Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Let us start with a question you have probably asked yourself more than once - Why does running a healthcare practice feel more complicated every year, even when you are investing in new tools?
If this sounds familiar, you are not imagining it.
This is exactly why healthcare practice management software development has moved from a nice-to-have to a business priority.
Here is what the data tells us.
The global practice management system market is projected to grow $13.76 billion, driven largely by clinics and hospitals in North America adopting digital operations tools.
At the same time, the broader medical software market is projected to cross $67 billion, showing how fast healthcare organizations are investing in smarter systems.
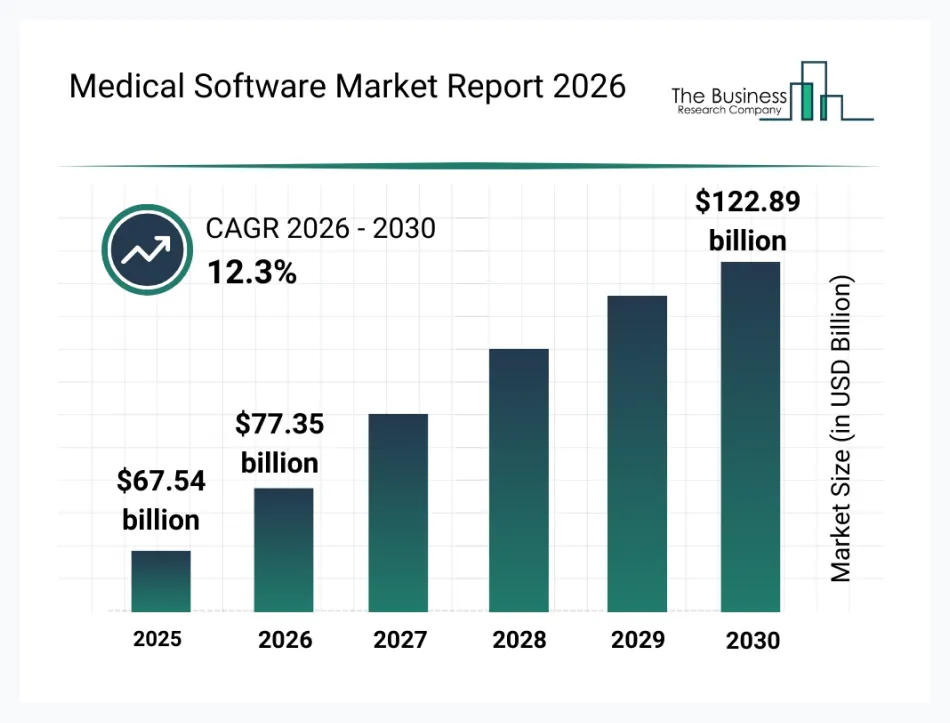
So, here is the real question - If investment is growing this fast, why does day-to-day operations still feel messy on the ground?
Most practices begin with disconnected tools. Scheduling in one system. Billing in another. Reports living in spreadsheets no one fully trusts. That setup might work early on, but growth exposes the cracks fast.
This is where developing healthcare practice management software becomes a strategic decision, not just a technical one.
You are no longer asking, “What software can we buy?”, instead you are asking, “How do we build healthcare practice management systems that actually fit how our teams work?”
This challenge is closely tied to staffing and operational efficiency. Many organizations see faster improvements when practice systems align with healthcare workforce management software, where schedules, workloads, and resources finally move in sync instead of competing with each other.
Whether your goal is to create medical practice management software for a growing clinic or plan healthcare practice management platform development for a larger organization, everything starts with understanding the real problem you are trying to solve.
So, before we talk about features or technology, let us step back.
What exactly is healthcare practice management software, and why has it become impossible for modern providers to ignore?
If scheduling, billing, and growth feel harder than they should, it is time to rethink your systems.
Let's TalkLet us simplify this.
Healthcare practice management software is the operational engine of your healthcare organization. It manages everything that happens before, around, and after patient care, from scheduling and registration to billing, insurance processing, and performance reporting.
If your EHR documents clinical care, your practice management system runs the business.
When you invest in healthcare practice management software development, you are building a centralized system that connects your front desk, billing team, operations leaders, and finance department. Instead of juggling disconnected tools, your workflows live in one structured environment.
