Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

“Why does our clinic still have 3 full-time employees handling prior authorization requests all day while physicians wait, patients call repeatedly for updates, and approvals still take 8 days to process?”
That question is becoming common across mid-size clinics dealing with growing payer complexity and rising administrative pressure. Prior authorization teams are spending hours chasing insurance portals, collecting missing documents, and correcting submission errors that delay reimbursements.
In many clinics, the process has quietly turned into a major operational bottleneck. Physicians now complete nearly 39 prior authorization requests every week, while staff spend close to 13 hours handling approvals and follow-ups tied to those requests.
The pressure extends beyond paperwork. Delayed authorizations interrupt treatment schedules, slow imaging approvals, and create growing frustration across clinical and administrative teams. In fact, 89% of physicians say prior authorization contributes to burnout because patient care keeps getting interrupted by repetitive approval tasks.
For many clinics, the issue becomes harder as request volumes increase:
This is where AI prior authorization software development for mid-size clinics becomes a practical operational investment. This blog will walk you through building a custom AI prior authorization system with real time eligibility verification and payer requirement matching capabilities. You will understand how clinics are using it to reduce authorization delays, improve approval accuracy, and handle growing administrative workloads more efficiently.
As we dive deep, let's start by understanding the prior authorization crisis in mid-size clinics.
As patient volumes grow, prior authorization starts affecting multiple departments inside a clinic at the same time. What begins as an insurance approval task quickly turns into a coordination problem between physicians, billing teams, front-desk staff, and payer portals. Mid-size clinics feel this pressure more aggressively because they process higher authorization volumes without having large enterprise-level administrative infrastructure.
In many clinics, staff members spend a major part of their workday handling repetitive authorization tasks instead of patient-focused responsibilities. Recent reporting shows:
As authorization requests increase across specialties, these delays start spreading into scheduling, treatment approvals, and reimbursement cycles.
The issue becomes harder to control because every payer follows different requirements, approval rules, and documentation formats. Teams often move between multiple payer portals, fax systems, EHR screens, and spreadsheets just to complete a single request.
This creates several operational gaps inside mid-size clinics:
Prior authorization workflows break at mid-size clinic scale because the process depends heavily on manual coordination across disconnected systems. As request volumes continue rising, clinics need a workflow structure that can process authorizations faster without increasing administrative workload at the same pace.
Prior authorization is becoming one of the most expensive administrative responsibilities inside mid-size clinics costing upto $35 billion of US health care administrative spending.
The financial strain does not come from a single denial or delayed approval. It builds slowly through staff hours, repeated claim corrections, reimbursement delays, and growing operational overhead tied to manual processing. Take a look:
Every authorization request requires document collection, payer verification, status follow-ups, and coordination between departments. As patient volumes increase, clinics end up dedicating more payroll hours to administrative work that keeps expanding every month.
Current estimates show prior authorization handling costs nearly $11,000 per clinician annually. Clinics also spend around $20–$30 for every authorization submission, while the average practice processes nearly 45 prior authorizations each week.
For mid-size clinics operating across multiple specialties, these costs scale quickly across billing and administrative teams.
The financial impact becomes heavier when authorization issues lead to denied claims. Staff members often spend additional time correcting documentation, preparing appeals, resubmitting claims, and responding to payer clarification requests before reimbursements can move forward.
The average denied claim rework cost ranges between $25 and $181 per claim. At the same time, nearly 35–60% of denied or returned claims never get resubmitted, creating direct revenue leakage for clinics already operating under tight margins.
Manual authorization processing often creates hidden financial pressure through:
As authorization workloads continue increasing, many mid-size clinics struggle to maintain financial stability while managing growing payer-related administrative expenses.
Many mid-size clinics already use EHR software and revenue cycle management systems expecting them to simplify prior authorization workflows. In reality, authorization delays continue growing because these systems were not designed to manage payer-specific approval complexity at scale.
Most EHR platforms help clinics manage patient records, physician documentation, scheduling, and billing workflows. They centralize information effectively, but prior authorization requires much more than storing clinical data.
Authorization teams still need to:
As a result, staff members continue moving between multiple systems even after the clinic has invested heavily in EHR infrastructure.
Revenue cycle management systems help clinics manage claims submission, payment tracking, and reimbursement workflows. However, most traditional RCM tools operate after services are delivered, while prior authorization problems begin much earlier during treatment approval stages.
This creates a major operational gap. Clinics often discover missing authorizations, incomplete documentation, or payer mismatches only after claims move toward denial.
For mid-size clinics handling multiple insurance providers, the situation becomes harder because every payer follows different approval criteria and submission processes.
Also Read: How to Develop a Healthcare Revenue Cycle Management Software (RCM)
Even with digital systems in place, prior authorization workflows still depend heavily on human coordination. Staff members manually review payer websites, upload documents, respond to clarification requests, and track approval status across disconnected platforms.
