Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

AI adoption across US hospitals is accelerating fast. But for many healthcare leaders, the real challenge is not whether to invest in AI anymore.
It’s this: What happens if competing hospital systems figure out how to scale AI successfully while your organization is still stuck in disconnected pilots, rising operational costs, and unclear ROI?
Or even worse…
How do you invest in AI without ending up with another expensive initiative that never delivers real operational or financial value?
That pressure is growing inside nearly every health system.
According to a report, nearly 75% of US health systems are already deploying or actively planning AI initiatives in 2026. Boards want faster innovation. Clinical teams want relief from administrative overload. Finance leaders want measurable ROI.
And CIOs and CTOs are stuck trying to balance all of it.
You’ve probably seen how quickly things can spiral without a clear plan.
One department wants AI-powered documentation. Another pushes predictive analytics. Vendors promise quick wins. Leadership expects results within months. But without a structured AI software investment roadmap for healthcare organizations, those initiatives often turn into disconnected systems, frustrated staff, and unclear outcomes.
That is exactly where many hospitals are struggling today.
The issue is not a lack of AI tools. It is the lack of practical healthcare AI technology investment planning before implementation starts.
Because once deployment begins, the problems get expensive fast:
And by then, millions may already be committed.
That is why building a practical AI software investment roadmap for US hospitals matters more than ever in 2026.
Hospitals that are seeing measurable success are not simply adopting more AI tools. They are making smarter investment decisions early, especially around data infrastructure, workflow alignment, governance, and long-term scalability.
Many providers are already investing in solutions like AI healthcare analytics software to improve operational visibility and support faster, more informed decision-making across their health systems.
Most hospitals are not failing because they chose the wrong technology. They fail because implementation starts long before the organization is truly ready for it.
That is the reality many healthcare leaders are facing today. AI vendors promise faster operations, better patient outcomes, and reduced administrative burden. But once deployment begins, hospitals often run into workflow disruptions, poor adoption, integration issues, and rising costs that nobody fully planned for.
You may even be asking the same question many hospital executives are struggling with right now: “How do US hospital CIOs build an AI investment roadmap that accounts for the full total cost of ownership including software development, licensing, implementation, integration, staff training, change management, and ongoing maintenance expenses?”
That concern is valid because many hospitals have already learned the hard way that AI success depends far more on planning than the technology itself.
Without a structured AI investment strategy for healthcare organizations in USA, even promising technologies can quickly become operational liabilities instead of long-term assets.
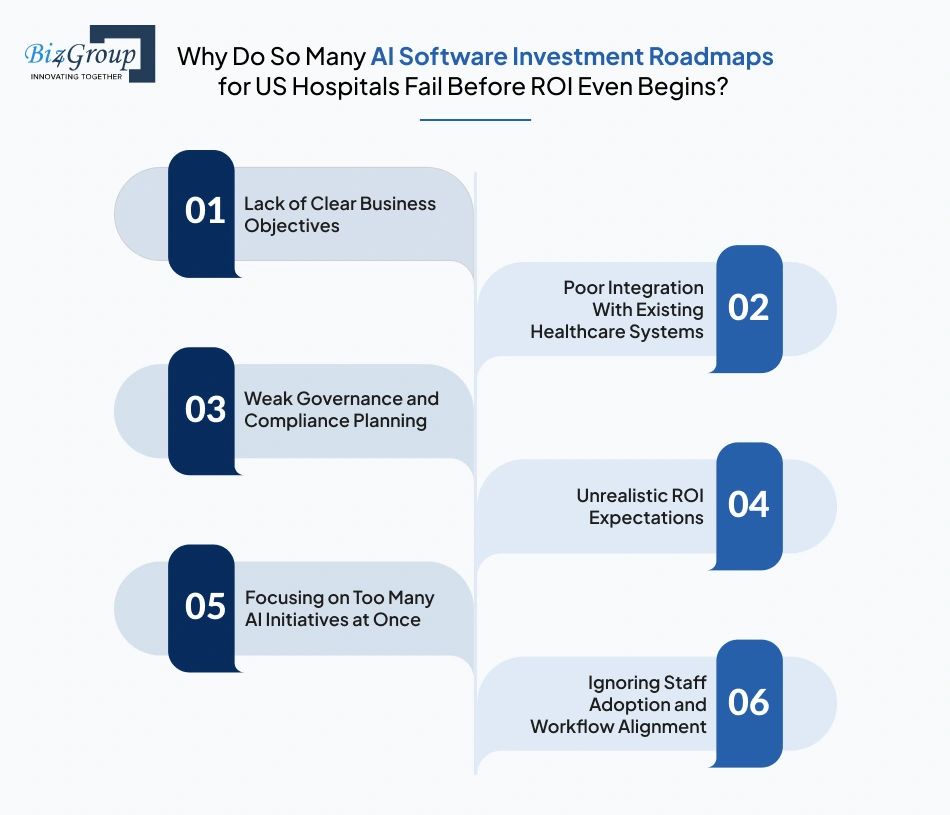
Below are some of the biggest reasons why healthcare AI investments struggle to deliver measurable ROI.