Many healthcare leaders decide to develop healthcare practice management software when they realize off the shelf systems do not reflect how their teams actually work. Growth makes this gap visible fast. What worked for 10 providers does not hold up at 40.
That is why organizations choose to build healthcare practice management systems tailored to their billing models, staffing structure, and expansion plans.
Today, many platforms are delivered as scalable healthcare SaaS solutions, giving you flexibility without heavy infrastructure overhead. But SaaS alone is not the answer. The real value comes from software that aligns with how your operations actually function.
This is why custom healthcare practice management software development is no longer a technical decision. It is a business decision tied directly to efficiency, compliance, and sustainable growth.
Next, we will look at practical use cases where healthcare organizations see measurable results after implementing the right practice management system.
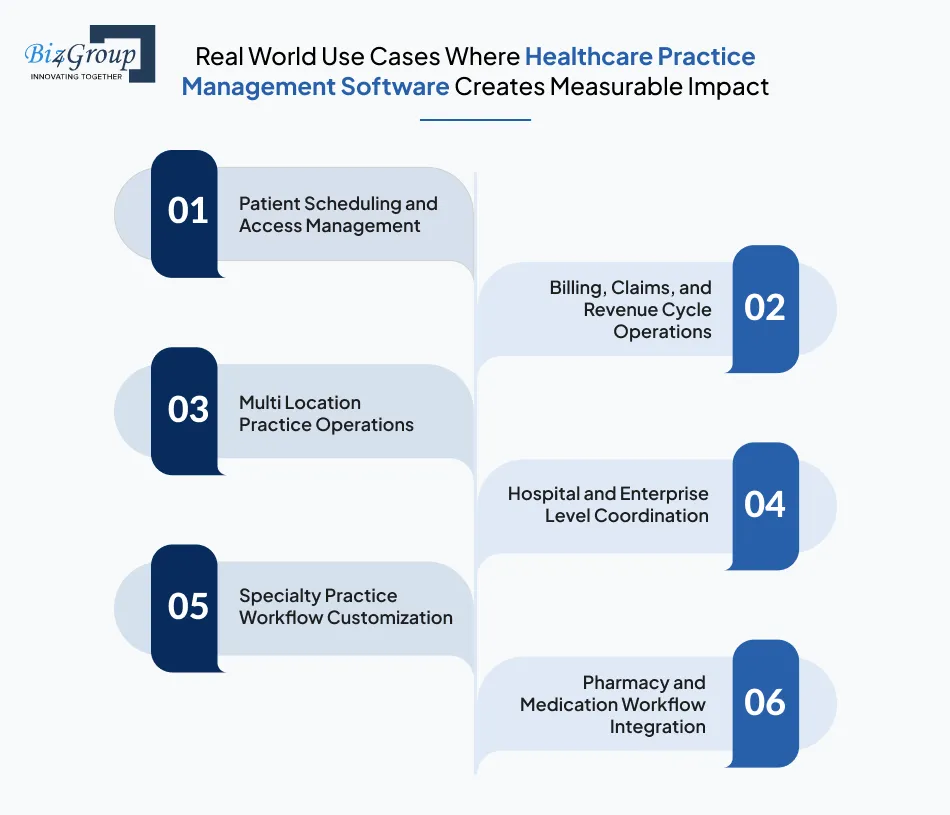
Use cases matter because this is where healthcare practice management software development turns into real operational results. These are not theoretical scenarios. They are the exact problems clinics, hospitals, and healthcare groups solve every day with the right system in place.
Scheduling is usually the first place where operations start to break down. As patient volume increases, manual coordination leads to overlaps, no shows, and underused provider time. When you develop healthcare practice management software, scheduling becomes structured and predictable.
Core features supporting this use case:
Revenue issues often come from slow or error prone billing workflows. Many practices invest in custom healthcare practice management software development when generic billing tools cannot handle payer complexity or specialty requirements. Here, AI medical billing software helps these companies in streamlining the operations.
Core features supporting this use case:
Running multiple clinics without centralized systems quickly leads to inconsistency. Reporting becomes fragmented and leadership loses visibility. This is where organizations build healthcare practice management systems designed to scale across locations.
Core features supporting this use case:
Hospitals deal with higher volumes, more departments, and stricter oversight. Healthcare practice management software development for hospitals focuses on coordination and control at scale.