Several limitations continue slowing clinics down:
Traditional RCM and EHR systems help clinics organize healthcare operations, but they do not actively manage the real-time decision complexity involved in prior authorization workflows.
Since we have now seen where operational and financial problems originate, the next step is understanding how AI prior authorization software changes the picture for mid-size clinics.
Disconnected workflows quietly drain approvals, staff hours, and reimbursement momentum every single day
Fix The Workflow BottleneckAI prior authorization software is a custom operational system that helps mid-size clinics manage insurance approval workflows before treatments, procedures, imaging requests, or medications move into the claims process. It helps clinics organize and manage prior authorization activities that usually remain scattered across payer portals, EHR screens, emails, phone calls, and manual follow-ups.
Typically, the system helps clinics manage responsibilities such as:
For mid-size clinics, this creates a centralized authorization workflow that helps administrative teams manage approvals with better process visibility and fewer disconnected steps.
An important distinction is that AI prior authorization software works as a preventive system instead of a reactive one. The purpose is to identify documentation gaps, missing payer requirements, and approval risks before claims move toward denial. Rather than investigating denied claims after revenue disruption happens, the system helps clinics reduce authorization-related issues earlier in the workflow itself.
AI prior authorization platforms handle the operational tasks involved in preparing, reviewing, submitting, and monitoring insurance authorization requests across clinical and administrative workflows. The system manages multiple process-level responsibilities that clinics traditionally handle manually during prior authorization processing.
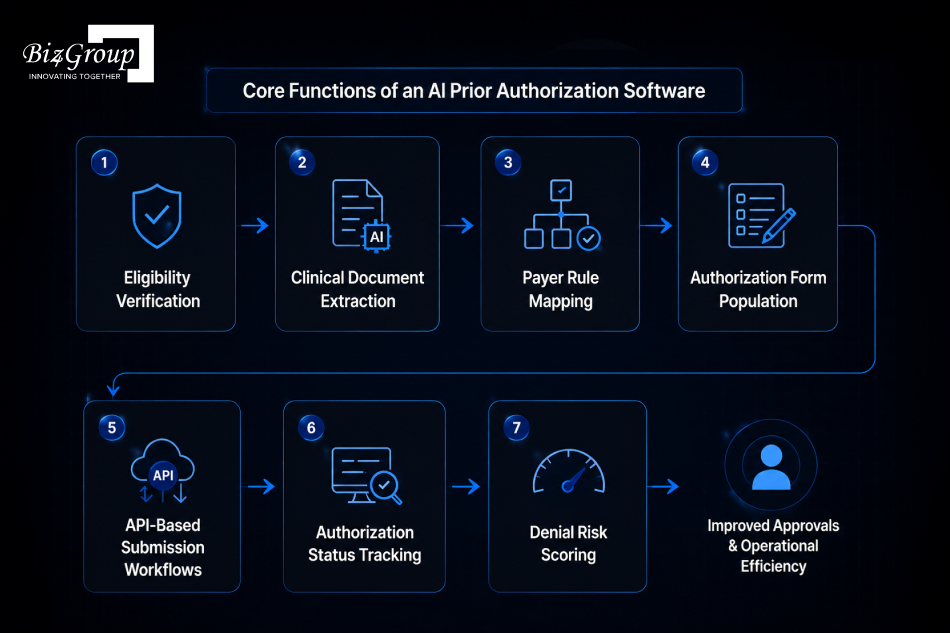
These core functions allow AI prior authorization platforms to manage critical authorization responsibilities across payer workflows, clinical documentation review, and authorization monitoring inside mid-size clinic operations.
Let intelligent authorization workflows handle repetitive review cycles before teams get overloaded
See Smart Authorization In Action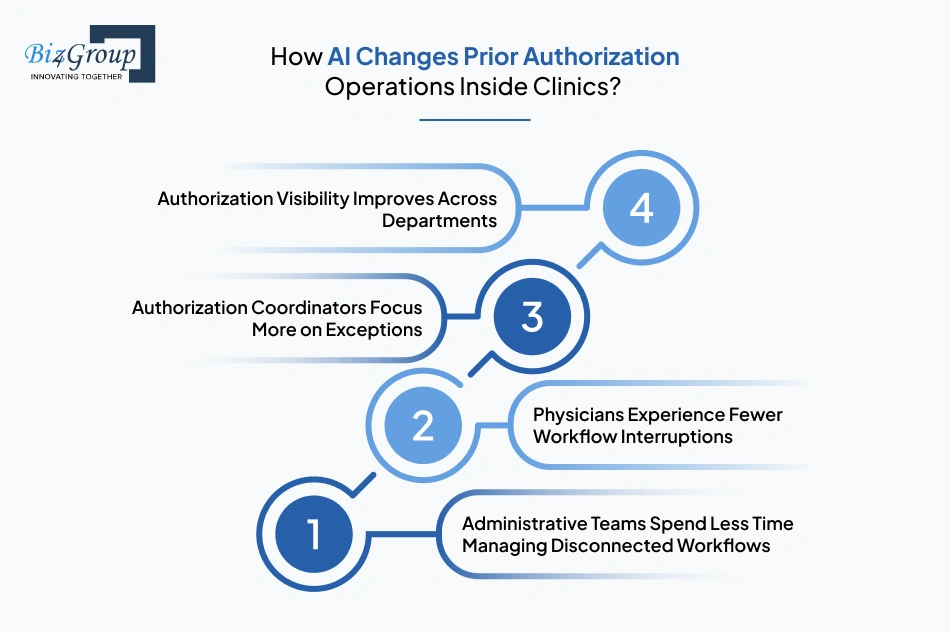
Prior authorization workflows inside mid-size clinics often involve constant coordination between physicians, front-desk teams, billing staff, referral coordinators, and insurance portals. After AI-driven authorization workflows are introduced, the operational structure inside clinics starts shifting from manual follow-up management toward guided workflow handling.
