Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Are claim denials and coding inefficiencies quietly draining your revenue even when your team is doing everything right?
If you are running a hospital or clinic, this probably feels familiar. And if you are planning to develop an AI medical coding automation system, you are likely already questioning how long your current process can keep up.
Your team is working hard. Yet claims still get delayed, reworked, or rejected. You fix one bottleneck, another appears. We've seen this happen when manual workflows hit their limit.
So what's really causing the gap?
According to a report, the market for AI in medical coding is expected to grow from $2.86 billion in 2025 to $8.62 billion by 2033, driven by rising administrative burden and the need for better revenue cycle efficiency.
That is why more organizations are moving toward AI medical coding automation system development and adopting AI medical coding software to improve accuracy and reduce manual workload.
But before you move forward, one thing matters most.
Do you clearly understand what an AI medical coding automation system actually is and how it works in a real healthcare setup?
An AI medical coding automation system converts clinical documentation into standardized medical codes such as ICD, CPT, and HCPCS without relying entirely on manual effort. It reads patient records, physician notes, and discharge summaries using AI models, then identifies the right codes based on context, medical terminology, and historical patterns.
Instead of coders reviewing everything line by line, the system assists or automates large parts of the process while keeping human validation where needed.
This is what AI medical coding automation system development is focused on today. Not just automation, but accuracy, speed, and scalability across the revenue cycle. If you are planning to develop AI medical coding automation system solutions for healthcare, this is the shift you are aiming for.
Now the real question is, why are healthcare leaders prioritizing this so aggressively?
Here's what is driving adoption:
Many organizations are combining this with systems like AI medical billing software to streamline the entire billing and claims process, not just coding.
Whether you want to build an AI medical coding automation system for hospitals or make an AI medical coding automation system for clinics, the goal remains the same. Reduce dependency on manual workflows and create a system that keeps up with growing demand.
So now that you know what it is and why it matters, the next step is understanding how it actually works in a real-world setup.
Let’s help you develop an AI medical coding automation system that actually improves accuracy and revenue.
Let’s Talk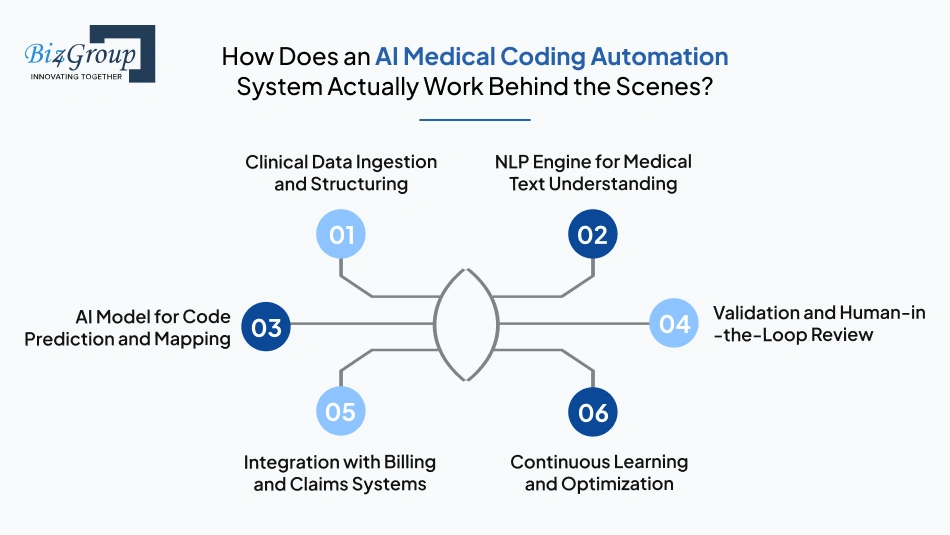
When you develop an AI medical coding automation system, you are building more than just a coding tool. You are creating a system that can read clinical data, understand medical context, assign accurate codes, and connect directly with your revenue cycle workflows.
If you are planning to develop AI coding automation system solution for healthcare, understanding this flow is critical before you start building.
Let's break it down step by step.
Every system starts with data coming from multiple sources like EHRs, EMRs, physician notes, and lab reports. This data is usually unstructured and inconsistent. The first step is to clean, standardize, and structure this data so the system can process it correctly. Without this, even the best models will fail.
