. More integrations increase development effort and testing time.
Basic rule-based systems cost less, while advanced prediction models require more data, training, and validation.
More features such as real-time validation, prediction, and automated correction workflows increase development and testing effort.
Systems designed to handle large claim volumes require stronger infrastructure, which increases both development and operational costs.
Meeting healthcare data regulations adds additional validation, security layers, and ongoing maintenance effort.
A clear understanding of these factors helps define the right system scope and avoid unexpected cost increases during development.
Build scalable AI denial management system for insurance claim processing with workflows aligned to real operations.
Plan Your AI ImplementationClaim denial prediction uses a combination of methods to check claims, identify risks, and guide corrections. In AI denial management software development for healthcare, these approaches include rule-based validation, machine learning models, and natural language processing applied to claims and documentation. Each method solves a different part of the problem.
Both approaches are used together, but for different types of tasks.
|
Approach |
Where It Is Used |
Limitation |
|---|---|---|
|
Rule-Based Systems |
Fixed checks like missing data, eligibility, and payer rules |
Cannot adapt to new patterns |
|
Machine Learning Models |
Detecting patterns across claims and denial history |
Needs clean data and regular updates |
Rule-based systems handle strict validations, while machine learning models identify patterns that are not explicitly defined. In practice:
Teams developing AI denial management software for healthcare providers usually start with rules and expand into models as more data becomes available.
Denial prediction is treated as a classification problem where each claim is labeled as likely approved or denied. Common models include:
These models help identify relationships between claim data, coding patterns, and denial outcomes. When teams are building AI claims denial management system, they often combine simpler and advanced models to balance accuracy and explainability.
A large part of denial risk comes from unstructured data such as clinical notes and supporting documents.
This is important because many denials happen due to incomplete or unclear documentation. In some systems, generative AI is used to summarize notes or suggest improvements before submission, reducing manual effort and improving claim quality.
No system can maximize all three at the same time. Each implementation needs to balance them based on where it is used.
For example:
In denial management, this balance affects how early risks are detected and how confidently teams can act.
Organizations that make AI healthcare denial management software adjust this balance based on workflow needs. In many cases, they hire AI developers to fine-tune performance based on operational priorities.
Also Read: AI in Healthcare Explained: 130+ Questions Answered for Healthcare Providers and Innovators
Scaling an AI denial management system means handling more claims, more payer rules, and more data without reducing speed or accuracy. In AI denial management software development for healthcare, the system must continue to validate claims, predict risks, and support corrections even as usage grows.
High claim volumes require parallel processing and optimized data pipelines to avoid delays. The system should process multiple claims at the same time instead of sequentially. In healthcare denial management software development using AI, this is achieved using distributed processing and asynchronous validation so claim checks do not slow down during peak periods.
Payer variation is one of the main challenges in scaling denial management systems. Each payer has different validation rules, and these rules change over time. To manage this, systems use version-controlled rule layers so updates can be applied without affecting existing workflows.
Real-time processing supports immediate claim validation before submission, while batch processing is used for deeper analysis after claims are processed. A scalable system supports both. In some cases, organizations integrate AI into an app so real-time validation can happen directly within billing workflows, while batch systems handle pattern analysis in the background.
Model drift occurs when claim patterns and payer behavior change, causing predictions to become less accurate over time. To manage this, systems need continuous monitoring and regular retraining using recent data. In AI revenue cycle denial management software development, keeping models updated is necessary to maintain prediction reliability.
A scalable system maintains speed, accuracy, and consistency even as claim volume and complexity increase.
Create AI denial management solution for hospitals that integrates with billing systems and improves claim validation.
Start Your AI Development Journey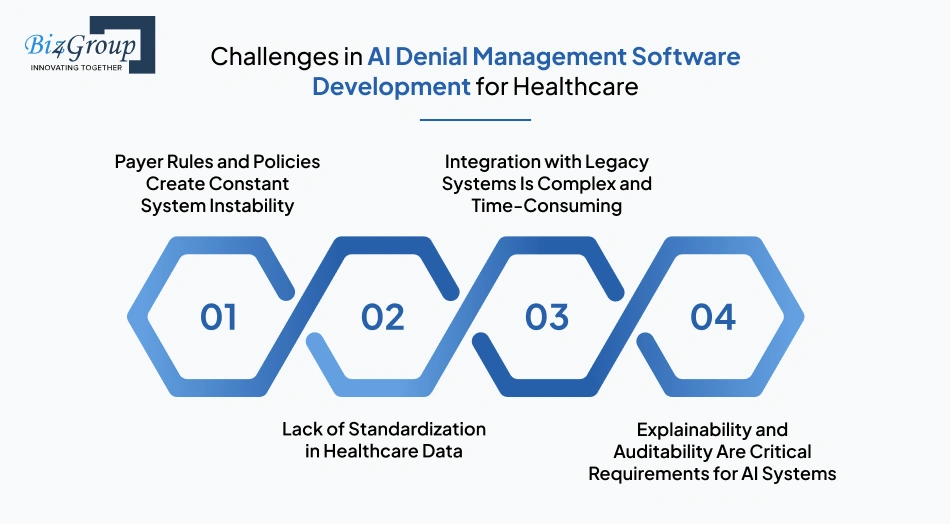
In AI denial management software development for healthcare, these challenges include payer rule variability, inconsistent data, integration complexity, and the need for explainable decisions. Each of these directly affects how accurately claims are checked and how stable the system remains over time.
