Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Insurance claims processing is one of the most resource-intensive operations in the industry. Many insurers still rely on manual workflows for document review, data entry, and claim validation. This leads to delays, higher operational costs, and inconsistent outcomes. To address these challenges, organizations are increasingly choosing to develop an AI automated system for insurance claim that can standardize and accelerate the entire process.
An AI automated system for insurance claims is a software system that ingests claim data, extracts relevant information from documents, evaluates policy coverage, and supports decision-making using a combination of machine learning models and rule-based logic. The system operates across multiple stages of the claim lifecycle, reducing manual effort while maintaining auditability and control.
In real world, insurers use such systems to build AI insurance claim automation system capabilities that can process high volumes of claims with consistent accuracy. Instead of routing every claim through manual verification, the system identifies required data, validates inputs, and flags exceptions for review. This allows teams to focus only on complex or high-risk cases.
Implementing this type of solution requires more than just model development. It involves coordinated insurance automation software development, where data pipelines, decision engines, and workflow systems must work together reliably. Without this alignment, automation remains partial and difficult to scale.
If you’ve been exploring this space through AI tools or search platforms, your queries may look like this:
These queries indicate a shift toward structured, scalable automation rather than incremental process improvements. Working with an experienced AI development company becomes important when the goal is to design systems that integrate with existing infrastructure and support long-term operational efficiency.
This guide explains how to create AI insurance claim processing software, covering system components, workflows, architecture, data requirements, and decision frameworks needed to implement a scalable and reliable solution.
Insurance claims processing involves multiple steps such as data capture, document review, policy validation, and decision-making. These steps are often handled across disconnected systems, which slows down processing and increases operational overhead. To address this, organizations choose to develop an AI automated system for insurance claim that can unify these steps into a single, structured workflow.
An AI automated system for insurance claim is a software system that captures claim inputs, extracts structured data from documents, evaluates coverage rules, and supports decision-making using machine learning models and rule-based logic. It functions as a centralized processing layer that connects data inputs, validation logic, and decision workflows into a continuous pipeline.
In practice, this system is implemented through AI automated system development for insurance claim, where components such as document processing, validation engines, and workflow orchestration operate together to process claims in a consistent and traceable manner.
Claims operations often suffer from delays, inconsistent evaluations, and fragmented processing steps. These issues become more pronounced as claim volumes increase.
An AI-based claims system addresses these problems by:
Extracting structured data directly from documents instead of manual transcription
Each claim follows a defined path, making it easier to monitor processing status and audit decisions when required.
AI systems are most effective in stages where decisions depend on structured inputs and repeatable logic. These stages can be automated either fully or partially based on system design.
Common automation areas include:
These capabilities are enabled through insurance claim automation software development, where automation is applied to high-frequency tasks while maintaining control over decision logic.
AI systems are designed to handle structured and repeatable tasks, but certain claim scenarios require human judgment. Human review is typically required in:
In these scenarios, the system routes claims to human reviewers along with relevant data and system-generated insights. This ensures that complex cases are handled with context while routine processing remains automated.
Organizations often implement such systems as part of broader enterprise AI solutions, where automation and human oversight are combined to maintain accuracy, accountability, and operational control.
An AI insurance claim system is built as a set of modular components, where each component handles a specific function such as data extraction, validation, decisioning, or workflow control. To develop an AI automated system for insurance claim, these components must be clearly defined and structured so that claim data can move through the system without manual intervention at each step.
Each component is responsible for transforming inputs into usable outputs. When combined, they form a processing pipeline that ensures claims are handled in a consistent, traceable, and scalable manner.
|
Component |
What It Does |
Why It Matters |
|---|---|---|
|
Document Processing and Data Extraction |
Extracts structured data from claim documents using OCR and NLP |
Ensures consistent and usable data for downstream processing |
|
Claim Validation and Decision Engine |
Applies rules and logic to evaluate coverage and eligibility |
Enables consistent and faster claim decisions |
|
Fraud Detection System |
Identifies anomalies and assigns risk scores |
Flags suspicious claims early to reduce financial risk |
|
Workflow Automation and Orchestration |
Routes claims and manages processing steps |
Prevents delays and ensures smooth claim progression |
|
Integration with Core Insurance Systems |
Connects with policy, CRM, and payment systems |
Enables end-to-end processing without data silos |
These components do not operate in isolation. The output of one module becomes the input for the next, creating a continuous flow where data is progressively refined and evaluated.
