Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Why do patient delays, missed visits, and bed bottlenecks still disrupt hospital operations even after multiple digital systems are already in place?
For healthcare IT managers, medical directors, and operations leaders in healthcare, the real challenge often begins when patient movement across scheduling, triage, treatment, and discharge depends on disconnected workflow handoffs. A missed signal in one stage quickly affects the next, leading to longer waiting times, inefficient bed turnover, and rising coordination pressure on staff.
This is exactly where hospitals are creating intelligent automation systems for hospital patient journey optimization to bring continuity into every care-stage decision. When scheduling intelligence is aligned with patient flow patterns, hospitals have already seen waiting times drop by 37.5%. Not only that AI smarter resource allocation has also improved bed occupancy efficiency by 29% by helping teams act on real-time workflow triggers instead of delayed manual updates.
That operational clarity becomes even stronger during development when the system is designed around measurable workflow goals such as:
As hospitals move to develop AI patient journey automation system for hospitals, the focus shifts from isolated task automation to connected workflow intelligence. In practice, embedding no-show prediction into scheduling workflows has already reduced missed visits by 50.7%. This makes end-to-end development of AI patient journey solutions a strategic priority for teams working with the right AI development company.
Now with all that being said, the next step is understanding how the AI-driven patient journey automation system supports the complete hospital care journey. We’ll also get insights into which firms specialize in creating AI patient journey systems for hospitals?
Every hospital leader sees the pressure points differently. For some, it starts with fragmented patient coordination. For others, it shows up in missed handoffs between departments. Before moving into workflows and implementation, it helps to first establish what this system actually means in a hospital setting and why it matters strategically.
An AI-driven patient journey automation system is a hospital-focused software layer that helps care teams manage how patients move through key stages of care with better continuity and fewer manual follow-ups. Instead of handling every scheduling update, triage signal, discharge milestone, or follow-up reminder separately, the system keeps these touchpoints connected so teams can act with better timing and clearer visibility.
At its core, this system is designed to support decisions around:
For healthcare CTOs and digital transformation leaders, this is the foundation used to build AI system for patient journey management in a way that supports operational consistency with future-ready AI automation services across hospital workflows.
Once the system is in place, its value shows in how smoothly patients move from one care stage to the next. Each interaction is connected to the next expected step, so delays and missed follow-ups are reduced. It:
This stage-based support model gives healthcare leaders a clearer view of how continuity is maintained and help create automated patient journey systems using AI
For healthcare CTOs and digital transformation leaders, the difference becomes clearer when both approaches are viewed through day-to-day patient movement and coordination outcomes. Have a look:
|
Workflow Area |
Traditional Hospital Workflow Management System |
AI-Driven Patient Journey Automation System |
|---|---|---|
|
Patient routing |
manual assignment after intake |
care-stage based guided routing |
|
Care coordination |
staff-led follow-up between stages |
next-step triggers based on patient progress |
|
Discharge flow |
checklist-driven handoffs |
milestone-based readiness support |
|
Post-care continuity |
manual calls and reminders |
proactive follow-up and recovery nudges |
The difference becomes especially valuable...
The role becomes clearer when seen across the hospital systems and teams that shape patient continuity. It:
This foundation helps healthcare leaders clearly see where patient continuity needs stronger coordination. For teams planning to develop AI patient journey automation system for hospitals, it creates the right strategic context to evaluate the investment priorities discussed in the next section.
Turn workflow confusion into connected patient movement with a system hospitals can actually scale
Contact us to Map Your WorkflowHealthcare leaders are under growing pressure to improve patient continuity while proving measurable returns from digital initiatives. That urgency is also reflected in market momentum, with patient experience technology projected to grow from USD 0.6 Billion in 2026 to USD 1.20 Billion by 2033.
With that direction now clearly visible, building an AI patient journey automation system for hospitals becomes a timely and strategically grounded investment priority.
For hospitals, one of the earliest measurable gains comes after the patient leaves the facility, where weak follow-up coordination often drives avoidable returns. When discharge milestones and predictive follow-up stay connected, readmissions can drop by 20–30%, giving healthcare administrators and healthcare consultants stronger control over continuity outcomes.
This improves operational continuity through:
A large part of workflow friction comes from repetitive coordination tasks that pull teams away from patient-focused decisions. When journey orchestration connects scheduling, follow-up, discharge, and recovery actions, hospitals have reduced administrative overhead by 45%.This helps teams spend less time on manual updates and more time on active care coordination.
This operational relief shows up through:
Length of stay directly affects both bed availability and treatment cost when care milestones are delayed during active recovery stages. With AI-assisted care pathway automation, hospitals have reported a 20% reduction in post-operative length of stay. This reduced LOS and ICU time, which is translated into $3,336–$8,671 savings per patient in measured care settings.
This creates measurable impact through:
For hospitals planning long-term workflow modernization, financial return becomes clearer when journey automation improves multiple care stages at once. Organizations typically achieve an average $3.20 ROI for every $1 invested in workflow automation. This makes patient journey orchestration a financially grounded initiative for healthcare administrators managing digital transformation budgets.
This business return grows through:
As patient journey automation expands from one department to multiple care units, scalability becomes a direct business advantage for hospitals managing long-term transformation. This is where healthcare enterprise AI solutions create stronger value by helping leadership teams extend proven workflow gains across locations, specialties, and shared care pathways without rebuilding processes from scratch.
This supports growth through:
Once the operational and business gains are clearly mapped, it becomes easier to create an AI tool to personalize and automate patient care pathways in a way that supports measurable hospital growth and stronger care continuity outcomes.