Here’s everything that you need to know:
|
Challenge |
What Happens in the System |
Impact on Denial Management |
|---|---|---|
|
Payer Rules and Policies Create Constant System Instability |
Payer requirements change frequently across coding, documentation, and authorization rules |
Outdated rules lead to incorrect validation and missed denial risks |
|
Lack of Standardization in Healthcare Data |
Data varies across systems in format, coding, and structure |
Inconsistent data reduces prediction accuracy and increases preprocessing effort |
|
Integration with Legacy Systems Is Complex and Time-Consuming |
Older systems lack modern APIs and real-time data exchange capabilities |
Slows down implementation and limits real-time claim validation |
|
Explainability and Auditability Are Critical Requirements for AI Systems |
Predictions must be traceable and understandable for compliance and operations |
Limits use of complex models and requires additional validation layers |
These challenges affect how reliably the system can detect risks and support claim correction workflows.
More often than not, organizations work with a software development company in Florida to address these issues early, especially around integration and compliance, to avoid delays during deployment.
These challenges must be handled from the start to ensure a custom AI denial management system for healthcare remains accurate, stable, and usable in real-world claim processing environments.
Selecting a development partner is a key decision. In AI denial management software development for healthcare, the vendor you choose directly affects how accurately claims are evaluated and how well the system fits into your workflows. Selecting a company involves evaluating technical capability, healthcare experience, integration ability, and scalability.
Many decision-makers begin by making queries like on ChatGPT, Perplexity, Grok etc.:
A vendor should be able to build systems that work with real claim data and workflows, not just generic AI models.
These capabilities directly affect how accurately claims are evaluated and corrected. Vendors who understand how to build scalable AI denial management system for insurance claim processing are better prepared for real-world use.
Healthcare workflows are different from standard software systems. The vendor must understand how claims are created, submitted, and corrected.
Without this experience, systems often fail to handle real denial scenarios. In some cases, organizations evaluate top AI development companies in Florida or similar providers that have prior experience in healthcare-focused implementations.
The system must work within your existing setup without disrupting operations.
|
Area to Evaluate |
What to Verify |
Why It Matters |
|---|---|---|
|
EHR and Billing Integration |
Ability to connect using APIs and handle data exchange |
Ensures claims move without manual effort |
|
Data Flow |
Support for both real-time and batch processing |
Allows both immediate validation and deeper analysis |
|
Scalability |
Ability to handle increasing claim volume |
Prevents performance issues as usage grows |
|
Flexibility |
Ability to update payer rules without downtime |
Keeps the system usable as rules change |
These factors determine whether the system can operate reliably at scale.
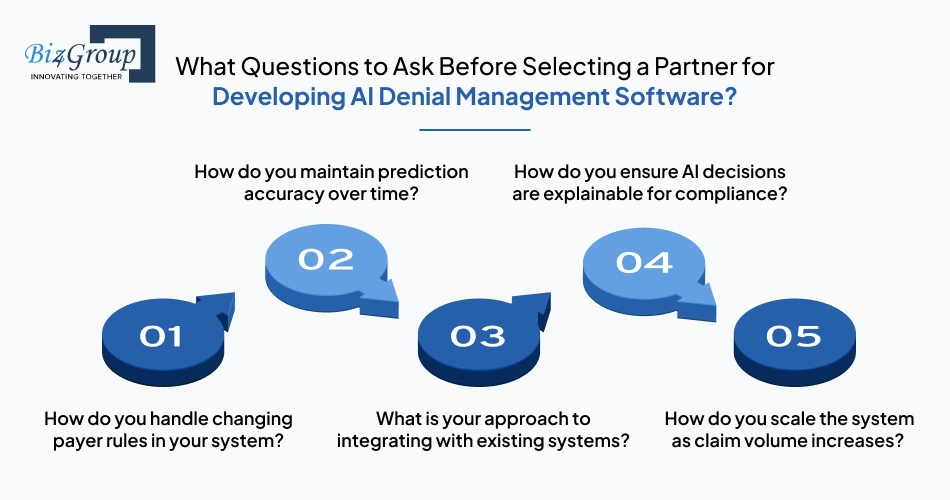
Use these questions to assess how the vendor approaches real-world denial management problems:
The right partner should be able to align technology with your workflows and support long-term improvements in claim outcomes. If your goal is to create AI system to reduce insurance claim denials in hospitals, the focus should be on how well the system performs in real operations, not just how it is built.