This interconnected design is central to AI insurance claims management system development, where the goal is to ensure that each stage of claim processing is both automated and logically consistent across the system. In practice, organizations often rely on AI integration services to connect these components with existing infrastructure and ensure reliable system behavior.
The workflow of an AI insurance claim system defines how a claim moves from submission to final decision through a sequence of automated steps. To develop an AI automated system for insurance claim, this workflow must be designed as a connected pipeline where each stage processes data, applies logic, and passes structured outputs to the next stage without manual handoffs.
The system captures claim data from sources such as digital forms, emails, or uploaded files. It standardizes inputs by organizing structured fields and storing unstructured data for further processing. This step ensures that all incoming claims enter the system in a consistent format.
The system extracts key information from documents such as invoices, reports, and forms. Using OCR and language processing, it converts unstructured content into structured data fields. This allows downstream processes to operate on normalized inputs.
The system checks claim details against policy terms, coverage limits, and predefined rules. It determines whether the claim meets eligibility conditions. This step filters out invalid or incomplete claims early in the process.
The system evaluates claim characteristics using scoring models and predefined criteria. It assigns a risk score and flags claims that deviate from expected patterns. This helps prioritize which claims require closer review.
The system determines the claim outcome based on validation results and risk assessment. It approves, rejects, or routes the claim for further review. For approved claims, it triggers settlement actions such as payment processing or notifications.
The system routes complex or flagged claims to human reviewers. These include cases with missing data, inconsistencies, or high-risk indicators. Reviewers receive structured data and system insights to support faster decision-making.
This workflow acts as a decision pipeline where each stage refines claim data and reduces uncertainty before the final outcome. It forms the foundation of AI insurance claims management system development, where consistent inputs and rule-based evaluation drive decisions. Organizations often use AI consulting services to align this workflow with policy logic and operational constraints.
Learn how to develop an AI automated system for insurance claim with structured data, validation, and automation layers.
Explore AI Claim AutomationFraud detection in an AI insurance claim system is the process of checking claim data for patterns that indicate unusual or suspicious behavior. When organizations develop an AI automated system for insurance claim, fraud detection works as a scoring layer that evaluates risk at different stages of the workflow.
Fraud detection systems are built to identify both known fraud patterns and unexpected behavior.
Common fraud patterns include:
These patterns are evaluated using historical data, rule checks, and anomaly detection models as part of custom AI automated system development for insurance claim.
|
Approach |
How It Works |
Key Trade-Off |
|---|---|---|
|
Rule-Based Detection |
Applies predefined conditions such as thresholds, duplicates, or known fraud signals |
Easy to explain and audit, but limited to known patterns |
|
Machine Learning Detection |
Learns patterns from past data to identify unusual behavior |
Can detect new patterns, but needs ongoing training and monitoring |
Key takeaway:
Most systems combine both approaches when they develop AI claims processing system for insurance.
Fraud detection is usually implemented through a scoring pipeline that evaluates each claim using multiple signals. Pipeline structure:
This ensures that every claim is evaluated in the same way without relying on manual checks.
Fraud detection systems improve over time by learning from real outcomes.
This ongoing improvement depends on continuous AI model development, where detection systems adapt to new fraud patterns.
Fraud detection works as a continuous evaluation layer where each claim is checked before a decision is made. It is a key part of AI insurance claims management system development, ensuring that risk is measured consistently and used in claim processing decisions.