Core features supporting this use case:
Specialty practices often follow unique care and billing models. Off the shelf systems rarely support this well. That is why many specialists choose to create medical practice management software aligned with their workflows.
Core features supporting this use case:
Practices that handle prescriptions or operate alongside pharmacies need tighter coordination. Integrating practice operations with pharmacy management software reduces medication errors, billing mismatches, and inventory gaps.
Core features supporting this use case:
Across all these use cases, the objective is the same - simpler workflows, better visibility and systems that scale without adding operational burden.
Now, we will see the core features every healthcare practice management system must include to support these use cases effectively.
Also Read: Healthcare Kiosk Software Development
When you invest in healthcare practice management software development, these are the non negotiable building blocks. If any of these features are weak or missing, operational issues will surface no matter how good the rest of the system looks.
A practice management system must include a centralized scheduling engine that manages providers, locations, services, and resources in one place. It should support real-time availability updates and prevent conflicts automatically. When you develop healthcare practice management software, scheduling must work at scale without manual oversight. This feature directly impacts patient access and provider utilization.
Patient registration should be handled through structured digital workflows that capture demographic, insurance, and consent data accurately. This feature eliminates repetitive data entry and reduces front desk dependency. In custom healthcare practice management software development, intake logic is tailored to your operational flow. Clean intake data is essential for downstream billing and reporting accuracy.
Billing functionality must be built directly into the practice management system, not bolted on later. This includes coding support, claim generation, submission workflows, and payment tracking. Organizations often choose to make healthcare practice management software with billing integration to avoid revenue leakage caused by disconnected systems. Billing is where operational efficiency turns into financial performance.
Eligibility verification and prior authorization management must be automated within the platform. This feature ensures payer rules are validated before services are delivered. When you develop healthcare billing and scheduling software together, insurance logic becomes proactive instead of reactive. This reduces claim denials and patient billing disputes.
A practice management system must integrate seamlessly with clinical systems to exchange patient and visit data. While it does not replace clinical documentation, it must stay synchronized with AI EMR/EHR software to avoid data gaps. Integration ensures that operational workflows align with care delivery. Without this layer, duplicate work and errors increase rapidly.
Document handling should be centralized, searchable, and securely managed within the platform. Integration with AI medical records management software improves accuracy, retrieval speed, and compliance readiness. This feature supports long term scalability when you create scalable medical practice management systems. Paper-driven workflows do not scale in healthcare.
Every practice management system must include built in reporting for scheduling, billing, and performance metrics. Dashboards should update in near real time to support decision making. Many organizations extend this capability using AI healthcare analytics software for deeper operational insight. Without analytics, leadership operates on assumptions instead of data.
The platform must enforce role based access, audit trails, and secure data handling across all workflows. Building systems that are HIPAA compliant is mandatory, not optional. This feature protects patient data and reduces organizational risk. Compliance must be designed into the system, not layered on later.
Usability is a core feature, not a design preference. The system must be intuitive for front desk staff, billing teams, and administrators. Strong design ensures faster adoption and fewer operational errors. If users struggle, the software will fail regardless of features.
Once the foundational system is stable, advanced capabilities are what elevate healthcare practice management software development from operational support to strategic advantage. These features are designed for organizations that want to scale, optimize, and compete intelligently.