Once the data is structured, the system uses NLP to interpret clinical language. Medical documentation is complex, and the system must understand both terminology and context. This layer ensures that the system knows the difference between similar terms and identifies what actually matters for coding.
This is where the system assigns codes. The AI model analyzes extracted data and predicts the correct ICD, CPT, or HCPCS codes. Most systems use a hybrid approach combining machine learning, rules, and sometimes LLMs to improve accuracy. This is essential when you build an AI medical coding automation system for hospitals where complexity is higher.
No system should operate without validation. Even advanced models need oversight, especially in healthcare where compliance matters. This layer ensures that uncertain or complex cases are reviewed before submission. It also helps improve the system over time.
Once codes are finalized, they need to move into billing and claims workflows without friction. Integration is what turns coding into real revenue impact. This step ensures your system works seamlessly with billing platforms and reduces delays in claim submission.
A strong system improves over time. As it processes more data and receives feedback, it becomes more accurate and efficient. This is especially important when you create an AI coding automation system for healthcare providers that need to scale across departments or locations.
This is how you develop an AI healthcare coding automation system that works reliably in real-world environments, not just in theory.
So now that you understand how the system works, the next question is just as important.
How do you build this while staying compliant with strict healthcare regulations?
When you develop an AI medical coding automation system, compliance is not something you handle later. It has to be built into the system from day one. If you are planning AI medical coding automation system solution development, missing even one regulatory requirement can lead to claim rejections, penalties, or data security risks.
So, what exactly do you need to focus on?
Any system handling patient data must follow strict HIPAA requirements. This means protecting sensitive health information at every stage, from data ingestion to storage and processing. You need to ensure encryption, secure access controls, and audit mechanisms are in place. It is not just about avoiding breaches, but about building trust with patients and providers.
This is why most organizations prioritize building HIPAA compliant systems that ensure data privacy and security are maintained across the entire workflow.
Your system must follow standardized coding frameworks like ICD-10, CPT, and HCPCS. These are not optional. They directly impact claim approval and reimbursement. Beyond that, payer-specific rules and CMS guidelines must also be considered. If your system does not align with these standards, even accurate codes can result in denied claims.
When you develop AI medical coding automation system solutions for healthcare, keeping these standards updated and embedded in the system is critical.
Healthcare systems require transparency. Every coding decision made by your system should be traceable and explainable. This means maintaining detailed logs of how codes were generated, what data was used, and whether any manual changes were made.
Explainability is especially important when audits happen. It helps your team justify coding decisions and reduces compliance risks.
Your system must work seamlessly with existing healthcare infrastructure like EHRs, billing systems, and payer platforms. Standards like HL7 and FHIR ensure that data can move across systems without loss or misinterpretation. Without proper interoperability, even a well-built system can fail in real-world use.
If you are planning to build an AI medical coding automation system for hospitals, this becomes even more critical due to multiple systems and departments involved.
Compliance is not a one-time setup. Regulations, coding standards, and payer rules change frequently. Your system must be designed to adapt to these changes without requiring major rework. Regular updates, monitoring, and validation processes are essential to keep the system aligned with current requirements.
This is a key part of building enterprise AI medical coding automation system solutions development for healthcare that remain reliable over time.
If compliance is built correctly, your system becomes not just efficient, but trustworthy and scalable.
So what features actually make this system effective in real-world use?
When you develop an AI medical coding automation system, features are not just checkboxes. Each capability should directly improve accuracy, speed, or revenue cycle performance.
If you are planning AI medical coding automation system solution development, here are the features that truly make a difference in real-world healthcare environments.
