Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Is your healthcare organization unknowingly losing revenue to fraud that traditional systems fail to detect?
Healthcare fraud goes far beyond basic billing mistakes. Today, it involves complex schemes that are difficult to identify using manual reviews or rule-based tools alone. This is where AI healthcare fraud detection systems are making a real difference by uncovering hidden patterns, detecting anomalies in real time, and helping organizations prevent financial losses before they escalate.
Many healthcare leaders are now asking, I want to build an AI system to detect healthcare fraud, which companies can help me develop it? The answer lies in combining advanced AI capabilities with deep healthcare expertise to create systems that are both accurate and scalable.
Organizations planning to develop AI healthcare fraud detection software need to think beyond automation. The goal is to build systems that can learn from historical claims data, adjust to emerging fraud tactics, and deliver meaningful insights that teams can act on quickly. At the same time, there is a growing need for developing scalable AI solutions for healthcare fraud prevention, especially as data volumes continue to expand across hospitals, insurers, and public healthcare systems.
From insurance providers to healthcare startups, businesses are actively investing in the end-to-end development of AI healthcare fraud detection software to improve efficiency, reduce losses, and meet regulatory expectations. This blog is created for healthcare decision-makers, CTOs, product leaders, and founders who want a clear, practical roadmap to building effective AI-driven fraud detection systems, including architecture, development steps, costs, and key challenges.
AI healthcare fraud detection software is a system that uses artificial intelligence and machine learning to identify suspicious activities in healthcare data.
It analyzes large datasets such as insurance claims, billing records, prescriptions, and patient histories to detect patterns that may indicate fraud.
Unlike traditional rule-based systems, AI systems continuously learn and improve, making them more effective in detecting new and evolving fraud tactics.
Healthcare systems in 2026 are handling massive volumes of digital data, making fraud harder to track using traditional methods. This shift has made AI healthcare fraud detection a critical investment for insurers, hospitals, and government programs aiming to reduce losses and improve operational control.
AI is changing the way fraud is identified by moving from reactive audits to proactive monitoring. Instead of reviewing claims after payments are made, AI systems analyze transactions in real time and flag suspicious activities instantly. This approach helps organizations prevent fraud before financial damage occurs.
Healthcare data is complex and often unstructured, including clinical notes, billing codes, and patient histories. By leveraging AI to help detect fraud in medical datasets, organizations can uncover patterns that are difficult for humans to identify. AI models can connect data points across multiple systems, revealing hidden relationships and unusual behaviors.
Manual fraud detection processes are time-consuming and prone to errors. With AI for healthcare fraud detection, organizations benefit from faster analysis and higher accuracy. Machine learning models can process thousands of claims within seconds and continuously improve as they learn from new data.
As healthcare organizations grow, so does the complexity of their data. Healthcare fraud detection software development integrating AI allows systems to scale efficiently without increasing manual workload. These solutions adapt to new fraud patterns and maintain performance even as data volumes increase.
In 2026, organizations that adopt AI-driven fraud detection are better positioned to protect revenue, improve trust, and operate more efficiently in a data-driven healthcare ecosystem.
A well-structured architecture is the foundation of any successful fraud detection platform. When organizations aim to create AI-powered fraud detection solutions for healthcare, they need a system that can handle large datasets, process information quickly, and generate accurate insights in real time.
The architecture of an AI-driven fraud detection system is typically designed in multiple layers, each responsible for a specific function.
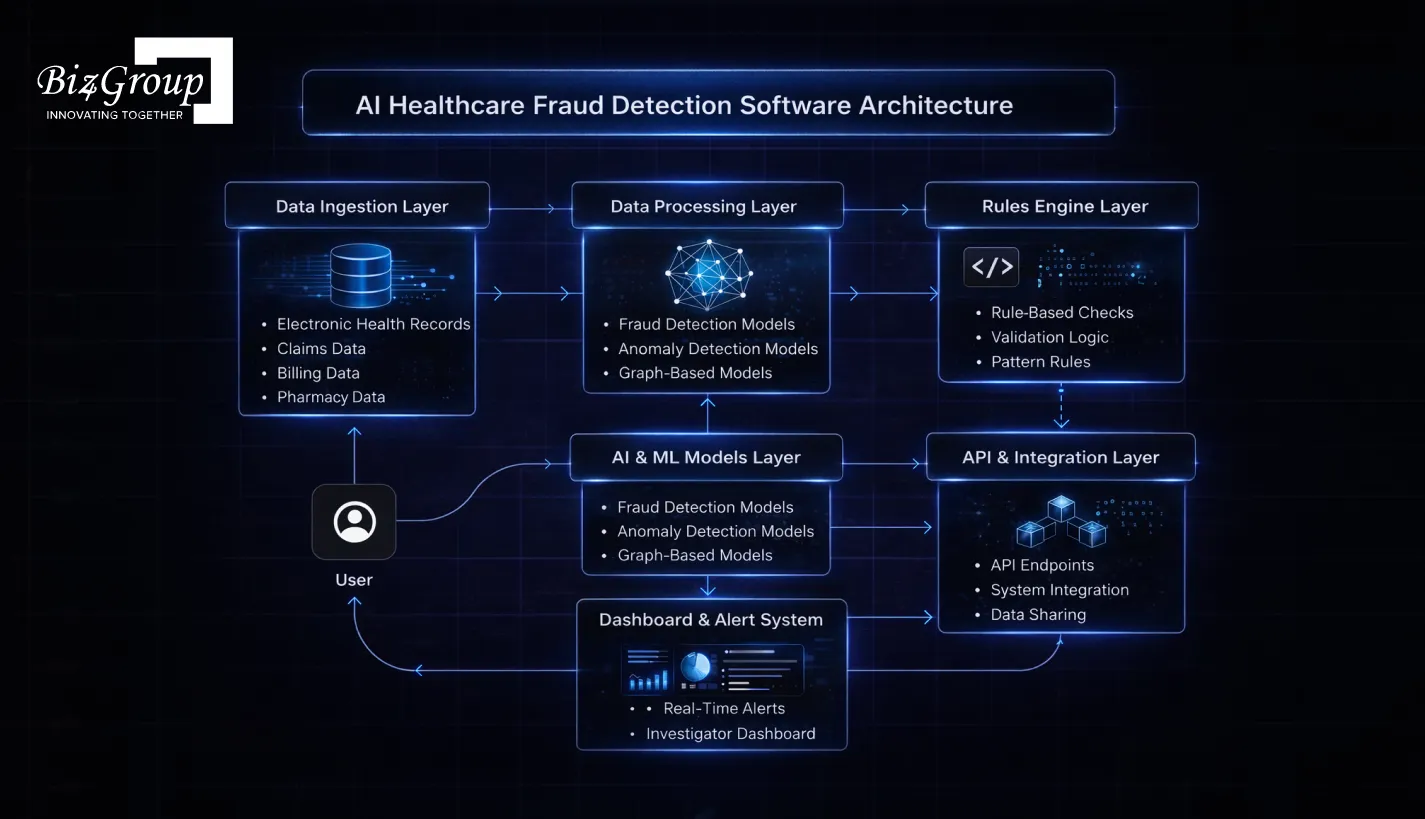
This layer collects data from multiple healthcare sources such as:
The goal is to centralize all relevant data so the system can analyze it effectively.