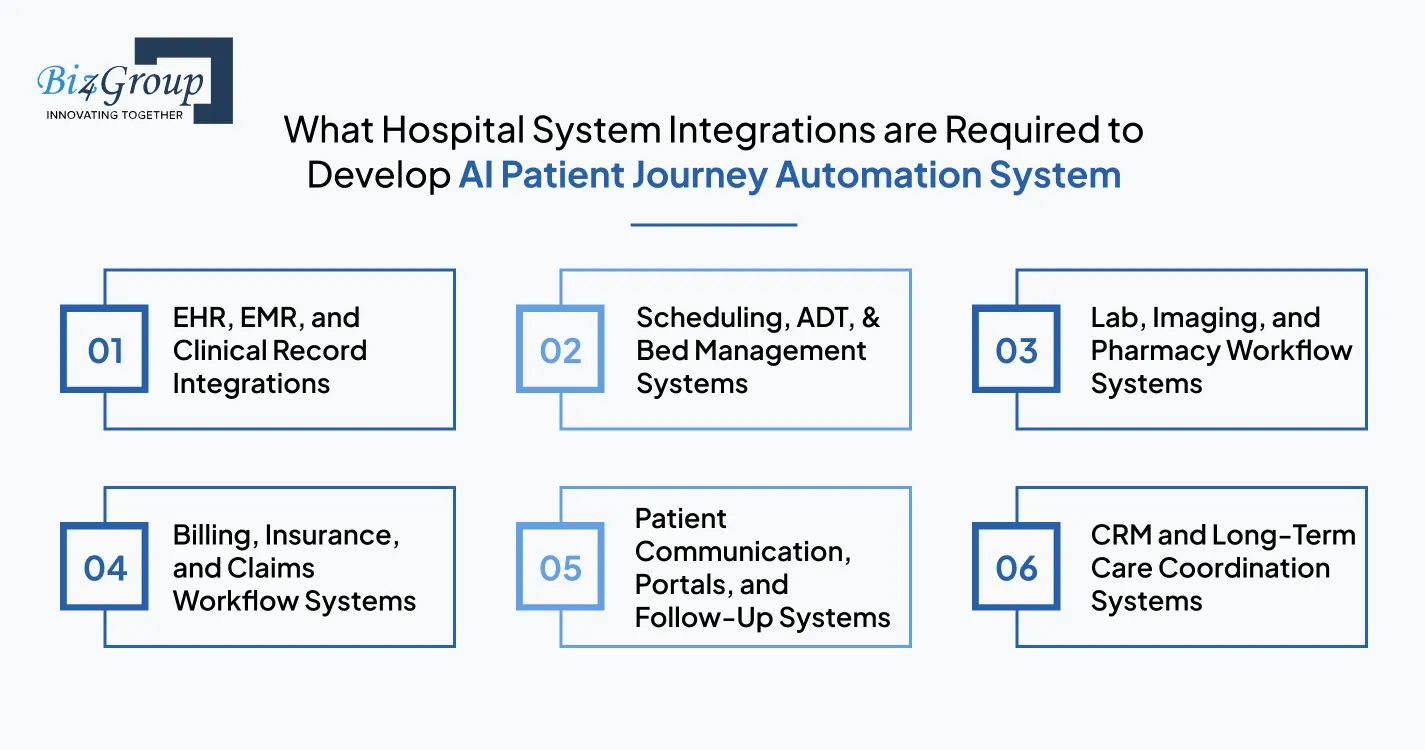
Patient journey automation only works when the system stays connected to the hospital tools already driving daily care movement. That is why building integrated AI systems to manage patient journeys across healthcare services starts with identifying which operational systems must continuously share patient context, status changes, and next-step signals.
The first integration layer should connect the automation system with the hospital’s clinical record environment, so every journey action stays aligned with live patient information. When teams integrate AI with EHR/EMR system workflows, appointment context, diagnosis updates, treatment notes, medication history, and discharge summaries remain available across every care stage.
This integration layer should continuously exchange:
Also Read: A Complete Guide to AI EMR/EHR Software Development
The next integration layer should connect the systems that control how patients move through admission, transfer, discharge, and appointment timelines. When scheduling, ADT, and bed management systems stay connected, the journey platform always receives the latest status changes that affect the next care-stage transition.
This integration layer should continuously share:
Patient journey continuity also depends on the systems that confirm when diagnostics and medication steps are ready for the next stage of care. When lab, imaging, and pharmacy platforms stay connected, care teams can move patients forward based on real clinical progress rather than waiting for manual coordination updates.
This integration layer should continuously share:
Also Read: How to Build an AI Radiology Information System for Healthcare Enterprises?
Financial clearance points often influence whether the next patient journey step can move forward without delay. When billing, insurance, and claims systems stay connected, the automation layer can stay aware of authorization, payment, and discharge-related financial checkpoints that affect continuity.
This integration layer should continuously share:
The journey also depends on the systems patients directly interact with before and after care milestones. When communication channels and portal systems stay connected, every instruction, reminder, and follow-up message stays aligned with the patient’s latest journey stage without relying on disconnected outreach tools.
This integration layer should continuously share:
Also Read: AI Patient to Nurse Communication System Development
Long-term journey continuity depends on systems that track patient relationships beyond the immediate episode of care. When the automation layer connects with a healthcare CRM, care teams can keep chronic follow-ups, preventive outreach, and case-management touchpoints aligned with the patient’s broader care history.
This integration layer should continuously share:
Also Read: Artificial Intelligence in CRM: Use Cases & Roadmap
This integration view should now make one implementation reality clear: patient journey automation succeeds only when every care dependency stays connected to the right hospital systems. With that clarity in place, teams can create a custom AI system for patient journey and care coordination with stronger continuity and cleaner development decisions.
Unify care-stage signals across hospital tools before missed handoffs become operational risk
Plan AI Integrations with usThe real strength of patient journey optimization lies in what the platform can actively do inside day-to-day hospital workflows. That is why AI patient journey automation software development for hospitals must focus on realistic product capabilities that directly improve patient movement across every care stage.