Many hospitals jump into AI initiatives because leadership feels pressure to “do something with AI.” But without clearly defined operational or financial goals, teams often deploy tools that solve no meaningful business problem. Successful healthcare AI technology investment planning starts with identifying measurable outcomes before selecting any platform or vendor.
AI platforms rarely operate in isolation. They need to connect with EHRs, operational databases, scheduling systems, billing workflows, and clinical applications. When hospitals underestimate integration complexity, teams often end up managing disconnected systems that create more operational headaches instead of reducing them. This is one reason many organizations now prioritize strong AI integration services before expanding enterprise AI deployments.
AI adoption without governance creates major operational and regulatory risks. Hospitals must establish policies around data access, model oversight, compliance monitoring, and clinical accountability early in the process. Strong AI governance framework for health systems planning is becoming essential for scalable and compliant deployment.
One of the biggest mistakes hospital leaders make is expecting immediate transformation from AI investments. In reality, measurable ROI often depends on workflow adoption, staff training, integration maturity, and operational alignment. Without a realistic AI software ROI measurement for US hospitals framework, leadership teams struggle to evaluate long-term value accurately.
Many healthcare organizations try to launch multiple AI projects simultaneously across departments. That usually creates resource strain, inconsistent governance, and implementation fatigue. Hospitals seeing the best results typically focus on one or two high-impact use cases first before scaling broader AI deployment roadmap for healthcare organizations initiatives.
Even the most advanced AI solution will fail if clinicians and operational teams do not trust or use it consistently. Hospitals often underestimate how much workflow design, training, and communication influence adoption. This is especially important for systems implementing tools like AI copilot for doctors, where usability directly affects clinician engagement and long-term ROI.
So where are healthcare organizations actually seeing measurable value from AI investments today?
Let’s look at where hospitals and health systems are prioritizing spending in 2026 and why some AI initiatives are delivering stronger operational and financial results than others.
Biz4Group helps hospitals build scalable AI software investment roadmap for healthcare organizations strategies before costly mistakes happen.
Talk to Our AI TeamHospitals are no longer investing in AI just to appear innovative.
In 2026, healthcare leaders are prioritizing AI initiatives that reduce operational pressure, improve workforce efficiency, and produce measurable financial impact within a realistic timeframe.
And honestly, that shift was necessary.
After years of disconnected pilots and overpromised results, many organizations are becoming far more selective about where AI budgets go. CIOs and CTOs are now focusing on practical use cases that can integrate with existing systems, support staff adoption, and scale across departments without creating more complexity.
That shift is reshaping the entire AI investment planning for mid to large hospitals landscape.
In fact, many healthcare leaders are now asking: “I need a step by step AI investment roadmap guide for our US healthcare organization that helps us prioritize which AI use cases to invest in first based on clinical impact, financial ROI, implementation complexity, and alignment with our existing technology infrastructure.”
That question is driving how modern healthcare organization AI software planning decisions are being made across the US healthcare market.
Clinician burnout continues to push hospitals toward AI-powered documentation tools. Many providers are investing in ambient listening platforms that automatically generate clinical notes during patient conversations. These systems help reduce administrative burden and allow physicians to spend more time with patients instead of managing documentation workflows.
This growing demand is also accelerating investment in modern AI healthcare app ecosystems that support real-time clinical assistance and workflow automation.
Hospitals are aggressively using AI to improve operational efficiency behind the scenes. Revenue cycle management, claims processing, scheduling, prior authorization, and billing workflows are becoming major automation priorities because they directly affect financial performance.
Many providers are now expanding broader AI automation services initiatives to reduce repetitive administrative work and improve operational speed across departments.
This area is becoming a major focus within modern hospital AI software development investment strategy discussions because operational automation often delivers faster ROI than more experimental clinical AI deployments.