Raw healthcare data is often inconsistent and unstructured. This layer cleans, transforms, and organizes the data into a usable format.
Key tasks include:
This step is critical while developing an AI healthcare fraud detection software, as data quality directly impacts model performance.
This is the core intelligence layer where fraud detection happens. Organizations that want to build intelligent fraud detection systems for hospitals and insurers rely heavily on this component.
It includes:
These models continuously learn from new data and improve over time.
Alongside AI models, a rules engine applies predefined conditions such as:
This hybrid approach improves detection accuracy and reduces false positives.
This layer connects the fraud detection system with existing healthcare infrastructure.
It enables:
The final layer presents insights in a user-friendly way.
Features include:
This ensures that decision-makers can act quickly on suspicious activities.
A robust architecture is essential to successfully create scalable and efficient fraud detection systems for healthcare. By combining data processing, AI models, and seamless integrations, organizations can build solutions that not only detect fraud accurately but also adapt to evolving healthcare challenges.
Turn your idea into a scalable AI healthcare fraud detection solution with expert guidance.
Get StartedHealthcare organizations are not investing in AI fraud detection just for innovation. The decision is driven by real financial pressure, rising fraud complexity, and the need to operate efficiently at scale. In 2026, this shift is becoming a strategic priority across insurers, hospitals, and even investors.
The numbers clearly show why companies are actively investing in this space:
These numbers are not just growth indicators. They reflect a strong shift toward investing in AI-driven systems to combat fraud at scale.
Fraud in healthcare is not a minor issue. Governments and insurers are losing billions every year.
This level of loss is forcing organizations to invest in smarter detection systems that can identify fraud early rather than relying on post-claim audits.
Traditional systems often detect fraud after payments are processed. That approach leads to financial recovery challenges.
Companies are investing in AI because it enables:
This is one of the strongest reasons behind investing in AI for healthcare fraud detection, especially for large insurers handling millions of claims daily.
Manual fraud investigation teams require time, resources, and domain expertise. AI helps automate a large portion of this process.
Organizations investing in AI systems are seeing:
This makes healthcare fraud detection software development integrating AI a cost-saving strategy, not just a technology upgrade.
Fraudsters are using advanced techniques, including automation and synthetic identities. Static rule-based systems struggle to keep up.
AI systems help by:
This is a key reason why companies are actively investing in intelligent fraud detection platform development instead of relying on legacy systems.
If you are thinking, "I am planning to invest in startups developing AI solutions for detecting fraud in healthcare claims and billing", you are aligned with current market trends.
Recent developments show clear investor confidence:
This indicates that venture capital and enterprises are both investing in this space to capture future growth.
Healthcare systems must comply with strict regulations related to billing transparency and fraud prevention.
AI helps organizations:
This makes investing in AI fraud detection for healthcare system development not optional, but necessary for long-term sustainability.
Companies that invest early in AI-driven fraud detection gain:
This creates a clear competitive edge, especially in insurance and large healthcare networks.
From the rising financial losses and growing fraud complexity to strong market growth and investor interest, these factors clearly show why healthcare companies are investing in the development of AI fraud detection software as a strategic necessity.
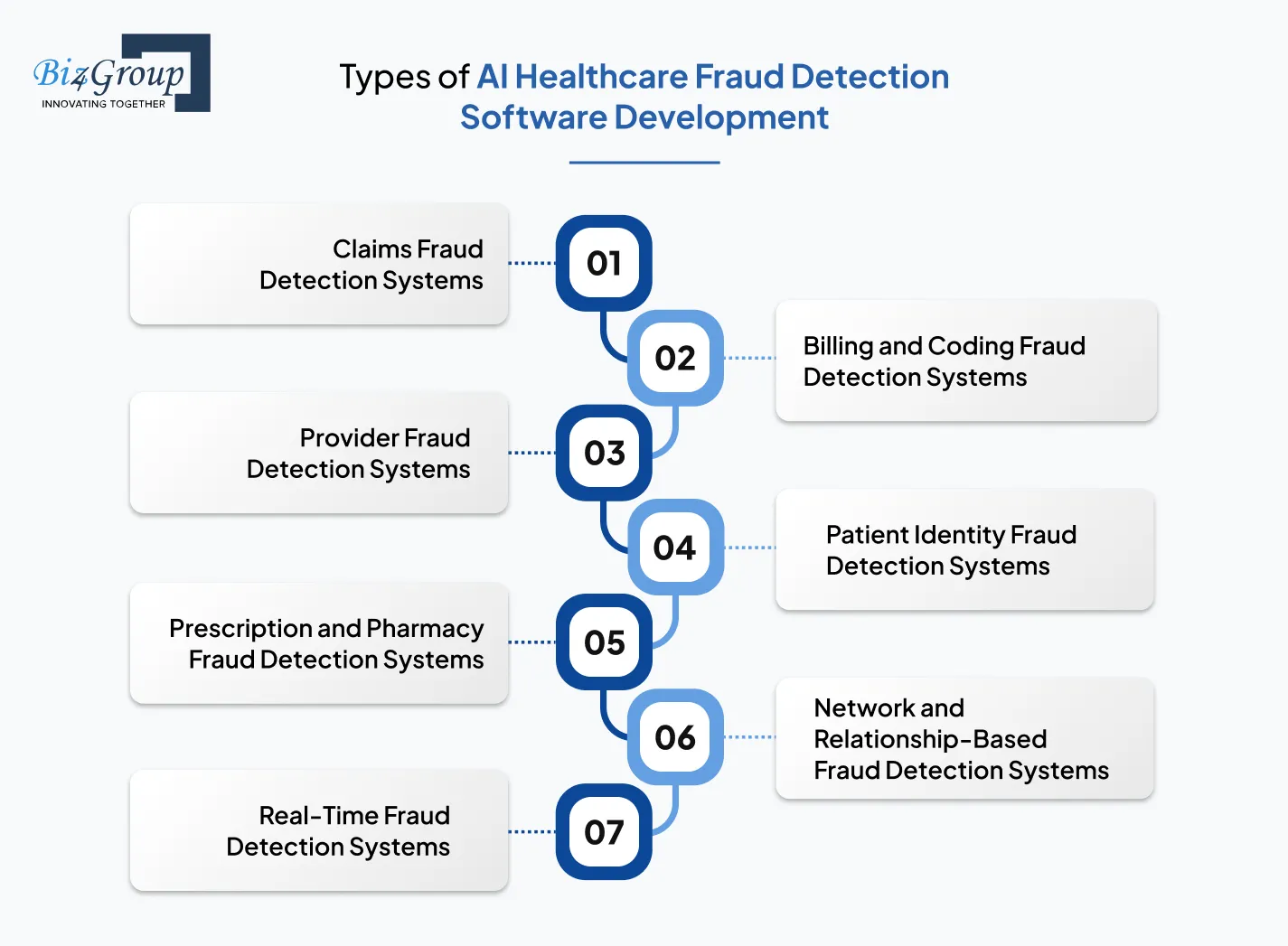
When organizations start exploring fraud prevention, they often realize there is no one-size-fits-all solution. The type of system you choose depends on your data, business model, and fraud risks. If you are looking to build an end-to-end AI healthcare fraud detection system, understanding the different types of solutions is the first step.