AI-driven workflows centralize authorization activities into a more structured operational environment. Operationally, this changes how teams handle daily authorization workloads:
Also Read: AI Medical Coding Software Development
Prior authorization delays often pull physicians into repeated documentation clarification requests during active patient care schedules. Operational workflows become more organized when supporting records and authorization requirements are reviewed earlier during the approval cycle.
Inside clinic operations, this often leads to:
Manual workflows usually require coordinators to manage every authorization request individually from submission through approval. Operational responsibilities begin shifting after automated review and monitoring processes are introduced into the workflow.
Instead of manually handling every request stage, coordinators spend more time managing:
Many clinics struggle with fragmented visibility during active authorization cycles because updates remain scattered across payer systems and departmental communication channels. More centralized workflow monitoring improves how teams coordinate around active requests.
Operationally, clinics gain:
As operational workflows become more structured, clinics gradually shift from manually chasing every authorization update toward managing exceptions, escalations, and high-priority cases more efficiently across departments.
Prior authorization problems eventually turn into financial problems for mid-size clinics. For clinics processing large authorization volumes every week, even small workflow inefficiencies can create significant revenue leakage over time.
As clinics evaluate a prior authorization AI automation system development for clinic operations, the discussion usually shifts from administrative workload toward measurable business impact. Here’s how it creates a measurable business impact:
Long authorization cycles often delay procedures, imaging approvals, specialty treatments, and claim submissions. When approvals move faster, clinics can stabilize scheduling workflows and reduce reimbursement delays tied to pending authorizations.
Many healthcare organizations using automated authorization workflows report nearly 60% reduction in prior authorization processing time. AI-powered systems also reduce approval turnaround from multiple days to only minutes in certain authorization workflows.
For mid-size clinics, this directly impacts:
When approval risks are identified earlier in the authorization cycle, clinics avoid a large portion of the financial waste tied to preventable denials. Fewer rejected requests mean fewer delayed reimbursements, lower claim recovery costs, and reduced revenue leakage caused by unresolved authorization issues.
For mid-size clinics processing high authorization volumes every month, stronger approval accuracy directly improves:
Automation changes the financial equation by reducing the amount of manual coordination required during authorization handling. Healthcare providers adopting automated authorization systems see nearly 35% reduction in administrative costs tied to prior authorization management.
This creates measurable financial impact through:
Healthcare organizations implementing AI automation tools for prior authorization workflows frequently report positive ROI within 3–6 months after deployment, particularly in high-volume specialty environments.
Clinics experience measurable financial improvements through:
For mid-size clinics dealing with rising authorization burdens, AI prior authorization software development for mid-size clinics is increasingly becoming a revenue protection and operational sustainability investment rather than only an administrative upgrade.
Authorization inefficiencies usually surface financially long before clinics notice operational damage
Reduce Revenue Leakage FasterPrior authorization platforms must exchange information continuously across EHR systems, payer environments, billing platforms, scheduling systems, and clinical record repositories. Integration architecture determines how accurately authorization data moves between these systems during approval processing and status management.
AI prior authorization platforms connect with EHR systems to access patient demographics, diagnosis records, physician notes, medication history, procedure details, and treatment documentation required during authorization submission workflows.
Most integrations support healthcare standards such as:
These connections allow authorization systems to synchronize patient-related information directly from clinical records without separate manual data transfer processes.
Also Read: How to Integrate AI with EHR/EMR Systems to Transform Healthcare Operations?
Prior authorization software also connects with payer communication environments to manage authorization submission activity, response updates, and approval tracking processes.
Depending on payer infrastructure, integrations usually support:
These integrations maintain authorization data exchange between clinic systems and insurance providers throughout active review cycles.
Authorization processing often involves referrals, prescriptions, physician notes, imaging reports, and scanned medical documentation stored across multiple systems. Integration workflows synchronize these records during authorization review and submission handling.