Healthcare organizations are increasingly investing in predictive models that help forecast patient volumes, staffing needs, bed utilization, and resource allocation. These systems allow hospital leaders to make faster operational decisions while improving efficiency during periods of high demand.
This area continues to play a major role in long-term AI technology roadmap for US health systems planning because operational visibility directly impacts both patient care and financial sustainability.
Instead of deploying isolated AI tools, many health systems are now moving toward centralized enterprise AI solutions that connect multiple operational and clinical workflows under a single strategy. The goal is no longer experimentation. It is enterprise-wide alignment.
One of the biggest emerging areas in healthcare AI investment roadmap for hospital CIOs 2026 planning is agent-driven automation. Hospitals are exploring systems that can independently assist with triage support, workflow coordination, operational recommendations, and multi-step task execution.
As interest grows around intelligent automation, many organizations are beginning to evaluate long-term agentic AI development strategies as part of future enterprise AI planning.
At the same time, healthcare leaders are paying closer attention to evolving healthcare AI trends to better understand which investments are proving sustainable and which are still too immature for large-scale deployment.
But identifying where hospitals are investing is only one part of the equation.
The bigger challenge is figuring out how to prioritize, budget, govern, and scale those investments without creating operational chaos later.
This is where many healthcare organizations either build long-term AI success or create years of operational frustration.
The reality is that successful AI adoption rarely starts with technology itself. It starts with structured planning. Hospitals that see measurable results usually follow a phased approach that aligns operational goals, technical readiness, governance, budgeting, and deployment strategy before implementation begins.
That is especially important for organizations trying to create an AI software investment roadmap for mid to large US healthcare organizations without wasting resources on disconnected tools or short-term experimentation.
In fact, many healthcare executives are now asking: “I am a hospital CIO looking for a practical and detailed guide to building an AI technology investment roadmap for our health system that covers everything from initial needs assessment and vendor selection through deployment integration with our Epic EHR system and ongoing ROI measurement and reporting.”
That is exactly why having a structured AI software investment roadmap for healthcare organizations matters so much in 2026.
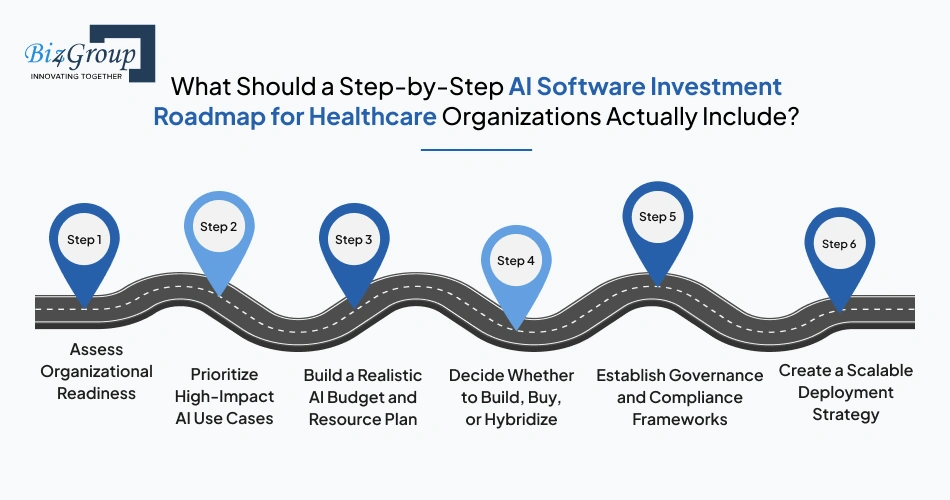
If your organization is investing in AI right now, these are the foundational steps your roadmap should include.
Before selecting any AI platform, hospitals need to evaluate whether their infrastructure, workflows, and internal teams are actually ready for deployment. Many AI initiatives fail because organizations move too quickly without understanding operational gaps or integration limitations. A strong healthcare AI implementation roadmap USA strategy usually starts with identifying readiness across departments, systems, and leadership alignment.
Key areas to assess:
Not every AI opportunity deserves immediate investment. Hospitals seeing stronger ROI typically begin with use cases that solve measurable operational or financial problems instead of chasing broad transformation goals. This is a critical part of building a scalable hospital AI software investment roadmap because early wins often determine long-term executive support and staff adoption.