This is the most widely used type of solution in healthcare.
Claims fraud detection systems focus on analyzing insurance claims to identify:
When developing an AI-based healthcare fraud detection platform, this module often becomes the core component. It uses historical claims data to detect unusual patterns and flag suspicious submissions in real time.
These systems are heavily used by:
Healthcare billing involves complex coding standards such as ICD and CPT codes. Fraud often happens when codes are manipulated to increase reimbursements.
This type of system helps in:
Organizations that aim to build a secure and compliant AI solution for healthcare fraud detection prioritize this system to ensure accuracy and regulatory compliance.
Not all fraud comes from patients. In many cases, providers may engage in suspicious practices.
This system focuses on:
When building AI-driven healthcare fraud detection systems, this layer helps create a more comprehensive view of fraud risks across the ecosystem.
Identity theft is becoming a serious concern in healthcare. Fraudsters may use stolen identities to claim medical services or prescriptions.
This system helps:
It is essential for organizations developing AI-based healthcare fraud detection platforms that handle large patient databases.
Prescription fraud includes fake prescriptions, drug abuse, and illegal distribution of medications.
This type of system focuses on:
Pharmacy chains and insurers often rely on this as part of a broader fraud detection strategy.
Fraud is often organized and involves multiple entities working together.
These systems use graph-based AI models to:
If you are planning to build intelligent fraud detection systems for hospitals and insurers, this advanced capability adds significant value.
Traditional systems detect fraud after claims are processed. Real-time systems work differently.
They:
Organizations looking to build an end-to-end AI healthcare fraud detection system
Choosing the right combination of these systems is essential when defining the types of AI healthcare fraud detection software you develop, as each layer strengthens your overall fraud prevention strategy.
AI models are the core engine behind any fraud detection system. They help create systems that can identify hidden patterns, predict suspicious behavior, and continuously improve with new data. When businesses plan to make intelligent fraud detection capabilities, selecting the right combination of models becomes essential.
Below are the key AI models commonly used to build effective healthcare fraud detection systems.
Supervised learning is widely used to create fraud detection systems when labeled data is available.
These models are trained on past examples of fraudulent and legitimate claims to make future predictions.
Common techniques include:
They help:
This approach is useful when organizations want to create reliable prediction systems using historical datasets.
In many cases, fraud data is not labeled. This is where unsupervised learning helps build smarter systems.
These models focus on identifying anomalies or unusual behavior without prior labels.
Common techniques include:
They help:
Businesses often use this approach to make systems that can catch fraud patterns that have never been seen before.
Deep learning helps create more advanced fraud detection systems that can process large and complex datasets.
These models use neural networks to:
Examples include:
They are especially useful when working with large-scale healthcare systems and complex fraud scenarios.
Healthcare data is not always structured. Clinical notes, prescriptions, and reports contain valuable information in text format.
Natural Language Processing helps make sense of this unstructured data.
It is used to:
This is important for organizations that want to create more comprehensive fraud detection systems beyond structured data.
Fraud often involves multiple entities working together. Graph-based models help uncover these hidden relationships.
These models create networks of:
They help:
Businesses that aim to make advanced fraud detection platforms often include graph-based intelligence to strengthen their systems.
No single model can solve all fraud detection challenges. Hybrid models combine multiple techniques to improve accuracy and coverage.
A hybrid system may include:
This approach helps create balanced systems that reduce false positives and improve detection performance.
Building an effective AI fraud detection system for healthcare requires combining multiple AI models to create a solution that is accurate, scalable, and capable of adapting to evolving fraud patterns.
Also Read: How to Seamlessly Integrate AI Models into Development Workflow?
Get personalized insights on AI healthcare fraud detection software development for your business.
Book a ConsultationBuilding a strong fraud detection system is not just about adding AI models. It requires a clear understanding of the technical capabilities required for the development of AI healthcare fraud detection software. The right set of features ensures the system is accurate, scalable, and practical for real-world use.
Organizations that aim to develop a scalable AI-based fraud detection platform for healthcare organization must focus on features that support real-time processing, adaptability, and compliance.
Feature |
Description |
|---|---|
The system should analyze claims and transactions instantly as they are processed. This helps prevent fraudulent payouts instead of detecting them after the loss has already occurred. It improves response time and reduces financial risks. |
|
Anomaly Detection Engine |
This feature identifies unusual patterns in claims, billing, or patient behavior. It works even when fraud patterns are unknown, helping uncover new types of fraud. It is essential for proactive fraud prevention. |
Risk Scoring Mechanism |
Each transaction or claim is assigned a risk score based on predefined factors and AI predictions. This helps investigators prioritize high-risk cases. It improves decision-making efficiency. |
Machine Learning Model Integration |
The system should support multiple AI models working together. This allows better accuracy and adaptability. It also ensures the platform evolves as new data becomes available. |
Automated Alerts and Notifications |
Alerts should be triggered when suspicious activity is detected. These alerts must be timely and actionable. It helps teams respond quickly to potential fraud cases. |
Data Integration Capabilities |
The platform must connect with EHR systems, billing platforms, and third-party databases. This ensures a unified view of all data. It improves the quality of fraud detection. |
Scalable Data Processing |
The system should handle growing volumes of healthcare data without performance issues. This is critical for large hospitals and insurers. Scalability ensures long-term usability. |
Fraud Pattern Recognition |
The system should learn from past fraud cases and identify recurring patterns. This helps detect similar fraud attempts in the future. It strengthens predictive capabilities. |
User-Friendly Dashboard |
A clear dashboard helps investigators view alerts, reports, and insights easily. It should present complex data in a simple format. This improves usability and decision-making. |
Case Management System |
This feature allows teams to track, investigate, and resolve fraud cases. It organizes workflows and maintains records. It improves operational efficiency. |
Compliance and Audit Trails |
The system should maintain detailed logs of all activities and decisions. This supports regulatory compliance and auditing. It also increases transparency. |
Data Security and Encryption |
Sensitive healthcare data must be protected using strong encryption and access controls. This ensures patient privacy and data safety. It is critical for trust and compliance. |
APIs allow the system to communicate with external tools and platforms. This makes integration seamless. It also supports system expansion in the future. |
|
Continuous Learning and Model Updates |
The system should update its models regularly based on new data. This helps adapt to evolving fraud patterns. It ensures long-term effectiveness. |
Explainable AI Capabilities |
The system should provide clear reasons behind its decisions. This helps users trust the results. It is also important for regulatory and audit purposes. |
The right combination of these features ensures you can develop a scalable, secure, and intelligent fraud detection system that delivers real value in real-world healthcare environments.