|
Core Feature |
What This Feature Enables in Hospital Journey Optimization |
|---|---|
|
Intelligent patient routing |
Helps the system move patients to the right specialty, department, or care stage based on urgency, appointment type, and treatment progress so avoidable delays are reduced early. |
|
No-show risk alerts |
Uses predictive analysis to identify patients likely to miss visits, allowing teams to trigger reminders, rescheduling, or follow-up actions before appointment slots are lost. |
|
Pre-visit task automation |
Keeps forms, consent collection, insurance checks, and visit preparation tasks aligned to the scheduled care stage, so front-desk delays are minimized. |
|
Treatment milestone tracking |
Gives care teams visibility into whether diagnostics, consultations, procedures, and medication steps are completed on time during active treatment. |
|
Discharge readiness monitoring |
Tracks discharge blockers such as pending medication, documentation, or follow-up instructions, so patients do not stay longer than required. |
|
Follow-up journey automation |
Automatically keeps post-discharge visits, recovery check-ins, and medication reminders aligned to the patient’s next care milestones. |
|
Readmission risk alerts |
Flags patients showing recovery-stage risk signals so care teams can intervene before avoidable returns happen. |
|
Recovery adherence tracking |
Monitors whether patients are completing medication plans, therapy visits, and recovery checkpoints after discharge. |
|
Exception and escalation alerts |
Highlights missed actions, delayed milestones, or urgent patient risks so care teams can intervene quickly. |
|
Journey performance dashboards |
Supported by reliable AI model development, this gives leadership visibility into delays, drop-offs, recovery bottlenecks, and care continuity gaps. |
Once these core capabilities are clearly defined, the path to product planning becomes far more practical for hospital leadership and delivery teams. This feature layer gives the functional clarity needed to develop AI patient journey automation system for hospitals with realistic workflow outcomes before moving into system architecture decisions next.
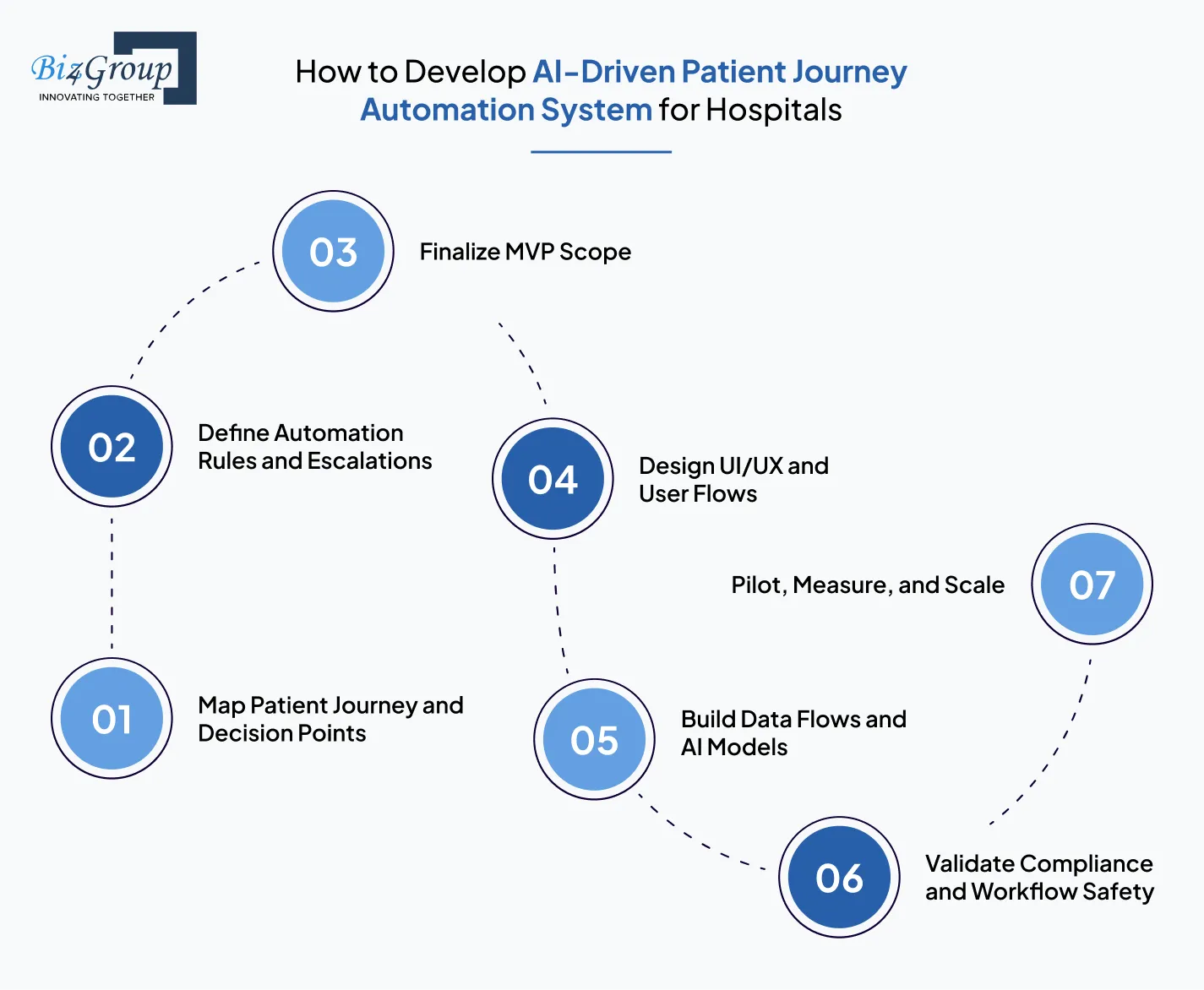
Hospital workflow modernization becomes much easier to execute once the development path is broken into clear delivery stages. If you are wondering, how can I develop AI-Driven Patient Journey Automation Systems for my healthcare business?
The most practical way is to move step by step from workflow discovery to controlled hospital rollout.
Start by identifying how patients move from intake to discharge and follow-up, so the product reflects real care-stage decisions instead of assumed workflows.
This step should clearly map:
Once the journey path is clear, define the rules that decide what should happen next when a milestone is delayed, completed, or flagged as risky.
This step should cover:
The first release should stay focused on one high-impact workflow, so teams can validate outcomes faster with the right MVP development services support.
This step should prioritize:
Also Read: Top MVP Development Companies in USA
The product experience should make daily decisions easier for nurses, coordinators, discharge teams, and patient-facing workflows so every role can act on the right journey stage without delay.
This step should define:
Also Read: Top UI/UX Design Companies in USA
This is the execution stage where live hospital workflow signals begin moving into the intelligence layer so patient progression decisions can start working on real care-stage data.