|
Advanced AI Capability |
How It Works in Practice Management Software |
Business Value for Providers |
|---|---|---|
|
AI Predictive Scheduling Intelligence |
Uses historical appointment data, provider behavior, and patient attendance patterns to predict no shows and optimize time slots automatically |
Helps clinics build healthcare practice management systems that increase utilization and reduce lost revenue without adding staff |
|
Revenue Risk Prediction Models |
Applies machine learning to billing and claims data to flag denial risks before claims are submitted |
Strengthens cash flow and supports develop healthcare practice management systems for operational efficiency |
|
Predictive Staffing and Workload Forecasting |
Forecasts patient demand, visit types, and staffing requirements weeks in advance |
Enables leadership to plan staffing proactively when they build custom healthcare practice management software for clinics |
|
Autonomous Workflow Orchestration |
Executes multi step operational workflows across scheduling, billing, and follow ups without human intervention |
Reduces administrative workload and supports scalable healthcare practice management platform development through AI automation services |
|
Conversational AI for Operational Tasks |
Handles appointment changes, billing questions, and intake interactions using natural language |
Improves patient experience and reduces call volume using an AI chatbot |
|
Automatically extracts structured data from referrals, forms, and scanned documents |
Speeds up onboarding and documentation when organizations create medical practice management software |
|
|
Cross System AI Synchronization |
Monitors data changes across systems and resolves mismatches automatically |
Ensures consistency across platforms during medical practice software application development with AI integration services |
|
Self-Improving Analytics Models |
Learns from operational outcomes to continuously improve forecasts and recommendations |
Enhances leadership decision making through AI healthcare analytics software |
|
Autonomous Decision Agents |
Observes operational patterns and initiates corrective actions without manual prompts |
Enables continuous optimization using an AI agent |
|
Goal Oriented AI Execution |
Executes complex multi system tasks aligned with defined business goals |
Supports advanced automation strategies through agentic AI development |
|
Custom AI Models for Practice Operations |
Trains AI models on your organization’s unique operational data |
Differentiates platforms through custom AI healthcare software and supports long term growth |
|
Enterprise Scale AI Governance |
Manages AI access, behavior, and performance across departments and locations |
Essential for enterprise practice management system development for hospitals using enterprise AI solutions |
Advanced AI is not about adding complexity. It is about removing uncertainty. When healthcare organizations create scalable medical practice management systems, these capabilities allow them to predict issues before they occur, automate decisions safely, and operate with far greater precision.
This is why forward looking providers treat AI as a core part of healthcare practice management software development, not a future add on.
If not, your software may be holding your team back instead of helping them move faster.
Talk to Our Experts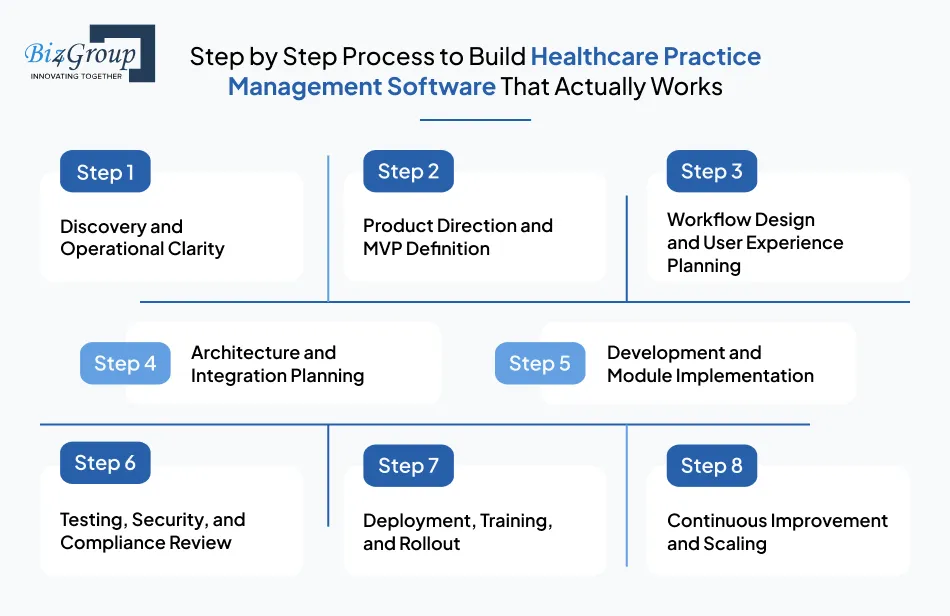
Successful healthcare practice management software development follows a disciplined process. Whether you are planning to develop healthcare practice management software for a clinic or an enterprise rollout, these steps help you avoid rework, control cost, and build a system your teams actually use.
This step defines what you are really building and why. Teams analyze workflows, billing operations, compliance needs, and growth plans to ensure the foundation is solid. This clarity is critical when you aim to build healthcare practice management systems that reflect real operational needs.
Key activities in this step:
Rather than building everything at once, teams define a focused first release that delivers immediate value. This is a practical answer to how to develop healthcare practice management software without unnecessary risk. Many organizations begin with MVP development to validate assumptions early.