Also Read: How to Outsource AI Healthcare Software Development: A Complete Strategy Guide
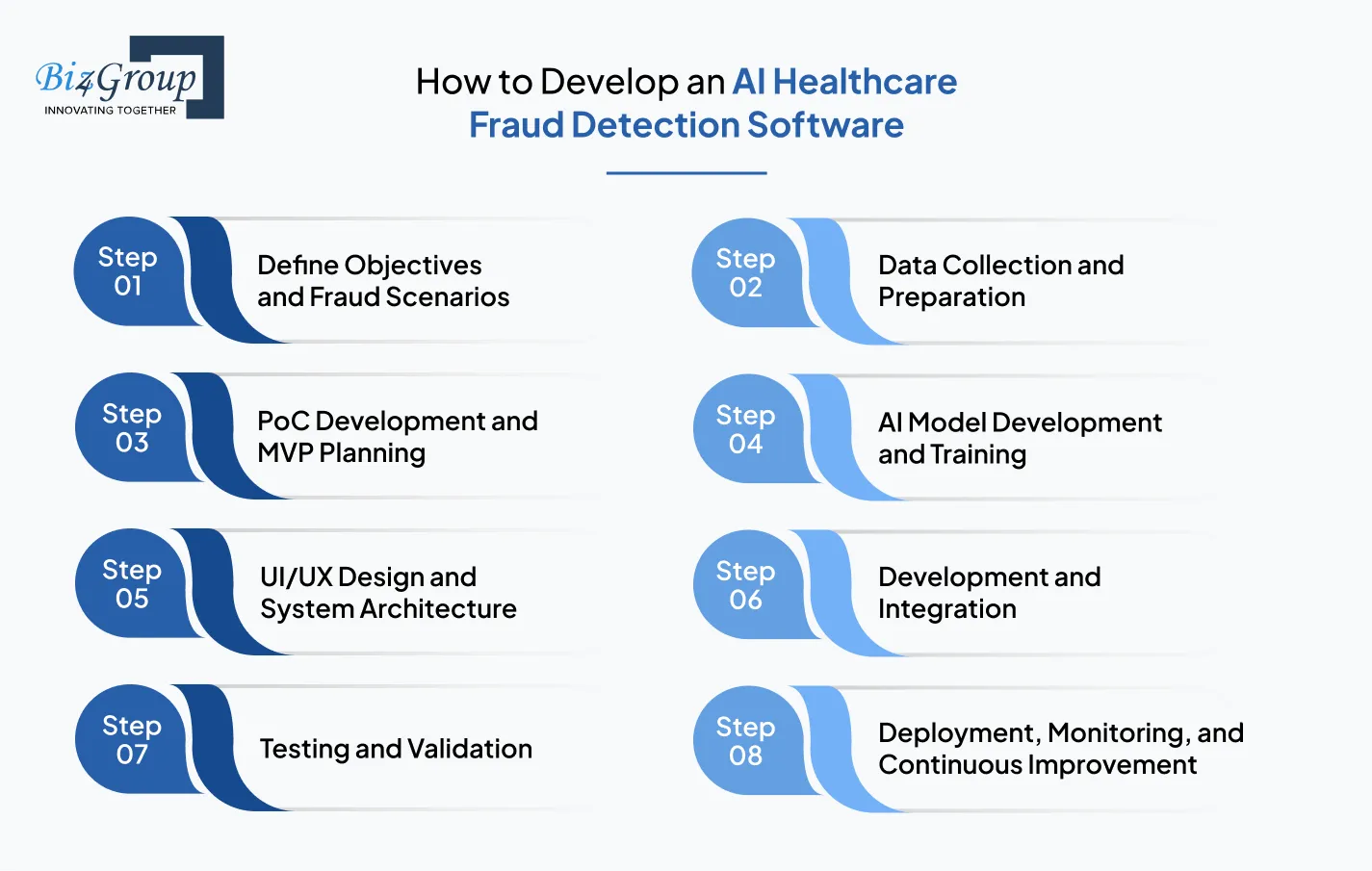
Building a fraud detection system requires more than just training a model. It involves a structured approach that combines data, design, engineering, and compliance. If you are thinking, we are looking to develop an AI healthcare fraud detection system for our healthcare platform, this step-by-step process will give you a clear roadmap.
The development process of AI healthcare fraud detection software focuses on creating scalable, accurate, and secure systems that can handle real-world healthcare complexity.
The first step in building an AI healthcare fraud detection software is to clearly define the problem space and expected outcomes. This includes identifying the types of fraud you want to detect such as duplicate claims, phantom billing, identity misuse, or upcoding. It is also important to understand who will use the system, whether it is insurers, hospitals, or internal compliance teams.
You should map out key workflows, data touchpoints, and business rules early on. This stage often involves collaboration between domain experts, analysts, and stakeholders to ensure that nothing critical is missed. A clear definition at this stage reduces confusion later and sets realistic expectations.
Goal of this step:
To establish a strong foundation by aligning business needs with technical direction, ensuring your approach to AI for healthcare fraud is focused, measurable, and aligned with real-world use cases.
Data plays a central role in determining how effective your system will be. Collecting data from multiple sources such as claims systems, EHRs, billing platforms, and pharmacy records is essential. However, raw data is often messy and inconsistent, so it needs to be cleaned and structured before use.
This step includes removing duplicates, handling missing values, standardizing formats, and labeling data where possible. Data enrichment techniques can also be applied to improve quality. Since fraud cases are often rare, addressing data imbalance is another critical task.
Strong data preparation helps you create automated fraud detection systems for healthcare that are reliable and capable of identifying subtle patterns.
Goal of this step:
To build a high-quality, structured dataset that supports accurate AI model development and improves the overall performance of fraud detection models.
Before committing to full-scale development, it is practical to validate your idea through PoC development. A Proof of Concept helps test whether your selected approach can actually detect fraud using real or sample data. It allows teams to experiment with models, features, and workflows in a controlled environment.
Once the PoC shows promising results, the next step is to move toward MVP development services. The MVP focuses on building a simplified version of the system with essential features such as basic fraud detection, alerts, and dashboards. This version can be tested with real users to gather feedback.