This step should include:
Before hospital rollout, every workflow path should be tested for safety, continuity, and role-level reliability, often with support from experienced software testing companies.
This step should validate:
Start with one department where workflow friction is already measurable, then expand only after KPI improvements are validated in real care settings.
This step should focus on:
This step-by-step roadmap gives hospitals a realistic path to develop AI patient journey automation system for hospitals with lower rollout risk and stronger operational readiness before architecture planning begins.
Move from workflow plans to delivery-ready product milestones with the right healthcare build partner
Build Your RoadmapOnce the workflow logic, features, and rollout stages are defined, the next priority is structuring how the platform will technically support them at scale. For teams focused on building intelligent patient journey automation platforms for healthcare providers, the architecture should keep patient continuity, decision logic, and live hospital events moving through clearly defined layers.
To translate this architecture into a production-ready hospital platform, each internal layer needs a clearly matched technology choice that supports scale and reliability as patient volume grows.
|
Architecture Layer |
Recommended Technology |
Purpose |
|---|---|---|
|
Experience Layer |
Supports care-team dashboards and patient-facing web development workflows |
|
|
API Gateway Layer |
Kong, NGINX |
Secures routing, request control, and service-level traffic governance |
|
Workflow Orchestration Layer |
Temporal, Camunda |
Manages workflow state execution and event sequencing |
|
Business Rules Layer |
Drools, custom rule engine |
Handles escalation logic, role-based conditions, and milestone rules |
|
AI Intelligence Layer |
Python, FastAPI, PyTorch |
Runs inference pipelines and journey-state risk scoring |
|
Data Flow Layer |
Kafka, RabbitMQ |
Moves live patient-state events across internal services |
|
Integration Service Layer |
REST, GraphQL, gRPC |
Standardizes internal service communication and exchange contracts |
|
Storage Layer |
PostgreSQL, MongoDB |
Stores workflow state, alerts, logs, and journey history |
|
Security and Audit Layer |
Keycloak, OAuth 2.0 |
Protects role access, audit visibility, and override tracking |
|
Cloud and Monitoring Layer |
AWS, Docker, Kubernetes, Grafana |
Supports uptime, scaling, observability, and resilient deployment |
With the architecture and technology layers now clearly mapped, the path to full stack development becomes far more practical. This gives healthcare teams a clearer foundation to build AI-powered patient journey automation solutions that scale reliably across hospital workflows and future care-stage expansion.
Also Read: Why to Choose the Full Stack Development for Modern Business
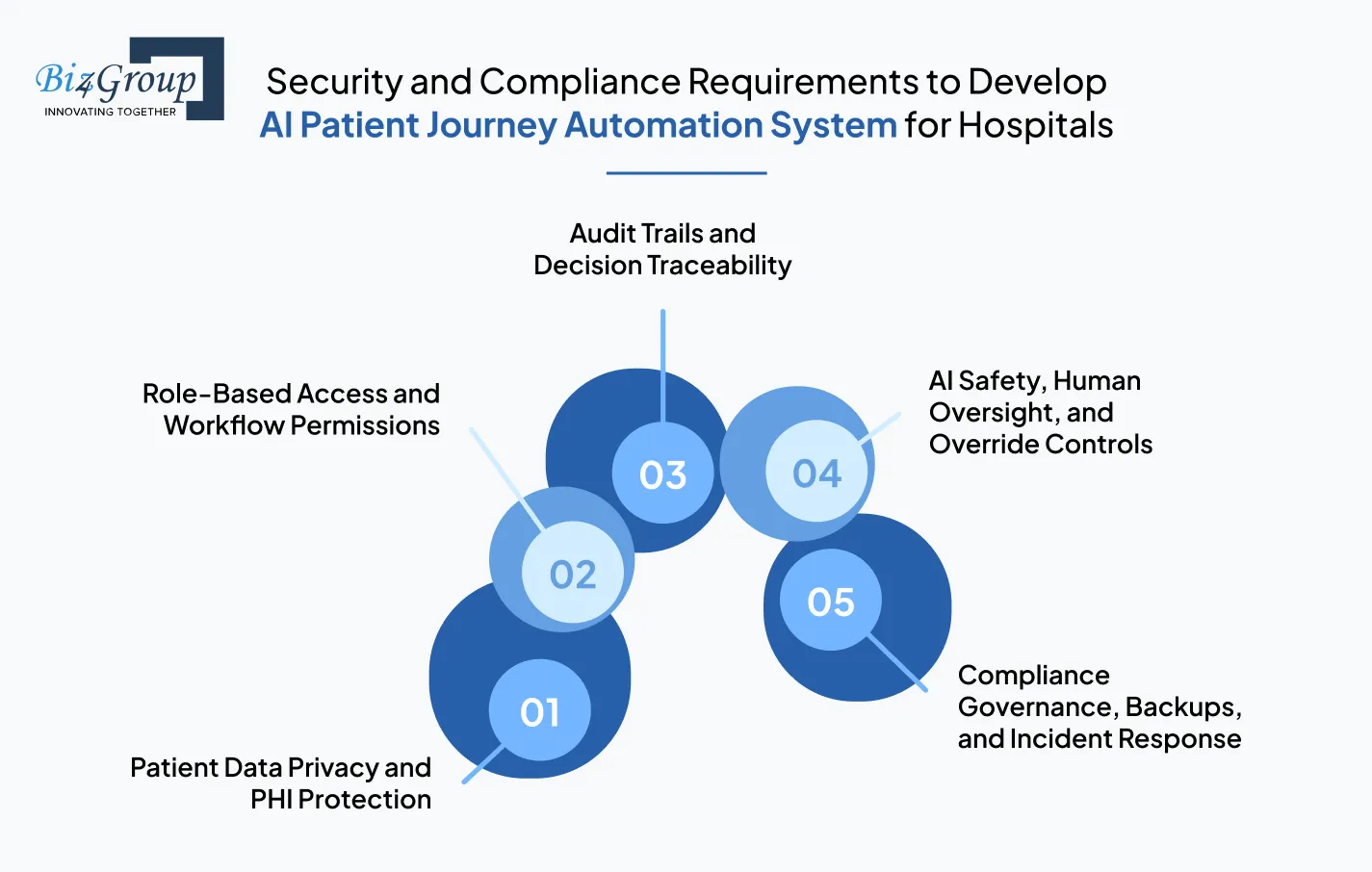
Patient trust and hospital rollout readiness depend heavily on how securely the platform handles care-stage decisions and patient data from day one. To create AI-powered patient journey automation solutions that hospitals can confidently adopt, security and compliance controls must be planned as core product requirements, not post-deployment fixes.