Key activities in this step:
Adoption depends on usability. This step focuses on designing workflows that match how staff actually work, reducing training time and resistance. Strong UI/UX design is essential when you create medical practice management software for busy clinical teams.
Key activities in this step:
Here, teams define how the system will scale securely and integrate with other healthcare platforms. Architecture decisions are especially important for healthcare practice management software development for hospitals and multi-location clinics.
Key activities in this step:
With a clear plan in place, development moves forward in iterations. Core modules like scheduling and billing are built first, followed by advanced capabilities. This stage is where teams make healthcare practice management software with billing integration instead of treating billing as an afterthought. Many organizations work with a trusted custom software development company to ensure healthcare domain expertise.
Key activities in this step:
Healthcare platforms must perform reliably and protect sensitive data. Testing validates functionality, performance, and compliance readiness, especially for organizations pursuing custom healthcare practice management software development.
Key activities in this step:
Deployment is where planning meets reality. Data is migrated, teams are trained, and performance is monitored closely. This step is critical when you create healthcare practice management software for multi-location clinics to avoid operational disruption.
Key activities in this step:
Once live, real usage data guides improvement. Enhancements are rolled out gradually to support growth. This approach helps organizations create scalable medical practice management systems that evolve with operational needs. Some teams expand internal capabilities by choosing to hire AI developers as requirements mature.
Key activities in this step:
Choosing the right technology stack is not about chasing trends. It is about reliability, security, scalability, and long-term maintainability. A well-planned stack ensures your healthcare practice management software development effort supports growth instead of creating technical debt.
Below is a practical view of the technology layers commonly used when teams develop healthcare practice management software for clinics, hospitals, and healthcare groups.
|
Technology Layer |
Common Tools and Frameworks |
Why This Layer Matters |
|---|---|---|
|
Frontend Applications |
React, Angular, Vue.js, Next.JS |
These frameworks support fast, responsive user interfaces for scheduling, billing, and administrative workflows. They are widely used to create medical practice management software that staff can learn quickly and use daily. |
|
Backend Development |
Backend services handle business logic, billing rules, scheduling engines, and data processing. A strong backend is essential to build healthcare practice management systems that remain stable under high usage. |
|
|
Database Management |
PostgreSQL, MySQL, MongoDB |
Databases store patient, billing, and operational data securely. The right database design is critical when teams want to create scalable medical practice management systems that grow without performance issues. |
|
Cloud Infrastructure |
AWS, Microsoft Azure, Google Cloud |
Cloud platforms enable scalability, high availability, and disaster recovery. They are commonly used in healthcare practice management platform development to support multi-locate clinics and hospitals. |
|
API and Integration Layer |
REST APIs, HL7, FHIR |
Integrations connect practice management systems with EHRs, billing platforms, labs, and third party tools. This layer is key for medical practice software application development that avoids data silos. |
|
Security and Compliance Tools |
Encryption frameworks, IAM, audit logging tools |
Security tools protect sensitive healthcare data and support regulatory compliance. They are mandatory when building systems used across clinics and hospitals. |
|
AI and Data Processing |
TensorFlow, PyTorch, Python ML libraries |
AI components support predictive scheduling, analytics, and automation. These capabilities are often built as part of AI app development to enhance operational intelligence. |
|
Analytics and Reporting |
Power BI, Tableau, custom dashboards |
Reporting tools give leadership real time visibility into operations and revenue. This layer supports decision making across departments and locations. |
|
DevOps and Monitoring |
Docker, Kubernetes, CI/CD pipelines |
DevOps tools ensure smooth deployments, faster updates, and system reliability. They are critical for organizations managing ongoing enhancements. |
The best stack is the one that fits your operational reality, clinics often prioritize speed and simplicity. Hospitals focus on scalability, integration, and governance.
When teams align technology decisions with business goals, healthcare practice management software development becomes easier to maintain and far more effective over time.
Now the main question arises: how much does it cost to develop healthcare practice management software? Let’s take a look at that as well.
Also Read: React JS Development Services
Before you commit to healthcare practice management software development, you need a realistic view of cost. Most organizations underestimate this step, not because pricing is unclear, but because costs vary widely based on scope, complexity, and long-term goals.
As a reference point, the estimated cost to develop healthcare practice management software typically ranges between $40,000 to $300,000+. This range exists because a simple clinic system and an enterprise hospital platform are two very different products.