This stage helps refine your strategy and ensures that resources are used efficiently.
Goal of this step:
To validate feasibility early, reduce development risks, and create a clear roadmap for scaling the solution.
Also Read: Top 12+ MVP Development Companies to Launch Your Startup
This is where the intelligence of the system is built. During this phase, teams focus on selecting appropriate algorithms, engineering features, and training models using prepared data. Depending on the use case, supervised, unsupervised, or hybrid models can be used.
Advanced approaches such as agentic AI in healthcare can also be explored to enable systems that adapt and make decisions dynamically. Continuous experimentation is required to improve model accuracy and reduce false positives.
The models should also be tested against real-world scenarios to ensure they perform well under different conditions.
Goal of this step:
To develop accurate, adaptive, and scalable models that can detect fraud patterns effectively and evolve with changing data.
A powerful backend system is not enough if users cannot interact with it easily. This is where collaboration with a UI/UX design company becomes valuable. The goal is to design intuitive dashboards, clear visualizations, and smooth workflows that help investigators and analysts take action quickly.
At the same time, system architecture needs to be designed carefully. This includes defining data pipelines, selecting cloud infrastructure, and planning integrations with existing healthcare systems.
A well-planned architecture ensures smooth performance when implementing AI in healthcare environments and supports future scalability.
Goal of this step:
To create a user-friendly, scalable, and efficient system that balances technical performance with usability.
In this stage, the actual product is built based on the defined architecture and design. Development includes both frontend and backend components, along with APIs for seamless communication between systems.
Integration is a critical part of this step. The system must connect with hospital management systems, insurance platforms, and external data sources without disrupting existing workflows. This often requires careful planning and testing.
Partnering with top AI healthcare software development companies can help ensure high-quality implementation and faster delivery.
Goal of this step:
To build a fully functional system that integrates smoothly into existing healthcare infrastructure and supports real-time operations.
Testing ensures that the system performs reliably in different scenarios. This includes validating AI models, checking system performance, and ensuring data accuracy. Both functional and non-functional testing are important at this stage.
Testing also focuses on reducing false positives and ensuring that genuine claims are not incorrectly flagged. Security testing is equally important to protect sensitive healthcare data.
Working with top AI software testing companies can help identify hidden issues and improve overall system quality before launch.
Goal of this step:
To ensure the system is accurate, secure, and ready for deployment without performance or reliability issues.
Once testing is complete, the system is deployed in a production environment. This can be done on cloud platforms or on-premise infrastructure depending on business requirements.
After deployment, continuous monitoring is essential. The system should track performance metrics, detect drifts in model accuracy, and update models with new data regularly. Feedback from users should also be incorporated to improve usability and functionality.
This ongoing process ensures that your AI fraud detection software development services healthcare solution remains effective over time.
Goal of this step:
To maintain long-term performance, adapt to evolving fraud patterns, and continuously improve the system based on real-world usage.
A well-structured development process ensures that your AI healthcare fraud detection system is not only functional but also scalable, reliable, and ready to handle real-world fraud challenges effectively.
Also Read: AI Medical Claim Processing Software Development: Cost, Technology Stack & Roadmap
One of the most common questions businesses ask is, what is the cost to build AI healthcare fraud detection software? The answer depends on several factors such as system complexity, data volume, integrations, and the level of AI capabilities required.
On average, the cost of building an AI healthcare fraud detection software ranges between $40,000 to $300,000+.
The overall AI healthcare fraud detection software development cost can vary significantly depending on business needs and technical requirements.
For a more detailed breakdown and cost estimation, explore our dedicated guide on AI healthcare fraud detection software development cost.
Also Read: How Much Does It Cost to Develop AI Healthcare App
When planning a fraud detection system, one of the most common questions is, Can you recommend firms that create AI solutions for detecting medical billing fraud? The answer often depends on the technologies they use and their ability to build scalable, secure systems.
The tools required to build AI healthcare fraud detection system play a critical role in performance, accuracy, and long-term scalability. Choosing the right frameworks to create AI healthcare fraud detection platform ensures that your system can process large datasets, integrate with healthcare systems, and adapt to evolving fraud patterns.
Technology Layer |
Tools / Technologies |
Description |
|---|---|---|
Programming Languages |
Python, R |
Python is widely used for AI model development due to its extensive libraries and community support. R is useful for statistical analysis and data modeling, especially in research-heavy environments. |
AI/ML Frameworks |
TensorFlow, PyTorch, Scikit-learn |
These frameworks enable developers to build, train, and deploy machine learning models. They support various algorithms needed for classification, anomaly detection, and predictive analytics. |
Data Processing Tools |
Apache Spark, Hadoop |
These tools handle large-scale healthcare data efficiently. They allow distributed processing, making it easier to manage and analyze massive datasets. |
Natural Language Processing |
NLTK, SpaCy, Hugging Face |
NLP tools are used to process unstructured data such as clinical notes and medical reports. They help extract meaningful insights for fraud detection. |
Database Management |
PostgreSQL, MongoDB |
These databases store structured and unstructured data securely. They support fast queries and are essential for managing healthcare records. |
Cloud Platforms |
AWS, Microsoft Azure, Google Cloud |
Cloud platforms provide scalable infrastructure for deploying AI systems. They support storage, computing, and advanced AI services. |
REST APIs, GraphQL |
APIs enable seamless communication between fraud detection systems and existing healthcare platforms. They are critical for system integration. |
|
Visualization Tools |
Tableau, Power BI, custom dashboards |
These tools present fraud insights through dashboards and reports. They help stakeholders understand patterns and take action quickly. |
Security Tools |
SSL encryption, IAM, OAuth |
Security tools ensure data protection and compliance with healthcare regulations. They help safeguard sensitive patient and financial data. |
DevOps and Deployment |
Docker, Kubernetes, CI/CD pipelines |
These tools automate deployment, manage scalability, and ensure system reliability. They support continuous updates and efficient system management. |
A well-chosen tech stack lays the foundation for building a secure, scalable, and efficient AI healthcare fraud detection system that performs reliably in real-world environments.
Launch a secure and intelligent fraud detection system tailored to your healthcare needs.