|
Feature |
What It Does |
Why It Matters for Your Organization |
|---|---|---|
|
Clinical Data Processing Engine |
This layer collects and organizes data from EHRs, EMRs, physician notes, discharge summaries, and lab reports. It converts unstructured and inconsistent clinical data into a structured format that AI models can process. |
Without clean and structured data, your system cannot function reliably. This ensures your automation works with real-world healthcare data instead of breaking due to inconsistencies. |
|
Advanced NLP for Medical Context |
The NLP engine reads clinical text and understands medical terminology, relationships, and intent. It can differentiate between similar terms, identify conditions, and capture context like severity or timing. |
Medical language is complex. This feature ensures your system interprets records correctly, which directly impacts coding accuracy and reduces errors. |
|
Automated Code Assignment (ICD, CPT, HCPCS) |
Based on extracted data, the system assigns or suggests appropriate medical codes using trained AI models and predefined logic. It can handle large volumes of records quickly and consistently. |
This is where most of the time is saved. It reduces manual coding effort and speeds up the entire process without compromising consistency. |
|
After assigning codes, the system verifies them against coding standards, payer rules, and historical patterns to detect mismatches or errors before submission. |
Helps prevent incorrect coding that leads to denials, rework, or compliance issues, improving overall claim quality. |
|
|
Human-in-the-Loop Review System |
The system allows coders to review AI-generated outputs, especially in complex or low-confidence cases. It combines automation with human expertise for better accuracy. |
Maintains control and compliance while gradually building trust in the system. It also helps train the model over time. |
|
Real-Time Error Detection |
Identifies missing data, incorrect mappings, or inconsistencies during the coding process rather than after submission. |
Fixing issues early reduces costly rework and speeds up claim processing timelines. |
|
Integration with Billing & Claims Systems |
Connects coding outputs directly with billing platforms and claim processing systems to ensure seamless data flow across the revenue cycle. |
Eliminates manual handoffs and delays, improving end-to-end efficiency, especially when integrated with AI medical claim systems. |
|
Denial Prediction and Prevention |
Uses historical claim data and patterns to identify high-risk claims that are likely to be denied before submission. |
Allows your team to fix issues proactively, improving approval rates and reducing revenue leakage. |
|
Audit Trail and Compliance Tracking |
Records every action, decision, and modification made by the system or user, including how codes were generated. |
Essential for audits, compliance checks, and maintaining transparency in coding decisions. |
|
Custom Rule Engine for Payers |
Applies specific payer guidelines, coding rules, and contract terms automatically during code assignment and validation. |
Ensures higher claim acceptance rates across different insurance providers with varying requirements. |
|
Scalability for Multi-Facility Operations |
Designed to handle large volumes of data across multiple hospitals, clinics, or departments without performance issues. |
Critical if you want to build an AI medical coding automation system for hospitals or expand across healthcare networks. |
|
Analytics and Performance Dashboard |
Provides insights into coding accuracy, turnaround time, denial trends, and operational performance through dashboards and reports. |
Helps you track ROI and identify areas for improvement, often powered by AI healthcare analytics software. |
|
Continuous Learning and Model Improvement |
The system improves over time by learning from corrections, feedback, and new data inputs. It adapts to changing coding standards and workflows. |
Ensures long-term value and scalability, especially when enhanced with capabilities like agentic AI in healthcare. |
These features define whether you simply create AI medical coding automation system solutions or build something that actually delivers measurable results.
So now that you know what features matter, the next step is understanding how to actually build this system step by step without wasting time or budget.
We’ll map out a custom AI medical coding automation system solution tailored to your workflows.
Get a Custom Strategy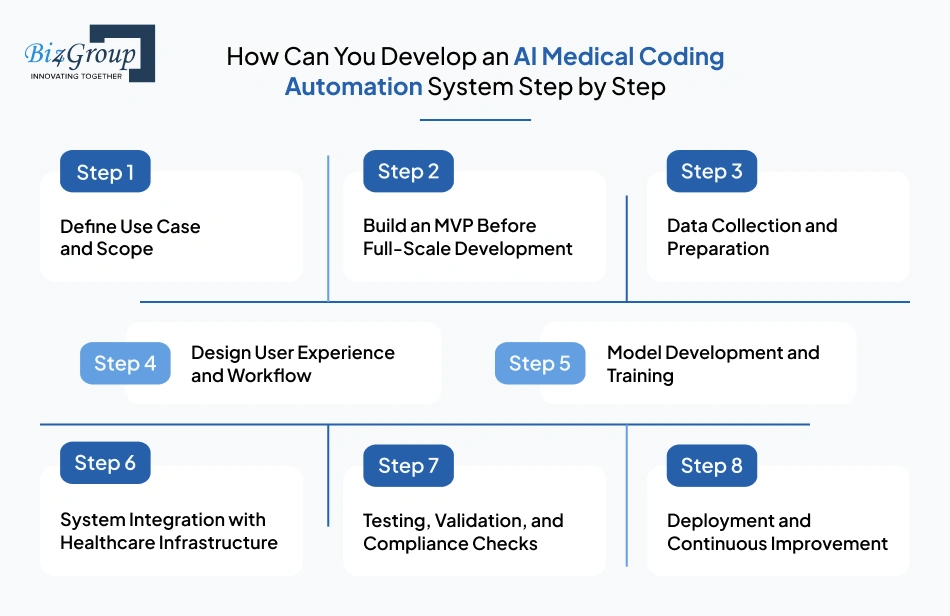
When you develop an AI medical coding automation system, the biggest mistake teams make is jumping straight into development without a clear structure.