Many clinics also connect document repositories and OCR systems to process:
This keeps authorization-related documentation aligned across connected systems.
Scheduling systems and billing platforms also connect with authorization workflows to maintain synchronized approval status information during treatment coordination and reimbursement preparation.
These integrations help systems exchange:
Connected workflows reduce disconnected data handling across administrative systems.
Also Read: AI Medical Scheduling Software Development Cost
Strong integration architecture allows prior authorization platforms to exchange information consistently across healthcare systems, payer environments, and clinical record workflows. AI prior authorization software fits more effectively into clinic operations when authorization data remains synchronized across connected platforms and approval channels.
Prior authorization workflows involve multiple operational layers across payer verification, documentation review, approval coordination, and authorization tracking. AI prior authorization software development for mid-size clinics require feature planning that supports both administrative efficiency and workflow reliability across daily clinic operations.
|
Feature |
Purpose |
|---|---|
|
Clinical document extraction |
Pulls relevant patient and treatment information from uploaded records and physician notes |
|
Payer rule matching |
Reviews authorization requests against payer-specific approval conditions before submission |
|
Denial risk identification |
Flags authorization requests that may contain missing documentation or workflow gaps |
|
Automated authorization routing |
Sends requests through the correct payer workflow based on insurance requirements |
|
Smart workflow prioritization |
Helps teams identify urgent or time-sensitive authorization cases faster |
|
Feature |
Purpose |
|
Centralized authorization dashboard |
Gives teams one place to monitor active requests and pending approvals |
|
Authorization queue management |
Organizes requests based on status, urgency, payer type, or department workflows |
|
Escalation workflow handling |
Routes delayed or exception-based cases for manual review when needed |
|
Approval status monitoring |
Tracks authorization progress across payer review cycles |
|
Task assignment controls |
Helps managers distribute authorization workloads across staff members |
|
Feature |
Purpose |
|---|---|
|
Supporting document validation |
Reviews whether required records are attached before submission |
|
Physician note synchronization |
Pulls clinical notes into authorization workflows automatically |
|
ICD and CPT code verification |
Checks whether diagnosis and procedure codes align correctly during submission preparation |
|
Missing information alerts |
Identifies incomplete authorization requests before payer review begins |
|
Multi-document management |
Organizes referrals, imaging records, prescriptions, and supporting files together |
|
Feature |
Purpose |
|---|---|
|
Multi-payer workflow support |
Handles authorization requirements across different insurance providers |
|
API-based authorization submission |
Sends authorization requests electronically through connected payer systems |
|
Real-time eligibility verification |
Checks active patient coverage and authorization requirements instantly |
|
Payer response synchronization |
Updates authorization status automatically after payer review activity |
|
Portal workflow support |
Supports payer workflows that still require external portal processing |
|
Feature |
Purpose |
|---|---|
|
Role-based access management |
Restricts authorization data access based on staff responsibilities |
|
Audit trail logging |
Records workflow activity and authorization-related actions for compliance review |
|
Encrypted data handling |
Protects patient records during storage and workflow transmission |
|
Multi-factor authentication |
Adds additional login protection for sensitive healthcare workflows |
|
Session monitoring controls |
Tracks user activity during authorization handling workflows |
The right feature structure helps clinics manage authorization operations more consistently as payer complexity and approval volumes continue increasing. Teams planning to build AI prior authorization software for clinics usually achieve better long-term workflow stability when operational, payer, and compliance requirements are addressed together during feature planning.
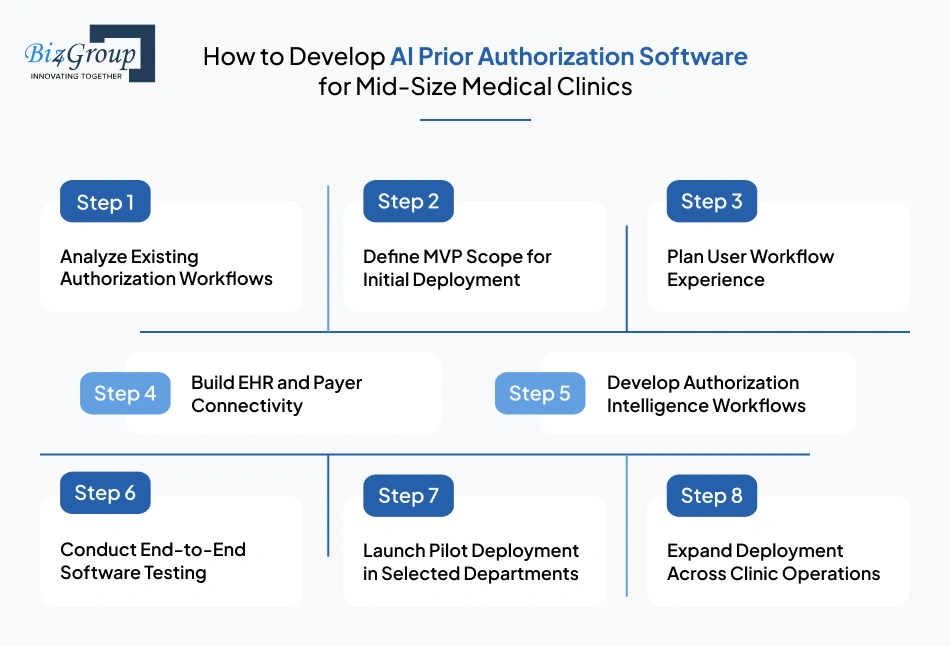
Prior authorization workflows vary significantly across specialties, payer environments, and clinic operations. That is why clinics planning to develop AI prior authorization software for medical clinics need a structured development roadmap that aligns technical execution with real approval dependencies, and reimbursement requirements.