Request a Proposal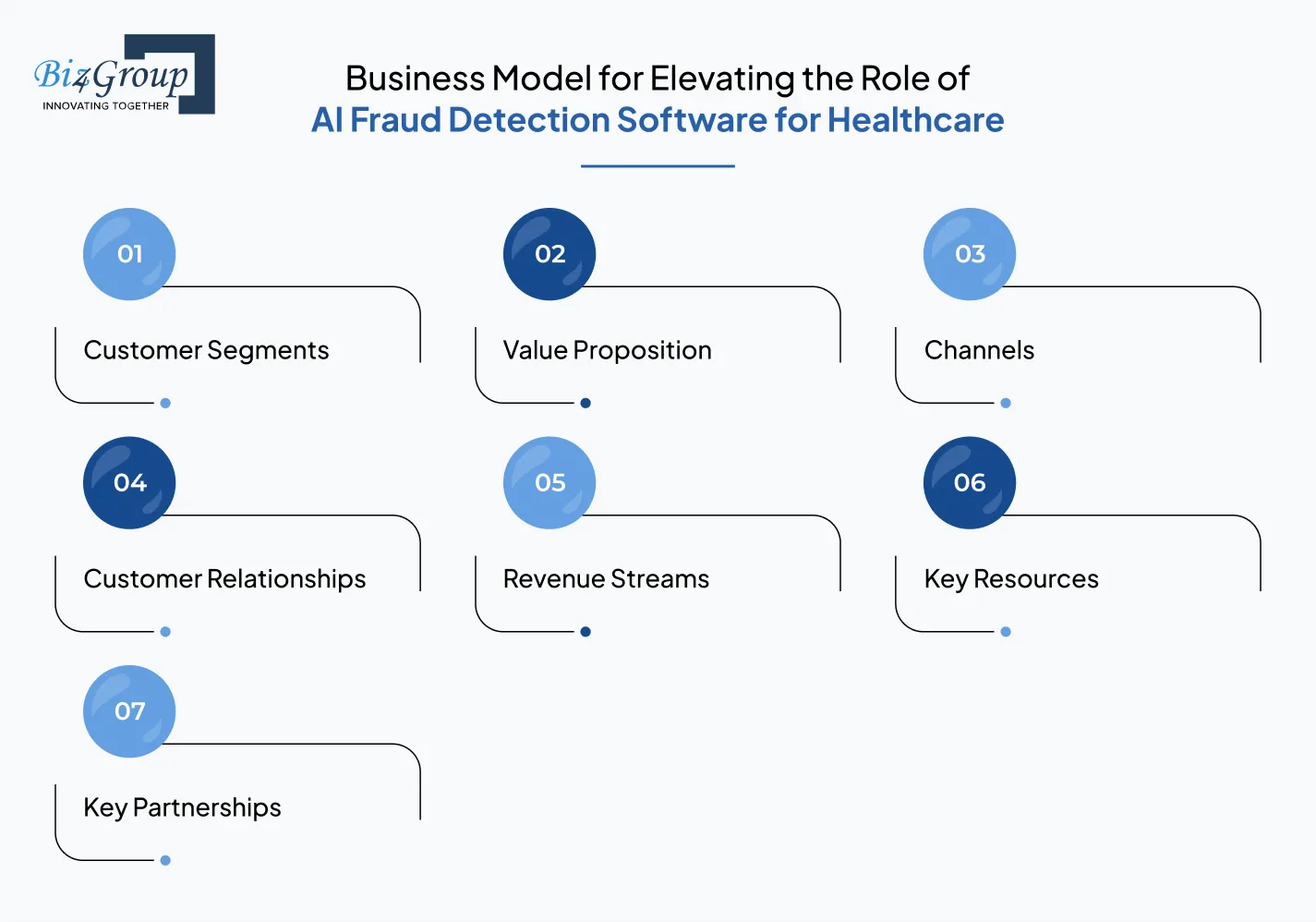
Building a successful AI healthcare fraud detection product is not just about technology. It also requires a strong business model that defines how value is created, delivered, and monetized. For companies offering AI fraud detection solutions in healthcare, a well-structured model helps scale adoption across insurers, hospitals, and healthtech platforms.
Below is a practical breakdown of the key components of a business model tailored for AI healthcare fraud detection software.
Identifying the right audience is the first step toward building a sustainable business.
Key customer segments include:
Each segment has different fraud detection needs, so solutions should be flexible and customizable.
The value proposition defines why customers should choose your solution.
Core offerings include:
Offer white-label solutions that allow enterprises to rebrand and use the platform as their own. This is especially useful for large insurers and SaaS providers who want to deliver fraud detection under their brand.
Provide APIs so developers can integrate fraud detection capabilities into their own systems. This approach supports ecosystem growth and allows faster adoption across multiple platforms.
Offer AI consulting services to help organizations implement, customize, and optimize fraud detection systems. This includes strategy, compliance guidance, and performance tuning.
Channels define how you reach and deliver value to customers.
Common channels include:
Maintaining strong relationships is critical for long-term success.
Approaches include:
A strong relationship builds trust and encourages long-term contracts.
Also View This Product: Customer Service AI Chatbot
Revenue models can vary depending on the target market.
Common revenue streams:
A combination of these models helps diversify income and improve profitability.
These are the essential assets required to deliver value.
Key resources include:
These resources ensure the system remains competitive and effective.
Partnerships play a major role in scaling the business.
Important partnerships include:
Strategic partnerships help expand reach and improve solution capabilities.
A well-defined business model ensures that AI healthcare fraud detection software not only delivers technical value but also achieves sustainable growth and market adoption.

When you think about developing AI-driven fraud detection in healthcare, it quickly becomes clear that the process involves more than just technology. There are practical challenges related to data, systems, compliance, and evolving fraud behavior. Addressing these challenges early helps in creating systems that actually perform well in real-world healthcare environments.
Healthcare data is often incomplete, inconsistent, and spread across multiple systems. Missing values, duplicate entries, and unstructured formats make it difficult to train accurate AI models. In many cases, different systems follow different standards, which creates additional complexity during data consolidation and analysis. Poor data quality directly impacts the accuracy of fraud detection results.
Solution:
Set up strong data preprocessing pipelines, standardize formats across systems, and enrich datasets wherever possible. Using reliable data sources and synthetic data can also improve model performance and consistency.
Fraud cases usually represent a very small portion of the total dataset, while legitimate transactions dominate. This imbalance makes it difficult for AI models to learn fraud patterns effectively. As a result, models may become biased toward predicting non-fraud cases, reducing their ability to detect actual fraud incidents in real-world scenarios.
Solution:
Apply techniques like oversampling minority classes, undersampling majority classes, and using anomaly detection models. Combining supervised and unsupervised learning approaches can also help improve detection performance.
Incorrectly flagging genuine claims as fraudulent can create operational challenges and frustration for both providers and patients. It may delay claim processing and reduce trust in the system among users. A high false positive rate can also increase the workload for investigation teams, making the system less efficient overall.
Solution:
Use multi-layer validation techniques such as risk scoring, threshold tuning, and combining AI models with rule-based logic. Continuous model refinement helps improve precision and reduce unnecessary alerts.
Fraudsters continuously adapt their techniques, making it difficult for static systems to remain effective over time. New fraud patterns may not match historical data, which reduces the effectiveness of traditional detection approaches. This creates a constant need for systems that can adapt and learn from new behaviors.
Solution:
Enable continuous model training using fresh data and implement adaptive learning techniques. Regular updates and monitoring ensure the system evolves alongside emerging fraud trends.