If you want to develop AI coding automation system solution for healthcare or even build AI medical billing automation system solutions, you need a step-by-step approach that aligns with your workflows, data, and long-term goals.
Let's break it down.
Start by identifying exactly where you want automation. Are you trying to build an AI medical coding automation system for hospitals, or are you looking to make an AI medical coding automation system for clinics? Each setup has different needs, data complexity, and compliance requirements. Clarity at this stage prevents rework later and helps you prioritize the right features.
Instead of building everything at once, start with a focused version of your system. This allows you to test functionality, validate assumptions, and reduce risk early. A structured approach to MVP development is critical when you create AI medical coding automation system solutions that need to scale later.
Your system is only as good as the data it learns from. You need high-quality, labeled clinical data to train and validate your models. This step is essential if you want to develop an AI healthcare coding automation system that performs accurately in real-world scenarios.
Even the best system fails if users struggle to adopt it. Coders and billing teams need a clear, intuitive interface that fits into their daily workflow. Investing in UI/UX design becomes important when you create an AI coding automation system for healthcare providers that people actually use.
This is where your AI models are built and trained using prepared data. The goal is to accurately map clinical input to correct medical codes. A strong foundation here is key if you are planning enterprise AI medical coding automation system solutions development for healthcare.
Your system must connect with existing tools like EHRs, billing platforms, and claim systems. Without integration, even a strong model cannot deliver value. This step becomes critical when you make an AI medical coding automation system for revenue cycle management and need seamless data flow.
Before deployment, you need to test your system across different scenarios. This includes accuracy testing, workflow validation, and compliance checks. This ensures you are building a reliable AI medical coding automation system for hospitals development and other healthcare setups.
Once deployed, your system should not remain static. It needs to evolve based on feedback, new data, and changing regulations. Many organizations choose to hire AI developers when they develop an AI medical coding automation system to ensure continuous improvement and scalability.
This is how you develop an AI medical coding automation system that is scalable, compliant, and aligned with real healthcare workflows.
Now that you understand the process, the next question is just as important.
What technology stack do you actually need to build this system efficiently?
When you develop an AI medical coding automation system, choosing the right tech stack is not just a technical decision. It directly impacts scalability, performance, compliance, and long-term maintenance. If you are planning enterprise AI medical coding automation system development for healthcare, your stack should support large data volumes, real-time processing, and seamless integrations.
Here's a practical breakdown of the tech stack you actually need:
|
Layer |
Technologies / Tools |
Why It Matters |
|---|---|---|
|
Frontend (User Interface) |
React, Next.js, Angular, Vue.js |
Provides dashboards for coders and billing teams. A clean interface improves usability and adoption, especially when supported by strong design principles. |
|
Backend (Application Logic) |
Manages workflows, APIs, and system logic, ensuring smooth coordination between different modules. |
|
|
AI/ML & NLP Layer |
Python, TensorFlow, PyTorch, spaCy, Hugging Face |
Powers clinical text understanding and code prediction, forming the core of AI medical coding automation system development. |
|
Data Processing & Storage |
PostgreSQL, MongoDB, Apache Kafka, Snowflake |
Handles structured and unstructured healthcare data efficiently, which is essential when you develop an AI healthcare coding automation system. |
|
Cloud & Infrastructure |
AWS, Microsoft Azure, Google Cloud |
Enables scalability, security, and high availability for enterprise deployments, often as part of enterprise AI solutions. |
|
Integration Layer (APIs & Standards) |
HL7, FHIR APIs, REST APIs |
Ensures seamless connectivity with EHRs, billing systems, and third-party platforms when you develop AI coding automation system solution for healthcare. |
|
Security & Compliance Layer |
OAuth 2.0, JWT, encryption protocols |
Protects sensitive patient data and ensures compliance with healthcare regulations. |
|
Analytics & Monitoring Tools |
Power BI, Tableau, ELK Stack |
Provides insights into system performance, accuracy, and operational efficiency. |
|
DevOps & Deployment |
Docker, Kubernetes, CI/CD pipelines |
Supports continuous deployment, scalability, and system stability for large healthcare environments. |
A well-structured tech stack ensures your system is reliable, scalable, and ready for real-world healthcare demands.