The development process starts with operational workflow discovery. Development teams work with billing managers, authorization coordinators, physicians, and administrators to understand how prior authorization currently moves through the clinic.
This stage usually includes:
Clear workflow mapping helps prevent unnecessary system complexity during development.
Most mid-size clinics begin with a focused rollout instead of building a large-scale system immediately. Teams often work with providers offering MVP development services to define the minimum operational workflows required for launch.
The initial MVP generally focuses on:
This approach helps clinics validate operational performance before expanding system scope.
Also Read: Top MVP Development Companies in USA
Prior authorization systems are used daily by coordinators, billing staff, schedulers, and physicians. Workflow usability directly affects adoption inside clinics. During this phase, teams often collaborate with a UI/UX design company to structure practical workflow experiences around real authorization operations.
The design process usually includes:
Operational simplicity becomes critical during high-volume authorization handling.
Also Read: Top UI/UX Design Companies in USA
Once workflow planning is complete, development teams begin connecting the system with EHR platforms, payer communication channels, and authorization data workflows.
This stage generally includes:
Reliable data movement becomes essential before automation workflows are activated.
After connectivity is established, teams begin configuring operational logic that supports authorization handling across payer workflows. This is where AI automation tools are integrated into authorization processing activities.
The development phase commonly includes:
Operational workflows are usually refined continuously during this phase.
Prior authorization workflows involve sensitive patient, payer, and reimbursement data. Before launch, clinics typically work alongside internal QA teams or external software testing companies to validate workflow accuracy across different authorization scenarios.
Testing workflows generally focus on:
Testing helps reduce operational disruption after deployment.
Also Read: Top AI Software Development Companies in USA
Instead of releasing the platform clinic-wide immediately, most organizations begin with a controlled rollout inside one specialty or operational department.
Pilot deployment usually helps clinics:
Pilot environments provide operational feedback before broader expansion.
After pilot validation, clinics gradually extend the platform into additional specialties, payer environments, and administrative teams. Operational workflows continue evolving as authorization volumes increase, and payer requirements change over time.
Expansion stages commonly include:
A structured rollout strategy helps clinics maintain workflow stability while scaling authorization operations across departments.
Developing a successful authorization platform requires more than workflow automation alone. AI prior authorization software development for mid-size clinics depends heavily on operational alignment, realistic rollout planning, workflow usability, and long-term adaptability across changing payer environments.
Strong authorization systems succeed when operational planning happens before development begins
Plan Your Automation RoadmapFor custom prior authorization software development for mid clinics, the tech stack needs to support secure data flow, fast document handling, and reliable workflow logic. That is where the right mix of web development and mobile development tools starts shaping the system.
|
Architecture Layer |
Recommended Tool |
Purpose |
|---|---|---|
|
Presentation Layer |
React with Next.js |
Presents the authorization dashboard to clinic staff and gives them a clear interface for reviewing cases, managing queues, and handling daily workflows. |
|
Workflow Orchestration Layer |
Temporal or Camunda |
Controls how authorization tasks move from one step to another, so approvals, reviews, and escalations follow a consistent process. |
|
Backend API Layer |
Python with FastAPI |
Python development processes application requests, applies business logic, and connects the front end with the rest of the system. |
|
Rules Engine Layer |
Drools or a custom Python rules service |
Evaluates payer-specific approval logic and determines whether a request meets the required authorization conditions. |
|
Document Ingestion Layer |
Tesseract OCR with Python |
Reads scanned documents, faxed records, and PDFs so the system can extract usable information from unstructured files. |
|
AI Processing Layer |
PyTorch or TensorFlow |
Supports document classification, information extraction, and approval risk scoring using machine learning models. |
|
Integration Layer |
Mirth Connect with FHIR APIs |
Transfers data between the software, EHR systems, and payer-connected services in a structured healthcare format. |
|
Database Layer |
PostgreSQL |
Stores patient data, authorization history, payer rules, workflow records, and other structured information safely. |
|
Cache and Queue Layer |
Redis with RabbitMQ |
Manages background tasks, keeps status updates moving, and helps the system handle high request volumes efficiently. |
|
Security Layer |
Keycloak with encryption services |
Controls user access and protects patient information through authentication, encryption, and permission management. |
|
Audit Logging Layer |
Elasticsearch or PostgreSQL audit tables |
Records user actions and workflow events so the clinic can maintain traceability and compliance visibility. |
|
Analytics Layer |
Metabase or Grafana |
Displays operational metrics so teams can monitor performance, delays, approval trends, and workload patterns. |
|
Monitoring Layer |
Prometheus with Grafana |
Tracks system health, performance issues, and technical errors so problems can be identified early. |
|
Deployment Layer |
Docker with Kubernetes on AWS |
Manages application deployment, scaling, and release stability across clinic operations. |
This stack gives AI prior authorization platform development a clean base for speed, security, and scale. With full stack development handled well, clinics get a system that stays stable, readable, and ready for future workflow growth.