The priority is protecting every piece of patient-identifiable data that moves through the journey workflow, from intake details to discharge and recovery updates. To stay aligned with HIPAA privacy and security requirements, access to PHI and ePHI should remain limited to the minimum data required for each workflow action.
Data should remain protected through encryption at rest and in transit, secure consent handling, masked patient identifiers in non-clinical views, and clear retention rules for workflow logs. This keeps the platform aligned with hospital privacy expectations while reducing exposure risk during care-stage automation.
Also Read: HIPAA Compliant AI App Development for Healthcare Providers
The control layer should define exactly who can view, update, approve, or override each workflow action across the patient's journey. Access should always match the user's role in the care process so front-desk staff, nurses, discharge teams, coordinators, and administrators only see the workflow data required for their responsibilities.
This role-based visibility becomes critical when multiple departments interact with the same patient journey. Permissions should therefore be mapped by department, workflow stage, patient-status sensitivity, and action authority, so no one can trigger updates or view sensitive continuity data beyond their approved scope.
The next compliance requirement is making every automated workflow action reviewable after it happens. In hospital AI systems, this means every routing decision, escalation trigger, follow-up alert, and human override should leave a time-stamped audit trail that shows what changed, when it changed, and who approved it.
This traceability becomes even more important when AI influences patient movement decisions. The system should therefore preserve the workflow state before and after each automation event, the risk score that triggered the action, the user who reviewed it, and the final approved outcome.
The next requirement is keeping human control active in every high-impact workflow decision influenced by AI. If the system flags a risky discharge, escalates a follow-up, or recommends a pathway change, the final action should remain reviewable by the authorized hospital team.
The platform should therefore place approval checkpoints before sensitive journey transitions and preserve every manual override with the reason behind it. High-risk pathway changes should require explicit human confirmation, so the automation layer continues to support patient safety instead of acting without supervision.
The final compliance requirement is making sure the platform can stay safe and recoverable even during outages, cyber incidents, or workflow failures. For hospital AI systems, this means HIPAA contingency planning should include tested backup routines, disaster recovery procedures, and emergency access continuity. This ensures patient journey workflows remain available when critical systems go down.
Governance should also define how incidents are escalated, how vendors handling PHI are contractually accountable, and how breach notifications are managed within HIPAA timelines.
These safeguards turn compliance into rollout confidence and help hospitals develop AI patient journey automation system for hospitals with safer scale, stronger trust, and long-term operational resilience.
Protect patient trust with workflow controls built for hospital-grade compliance from day one
Contact Us to Secure Your Rollout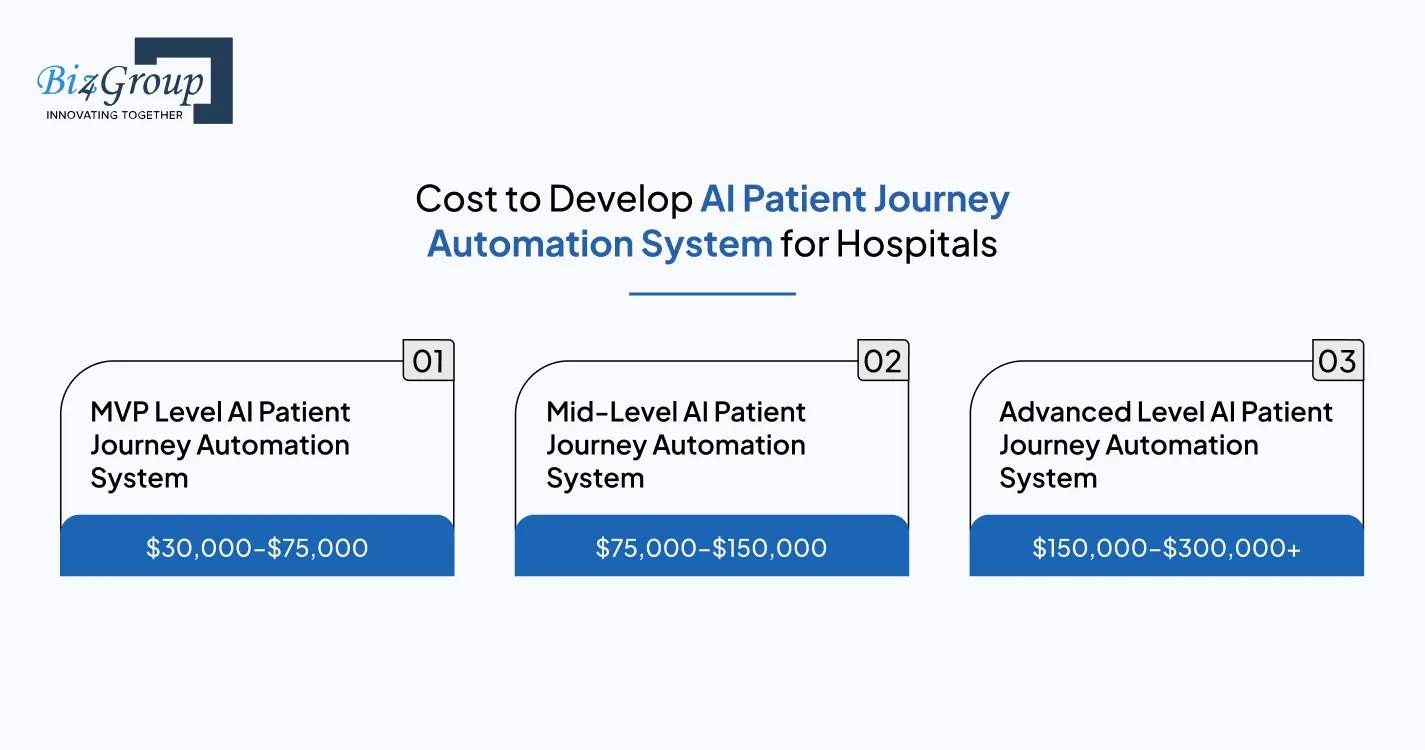
For hospitals planning AI patient journey automation system development for hospitals, the cost usually depends on rollout depth and how many departments need continuity from intake to post-discharge. In most realistic implementations, the total investment ranges from $30,000 to $300,000+, depending on the maturity level of the platform.