Now that you understand the technology behind it, the next question becomes critical.
How much does it actually cost to develop an AI medical coding automation system?
Also Read: React JS Development Services
If you are planning to develop an AI medical coding automation system, one of the first questions that comes up is cost.
In most cases, the cost to develop an AI medical coding automation system range between $30,000 to $250,000+, depending on the scope, complexity, and level of automation you are aiming for. A basic system with limited features will sit on the lower end, while a fully scalable, enterprise-grade platform with advanced AI capabilities will require a significantly higher investment.
If you are exploring AI medical coding automation system development, understanding where the cost of implementing AI in healthcare and cost comes from helps you plan better and avoid overspending.
When you build AI medical billing automation system solutions or coding platforms, each feature contributes differently to the overall cost.
|
Feature / Component |
Estimated Cost Range |
Why It Impacts Cost |
|---|---|---|
|
Clinical Data Processing |
$5,000 – $20,000 |
Requires handling large volumes of structured and unstructured healthcare data. |
|
NLP & Medical Text Understanding |
$10,000 – $40,000 |
Complex to train models that understand medical terminology and context. |
|
Automated Code Assignment Engine |
$15,000 – $50,000 |
Core functionality that requires accurate mapping of clinical data to codes. |
|
AI Model Training & Fine-Tuning |
$20,000 – $70,000 |
Depends on data quality, model complexity, and training cycles. |
|
Human-in-the-Loop System |
$5,000 – $15,000 |
Adds validation layers and user interaction features. |
|
Integration with EHR & Billing Systems |
$10,000 – $30,000 |
Requires API development and interoperability standards like HL7/FHIR. |
|
Compliance & Security Layer |
$8,000 – $25,000 |
Includes encryption, access control, and audit mechanisms. |
|
Analytics Dashboard |
$5,000 – $20,000 |
Tracks performance metrics, coding accuracy, and operational insights. |
|
Cloud Infrastructure & Deployment |
$5,000 – $25,000 |
Covers hosting, storage, and scalability setup. |
The cost of AI medical coding automation system solution development is not fixed. It varies based on several critical factors.
A simple assistive tool costs much less than a full-scale system that automates end-to-end coding and integrates with multiple systems.
If your data is unstructured or requires heavy cleaning and annotation, the cost increases significantly.
Basic rule-based systems are cheaper, while advanced AI models with NLP and continuous learning require more investment.
The more systems you need to connect, such as EHRs, billing platforms, and claims systems, the higher the development cost.
Healthcare systems require strict compliance, which adds additional layers of development effort and cost.
Many organizations underestimate the hidden costs involved in developing AI medical coding automation system solutions for healthcare.
Cleaning and labeling healthcare data takes time, resources, and domain expertise.
AI models require continuous updates to maintain accuracy and adapt to new coding standards.
As usage grows, cloud and storage costs increase, especially for real-time processing systems.
Your team needs training to adopt the new system, which adds indirect costs.
You can control costs effectively if you approach development strategically.
Build a focused version first, validate it, and then scale. This reduces initial investment and risk.
Leverage existing AI models instead of building everything from scratch to save time and cost.
Focus on features that directly improve accuracy and revenue cycle performance first.
Working with an experienced AI automation services provider helps you avoid costly mistakes and accelerate development.
Understanding the cost structure helps you make smarter decisions when you develop an AI medical coding automation system and ensures you invest in the right areas.