Also Read: Why to Choose the Full Stack Development for Modern Business
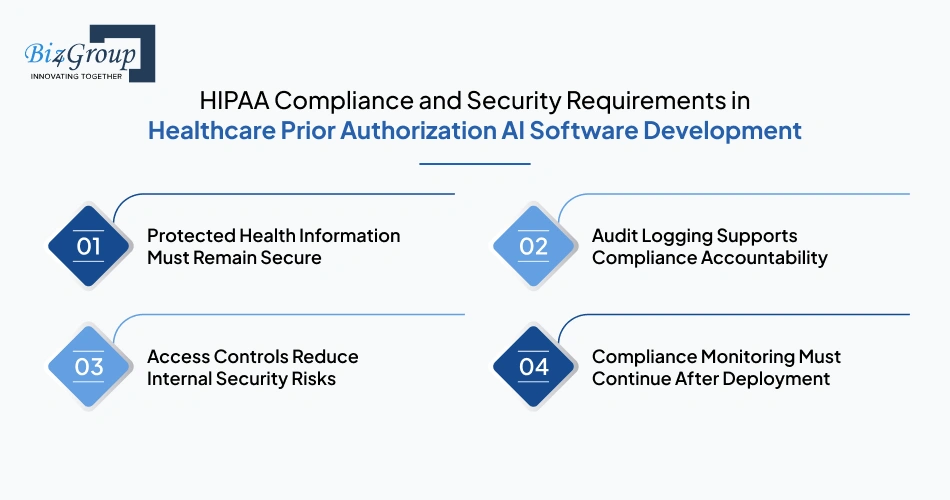
Patient authorization workflows involve large volumes of protected health information moving across clinical records, insurance documentation, administrative reviews, and payer communication channels. That is why clinics planning to develop a HIPAA compliant AI prior authorization automation system for medical practices processing high volumes of authorization requests must treat security planning as part of the core software architecture from the beginning.
Prior authorization systems continuously process patient names, diagnosis records, insurance details, treatment plans, physician notes, and supporting medical documentation. Every stage of the workflow must protect this information against unauthorized access and data exposure.
A secure authorization platform generally includes:
Security controls must remain active across both internal workflows and external payer communication channels.
Authorization workflows involve multiple administrative actions during document review, submission handling, approval updates, and status management. Clinics need complete visibility into who accessed records, modified workflows, or reviewed patient information during authorization processing.
Audit logging usually helps organizations:
Detailed activity tracking becomes especially important during payer disputes and compliance reviews.
Not every staff member inside a clinic should have unrestricted access to authorization-related patient information. Access permissions must align with operational responsibilities across departments.
Most HIPAA compliant AI software environments restrict access based on:
Structured access management helps clinics reduce unnecessary exposure to sensitive patient records.
Also Read: HIPAA Compliant AI App Development for Healthcare Providers
Healthcare compliance does not end after software launch. Authorization workflows continue evolving as payer requirements, operational policies, and healthcare regulations change over time. Clinics working with providers offering AI automation services typically maintain ongoing compliance reviews alongside operational updates.
Long-term compliance management often includes:
Maintaining compliance readiness requires continuous operational oversight after deployment.
Strong compliance architecture protects more than patient information alone. AI prior authorization software development for mid-size clinics also depends on maintaining operational trust, audit readiness, and long-term security stability across daily authorization workflows.
The overall budget for clinics planning prior authorization AI automation software development for mid-size clinics usually depends on workflow complexity, payer connectivity requirements, compliance planning, and automation depth. Most projects fall between $40,000 and $350,000+ depending on deployment scope, specialty coverage, and operational scale.
|
Development Level |
Estimated Cost Range |
Scope |
|---|---|---|
|
MVP Level AI Prior Authorization Software |
$40,000–$80,000 |
Covers core authorization workflows, limited payer support, basic dashboards, and initial automation for one specialty or department |
|
Mid-Level System AI Prior Authorization Software |
$80,000–$150,000 |
Includes broader payer workflows, EHR connectivity, approval tracking, workflow automation, and multi-department support |
|
Advanced Level AI Prior Authorization Software |
$150,000–$350,000+ |
Supports multi-location operations, advanced AI processing, high-volume authorization management, analytics, and enterprise-grade compliance architecture |
The cost changes based on how many EHR systems the platform must connect with and how deep the data exchange needs to be. A simple one-way connection costs much less than a two-way workflow that pulls patient data, updates authorization status, and keeps records synced across departments.