Let us break this down clearly.
|
Feature Area |
Estimated Cost Range |
What Drives the Cost |
|---|---|---|
|
Core Scheduling and Patient Management |
$8,000 to $20,000 |
Calendar logic, provider availability rules, patient intake workflows |
|
Billing, Coding, and Claims Processing |
$12,000 to $35,000 |
Payer complexity, billing rules, claim automation, reporting depth |
|
Insurance Eligibility and Authorization |
$6,000 to $15,000 |
Real-time eligibility checks, payer integrations, rule validation |
|
Multi-Location and Role Management |
$8,000 to $25,000 |
Number of clinics, access control logic, centralized reporting |
|
Reporting and Dashboards |
$5,000 to $20,000 |
Custom KPIs, financial views, operational analytics |
|
EHR and Third-Party Integrations |
$10,000 to $40,000 |
HL7 or FHIR integrations, legacy system complexity |
|
AI and Advanced Capabilities |
$15,000 to $60,000+ |
Predictive models, automation logic, intelligence depth |
|
Security and Compliance Framework |
$6,000 to $18,000 |
Data protection, audit trails, access control |
|
Testing and Quality Assurance |
$5,000 to $15,000 |
Performance testing, compliance validation, regression testing |
This is why custom healthcare practice management software development costs vary so much from one organization to another.
Several variables directly influence how much you will spend when you build healthcare practice management systems.
Many cost overruns happen after launch, not during development. These are the expenses teams often miss when planning healthcare practice management platform development.
If your platform also supports staff training or onboarding, integrating with healthcare LMS software can introduce additional costs that should be planned early.
Cost optimization is not about cutting corners. It is about making smarter decisions early.
Some organizations also reduce long-term expenses by designing systems that integrate operational tools early, rather than layering them later.
If your goal is to create scalable medical practice management systems, budget planning must account for both launch and growth. Lower upfront cost often leads to higher operational cost later.
A well planned investment in healthcare practice management software development gives you predictable operations, better revenue control, and systems that scale with your organization.
Next up, let's look at the challenges and ways to solve them.
Get clarity on cost, scope, and ROI before you commit to healthcare practice management software development.
Get a Cost Estimate
Even with the right plan, healthcare practice management software development comes with real challenges. Most failures are not caused by technology alone, but by gaps between operations, compliance, and execution.
Here the table outlines the most common challenges healthcare organizations face when they develop healthcare practice management software, along with proven ways to solve them.
|
Challenge in Healthcare Practice Management Software Development |
Why It Happens |
How to Solve It Effectively |
|---|---|---|
|
Misalignment with real clinical workflows |
Software is designed based on assumptions rather than how staff actually work |
Involve front desk, billing, and operations teams early to ensure workflows match reality when you build healthcare practice management systems |
|
Low user adoption by staff |
Systems feel complex, slow, or unintuitive |
Prioritize usability and workflow simplicity so teams trust and consistently use the platform you create medical practice management software on |
|
Billing errors and revenue leakage |
Disconnected billing logic or incomplete payer rules |
Design billing as a core module from day one when you make healthcare practice management software with billing integration |
|
Scalability limitations |
Architecture is designed only for current volume |
Plan infrastructure and data models early to create scalable medical practice management systems that support future growth |
|
Integration complexity with existing systems |
Legacy EHRs and third party tools were not considered upfront |
Define integration strategy early during medical practice software application development to avoid fragile workarounds |
|
Compliance and data security risks |
Security is added late instead of built in |
Embed compliance, access controls, and audit trails from the start in custom healthcare practice management software development |
|
Cost overruns during development |
Scope creep and unclear priorities |
Control scope with phased delivery and clear milestones when you develop healthcare practice management systems for operational efficiency |
|
Performance issues at scale |
Insufficient load testing and optimization |
Test under real usage scenarios, especially for healthcare practice management software development for hospitals |
|
Difficulty supporting multi-location clinics |
Inconsistent workflows and decentralized data |
Centralize logic and reporting when you create healthcare practice management software for multi-location clinics |
|
Slow innovation after launch |
No plan for post-launch evolution |
Treat the platform as a product, not a one-time project, especially in long-term healthcare practice management platform development |
Most of these issues become expensive only when they are discovered late. The earlier they are addressed, the easier and cheaper they are to fix.