Now that you have clarity on cost, the next question is just as important.
What challenges should you expect, and how can you solve them effectively?
Get a clear estimate to develop an AI medical coding automation system based on your exact needs.
Request Cost Breakdown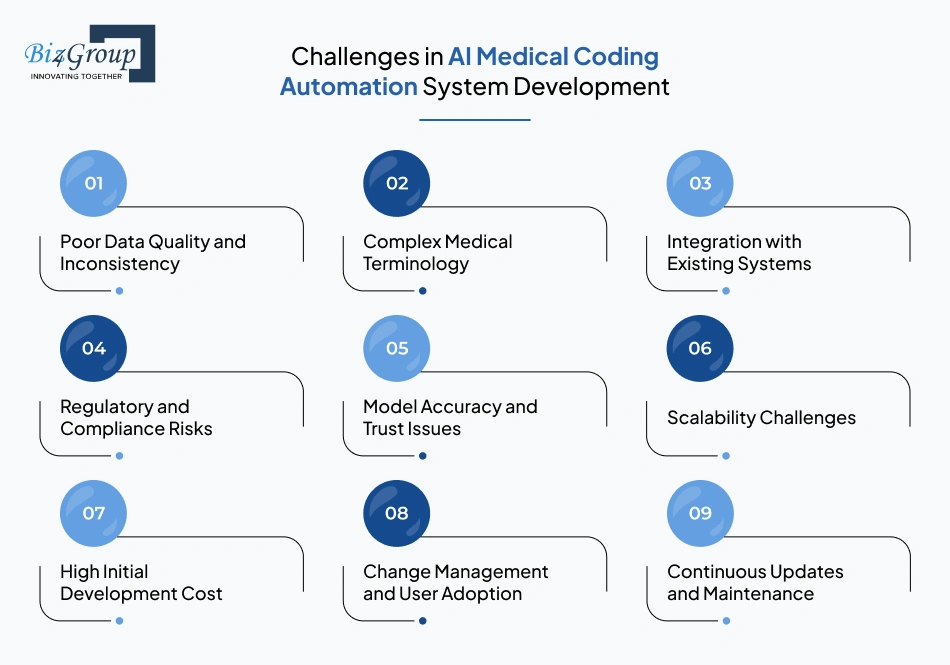
When you develop an AI medical coding automation system, challenges are not just technical. They impact accuracy, compliance, adoption, and ultimately your revenue cycle.
If you are planning AI medical coding automation system solution development, understanding these challenges early helps you avoid delays, cost overruns, and performance issues.
Here's a practical breakdown of the most common challenges and how to solve them:
|
Challenge |
What It Means in Real Scenarios |
How to Solve It Effectively |
|---|---|---|
|
Poor Data Quality and Inconsistency |
Clinical data from EHRs is often incomplete, unstructured, or inconsistent across departments. This leads to inaccurate model outputs. |
Invest in strong data preprocessing, normalization, and validation pipelines before model training. |
|
Complex Medical Terminology |
Medical language varies by provider, specialty, and documentation style, making it difficult for AI models to interpret correctly. |
Use advanced NLP models trained on healthcare-specific datasets and continuously refine them with real-world data. |
|
Integration with Existing Systems |
Connecting with EHRs, billing systems, and claims platforms can be complex and time-consuming. |
Use standardized APIs (HL7, FHIR) and consider expert-led AI integration services to ensure smooth connectivity. |
|
Regulatory and Compliance Risks |
Failure to meet healthcare regulations can result in penalties, claim denials, or data breaches. |
Build compliance into the system from the start, including audit trails, encryption, and access controls. |
|
Model Accuracy and Trust Issues |
Teams may hesitate to rely on AI if outputs are inconsistent or unclear. |
Implement human-in-the-loop validation and explainability features to build trust gradually. |
|
Scalability Challenges |
Systems that work for small datasets may fail when scaled across multiple hospitals or departments. |
Design cloud-based, scalable architecture that can handle large volumes of data efficiently. |
|
High Initial Development Cost |
Building a full-scale system requires significant upfront investment. |
Start with a custom MVP software approach and scale gradually to manage costs effectively. |
|
Change Management and User Adoption |
Coders and staff may resist switching from manual processes to automated systems. |
Provide proper training, intuitive interfaces, and gradual onboarding to improve adoption. |
|
Continuous Updates and Maintenance |
Coding standards, payer rules, and regulations change frequently. |
Set up continuous monitoring and update mechanisms to keep the system aligned with current requirements. |
These challenges determine whether you successfully create AI medical coding automation system solutions or struggle with delays and inefficiencies.