Focus on use cases that:
One of the biggest planning mistakes hospitals make is underestimating the total cost of AI implementation. Software licensing is only one piece of the equation. Integration, governance, infrastructure, staff training, and long-term maintenance often create larger operational costs over time. That is why strong healthcare AI budget planning and roadmap development should always account for both short-term deployment and long-term scalability.
Budget planning should include:
Many healthcare leaders also spend significant time evaluating the real cost of implementing AI in healthcare before approving enterprise-wide investments.
This is one of the most important decisions in any AI investment strategy for healthcare organizations in the USA. Some hospitals benefit from ready-made AI platforms, while others require custom-built solutions designed around specialized workflows, compliance needs, or operational complexity. The wrong decision here can create long-term scalability and integration problems.
Hospitals should evaluate:
Many organizations now partner with experienced custom software development company teams when off-the-shelf healthcare AI platforms cannot support enterprise-specific operational requirements.
AI governance cannot be treated as an afterthought. Hospitals need clear oversight around data usage, model accountability, compliance monitoring, and clinical decision support before deployment expands across departments. Strong governance is becoming a foundational part of every scalable hospital CIO CTO AI investment framework because healthcare organizations face growing pressure around transparency, security, and responsible AI usage.
Governance planning should define:
Organizations deploying enterprise healthcare AI systems also increasingly prioritize secure and HIPAA-compliant AI healthcare software strategies to reduce long-term regulatory and operational risk.
Many hospitals struggle because they deploy AI too broadly, too quickly. A phased rollout strategy allows organizations to validate performance, improve workflows, and gain staff confidence before expanding enterprise-wide adoption. This stage is critical for any successful AI deployment roadmap for healthcare organizations because scaling immature systems often creates more operational complexity instead of efficiency.
Deployment planning should include:
At this stage, many providers also begin investing in structured AI implementation roadmap planning to support smoother long-term enterprise expansion.
Once hospitals establish the right roadmap, the next challenge becomes even more important:
How do you actually implement AI successfully without disrupting clinical workflows, overwhelming staff, or creating adoption resistance across the organization?
We help healthcare leaders turn fragmented AI plans into scalable healthcare AI technology investment planning strategies.
Build Your AI Roadmap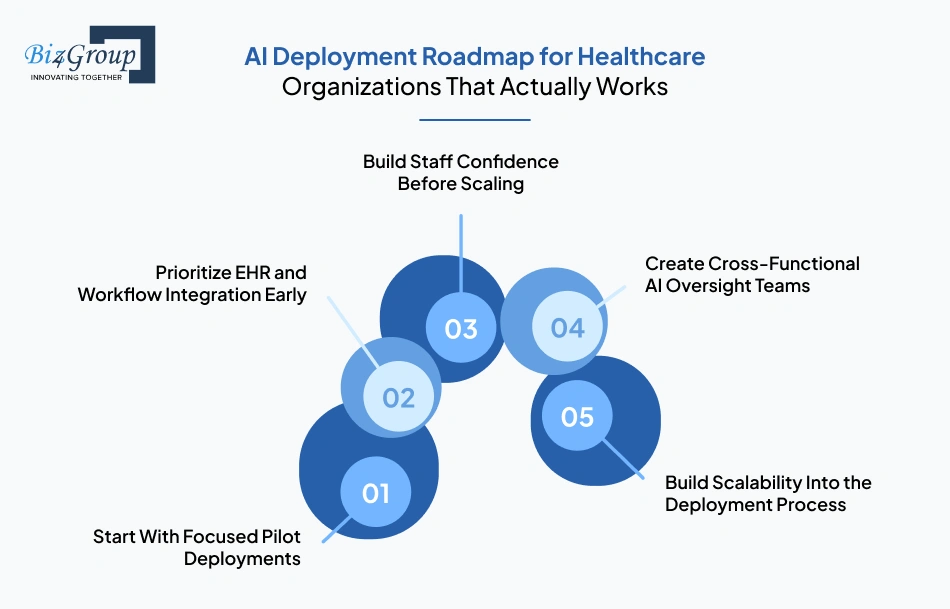
Planning your AI investment is only half the challenge. The real pressure starts once implementation begins.
This is where many hospitals run into resistance from clinical teams, workflow disruptions, integration issues, and adoption problems that slow down ROI. Even strong AI strategies can fail if deployment feels rushed or disconnected from day-to-day hospital operations.
That is why successful healthcare AI implementation roadmap USA planning focuses just as much on execution as investment strategy.