Also Read: Is Fraud Hurting Your Insurance Business? AI Can Detect and Prevent 90% of Fraudulent Claims
An AI insurance claim system is structured as a processing pipeline where claim data moves through ingestion, validation, scoring, and decision layers. To develop an AI automated system for insurance claim, the system must be designed so that each layer operates independently but passes structured outputs forward without reprocessing or manual intervention.
|
Design Area |
What It Involves |
Why It Matters |
|---|---|---|
|
What a Scalable Architecture Looks Like |
A modular setup where ingestion, processing, decision, and workflow components run as separate services |
Allows the system to handle increasing claim volumes without affecting performance |
|
How Data Flows Across the System |
Data moves through defined pipelines from intake to processing, validation, and decision stages |
Ensures each stage works on structured and consistent inputs |
|
How AI Models and Rule Engines Work Together |
Models generate outputs such as risk scores, while rule engines apply policy conditions and thresholds |
Maintains balance between adaptive detection and controlled decision-making |
|
Real-Time vs Batch Processing Decisions |
Real-time processing handles immediate claim actions, while batch processing handles bulk operations at intervals |
Helps manage trade-offs between speed, cost, and system efficiency |
In this setup, each layer performs a fixed role. Data is ingested once, transformed into structured format, evaluated through rules and models, and then passed to decision logic without duplication. When teams integrate AI into an app, this flow ensures that model outputs, rule evaluations, and workflow actions remain aligned without creating processing gaps.
This design allows the system to process claims as a continuous flow instead of isolated steps. Organizations that build AI-powered insurance automation system capabilities use this approach to maintain consistent data handling and decision logic as claim volume increases.
Start to build AI insurance claim automation system that reduces delays and improves decision accuracy across workflows.
Start Building Your SystemAn AI insurance claim system relies on specific technologies mapped to different stages of claim processing, such as data extraction, risk evaluation, workflow control, and system execution. To develop an AI automated system for insurance claim, each of these technologies must perform a defined role in the processing pipeline so that data can move from input to decision without rework or dependency on manual steps.
These models operate at the input layer of the system. They extract structured data from unstructured documents such as claim forms, invoices, and reports. Using OCR and language processing, they identify key fields like claimant details, incident data, and financial values. This is a core requirement in developing AI insurance processing system, where accurate input data is necessary for all downstream processing.
These models operate at the evaluation stage. They analyze claim data using historical patterns and assign risk scores based on anomalies or deviations. This helps identify claims that require additional review. Often built using generative AI and other ML techniques, they can adapt to new data patterns over time. This is also a key part of how to create AI insurance claim system with fraud detection features that can respond to evolving fraud behavior.
These tools operate at the orchestration layer. They define how claims move across stages, trigger actions based on conditions, and manage task execution. This ensures that claims follow a consistent path through the system without manual coordination.
This layer supports system execution. It includes cloud platforms, storage systems, and deployment environments that allow the system to run reliably, scale with demand, and handle large claim volumes. It also supports monitoring, logging, and updates.
Each technology layer performs a fixed function in the pipeline. Data is extracted, evaluated, routed, and processed using defined components without duplication across stages. As organizations continue developing AI insurance processing system, the focus is on selecting technologies that fit clearly into this flow and support consistent system behavior at scale.
Portfolio Spotlight
Insurance AI is an AI-powered assistant designed to support insurance agents through training, query resolution, and workflow guidance. Built to improve operational efficiency and knowledge access, it reflects how AI can structure decision support systems, a key layer when building scalable insurance claim automation platforms.
Data in an AI insurance claim system is not just an input layer, it directly determines how accurately the system can extract, validate, and decide on claims. To develop an AI automated system for insurance claim, data must be available in forms that support both rule-based evaluation and model-driven analysis across different stages of the workflow.
Insurance claim systems operate on two distinct data layers, and both are required together.
|
Data Type |
Examples |
Role in the System |
|---|---|---|
|
Structured Data |
Policy records, claim history, customer details |
Used for validation, rule checks, and decision logic |
|
Unstructured Data |
Invoices, reports, images, claim descriptions |
Used for data extraction and context understanding |
In most real-world setups, unstructured data dominates the intake stage. This is why systems focus heavily on developing AI insurance automation system with document processing, where raw inputs must be converted into structured fields before any logic can be applied.
AI models do not interpret raw data without guidance. They require labeled examples to learn patterns. Typical labeling workflow:
This process is usually handled in controlled environments within a custom software development company, where domain knowledge is applied to ensure labels match real claim behavior.
Data issues are one of the most common reasons for system failure. These issues are not always visible until the system starts making inconsistent decisions.