|
Development Level |
Estimated Cost Range |
Scope |
|---|---|---|
|
MVP Level AI Patient Journey Automation System |
$30,000–$75,000 |
One workflow use case, limited department rollout, core routing, follow-up automation, essential dashboards |
|
Mid-Level AI Patient Journey Automation System |
$75,000–$150,000 |
Multi-stage patient journey workflows, stronger AI prediction logic, compliance controls, cross-team dashboards |
|
Advanced Level AI Patient Journey Automation System |
$150,000–$300,000+ |
Multi-department orchestration, advanced AI models, enterprise-scale security, KPI intelligence, hospital network expansion |
The largest cost shift comes from how many care stages and departments are included in the first release. Expanding from one discharge workflow to multi-department orchestration can increase costs by $15,000–$40,000, depending on workflow branching depth and approvals.
No-show prediction, LOS risk, readmission scoring, and care-stage prioritization directly increase AI integration costs. Adding advanced risk models and workflow intelligence can raise budgets by $20,000–$50,000, especially when real-time scoring is required.
Live data movement across scheduling, ADT, and patient-state services significantly affects the cost of implementing AI in healthcare workflows. Depending on internal system readiness, this usually adds $10,000–$30,000 to the total delivery budget.
Encryption, role-based access, audit trails, backup recovery, and incident response readiness can add $12,000–$35,000, especially for hospital groups requiring stronger governance before deployment approval.
Continuous model tuning, workflow threshold updates, and KPI recalibration often add $8,000–$35,000, depending on patient volume and how frequently automation logic evolves after launch.
|
Hidden Costs |
Estimated Cost Impact |
|---|---|
|
workflow redesign after pilot feedback |
$5,000–$20,000 |
|
compliance documentation and legal reviews |
$4,000–$15,000 |
|
backup, disaster recovery, and failover drills |
$3,000–$12,000 |
|
staff onboarding and workflow retraining |
$5,000–$18,000 |
|
post-launch AI threshold recalibration |
$6,000–$25,000 |
This cost view gives hospital teams a practical budgeting baseline before they develop AI patient journey automation system for hospitals with broader enterprise rollout and KPI ownership in the next stages.
Also Read: How Much Does AI Software Development Cost in 2025?
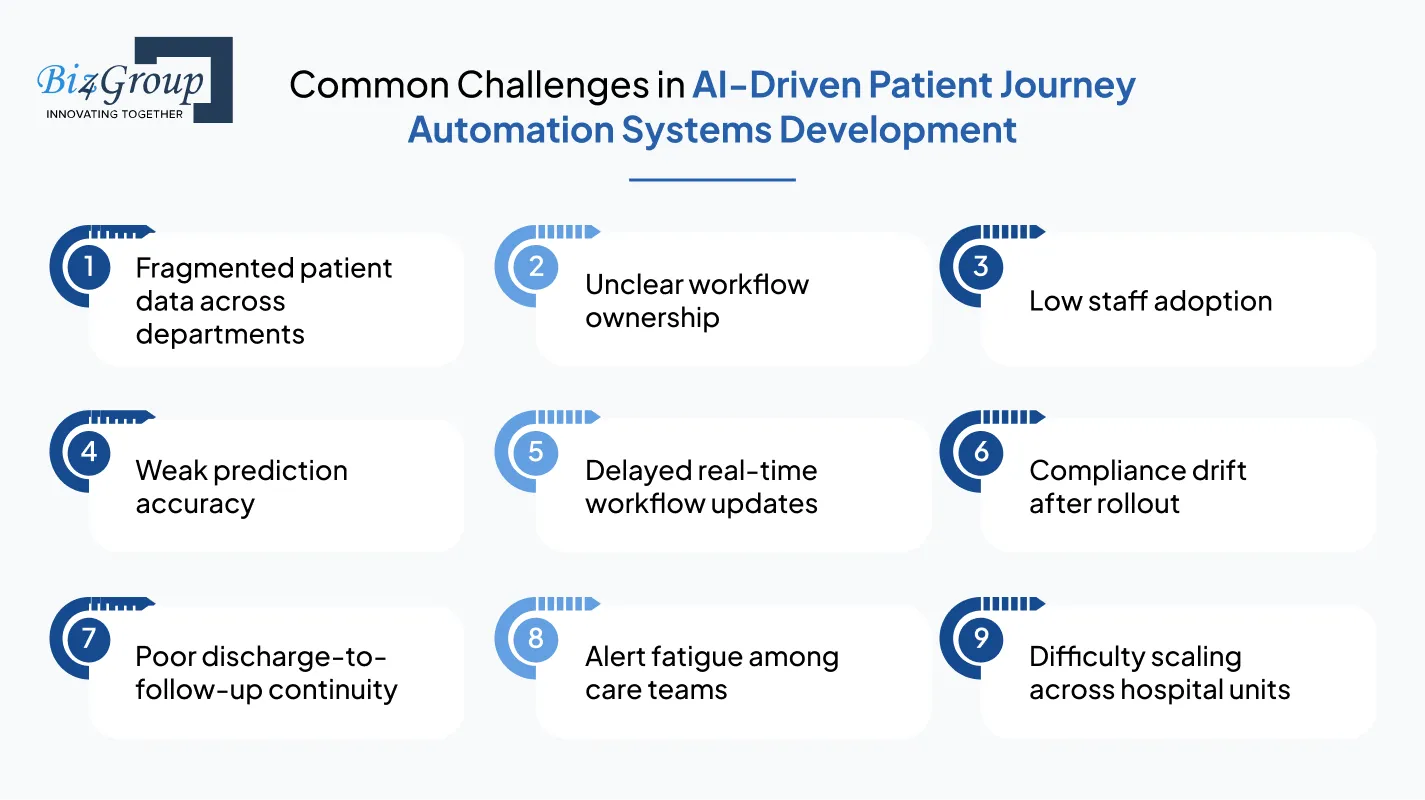
Even after roadmap, architecture, and budget planning are in place, hospital teams still face rollout barriers that can slow patient continuity outcomes. That is why creating automated AI tools for patient journey success also depends on solving operational, data, and adoption challenges before scale.