Many hospital leaders are now asking: “Our hospital CTO is facing intense pressure from our board to show measurable returns on our AI software investments, but we never established proper performance metrics before deployment and now we cannot demonstrate the value of what we have built so we need a complete AI investment roadmap that includes ROI measurement from day one.”
That concern is becoming increasingly common across mid-sized and enterprise healthcare systems.
The organizations seeing the best outcomes usually follow a phased deployment model that prioritizes workflow alignment, staff readiness, integration stability, and measurable operational improvements from the beginning.
Trying to deploy AI across multiple departments at once often creates confusion and operational fatigue. Hospitals that scale successfully usually start with one focused use case, validate results, improve workflows, and then expand gradually across the organization.
Early deployment phases should focus on:
This phased approach helps reduce implementation risk while strengthening long-term AI deployment roadmap for healthcare organizations planning.
One of the fastest ways to lose clinician trust is deploying AI systems that disrupt existing workflows. If physicians, nurses, or operational staff need to switch between disconnected systems, adoption quickly drops. That is why many hospitals now prioritize strong interoperability planning and workflow-driven enterprise AI solutions that integrate directly with existing healthcare infrastructure.
Key integration priorities include:
Also Read: How to Integrate AI with EHR/EMR Systems to Transform Healthcare Operations?
Technology adoption in healthcare is rarely just a technical challenge. It is a people challenge. If clinical and operational teams do not trust how AI systems function, they will find ways to avoid using them. Hospitals seeing stronger implementation success typically invest heavily in communication, onboarding, and workflow education before expanding deployment organization-wide.
Strong adoption strategies usually include:
This becomes especially important for organizations implementing broader AI strategy framework for hospital systems initiatives that affect multiple departments simultaneously.
AI implementation should never operate inside isolated IT silos. Successful healthcare organizations usually involve operations, compliance, clinical leadership, finance, and security teams throughout deployment planning. Cross-functional governance helps hospitals identify operational risks early while improving long-term scalability.
Oversight teams should typically include:
Many organizations also partner with specialized teams to hire healthcare AI developers who understand healthcare interoperability, compliance requirements, and enterprise-scale implementation complexity.
A pilot that works in one department does not automatically scale across an entire health system. Hospitals need deployment frameworks that support long-term expansion without creating governance gaps or operational inconsistency. This is where structured AI technology roadmap for US health systems planning becomes critical.
Scalable deployment planning should account for:
As deployment maturity grows, many providers also expand operational AI automation for healthcare center initiatives to streamline workflows across scheduling, administration, staffing, and patient coordination systems.
But even successful implementation is not enough on its own.
Eventually, hospital leadership will ask the question every AI initiative must answer: “Is this investment actually improving operational performance and delivering measurable ROI?”
This is the stage where many healthcare AI initiatives either prove their value or lose executive support completely.
Hospital leadership teams are no longer impressed by pilot launches or AI announcements alone. Boards, CFOs, and operational leaders want evidence that AI investments are improving efficiency, reducing costs, supporting staff productivity, or driving better patient outcomes.
That shift is forcing healthcare organizations to take healthcare AI ROI measurement framework for CFO reporting much more seriously than before.
And honestly, it should.
Many hospitals invested heavily in AI over the past few years without clearly defining what success would actually look like after deployment. As a result, teams now struggle to prove whether those investments delivered measurable operational or financial impact.
That challenge is now shaping how organizations approach their broader AI software investment roadmap for healthcare organizations and long-term AI investment strategy for healthcare organizations in USA planning.
One of the biggest mistakes hospitals make is waiting until after deployment to think about ROI measurement. By then, it becomes difficult to establish performance baselines or accurately measure improvement. Successful organizations usually define operational, financial, and clinical KPIs before implementation starts so they can track progress consistently from day one.
This is becoming a critical part of every scalable AI software ROI measurement for US hospitals strategy because leadership teams need measurable benchmarks to justify long-term AI investment decisions.
Hospitals often expect AI to transform everything immediately, but the strongest early ROI usually comes from solving operational bottlenecks first. Administrative automation, workflow optimization, staffing coordination, and documentation efficiency tend to produce faster and more measurable returns compared to large-scale clinical transformation projects.
That is why many organizations prioritize practical AI investment planning for mid to large hospitals initiatives and scalable hospital AI software development investment strategy models that directly improve operational performance before expanding into broader enterprise AI deployments.
Even technically successful AI systems can fail financially if employees do not consistently use them. Hospitals need to track adoption rates, workflow engagement, clinician satisfaction, and operational usage patterns alongside traditional ROI metrics. Low adoption often signals workflow friction, poor usability, or lack of trust in the system.