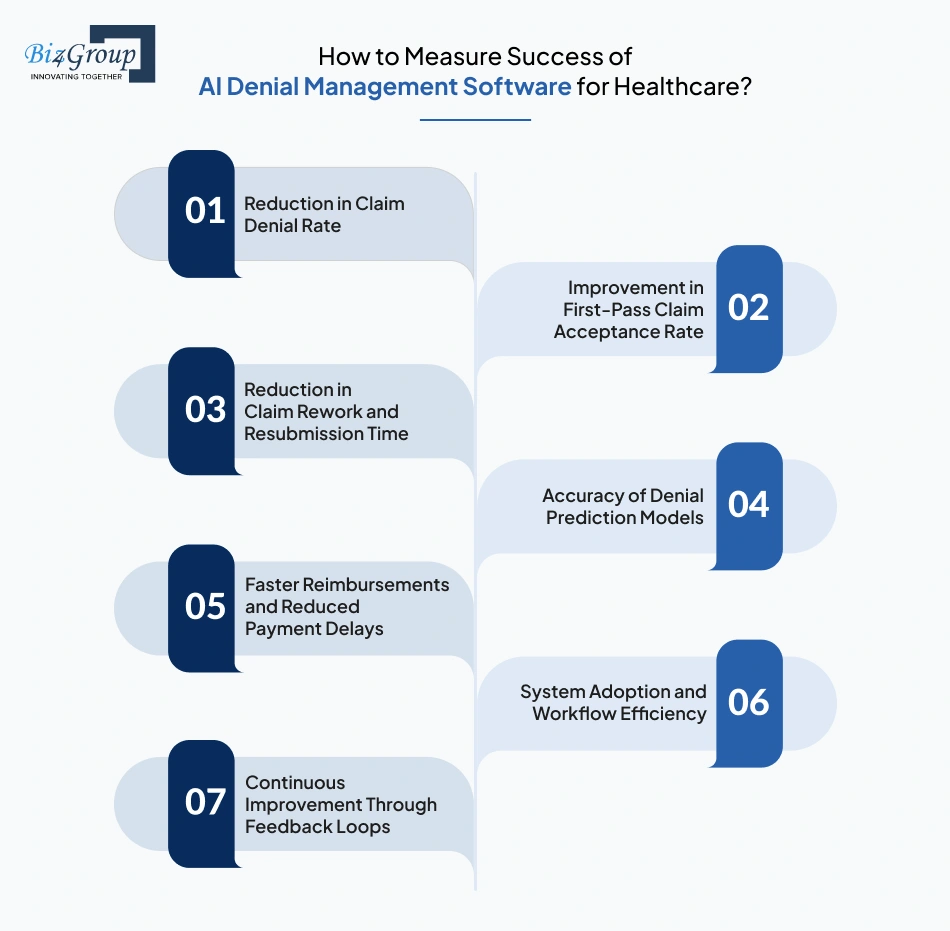
When it comes to AI denial management software development for healthcare, success is measured using denial rates, claim accuracy, processing time, and revenue cycle impact. These metrics show whether the system is preventing errors before submission and improving outcomes after denial.
This shows how many denials are avoided. It should be tracked overall and by denial category to understand where improvements are happening.
This measures how many claims are approved on the first submission. When teams build AI solution for healthcare claim denial prediction and prevention, a higher first-pass rate indicates better claim quality.
This tracks how long it takes to correct and resubmit denied claims. A lower time indicates fewer errors and more efficient workflows.
This measures how correctly the system identifies high-risk claims. It includes tracking precision, recall, and consistency over time.
This reflects how quickly payments are received after claim submission. Improvements here show better revenue cycle performance.
This shows whether billing and coding teams are actively using the system. In some cases, features similar to an AI assistant app help teams review and act on claims more efficiently.
This measures how the system improves over time using new claim data. Organizations that develop automated AI system for healthcare claims denial management rely on continuous updates to maintain accuracy.
These metrics should be tracked regularly to measure ongoing improvement. A successful system reduces denials, improves claim accuracy, and speeds up the revenue cycle.
AI denial management systems improve claim processing, but they also introduce risks that can affect accuracy and workflow performance. In AI denial management software development for healthcare, these risks include incorrect predictions, data issues, system limitations, and workflow misalignment. These risks affect data quality, system performance, and operational adoption, and if not managed, they can increase denial rates instead of reducing them.
If the system is used without human review, incorrect predictions can lead to wrong claim actions. This is especially risky for complex or high-value claims where manual validation is still required.
Incomplete or inconsistent data leads to unreliable predictions. If training data is not accurate, the system will repeat the same errors at scale.