By addressing them early, you can develop an AI medical coding automation system that is accurate, scalable, and ready for real-world healthcare demands.
So now the final question is, should you build this system in-house, or partner with the right team to accelerate development?
When you decide to develop an AI medical coding automation system, the outcome depends heavily on who builds it. The right partner helps you move faster, avoid costly mistakes, and build something that actually works in real healthcare environments.
Biz4Group stands out among the top AI healthcare software development companies in USA by focusing on practical, scalable solutions rather than generic implementations.
As an experienced AI development company, the team understands both the technical and operational challenges involved in AI medical coding automation system development, from data handling to compliance and system integration.
What makes the difference is their end-to-end approach to healthcare software product development, ensuring your system is not just built, but aligned with your workflows, users, and long-term goals.
If you are looking to develop an AI medical coding automation system that delivers accuracy, scalability, and real impact on your revenue cycle, working with the right team makes all the difference.
Partner with a team that knows how to develop AI medical coding automation system solutions for healthcare the right way.
Start Your ProjectBuilding the right system is no longer optional if you want to stay competitive in today's healthcare environment. When you develop an AI medical coding automation system, you are not just improving coding speed. You are strengthening accuracy, reducing revenue leakage, and creating a more predictable revenue cycle.
The difference comes down to execution. A well-planned approach to AI medical coding automation system development ensures your system integrates smoothly, stays compliant, and delivers measurable results from day one.
This is where experience matters. With deep expertise in healthcare AI and real-world implementation, Biz4Group has helped organizations move from fragmented workflows to scalable, intelligent systems powered by enterprise AI medical coding automation system solutions development for healthcare.
Whether you are starting from scratch or modernizing existing systems, partnering with a proven AI healthcare software development company ensures your solution is built for long-term success.
And if your goal is to go beyond coding and improve overall operations, integrating systems like AI hospital management software can further streamline workflows across departments.
The next step is simple. Contact Biz4Group and turn your coding process into a competitive advantage.
To build an AI medical coding automation system, you need access to high-quality clinical data, NLP and machine learning models, integration capabilities with EHR and billing systems, and a compliance-ready infrastructure. You also need domain expertise to ensure accurate coding and alignment with healthcare regulations.
The timeline to develop an AI medical coding automation system depends on complexity. A basic MVP can take 2 to 4 weeks, while a full-scale enterprise solution may take 6 to 8 weeks or more, especially if it includes integrations, compliance layers, and advanced AI models.
To develop an AI medical coding automation system for your hospital, start by defining your use case, collecting structured clinical data, building an MVP, and integrating it with your existing systems. Partnering with experienced teams helps accelerate development and ensures compliance with healthcare standards.
You can work with an experienced healthcare-focused AI team or the best company to develop an AI medical coding automation system for healthcare that understands both technical and regulatory requirements. This ensures your solution is scalable, compliant, and aligned with your workflows.
To create a scalable AI medical coding automation system for healthcare organizations, you need cloud-based infrastructure, modular architecture, continuous model training, and strong integration capabilities. Scalability also depends on how well your system handles increasing data volume and multi-location operations.
If your goal is how to make AI medical coding automation system for revenue cycle optimization, focus on features like automated coding, error detection, denial prediction, and seamless billing integration. These directly improve claim accuracy and reduce delays in reimbursement.
Building an enterprise AI automation system for medical coding helps reduce manual workload, improve coding accuracy, minimize claim denials, and speed up reimbursements. It also provides better visibility into performance metrics and supports long-term scalability across healthcare operations.
The cost to develop an AI medical coding automation system typically ranges between $30,000 to $250,000+, depending on the system's complexity, features, integrations, and compliance requirements. A basic solution with limited automation will cost less, while an enterprise-grade system with advanced AI, real-time processing, and multi-system integration will require a higher investment.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.