Estimated cost impact: $10,000–$60,000
Also Read: How Much Does It Cost to Develop an AI EHR Software?
Every payer has its own approval rules, documentation patterns, and submission flow. The more payer types the system needs to support, the more development time goes into rule mapping, workflow handling, and exception management. Clinics with mixed commercial and government payers usually need a larger budget here.
Estimated cost impact: $15,000–$70,000
A basic system can route requests and organize documents. A more advanced platform can extract clinical details, flag missing information, and score denial risk before submission. The deeper the automation, the more model training, testing, and workflow refinement the project needs.
Estimated cost impact: $20,000–$90,000
Healthcare software must protect patient data and maintain audit readiness. Costs rise when the project needs stronger access controls, audit trails, encryption layers, and policy documentation. Clinics handling sensitive records across multiple teams usually need a more robust setup.
Estimated cost impact: $10,000–$50,000
Some clinics want a standard prior authorization flow. Others need specialty-specific routing, approval exceptions, and department-level variations. The more closely the software must fit existing clinic operations, the more design and development work it takes increasing AI integrations cost.
Estimated cost impact: $15,000–$80,000
A system built for one clinic site costs less than one built for multiple locations or heavy request volume. Costs increase when the platform must handle more users, more submissions, more document traffic, and more background processing without slowing down.
Estimated cost impact: $10,000–$40,000
Basic reporting is usually cheaper. More detailed dashboards that track denial trends, approval delays, staff workload, and payer performance require additional development. Clinics that want stronger visibility into revenue cycle performance usually invest more here.
Estimated cost impact: $5,000–$25,000
|
Hidden Costs |
Where Cost Goes |
Estimated Cost Impact |
|---|---|---|
|
Payer workflow updates |
Continuous authorization rule maintenance |
$5,000–$25,000 annually |
|
Staff onboarding |
Workflow training and operational transition |
$3,000–$15,000 |
|
Compliance reviews |
Security audits and policy validation |
$5,000–$20,000 |
|
Infrastructure scaling |
Cloud expansion and storage growth |
$2,000–$18,000 annually |
|
Workflow optimization |
Post-launch operational adjustments |
$5,000–$30,000 |
Cost planning becomes more manageable when clinics align development scope with authorization volume and long-term workflow expansion goals. AI prior authorization system development for mid-size clinics works best when the investment strategy stays practical, phased, and operationally aligned from the beginning.
Also Read: How Much Does AI Software Development Cost?
Authorization platforms cost less when rollout priorities and workflow boundaries stay clearly defined
Estimate Your Real Project Cost
Operational realities inside mid-size clinics often make authorization automation more complicated than expected. During healthcare prior authorization AI software development, challenges usually appear around payer variability, workflow alignment, staff adoption, and long-term system maintenance.
Addressing these issues early helps clinics avoid operational disruption after deployment.
|
Challenges |
How to Solve Them |
|---|---|
|
Different payers follow different authorization workflows |
Configure payer-specific approval logic during workflow planning instead of forcing one universal process across every insurance provider. |
|
Clinical documentation remains inconsistent across departments |
Standardize documentation formats early and involve physicians during workflow review before building AI processing logic. |
|
Staff members resist operational workflow changes |
Introduce automation gradually through department-level rollout instead of replacing entire workflows at once. |
|
Authorization queues become difficult to manage during high request volumes |
Implement centralized queue visibility and workload prioritization during workflow architecture planning. |
|
EHR data quality issues affect authorization processing |
Validate patient records, coding accuracy, and clinical documentation quality before automation workflows are activated. |
|
Clinics underestimate workflow customization requirements |
Work with teams experienced in AI product development services so operational workflows reflect real clinic authorization processes. |
|
Internal technical teams lack healthcare workflow expertise |
Partnering with a custom software development company familiar with healthcare operations helps reduce workflow design errors early in development. |
|
AI workflow refinement takes longer than expected |
Clinics planning long-term automation projects should hire AI developers who understand healthcare documentation and payer approval logic. |
|
Operational workflows break after payer rule updates |
Maintain ongoing workflow monitoring and update payer rule logic regularly after deployment instead of treating automation as a one-time setup. |
|
Expanding the platform across multiple specialties becomes difficult |
Structure the rollout in phases while building AI software so workflows can be adjusted gradually across departments. |
Also Read: Cost to Hire an AI Software Developer in 2026
Successful automation projects usually depend less on software alone and more on how realistically the operational workflows are planned from the beginning. AI prior authorization software development for healthcare for clinics works best when technical execution stays closely aligned with daily authorization operations inside the clinic.