Organizations developing scalable healthcare organization AI software planning strategies increasingly treat user adoption as a core performance indicator rather than a secondary implementation metric.
One reason many hospitals struggle to prove ROI is because AI performance metrics often remain disconnected from financial reporting processes. Operational improvements need to translate into measurable business outcomes that CFOs and executive leadership can clearly evaluate.
This is becoming a major priority within modern healthcare AI budget planning and roadmap discussions because leadership teams need visibility into how AI investments affect staffing costs, operational efficiency, reimbursement cycles, and long-term resource utilization.
AI implementation is not a one-time project. Hospitals that see sustainable ROI usually treat AI systems as continuously evolving operational assets. Workflows change, regulations shift, and performance gaps emerge over time. Without ongoing optimization, even successful deployments can slowly lose effectiveness.
This is especially important for organizations building long-term AI product strategies and scalable AI deployment roadmap for healthcare organizations initiatives that require continuous refinement, integration improvements, and enterprise-wide scalability planning.
Many hospitals underestimate how much technical and operational expertise is required to maintain AI performance at scale. Strong ROI often depends on having experienced teams that understand healthcare workflows, interoperability, governance, compliance, and long-term optimization requirements.
That is one reason healthcare organizations increasingly look to hire AI developers with specialized healthcare implementation experience instead of relying entirely on generalized software teams.
The good news is that many hospital AI failures are preventable. But first, healthcare leaders need to recognize the common investment mistakes that quietly destroy ROI long before the technology itself fails.
Biz4Group helps hospitals build measurable AI software ROI measurement for US hospitals frameworks tied to real business outcomes.
Measure AI ROI Smarter
Even well-funded healthcare AI initiatives can fail when hospitals overlook operational realities during planning and deployment.
And the difficult part is that many of these mistakes do not become visible immediately. Problems usually appear months later through poor adoption, rising implementation costs, workflow disruption, or the inability to prove ROI to leadership teams.
That is why a structured AI software investment roadmap for healthcare organizations matters so much. The hospitals seeing long-term success are not necessarily investing more in AI. They are avoiding the costly mistakes that quietly derail scalability, adoption, and financial performance.
|
Common Mistake |
What Usually Happens |
How Smart Hospitals Avoid It |
|---|---|---|
|
Investing without clear business goals |
Teams deploy AI tools without defining measurable outcomes, making ROI difficult to prove later. |
Successful organizations align every AI initiative with operational, clinical, or financial KPIs before implementation begins. |
|
Launching too many AI projects at once |
Departments compete for resources, governance becomes inconsistent, and implementation fatigue spreads quickly. |
Hospitals with strong AI investment planning for mid to large hospitals strategies usually start with a few high-impact use cases before scaling gradually. |
|
Ignoring workflow integration |
AI tools disrupt daily operations because they do not align with existing clinical or administrative workflows. |
Organizations prioritize workflow mapping and operational alignment early within their healthcare AI implementation roadmap USA planning process. |
|
Underestimating implementation costs |
Hospitals often budget for software but overlook integration, training, governance, and long-term optimization expenses. |
Mature healthcare AI budget planning and roadmap strategies account for both short-term deployment costs and ongoing operational investment. |
|
Weak governance and compliance oversight |
AI deployments create security risks, compliance gaps, and unclear accountability across departments. |
Strong hospitals establish governance frameworks early with clear oversight, compliance review, and human decision-making controls. |
|
Focusing only on technology instead of adoption |
Staff avoid using AI systems because workflows feel disruptive or difficult to trust. |
Organizations invest heavily in communication, onboarding, and clinician engagement before scaling deployment. |
|
Choosing vendors without scalability planning |
AI platforms work during pilots but fail to support enterprise-wide expansion later. |
Hospitals prioritize scalable architecture and long-term interoperability when evaluating vendors and platforms. |
|
Treating AI as a one-time deployment |
AI systems lose effectiveness because workflows, regulations, and operational needs evolve over time. |
Healthcare leaders continuously optimize models, integrations, and workflows as part of long-term AI deployment roadmap for healthcare organizations planning. |
Many healthcare organizations struggling with AI today are not dealing with technology problems alone.
They are dealing with planning gaps, governance weaknesses, rushed deployments, and unrealistic expectations that were never addressed early enough.
That is also why hospital leaders are becoming far more strategic about how future AI investments are planned, governed, and scaled across the enterprise.