Common problems → corresponding fixes:
Instead of fixing issues after processing, systems are designed to detect and correct them early in the pipeline.
Data in insurance systems keeps changing. New claim types, new fraud patterns, and new document formats require the system to adapt. Rather than a one-time setup, the system follows an update cycle:
This continuous loop is a key focus area for companies that develop AI insurance claim automation systems, where maintaining model relevance is as important as initial deployment.
Data in an AI insurance claim system flows through multiple stages, from raw inputs to structured outputs and then into decision logic. As organizations continue developing AI insurance automation system with document processing, the priority is to ensure that data remains usable, consistent, and aligned with how the system processes claims at scale.
Use AI-driven workflows to create AI insurance claim processing software that improves speed, accuracy, and fraud detection.
See What AI Can Do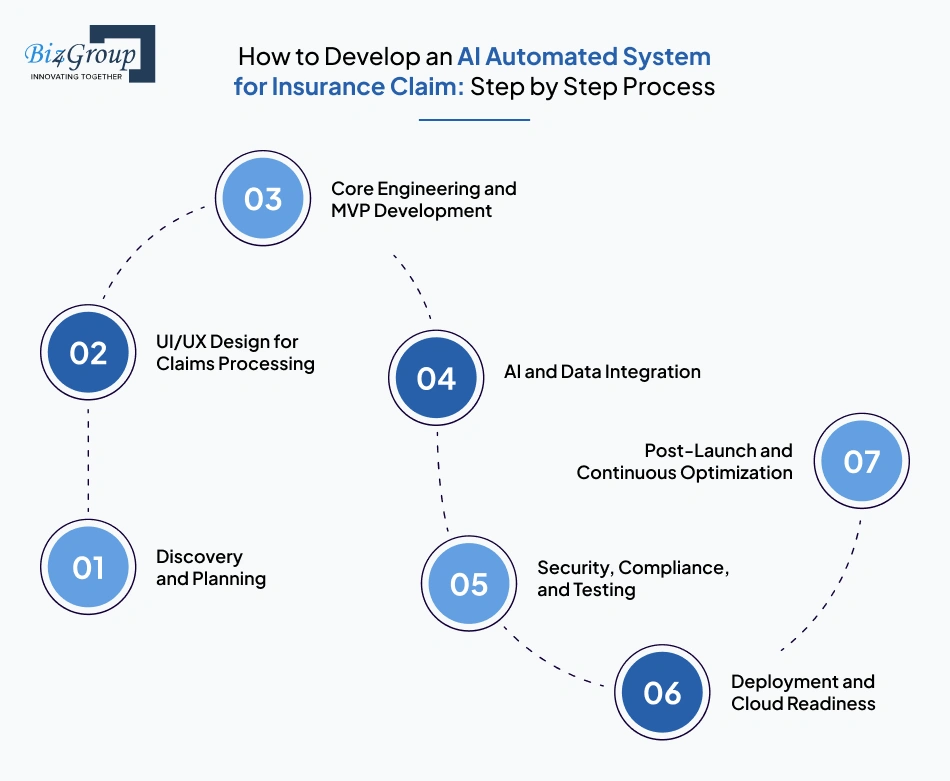
The development process for an AI insurance claim system defines how claim data, decision logic, and workflows are built and connected in a structured sequence. To develop an AI automated system for insurance claim, each step must prepare the system for the next, ensuring controlled implementation and measurable outcomes.
The first step focuses on identifying gaps in your existing claims workflow, such as delays in verification, inconsistent decisions, and manual dependencies. This stage defines the scope for the development of AI automated system for insurance claim based on actual operational inefficiencies.
At this stage, the focus shifts to designing interfaces that support how claims teams interact with the system daily. A well-structured UI/UX design is essential when teams build AI insurance claim automation system, as it directly impacts processing speed, usability, and adoption across stakeholders.
Also read: Top UI/UX design companies in USA
This step focuses on building a minimum viable system that handles core claim processing functions without overengineering. Teams typically start MVP development services to create AI insurance claim processing software, ensuring early validation before adding advanced automation and intelligence layers.