Once prior authorization workflows move into daily operations, clinics need clear performance visibility across approvals, payer response cycles, administrative workload, and workflow accuracy.
That is why AI prior authorization software development for mid-size clinics should include structured KPI monitoring from the beginning instead of relying only on operational assumptions.
Consistent KPI monitoring gives clinics a clearer operational view of how authorization workflows perform after deployment. AI prior authorization management software development becomes easier to manage when teams continuously track approval patterns, workflow delays, and operational exceptions across departments.
Many mid-size clinics reach a point where operational pressure turns into financial risk. Questions like, “we are losing approximately $400,000 annually in denied prior authorization claims because our manual submission process frequently misses payer specific documentation requirements. We need to find a development company that can build us an AI prior authorization system that checks documentation completeness before every submission?” are becoming increasingly common across healthcare organizations handling high authorization volumes.
That is where Biz4Group LLC becomes a strong execution partner. As a HIPAA compliant AI healthcare software development company, the team focuses on operational healthcare automation systems aligned with real clinical workflows, payer requirements, and administrative challenges faced by mid-size clinics. Here’s what we possess:
Prior authorization workflows involve much more than software development alone. We work closely with healthcare organizations to understand payer complexity, approval bottlenecks, documentation dependencies, and administrative coordination challenges before development begins.
This operational understanding becomes especially important during medical clinic prior authorization AI development projects where workflow accuracy directly affects reimbursements and patient scheduling.
Healthcare authorization systems sit directly between clinical operations and insurance workflows. We have experience working on AI insurance automation software solutions that involve workflow automation, document handling, payer coordination, and operational process optimization across healthcare environments. Still not convinced here’s the proof:
Every clinic handles authorizations differently based on specialties, payer mix, staffing structure, and approval complexity. We focus on workflow-specific system design instead of forcing clinics into rigid templates.
Our teams structure authorization platforms around:
Many clinics understand the operational problems they face but struggle to define the right rollout strategy. Through structured AI consulting services, we help organizations plan automation scope, workflow priorities, operational rollout phases, and long-term scalability before engineering work begins. This reduces unnecessary development expansion during early project stages.
Healthcare organizations often evaluate execution capability before committing to long-term automation investments. We maintain an extensive AI portfolio covering healthcare automation, operational workflow systems, AI-powered process management, and enterprise-grade custom platforms across multiple industries.
This gives clinics better visibility into practical AI implementation experience before starting development.
Successful authorization automation projects require more than software engineering alone. Biz4Group LLC works as a long-term execution partner for mid-size clinics by aligning healthcare workflows, payer requirements, and scalable AI implementation into one structured development approach for prior authorization automation.
Prior authorization problems rarely stay limited to administrative teams. Over time, they start affecting scheduling, reimbursements, physician coordination, and overall workflow stability inside the clinic. That is why many healthcare organizations now view AI prior authorization software development for mid-size clinics as a practical operational move instead of a long-term experimental initiative.
The real goal is not simply automation. It is creating a more reliable authorization process that reduces manual dependency and keeps approval workflows easier to manage as payer complexity grows. An experienced AI development company can help clinics approach that transition with clearer operational planning and realistic implementation strategies.
That is where Biz4group LLC supports mid-size clinics through structured workflow planning, healthcare-focused execution, and intelligent prior authorization software development aligned with real operational requirements.
To discuss your clinic’s authorization challenges and automation goals, schedule a consultation call with us today.
Modern authorization platforms use configurable payer-rule workflows that can be updated without rebuilding the entire system. This helps clinics adapt faster when insurance providers change documentation requirements, approval criteria, or submission conditions across specialties.
Yes. Many specialty clinics use AI prior authorization system development to manage high-complexity approvals tied to imaging, oncology, cardiology, orthopedic procedures, and specialty medications. The workflows can be customized around specialty-specific documentation and payer requirements.
The cost usually ranges between $40,000 and $350,000+ depending on workflow complexity, payer integrations, automation depth, compliance requirements, specialty coverage, and operational scale across clinic locations.
Most projects take around 4-16+ weeks depending on the development scope. Smaller MVP-level systems generally move faster, while enterprise-grade prior authorization automation software development projects require additional time for integrations, testing, compliance validation, and workflow customization.
Yes. Most healthcare prior authorization AI software development projects are designed to work alongside existing EHR infrastructure instead of replacing it entirely. The software typically connects with current workflows through APIs, healthcare data standards, and operational middleware.
Clinics should first identify their highest-volume authorization workflows, denial-prone payer environments, documentation bottlenecks, and operational escalation patterns. Clear workflow mapping usually prevents unnecessary customization delays during development.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.