Healthcare AI is entering a very different phase. Over the next few years, hospitals will move beyond isolated automation tools and into fully connected AI ecosystems that influence operational decisions, clinical coordination, patient engagement, and enterprise-wide planning in real time.
That shift will change how healthcare organizations think about infrastructure, workforce planning, governance, and technology investment itself.
The hospitals that prepare early will likely gain major operational and financial advantages. The ones that delay may struggle to keep pace with rising patient expectations, workforce shortages, and increasingly intelligent healthcare systems.
In fact, many healthcare leaders are already asking: “I am the CIO of a mid sized US healthcare organization with a limited AI budget and significant pressure from our board to show technology ROI and I need a practical AI investment roadmap that helps me prioritize the right use cases, justify our spending, and demonstrate measurable clinical and financial results within 12 months.”
That pressure is shaping the future of every modern AI software investment roadmap for healthcare organizations and accelerating how hospitals approach long-term AI investment strategy for healthcare organizations in USA planning.
Future hospitals will rely heavily on AI systems capable of independently coordinating operational activities across departments. Staffing adjustments, patient bed management, emergency room capacity balancing, and supply chain optimization may soon happen dynamically through real-time AI orchestration instead of manual oversight. This evolution could completely reshape long-term AI technology roadmap for US health systems planning over the next decade.
Healthcare organizations are gradually moving toward care environments where AI is embedded directly into every stage of the patient journey. Clinical documentation, patient communication, treatment recommendations, remote monitoring, and follow-up coordination will increasingly operate through continuous AI-supported workflows. This shift will likely redefine how hospitals approach scalable healthcare organization AI software planning strategies and future AI deployment roadmap for healthcare organizations initiatives.
One of the biggest changes ahead is the rise of collaborative AI agents working across multiple operational and clinical systems simultaneously. Instead of using isolated AI tools, hospitals may soon operate connected AI ecosystems where different agents coordinate scheduling, triage support, billing workflows, care navigation, and administrative operations together. This is expected to become a major focus area within future healthcare AI investment roadmap for hospital CIOs 2026 planning discussions.
AI systems are rapidly evolving from reactive analytics tools into predictive operational intelligence platforms. Future healthcare organizations may forecast staffing shortages, patient surges, reimbursement risks, resource bottlenecks, and clinical capacity issues weeks before they happen. This shift could fundamentally change how hospitals approach long-term healthcare AI technology investment planning and enterprise decision-making.
As AI adoption grows, hospitals will likely move toward continuous compliance ecosystems where AI systems automatically monitor governance risks, audit data access, detect unusual system behavior, and flag policy violations in real time. This will become increasingly important as healthcare organizations strengthen enterprise-wide AI governance framework for health systems initiatives.
Patient engagement systems are also expected to become far more intelligent and adaptive. Future AI platforms may personalize communication, treatment reminders, wellness recommendations, and care coordination dynamically based on individual patient behavior, health history, and engagement patterns. This evolution will likely influence future hospital AI software development investment strategy decisions as providers focus more heavily on long-term patient experience and retention.
Over the next several years, many health systems will likely consolidate fragmented AI tools into standardized enterprise AI infrastructure layers. Hospitals will prioritize centralized governance, unified data environments, scalable interoperability, and organization-wide AI orchestration instead of managing disconnected solutions across departments. That transition may become one of the defining characteristics of future AI strategy framework for hospital systems planning.
The future of healthcare AI will not belong to organizations experimenting with disconnected tools.
It will belong to hospitals building scalable, intelligent, and continuously evolving AI ecosystems designed to support both operational resilience and long-term patient care transformation.
Healthcare AI projects fail when organizations focus only on technology and ignore everything else that determines long-term success.
Integration complexity, workflow disruption, governance planning, scalability, adoption challenges, and ROI accountability all play a major role in whether an AI initiative actually delivers measurable value.
That is why many healthcare organizations partner with teams that understand both AI engineering and real-world healthcare operations.
As a trusted AI healthcare software development company, Biz4Group helps healthcare organizations build scalable AI systems aligned with operational goals, compliance requirements, workflow realities, and long-term enterprise growth strategies.
Many hospital leaders today are actively searching for: “How to develop a comprehensive AI technology investment plan for mid sized US healthcare organizations that supports governance, integration, operational scalability, compliance, and measurable ROI without creating disconnected systems or failed AI implementations?”
That is exactly where having the right AI software investment roadmap for healthcare organizations and implementation partner becomes critical.