Also read: Top 12+ MVP Development Companies to Launch Your Startup in 2026
Once the core system is functional, AI models and data pipelines are integrated to improve decision-making and automation depth. This stage is central to insurance claim automation software development, where system performance depends on how well data flows into models and decision logic.
At this stage, the system is prepared for real-world use by ensuring it meets security standards and regulatory requirements. Insurance claims involve sensitive data, so the system must be tested for reliability, compliance, and handling of complex claim scenarios.
Also Read: 15+ Software Testing Companies in USA in 2026
This step focuses on making the system operational under real claim volumes and conditions. The infrastructure must support scaling, monitoring, and stability, especially during peak claim periods such as disasters or high-frequency claim events.
After deployment, the system must continuously adapt to changing claim patterns and operational requirements. Organizations that invest in development of AI automated system for insurance claim treat this phase as ongoing, focusing on improving accuracy, efficiency, and system reliability over time.
This step-by-step approach ensures that the system is built in layers, where each stage adds a defined capability without disrupting existing workflows. It reduces implementation risk by validating core functions early and scaling only after data, models, and workflows are aligned.
The decision to develop an AI automated system for insurance claim is typically triggered when claim volumes, processing delays, or error rates exceed what manual or rule-based systems can handle consistently. It is less about timing and more about whether your current system can maintain speed, accuracy, and control under real claim workloads.
The need for automation becomes clear when operational inefficiencies start affecting claim outcomes.
These patterns indicate that the system is no longer scaling effectively and requires AI automated system development for insurance claim to standardize processing.
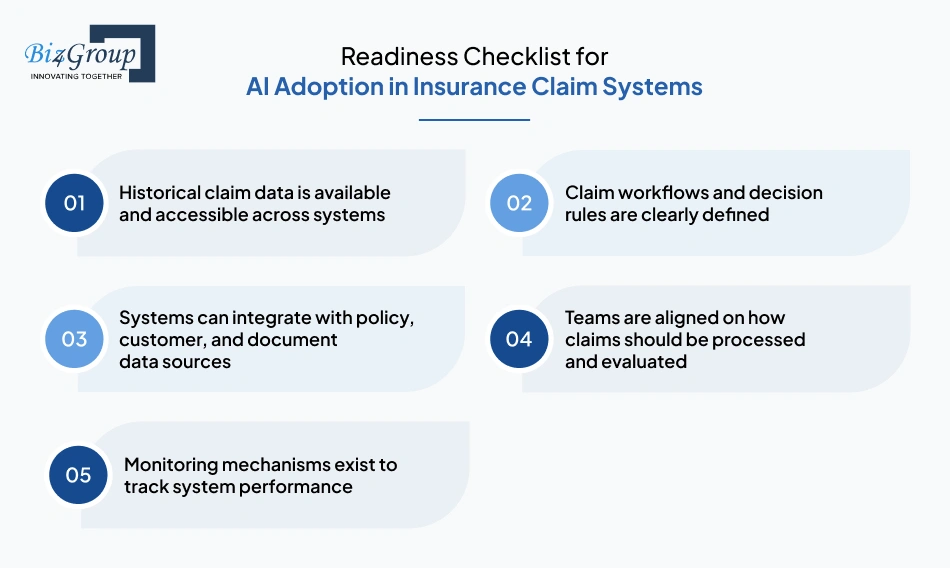
Before implementing automation, it is important to confirm whether your system can support AI-driven processing. Readiness indicators:
If these conditions are not met, automation may introduce inconsistencies instead of reducing them. Many organizations address this gap by choosing to hire AI developers who can align system design with existing workflows.
The choice between MVP and full-scale rollout depends on how stable your data and workflows are.
|
Approach |
When to Choose |
Outcome |
|---|---|---|
|
MVP (Minimum Viable Product) |
When workflows are partially defined or data quality is inconsistent |
Validates document processing, validation logic, and routing before scaling |
|
Full-Scale Rollout |
When workflows, integrations, and data pipelines are stable |
Enables end-to-end automation across all claim stages |
Decision rule:
Start with an MVP if there is uncertainty in data quality or workflow definition. Move to full-scale rollout only when claim processing logic is stable and repeatable.