|
Common Challenge |
Why It Happens in Hospital Workflows |
Practical Solution |
|---|---|---|
|
Fragmented patient data across departments |
updates remain split across care teams, making continuity difficult |
use strong AI integration services to unify patient-state events before workflow automation begins |
|
Unclear workflow ownership |
teams lack stage-level accountability for escalations and follow-ups |
define workflow ownership by care stage and approval responsibility |
|
Low staff adoption |
alerts and dashboards do not match real nurse or coordinator routines |
involve frontline teams early and align usability with experienced AI developers |
|
Weak prediction accuracy |
incomplete history and missing milestone data reduce AI reliability |
clean historical discharge, no-show, and recovery data before retraining models |
|
Delayed real-time workflow updates |
lag between departments creates missed triggers and continuity gaps |
use event-driven sync and stricter workflow state refresh intervals |
|
Compliance drift after rollout |
permissions and audit rules weaken as departments expand |
run governance reviews before every department-level scale phase |
|
Poor discharge-to-follow-up continuity |
post-care ownership gaps create readmission risk |
map post-discharge ownership and automate recovery-stage checkpoints |
|
Alert fatigue among care teams |
too many low-priority triggers reduce trust in the system |
prioritize risk thresholds and suppress low-value notifications |
|
Difficulty scaling across hospital units |
each department follows different care-stage logic |
standardize reusable workflow templates before multi-unit rollout |
Once these rollout barriers are addressed early, hospital teams can move forward with far fewer workflow disruptions and stronger adoption confidence. This makes it much easier to develop AI patient journey automation system for hospitals with scalable continuity, safer department expansion, and more predictable long-term outcomes.
Solve adoption friction and continuity blockers before they slow hospital-wide scale
Talk to UsWhen healthcare IT managers, medical directors, and operations managers in healthcare evaluate which companies provide end-to-end development of AI healthcare automation systems, the real focus goes beyond coding. It comes down to whether the partner understands patient workflows, clinical coordination, healthcare usability, and long-term operational continuity. This is exactly where Biz4Group LLC stands.
As a trusted healthcare software development company, we keep our execution grounded in how real healthcare teams work every day. Across our healthcare portfolio, we have consistently built products that support patient guidance, wellness continuity, health decision support, and AI-led engagement journeys.
A few of our healthcare implementations make that expertise clearer. Have a look:
Semuto is a healthcare recommendation and wellness guidance platform that helps users discover more relevant health pathways based on their needs and preferences. It supports guided digital health decisioning while keeping the user journey smooth and personalized.
Key Features:
CogniHelp is a dementia and cognitive AI support platform designed to assist patients and caregivers through structured care guidance and condition-aware interactions. It helps improve continuity through supportive prompts, health tracking, and patient-friendly engagement flows.
Key Features:
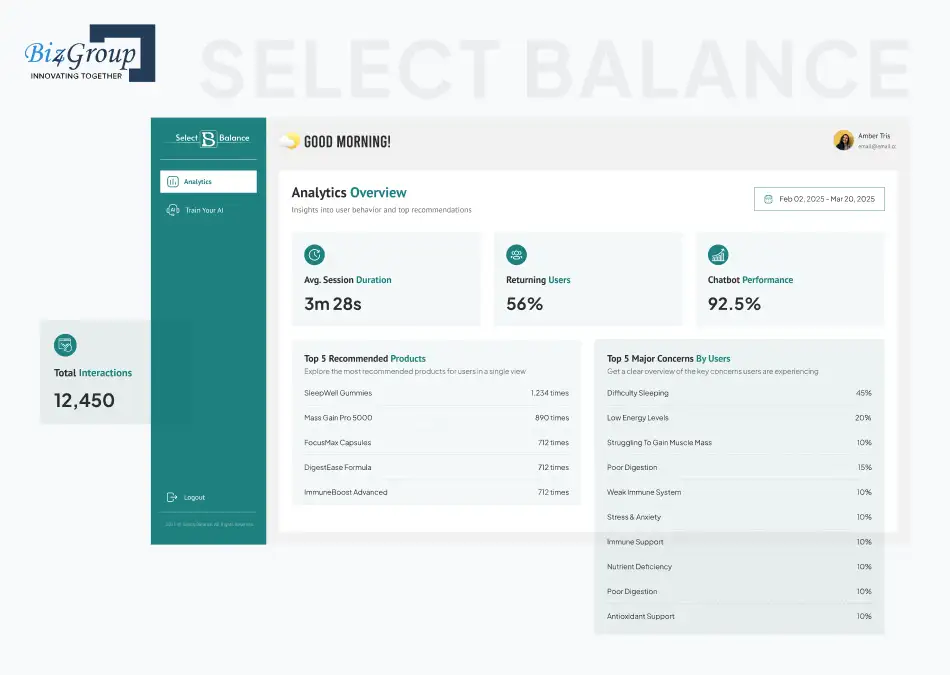
Select Balance is an AI chatbot for personalized supplement recommendation that guides users through structured symptoms and wellness-based journeys. It helps users move from initial inputs to meaningful health suggestions with clear digital pathways.