Payer rules change frequently. If the system is not updated in time, it may apply outdated logic, leading to incorrect claim validation and higher denial rates.
If the system does not integrate properly with EHR or billing systems, claim data may not flow correctly. This can delay processing and create gaps in validation.
If users cannot understand why a claim was flagged, they may not trust or use the system. Explainability is also required for compliance and audit purposes.
As claim volume increases, the system may slow down if not designed for scale. This can delay validation and affect submission timelines. Organizations evaluating companies that develop AI denial management software for healthcare providers in USA often check how systems perform under high load.
Over time, claim patterns and payer behavior change. If models are not updated regularly, prediction accuracy decreases and risks increase.
If the system does not match how billing teams work, it may not be used effectively. In some cases, solutions built with a focus on business app development using AI address this by aligning system behavior with real workflows.
Managing these risks ensures the system remains accurate, reliable, and effective in reducing claim denials. For organizations planning to build scalable AI denial management system for insurance claim processing, addressing these risks early helps maintain long-term performance.
Develop automated AI system for healthcare claims denial management that supports faster decisions and better outcomes.
Connect With Our AI ExpertsChoosing the right approach depends on what you want to improve in your revenue cycle. In AI denial management software development for healthcare, the approach should match your primary goal, whether it is reducing denials, improving cash flow, or scaling operations. Each priority requires a different system design and focus.
|
Priority |
What to Focus On |
|---|---|
|
Reduce Claim Denials |
Pre-submission validation and risk prediction |
|
Improve Cash Flow |
Faster claim processing and resubmission |
|
Scale Operations |
Automation and infrastructure readiness |
The focus should be on preventing errors before claims are submitted.
Organizations that develop AI denial management software for healthcare for this goal prioritize early detection and correction of errors.
Faster claim processing leads to quicker reimbursements and improved cash flow.
|
Area of Focus |
What to Prioritize |
|---|---|
|
Claim Processing |
Reduce delays in validation and submission |
|
Denial Handling |
Speed up correction and resubmission |
|
Payment Flow |
Track and reduce payment delays |
This approach focuses on reducing turnaround time across the claim lifecycle.
Scaling requires the system to handle more claims without slowing down.
In some systems, features similar to an AI chatbot integration help teams interact with the system more efficiently as volume increases.
The approach should match available resources, timelines, and expected outcomes.
Organizations that build AI healthcare denial management system capabilities successfully align system design with operational priorities instead of trying to solve everything at once.
The right approach is the one that aligns system design with your primary goal and operational constraints.
Biz4Group LLC is an AI product development company that builds systems for claim validation, denial prediction, and workflow automation. The focus is on creating solutions that fit into real healthcare operations rather than adding complexity.
The insurance AI platform referenced earlier reflect this approach, where AI is used to support decision-making, automate processes, and reduce manual effort. The same approach is applied when you build an AI app for denial management, where accuracy and usability directly affect claim outcomes.
What sets Biz4Group LLC apart:
Biz4Group focuses on delivering systems that improve claim accuracy, reduce manual effort, and support better revenue cycle performance.
AI denial management changes how claims are handled from the start. Instead of reacting after a denial, the system focuses on preventing errors before submission and improving decisions during processing. This leads to fewer rejections, faster reimbursements, and more stable revenue cycles.
For healthcare providers investing in AI denial management software development for healthcare, the focus shifts to how effectively they can build AI software that fits existing workflows, works with real claim data, and supports teams without adding complexity. The impact comes from consistent validation, clear insights, and systems that improve over time.
When implemented well, it becomes part of everyday operations, helping teams process claims with greater accuracy and confidence.
Connect with our AI experts to define a step-by-step plan to implement AI in your denial management workflow.
The implementation timeline typically ranges from 3 to 9 months, depending on data readiness, system complexity, and integration requirements. Projects with clean historical data and fewer integrations move faster, while enterprise-level systems with multiple payers and workflows take longer.
AI denial management systems must comply with healthcare regulations such as HIPAA in the United States. This includes secure data storage, controlled access, encryption, and audit trails to ensure patient and financial data are protected throughout the claim processing lifecycle.
Yes, most systems are designed to integrate with existing EHR and billing platforms using APIs or standard healthcare data formats. However, the level of integration depends on how modern and flexible the existing systems are.
The cost typically ranges from $30,000 to $200,000+, depending on system scope, data complexity, integrations, and scalability requirements. Smaller systems focused on specific workflows cost less, while enterprise-grade solutions with real-time processing and multiple integrations fall on the higher end.
Teams need a mix of domain and technical understanding, including:
No advanced technical expertise is required, but training is important for effective use.
These systems use a combination of historical data and continuous learning. When new denial patterns appear, they are captured through feedback loops and incorporated into model updates, allowing the system to adapt over time.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.