Organizations following AI insurance claims management system development often rely on AI automation services to accelerate implementation while maintaining control over system behavior and scalability.
This decision should be based on measurable operational limits rather than assumptions. When claim volume, variability, and processing delays exceed system capacity, automation becomes necessary to maintain consistent decision-making and processing speed.
Adopt AI automated system development for insurance claim with modular architecture and real-time processing capabilities.
Plan Your System ArchitectureThe build vs buy decision determines whether your organization should rely on existing tools or develop an AI automated system for insurance claim tailored to its workflows. This choice depends on how much control you need over claim data, decision logic, and system integration.
|
Approach |
When It Makes Sense |
Key Considerations |
|---|---|---|
|
Off-the-Shelf Solutions |
Suitable when claim workflows are standardized and require limited customization |
Faster deployment, lower upfront cost, but limited control over data handling and decision logic |
|
Custom Development |
Required when workflows are complex, involve multiple systems, or need advanced fraud detection |
Full control over system behavior, higher cost, longer implementation time |
|
Hybrid Approach |
Useful when combining vendor tools with custom-built components for critical workflows |
Balances speed and flexibility, but requires careful integration and system coordination |
Organizations that need to develop AI claims processing system for insurance typically choose custom or hybrid approaches when claim handling involves multiple data sources, policy variations, and dynamic decision rules. In such cases, working with a software development company in Florida or similar partners helps ensure that system components are integrated correctly across workflows.
The decision is less about cost alone and more about how your system needs to operate over time. If claim workflows are expected to evolve, require integration with multiple systems, or depend on custom decision logic, organizations typically develop AI claims processing system for insurance to maintain control and scalability.
The cost to develop an AI automated system for insurance claim typically ranges from $30,000 to $200,000+, depending on system scope, data readiness, and level of automation. This is a ballpark figure, as costs vary based on whether you start with a limited MVP or build a full-scale enterprise system.
|
System Level |
What It Typically Includes |
Estimated Cost Range |
|---|---|---|
|
MVP-Level AI Insurance Claim Automation System |
Basic document upload and data extraction, rule-based validation, simple workflow routing, limited integrations |
$30,000 – $60,000 |
|
Advanced AI Insurance Claim Automation System |
Enhanced document processing, machine learning-based risk scoring, fraud detection, multi-step workflows, integration with core systems |
$60,000 – $120,000 |
|
Enterprise-Grade AI Insurance Claim Automation System |
End-to-end automation across claim lifecycle, advanced fraud detection, real-time processing, multiple integrations, scalability, compliance layers |
$120,000 – $200,000+ |
Costs increase as the system moves from handling basic claim validation to supporting complex workflows, multiple data sources, and real-time decision-making. The level of customization, integration with legacy systems, and accuracy requirements for AI models also play a significant role in overall investment.
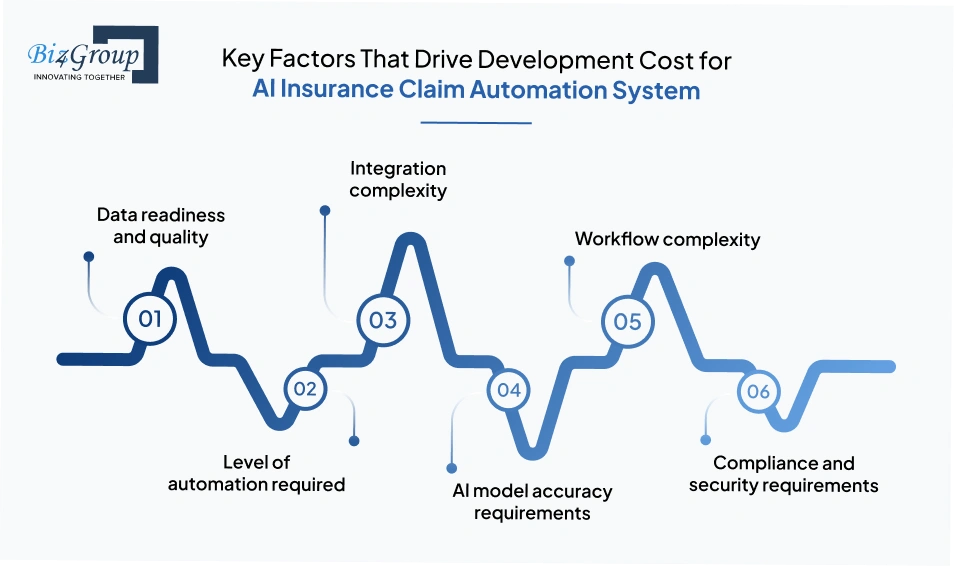
The overall cost of building an AI insurance claim system is influenced by several technical and operational factors. These directly affect development time, complexity, and long-term maintenance.