Many healthcare organizations still rely on legacy systems that were not designed to support modern AI technologies. Integrating new AI solutions with these systems can be complex and may disrupt existing workflows if not handled carefully. Data compatibility and system communication are often major concerns.
Solution:
Use APIs and middleware to bridge the gap between old and new systems. A phased integration approach helps minimize disruptions and ensures smooth system transitions.
Healthcare data is highly sensitive and subject to strict regulations such as HIPAA and GDPR. Ensuring compliance while developing and deploying AI systems can be challenging. Any failure in data protection can lead to serious legal and financial consequences.
Solution:
Incorporate compliance measures from the beginning. Use encryption, role-based access controls, and audit trails to ensure data security and meet regulatory requirements.
Many AI models operate as black boxes, making it difficult for stakeholders to understand how decisions are made. In healthcare, transparency is important for both compliance and trust. Without clear explanations, users may hesitate to rely on AI-driven decisions.
Solution:
Implement explainable AI techniques that provide clear insights into how and why decisions are made. This helps build trust and supports regulatory compliance.
As healthcare data continues to grow, the system must handle increasing workloads without compromising performance. Slow processing or system failures can reduce the effectiveness of fraud detection and impact user experience.
Solution:
Use cloud-based infrastructure and distributed computing frameworks to handle large datasets efficiently. Designing the system for scalability ensures it can grow alongside business needs.
Being aware of these challenges and addressing them with practical solutions helps ensure that AI healthcare fraud detection systems remain effective, reliable, and ready for real-world demands.
Compliance and security form the backbone of any healthcare AI solution. Fraud detection systems handle highly sensitive patient information, insurance records, and financial data, which makes them a prime target for breaches and misuse.
Organizations must ensure that every layer of the system is designed with strict regulatory adherence and strong protection mechanisms to avoid legal risks and maintain trust.
HIPAA defines how patient health information should be stored, accessed, and shared within healthcare systems in the United States. AI-based fraud detection platform development must ensure that protected health information is handled securely and only accessed by authorized individuals. Failure to comply with can result in heavy penalties and loss of credibility.
Implementation Approach:
Apply encryption for both stored and transmitted data, enforce strict role-based access controls, and maintain detailed audit logs to track every interaction with sensitive information.
Also Read: HIPAA-Compliant AI Healthcare Software Development: Benefits, Technology, Steps and Challenges
GDPR focuses on protecting personal data and giving users control over how their information is used. This regulation is critical for organizations operating in or serving users from Europe. It requires transparency in data processing and ensures that users can access or request deletion of their data.
Implementation Approach:
Design systems with privacy-first principles, include consent management features, and implement data anonymization techniques to protect user identity while maintaining analytical capabilities.
AI healthcare fraud detection systems process large volumes of sensitive data, making encryption a non-negotiable requirement. Without proper protection, data can be exposed during storage or transmission, leading to serious security breaches and compliance violations.
Implementation Approach:
Use industry-standard encryption protocols, secure communication channels, and regularly update security practices to safeguard data from evolving cyber threats.
Managing who can access the system is essential to prevent unauthorized usage and internal misuse. Without proper access control, sensitive data may be exposed to individuals who should not have visibility into it.
Implementation Approach:
Implement role-based access control, enable multi-factor authentication, and continuously monitor user activity to ensure only authorized users can interact with the system.
Tracking system activity is important for maintaining transparency and accountability. Audit trails help organizations monitor who accessed data, what changes were made, and when these actions occurred.
Implementation Approach:
Maintain detailed logs of all system activities and use monitoring tools to detect unusual behavior. This helps support compliance audits and identify potential security issues early.
Fraud detection systems often integrate with multiple healthcare platforms and external systems. These integrations can become points of vulnerability if not properly secured.
Implementation Approach:
Use secure API gateways, implement authentication and authorization protocols, and ensure encrypted communication for all data exchanges between systems.
Reducing exposure of sensitive information helps minimize risks and supports compliance requirements. Not all data used for fraud detection needs to include identifiable patient details.
Implementation Approach:
Apply data masking and anonymization techniques during processing and ensure that only necessary data is accessible for analysis and model training.
Security is an ongoing process that requires continuous monitoring and improvement. New vulnerabilities can emerge over time, making regular testing essential.
Implementation Approach:
Conduct periodic penetration testing, perform vulnerability assessments, and keep systems updated to address potential security gaps and maintain strong protection.
Consistent compliance and well-structured security measures ensure that AI healthcare fraud detection systems operate safely, protect sensitive data, and meet regulatory expectations without compromise.
The future of fraud detection in healthcare is being shaped by rapid advancements in AI, data processing, and regulatory technology. As organizations continue to build AI systems for healthcare fraud detection, the focus is shifting toward smarter, faster, and more adaptive solutions that can handle growing data complexity and evolving fraud tactics.
Below are the key trends that will define the next phase of AI healthcare compliance and fraud detection software development.
Future systems will move beyond reactive detection and focus on predicting fraud before it happens. AI models will analyze patterns in real time and identify risks during the transaction itself.
This approach will:
Organizations that adopt predictive capabilities will gain a strong operational advantage.
As AI systems become more complex, there is a growing need for transparency in decision-making. Explainable AI will help users understand why a claim was flagged as fraudulent.
This trend will:
Explainability will become a standard requirement in fraud detection platforms.
Blockchain technology is expected to play a role in improving data security and traceability. It can create tamper-proof records of healthcare transactions.
This will help:
Combining blockchain with AI will enhance both security and reliability.
Healthcare data is highly sensitive and sharing it across organizations can be challenging. Federated learning allows AI models to be trained across multiple systems without moving data.
Benefits include:
This approach will support safer and more scalable AI adoption.
Fraud is often organized and involves multiple entities. Future systems will use advanced graph analytics to detect relationships and hidden networks.
This will enable:
Graph-based intelligence will become a key component of advanced fraud detection systems.
The rise of agentic AI is enabling systems to take more autonomous actions. These systems can analyze, decide, and act with minimal human intervention. With growing demand for agentic AI development services, organizations are focusing on smarter and more self-operating fraud detection solutions.
This will help:
Agentic AI will play a major role in next-generation healthcare fraud detection platforms.
Regulations around healthcare data are becoming stricter. Future solutions will integrate compliance directly into system design.
This trend will:
AI healthcare compliance and fraud detection software development will increasingly focus on building systems that are secure, transparent, and regulation-ready.
The future of healthcare fraud detection lies in intelligent, adaptive, and compliance-focused AI systems that not only detect fraud but also prevent it in real time while maintaining trust and security.
Upgrade your system with advanced AI fraud detection capabilities and improve efficiency.
Schedule a DemoOrganizations planning the development of AI healthcare fraud detection software often look for a partner who can handle both technical complexity and healthcare-specific requirements. A common question is, which companies provide end-to-end development of AI fraud detection system for healthcare?