Organizations that succeed with healthcare practice management software development focus less on features alone and more on alignment between people, process, and technology.
When challenges are handled intentionally, practice management systems stop being a source of friction and start becoming a driver of operational clarity and growth.
Building a healthcare practice management system is not just about code. It is about aligning technology with real-world workflows, regulatory compliance, and future growth plans. Biz4Group brings more than technical expertise. As a trusted AI development company, we help healthcare organizations go beyond basic systems and move toward intelligent, future-ready platforms. We bring healthcare-aware engineering, deep design experience, and a track record of delivering systems that work in live environments, not just on paper.
Here’s how we help you move from concept to measurable impact:
One of Biz4Group’s standout projects is Dr. Ara, an AI-powered health solution built to help athletes converts raw blood data into actionable performance and health guidance. This platform showcases our ability to design, architect, and deliver sophisticated health software that turns complex data into personalized insights.
Dr. Ara is a centralized health platform where users upload blood test reports and receive personalized guidance on diet, hydration, sleep, and training. The system also enables private consultations and real-time health tracking, combining analytics with user engagement in one scalable solution.
Key Highlights from the Dr. Ara Project
This project illustrates how Biz4Group approaches complex health data safely and responsibly, turning analytical intelligence into features users adopt and trust. Projects like Dr. Ara show our strengths in healthcare-aligned data applications and system scalability, foundational skills that matter when you develop healthcare practice management software.
Partner with a team that understands healthcare operations, AI, and scalable software delivery.
Start Your Project with Biz4GroupAs healthcare organizations grow, disconnected systems and manual workflows quickly become barriers. Investing in healthcare practice management software development helps you streamline operations, improve billing accuracy, and build a foundation that supports long-term growth.
When you develop healthcare practice management software with the right strategy, you gain more than features. You gain control, visibility, and scalability across clinics and hospitals. This is especially critical for organizations looking to build healthcare practice management systems that adapt as patient volume, locations, and compliance needs increase.
Biz4Group brings proven experience in building secure, scalable healthcare platforms and delivering custom healthcare practice management software development aligned with real operational needs. From planning to execution, we help healthcare leaders make smarter technology decisions with confidence.
Healthcare practice management software focuses on administrative and operational workflows such as scheduling, billing, insurance processing, and patient flow, while EHR systems handle clinical data like diagnoses and treatment history. In healthcare practice management software development, these systems are often integrated, so business and clinical workflows stay aligned and operational efficiency improves across clinics and hospitals.
The timeline depends on scope and complexity. A focused MVP approach for healthcare practice management software development usually takes 2 to 4 weeks, covering core scheduling and billing workflows. More complex or enterprise practice management system development for hospitals typically takes 6 to 8 weeks, especially when integrations, security, and scalability are required.
The decision depends on workflows, growth plans, and operational complexity. Organizations often choose custom healthcare practice management software development when they need flexibility, scalability, or specialty billing logic. Off the shelf tools may work for smaller clinics, but teams looking to build healthcare practice management systems for long-term growth often prefer custom solutions.
Yes. Modern medical practice software application development follows standards such as HL7 and FHIR to enable seamless integration with EHR platforms, billing tools, and third party systems. This integration is essential when you develop healthcare practice management software that avoids data silos and manual duplication.
Security and compliance are critical. Healthcare practice management software development must follow HIPAA guidelines, including encryption, role-based access, audit trails, and secure authentication. These requirements are especially important for healthcare practice management software development for hospitals and multi-location organizations.
After launch, leaders should track scheduling efficiency, claim denial rates, billing turnaround time, patient no shows, and user adoption. These KPIs help measure ROI and determine whether developing healthcare practice management systems for operational efficiency goals are being met.
Small practices often see faster billing cycles, reduced administrative workload, and improved patient communication after adopting healthcare practice management software development solutions. Automation allows staff to focus on care delivery while maintaining operational control as the clinic grows.
The cost to develop healthcare practice management software typically ranges from $40,000 to $300,000+, depending on features, integrations, scalability, and compliance requirements. Basic clinic systems fall on the lower end, while enterprise practice management system development for hospitals or multi location clinics requires higher investment due to complexity and long-term scalability needs.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.