Systems with clean, structured, and labeled data require less preprocessing, while poor-quality or fragmented data increases effort significantly.
Automating only document processing is less expensive than building full claim lifecycle automation with decisioning and fraud detection.
Connecting with legacy policy systems, CRMs, and third-party services increases both development time and cost.
Higher accuracy for data extraction or fraud detection requires more training, validation, and tuning.
Multi-step workflows with conditional routing and exception handling increase system design and implementation effort.
Systems handling sensitive data may require additional layers for encryption, audit trails, and regulatory compliance.
Choosing the right level depends on how mature your claims process is and how much automation you need from the start, which often aligns closely with the challenges organizations face when implementing and scaling such systems.
Also Read: Insurance AI Chatbot Development Cost: Factors and Optimization Tips
Challenges in AI insurance claim systems arise when data, decision logic, and system integrations do not behave consistently under real claim conditions. When organizations develop an AI automated system for insurance claim, these challenges typically affect how accurately claims are processed, how quickly decisions are made, and how reliably systems scale.
|
Challenge Area |
What the Challenge Looks Like |
Why It Matters |
|---|---|---|
|
Data Quality and Availability Issues |
Missing fields, inconsistent document formats, and lack of labeled claim data across systems |
Leads to incorrect data extraction, unreliable model outputs, and increased manual intervention |
|
Regulatory and Compliance Constraints |
Strict rules around handling personal, financial, or medical claim data across regions |
Limits how data can be processed and requires additional validation, audit trails, and controls |
|
Model Accuracy and Edge Cases |
Difficulty handling rare claims, ambiguous documents, or incomplete inputs |
Forces more claims into manual review, reducing automation efficiency |
|
Legacy System Integration Complexity |
Integration with outdated policy or claims systems that lack modern APIs |
Creates delays in data flow and breaks end-to-end automation |
These challenges directly impact how the system performs in production. For example, poor data quality reduces model accuracy, while weak integrations slow down claim processing even if automation is in place. Teams working on custom AI automated system development for insurance claim often collaborate with top AI development companies in Florida to design systems that can handle inconsistent data and maintain stable integrations across workflows.
Handling these challenges effectively determines whether the system delivers consistent claim decisions or requires frequent manual correction. This is why system design, data readiness, and integration strategy are treated as core priorities.
Work with experts to develop AI claims processing system for insurance aligned with your workflows, data, and integrations.
Talk to Our AI ExpertsEvaluating vendors for AI insurance claim systems involves assessing their ability to handle real claim data, integrate with existing systems, and support decision logic across the claims lifecycle. When organizations develop an AI automated system for insurance claim, vendor capability directly affects system accuracy, scalability, and long-term maintainability.
The focus should be on how well the vendor can handle claim-specific workflows, not just general AI development.
Vendors involved in business app development using AI may offer broad capabilities, but their experience should be validated against insurance-specific use cases.

Questions should focus on how the system will behave under real claim conditions.
How do you handle incomplete, inconsistent, or conflicting claim data?
How will fraud detection and risk scoring models be trained and updated?
How will the system connect with existing policy and claims platforms?
How will the system perform during peak claim volumes?
How will updates be handled as claim patterns and regulations change?
Many decision-makers come with queries already explored in AI tools like ChatGPT or Perplexity, such as:
These questions help move the discussion from features to system behavior.
Certain signals indicate that a vendor may not be suited for insurance claim automation.
These issues often lead to systems that fail under real-world claim conditions, especially when teams try to build AI-powered insurance automation system without aligning system design to operational complexity.