This is where working with an experienced AI healthcare software development company like Biz4Group LLC makes a real difference.
Biz4Group specializes in AI healthcare fraud detection software development, helping businesses design and deploy intelligent systems that are scalable, secure, and aligned with compliance standards.
Their approach focuses on delivering practical solutions that solve real business problems while ensuring long-term scalability.
Biz4Group has delivered multiple AI-based healthcare solutions, demonstrating strong expertise across different use cases.
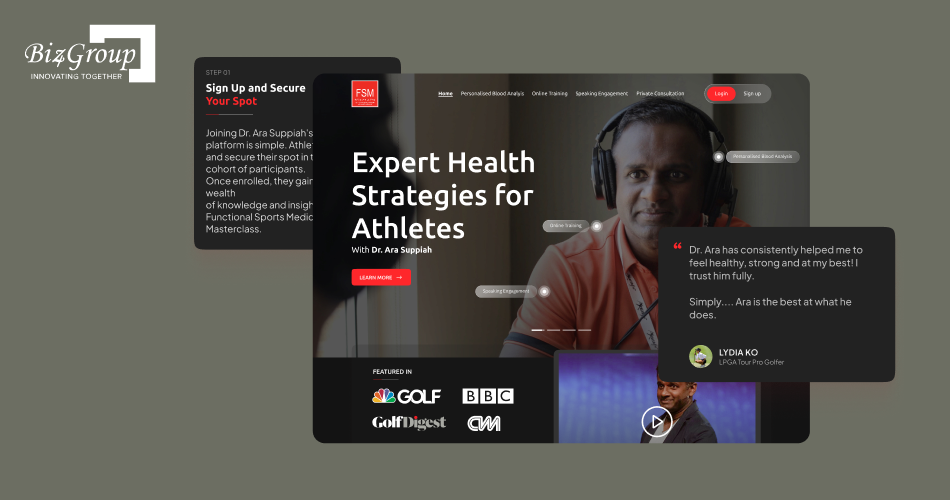
Dr. Ara is an intelligent AI-driven platform built to enhance athletic performance through detailed blood analysis and personalized health insights. It provides actionable recommendations, monitors key health indicators, and offers tailored guidance to help athletes achieve their fitness and performance goals more effectively.
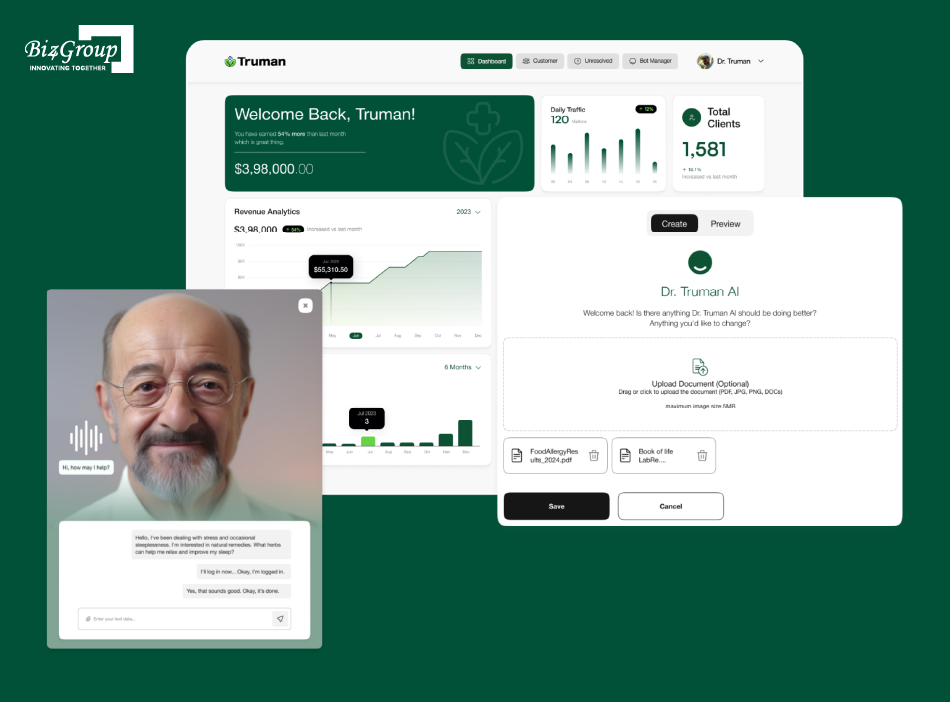
This solution features an AI-powered virtual health companion designed to make wellness more interactive and accessible. Users can communicate with an AI avatar for personalized health advice, explore curated wellness products, and access exclusive benefits through membership plans. The platform also enables users to manage their health records and track progress in one place.
So, connect with Biz4Group to build a secure, scalable, and high-performing AI healthcare fraud detection software solution tailored to your business needs and growth goals.
Healthcare organizations are under constant pressure to detect fraud faster, reduce financial losses, and maintain compliance with strict regulations. This is where AI healthcare fraud detection software development plays a crucial role by enabling smarter, faster, and more accurate fraud detection. From analyzing complex datasets to identifying hidden fraud patterns, AI-driven systems help organizations stay ahead of evolving risks.
Investing in the development of AI healthcare fraud detection software allows businesses to build scalable solutions that adapt to changing fraud tactics and growing data volumes. These systems not only improve operational efficiency but also strengthen trust across the healthcare ecosystem.
If you are wondering, who offers consulting and development for AI fraud detection software for healthcare systems? partnering with the right experts ensures long-term success.
Book an appointment today to discuss your requirements and explore the right AI solution for your healthcare platform.
AI analyzes large volumes of healthcare data such as claims, billing records, and patient history to identify unusual patterns. It uses machine learning models to flag anomalies, detect duplicate claims, and recognize suspicious behaviors in real time.
To develop AI healthcare fraud detection software, you need quality healthcare data, AI models, cloud infrastructure, and integration with existing systems. It also requires compliance with regulations like HIPAA and strong security measures.
The timeline depends on complexity. A basic MVP of AI healthcare fraud detection software can take around 2 to 4 weeks, while a full-scale enterprise solution may take 6 to 12 weeks, including development, testing, and deployment.
Benefits of integrating AI in healthcare fraud detection software improves detection accuracy, reduces manual effort, enables real-time fraud prevention, and helps organizations save costs. It also adapts to new fraud patterns over time, making it more effective than traditional systems.
The cost to make AI healthcare fraud detection system typically ranges from $40,000 to $300,000 or more, depending on features, integrations, and system complexity. Enterprise-level solutions with advanced AI capabilities may require higher investment.
Several AI healthcare software development companies offer end-to-end services for AI healthcare fraud detection software, including consulting, development, and deployment. Choosing a company with healthcare domain expertise and AI experience is important for building a reliable solution.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.