Key Features:
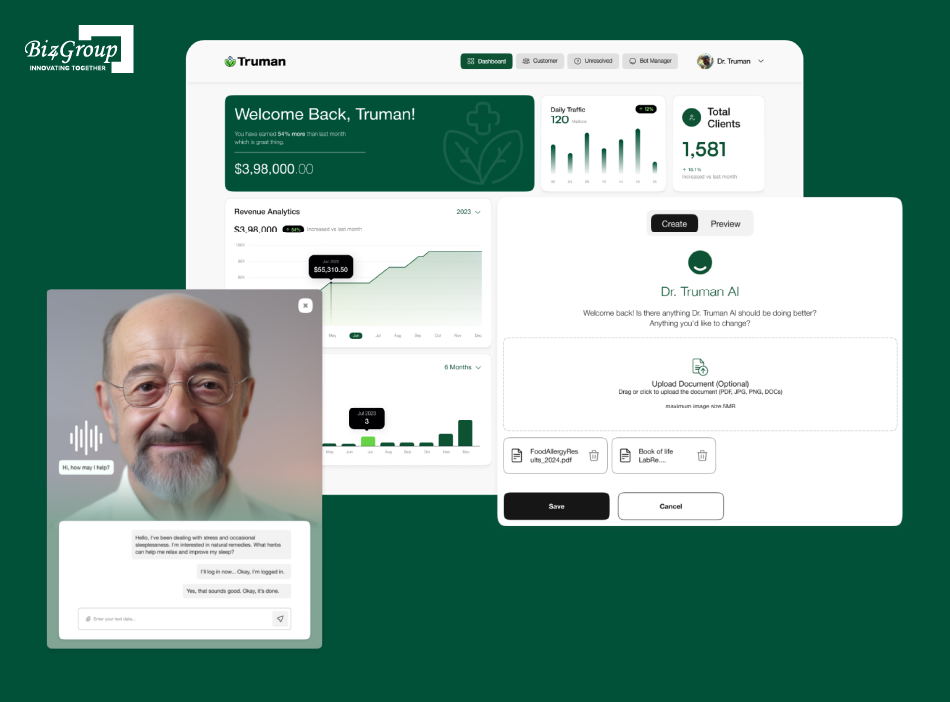
Truman is an AI wellness companion platform that supports users with personalized health coaching, interactive wellness prompts, and continuity-driven engagement experiences. It keeps long-term health journeys active through repeated, personalized interactions.
Key Features:
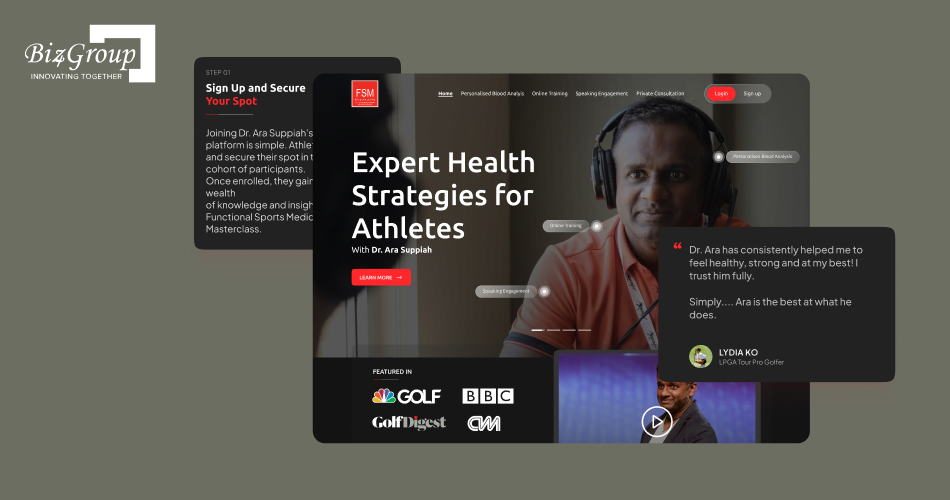
Dr. Ara is an AI-powered athletic health solution built to help users improve performance through detailed blood test analysis and personalized health consultations. The platform turns uploaded blood reports into practical guidance around hydration, sleep, nutrition, cholesterol, oxygen levels, and training improvement. It also supports ongoing progress tracking through repeat consultations.
Key Features:
These healthcare implementations reflect how our team turns complex care journeys into usable digital products with strong continuity and user adoption. That is the same execution depth our healthcare AI developers bring when hospitals plan to develop AI patient journey automation system for hospitals with long-term scalability and operational confidence.
Patient journey automation creates the most value when it fits how hospitals already deliver care, rather than forcing teams to adjust around disconnected tools. For CTOs in healthcare, this is where practical AI product development services matter most, because every workflow decision must support continuity, staff usability, compliance, and measurable operational outcomes.
The real opportunity is not just automating touchpoints but shaping a system that helps hospitals move patients more smoothly from intake to discharge and recovery with stronger coordination at every stage. When your next priority is to develop AI patient journey automation system for hospitals, the focus should stay on workflow fit, safe scale, and long-term adoption across departments.
That is exactly where Biz4Group LLC works as a long-term execution partner, helping healthcare teams turn complex patient operations into reliable digital systems that create measurable value in live care environments. If you are evaluating the next move for your healthcare platform, it would be worthwhile to discuss with us how this can translate into your product roadmap.
The delivery timeline usually ranges from 12-14weeks, depending on workflow depth, number of departments, rollout model, compliance approvals, and pilot complexity. A single discharge or follow-up workflow MVP may go live in 4-6 weeks, while multi-department orchestration requires phased deployment and validation cycles.
For enterprise hospital environments, the overall cost generally falls between $30,000 and $300,000+, based on department coverage, AI intelligence depth, compliance controls, rollout scale, and long-term workflow optimization requirements.
The strongest success indicators are workflow continuity and reduced handoff delays. Healthcare leaders should also track missed follow-ups, discharge turnaround improvement, and department-level throughput gains tied to patient progression milestones.
The best starting point is any department where continuity gaps already create measurable friction. Common priorities include discharge planning, surgical recovery, ICU transitions, chronic care coordination, and outpatient specialty workflows.
The decision usually depends on internal healthcare workflow expertise, AI product engineering maturity, compliance readiness, and the ability to support long-term optimization after pilot rollout. Hospitals with limited internal AI delivery bandwidth often move faster with a specialized healthcare technology partner.
Leadership teams should first track workflow completion and discharge-to-follow-up continuity. Other critical KPIs include alert response time, readmission reduction, bed turnover, and recovery adherence trends.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.