Vendor evaluation should be based on how well the system will perform after deployment, not just how it is presented during selection. The right vendor is one that can translate claim workflows, data variability, and decision logic into a system that remains stable as claim volume and complexity increase.
Before organizations develop an AI automated system for insurance claim, they need to ensure that claim data, validation logic, and workflows are clearly defined and consistent. Without this alignment, automation may process claims faster but still produce inconsistent or incorrect outcomes.
The first priority is to establish a stable foundation where data and workflows behave predictably across different claim scenarios. At a practical level, this means:
Systems perform best when data extraction, validation, and fraud detection are aligned from the start.
Most implementation failures come from incorrect assumptions rather than technical limitations.
Automating the full claim lifecycle without validating individual components creates systems that fail under real claim conditions.
Claims often include incomplete data, conflicting inputs, or unusual scenarios that require flexible handling.
AI should support decision-making, while rule-based logic ensures consistency and compliance.
Using isolated tools, such as solutions from an AI chatbot development company, without integrating them into the full workflow results in fragmented processing.
Execution requires translating defined workflows into system behavior in a controlled sequence. A practical approach:
This is where organizations typically work with companies that develop AI insurance claim automation systems to move from defined workflows to stable system implementation.
Systems that scale successfully are built by aligning data, validation logic, and workflows before expanding automation. When these elements are defined early, the system can process claims consistently even as volume and complexity increase.
Accelerate outcomes with custom AI automated system development for insurance claim built for real-world claim conditions.
Get Started with AI AutomationMany decision-makers come with queries they have already explored in AI tools like ChatGPT or Perplexity, such as:
I need a company that can build custom AI insurance claim systems for enterprises
Choosing a partner to develop an AI automated system for insurance claim calls for experience in building systems that handle real insurance workflows, data variability, and decision logic at scale. Biz4Group’s portfolio reflects this through practical implementations, including AI-driven insurance platforms designed for agent support, training, and workflow optimization.
These implementations are not isolated features but parts of broader systems that mirror how claim processing environments operate in production.
What Sets Biz4Group LLC Apart
Biz4Group’s approach focuses on translating business processes into reliable AI systems that perform consistently under real claim conditions, instead of delivering isolated automation features.
Insurance claims are not slow because they are complex. They are slow because systems handling them are fragmented, manual, or not designed for variability. The shift toward automation is less about adding AI and more about restructuring how data, validation, and decisions flow across the system when organizations develop an AI automated system for insurance claim.
Organizations that build AI software for claims processing see the difference when extraction, validation, fraud detection, and workflows operate as a connected system rather than separate steps. That is where processing time drops, accuracy improves, and manual effort reduces without losing control.
The real advantage comes from building systems that can handle edge cases, scale with claim volume, and adapt as policies and regulations change. This is where working with an experienced AI app development company becomes critical, not for adding features, but for designing systems that actually hold up in production.
Looking to move from manual workflows to structured claim automation? Let’s map your current process and identify where AI can make an immediate impact.
The development timeline typically ranges from 4 to 6 months, depending on system complexity, data availability, and integration requirements. MVP-level systems can be built faster, while enterprise-grade platforms with full automation and compliance layers take longer to implement and stabilize.
AI systems can handle a wide range of claims, including health insurance claims, auto accident claims, property damage claims, and travel insurance claims. The level of automation depends on how structured the data is and how clearly validation rules are defined.
AI systems use a combination of data validation rules, pattern recognition, and fallback workflows to handle incomplete or inconsistent data. In many cases, such claims are flagged for manual review, ensuring that automation does not compromise accuracy or compliance.
Yes, AI systems can be updated to reflect policy changes through rule updates, retraining of models, and workflow adjustments. Continuous monitoring and retraining ensure that the system remains aligned with evolving business rules and regulatory requirements.
The cost typically ranges between $30,000 and $200,000+, depending on the scope of automation, system complexity, and integration needs. Basic systems cost less, while enterprise-grade platforms with advanced features such as fraud detection and real-time processing require higher investment.
AI systems improve accuracy by combining structured data extraction, rule-based validation, and machine learning models. Decisions are often supported by confidence scores and validation layers, with uncertain cases routed for human review to maintain reliability.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.