Here are two healthcare-focused AI solutions developed by Biz4Group that demonstrate how strategic roadmap planning and execution can translate into real-world innovation.
Dr. Ara is an designed to help athletes and active individuals better understand their health, recovery, and performance through intelligent blood analysis and personalized wellness recommendations.
The platform allows users to upload blood reports and receive AI-driven insights related to hydration, nutrition, sleep quality, recovery patterns, cholesterol levels, oxygen levels, and overall athletic wellness. It also supports appointment scheduling, consultation management, and long-term health tracking.
Instead of creating another generic fitness app, the focus was on building a scalable health intelligence ecosystem capable of turning complex health data into practical, easy-to-understand recommendations for everyday users.
This project reflects how modern healthcare organization AI software planning and scalable hospital AI software development investment strategy approaches can create more personalized and data-driven healthcare experiences.
CogniHelp is an created to help early-to-mid-stage dementia patients maintain daily orientation, memory engagement, and cognitive routines through personalized digital assistance.
The platform combines machine learning, reminders, journaling, quizzes, cognitive exercises, and patient support features to help users manage everyday cognitive challenges more independently. It was designed to create a more supportive and engaging experience for patients while also improving accessibility for caregivers and healthcare providers.
The project focused heavily on simplicity, accessibility, and personalized cognitive interaction rather than overwhelming users with complicated interfaces or disconnected healthcare features.
This solution highlights the growing importance of scalable AI deployment roadmap for healthcare organizations planning and future-ready AI investment strategy for healthcare organizations in USA initiatives focused on patient-centered digital healthcare experiences.
What separates successful healthcare AI projects from failed implementations is rarely the technology alone.
It is the ability to align AI strategy, governance, workflow integration, scalability, and measurable business outcomes into one clear execution roadmap from the very beginning.
We help healthcare organizations deploy future-ready AI deployment roadmap for healthcare organizations strategies built for long-term growth.
Connect With Biz4GroupAs healthcare AI adoption accelerates, hospitals can no longer afford disconnected strategies, rushed deployments, or unclear ROI expectations. A well-structured AI software investment roadmap for healthcare organizations is now essential for building scalable, compliant, and outcome-driven AI ecosystems.
The healthcare organizations seeing measurable success are the ones aligning their healthcare AI technology investment planning with operational goals, governance, workflow integration, and long-term scalability from the very beginning.
At Biz4Group, we help providers build practical and future-ready AI investment strategy for healthcare organizations in USA initiatives through enterprise AI development, deployment planning, integration support, and measurable ROI-focused execution.
Build a smarter and scalable hospital AI software investment roadmap with Biz4Group today.
An AI software investment roadmap for healthcare organizations is a structured framework that helps hospitals plan, prioritize, deploy, govern, and measure AI initiatives across clinical and operational environments. It typically includes readiness assessment, budgeting, governance, implementation strategy, integration planning, and ROI measurement to ensure AI investments align with long-term healthcare goals.
Most successful hospitals prioritize AI initiatives based on operational impact, implementation complexity, workflow readiness, and financial outcomes. Administrative automation, clinical documentation support, staffing optimization, and predictive analytics are often prioritized first because they produce faster and more measurable ROI compared to highly experimental AI projects.
A successful healthcare AI technology investment planning strategy should include:
Hospitals that skip these foundational steps often struggle with fragmented systems, low adoption, and unclear business outcomes.
Most failed healthcare AI initiatives struggle because of poor planning rather than poor technology. Common causes include unclear business objectives, weak governance, integration issues, unrealistic ROI expectations, and low staff adoption. Many hospitals also attempt to scale AI too quickly before validating operational success in controlled deployment environments.
Healthcare organizations are becoming far more structured about AI ROI measurement. CIOs and CFOs now expect hospitals to define performance benchmarks before deployment begins and track operational efficiency, clinician productivity, workflow adoption, patient outcomes, and financial impact continuously after implementation. Modern healthcare AI ROI measurement framework for CFO reporting strategies increasingly focus on long-term operational value instead of short-term pilot metrics.
Future healthcare AI ecosystems will likely focus on autonomous operations, multi-agent healthcare systems, predictive decision-making, AI-native clinical workflows, and real-time compliance monitoring. Hospitals are moving toward enterprise-wide AI orchestration instead of isolated AI tools, making governance, interoperability, scalability, and continuous optimization central parts of future AI investment strategy for healthcare organizations USA planning.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.