Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

What does one weak access control decision cost when patient data, AI workflows, and compliance penalties collide?
That question sits at the center of the cost to develop a HIPAA compliant AI healthcare software, because the real budget is shaped long before the first model goes live. IBM's research shows that organizations hit by AI-related incidents lacked proper AI access controls in 97% of cases, while 63% still operated without formal AI governance policies. In healthcare, that gap directly turns into architecture, audit, and security engineering costs.
When you begin planning a HIPPA compliant AI healthcare software product, the first challenge is not model performance. It is defining what secure deployment must include from day one. That usually means PHI-safe data movement, encryption, audit trails, role-based access, and vendor governance entering the roadmap early, which is why the realistic investment often falls between $40,000-$400,000+.
But before the numbers start making sense, let us first look at the critical layers where this budget usually begins to spread:
Now that the real cost pressures are visible, in the next sections, we'll break down what is included in the cost of HIPAA-compliant AI healthcare software development and how each layer changes the final budget.
Before you estimate the cost to develop a HIPAA compliant AI healthcare software, you need to first know whether HIPAA applies to your product. This is the point where many healthcare teams get confused, because not every AI healthcare tool automatically falls under compliance.
HIPAA compliance means following the rules for how protected health information (PHI) is handled, shared, stored, and secured inside healthcare workflows. PHI includes any patient-identifiable data such as names, reports, prescriptions, lab results, medical images, billing records, or treatment history. If your AI software creates, receives, stores, shares, or processes this data for a healthcare provider, payer, clinic, or hospital, HIPAA applies. The same applies when your AI vendor, cloud partner, or model provider handles PHI as a business associate under a BAA.
A simple way to validate this is to check whether your AI software does any of the following:
The moment even one of these becomes part of your workflow, HIPAA compliance becomes part of the product's scope, and that is where the budget starts becoming real in the sections ahead.
Also Read: AI EHR App Development for Hospitals and Clinics
The real concern for healthcare providers is not just whether AI can improve workflows, but whether it can be trusted with patient data inside daily care operations. Once AI begins interacting with clinical records, communication systems, or provider workflows, HIPAA compliance becomes the deciding factor for safe deployment. More importantly, it directly impacts the overall cost of development, deployment, and long-term maintenance.
That confidence gap is very real in healthcare. With HIPAA Journal tracking over 7,400 major healthcare data breaches since 2009, secure AI implementation is not just a regulatory requirement but a financial safeguard. The cost of non-compliance often exceeds the investment required to build compliant systems from the start.
That provider confidence usually depends on a few non-negotiable outcomes:
The bigger advantage is practical and financial: when compliance is embedded into the product architecture from the beginning, healthcare providers gain a system that is not only secure but also cost-efficient to scale. It reduces avoidable risks, prevents expensive corrections, and ensures smoother expansion across patient journeys and clinical operations.
Also Read: HIPAA Compliant AI App Development for Healthcare Providers
With the provider-side impact now clearly in front of us, the next logical step is to translate these compliance and workflow layers into a realistic way to estimate how the budget actually takes shape.
The real cost begins when secure workflows are missing from your first roadmap
Talk to Our ExpertsOnce the compliance scope, provider risk, and workflow depth are clear, the budget becomes much easier to estimate when you break it into practical cost layers instead of relying on rough assumptions. For most healthcare teams, the challenge is not the final number itself but understanding which engineering and compliance blocks are actually shaping it.
Total Cost = (Development Hours × Hourly Rate) + AI Model Development Cost + AI Integrations Cost + HIPAA Security Layer + Testing + Post-Launch Support
This formula gives you a structured way to estimate the cost to develop a HIPAA compliant AI healthcare software without guesswork.
A simple way to use this formula is to calculate the cost layer by layer:
Let's take ballpark figures for all the components of the formula which are as:
Estimated Initial Cost: (1200 × 60) + $18,000 + $15,000 + $10,000 + $6,000 = $121,000
Post-launch support is calculated separately because it depends on usage growth and ongoing system improvements after deployment.
This formula turns budgeting into a guided planning exercise. Once these layers are visible, the next step is to see how these numbers change across MVP, growth-stage, and enterprise healthcare software levels.

The clearest way to understand the cost breakdown to create HIPAA-compliant AI medical software is to align the budget with the stage of product maturity you actually need. The same healthcare idea can stay lean at pilot level or expand into a multi-system enterprise rollout, and that shift is what moves the investment from $40,000 to $400,000+.
Before we break each level down in detail, lets first look at how the budget typically spreads across product maturity stages.
|
Development Level |
Estimated Cost Range |
Best Fit For |
Budget Behavior |
|---|---|---|---|
|
MVP Level HIPAA-Compliant AI Healthcare Software |
$40,000- $90,000 |
workflow validation, provider usability testing |
focused compliance-safe pilot with one core workflow |
|
Mid-Level HIPAA-Compliant AI Healthcare Software |
$90,000- $200,000 |
multi-workflow automation and care-team expansion |
interoperability, dashboards, stronger governance |
|
Advanced Level HIPAA-Compliant AI Healthcare Software |
$200,000- $400,000+ |
multi-hospital, enterprise-grade rollout |
predictive workflows, cross-system orchestration, enterprise scale |
With the budget spread now clear, the next step is to understand what each maturity level includes from a delivery and compliance standpoint:
Estimated Cost Range: $40,000-$90,000
At this stage, the budget is meant to validate one focused healthcare workflow inside a secure compliance boundary. The goal is to test provider usability, patient data handling, and one outcome-driven workflow before committing to deeper automation.
Most of the budget usually flows into:
Also Read: Generative AI App Development for Startups and Enterprises
Estimated Cost Range: $90,000-$200,000
This is where the product starts moving from validation into operational expansion. Budget increases because multiple workflows, care-team roles, and stronger interoperability begin entering the roadmap.
Most of the spend now expands into:
Also Read: AI Remote Patient Monitoring App Development Guide
Estimated Cost Range: $200,000-$400,000+
At this level, the investment supports scale across hospitals, specialties, and connected provider ecosystems. This is where the roadmap often evolves into broader enterprise AI solutions with predictive workflows and cross-department intelligence.
The higher budget is usually driven by:
This maturity-based view makes AI healthcare software development cost with HIPAA compliance easier to justify because the budget now maps directly to where the product needs to operate next.

Once the product maturity level is clear, the next budgeting layer depends on the workflow you want AI to handle. This is where teams usually ask what is the total budget required to create compliant AI healthcare software solutions, because the answer changes based on what you are automating in your healthcare operations.
Let's look at cost of HIPAA compliant AI healthcare software by its use cases:
Estimated Cost: $50,000-$110,000
This budget range usually stays focused on secure conversation workflows, escalation logic, and PHI-safe interaction storage. Costs rise further when an AI healthcare virtual assistant needs provider-side visibility, multilingual support, and secure escalation across care teams.
Most of the spend typically goes into:
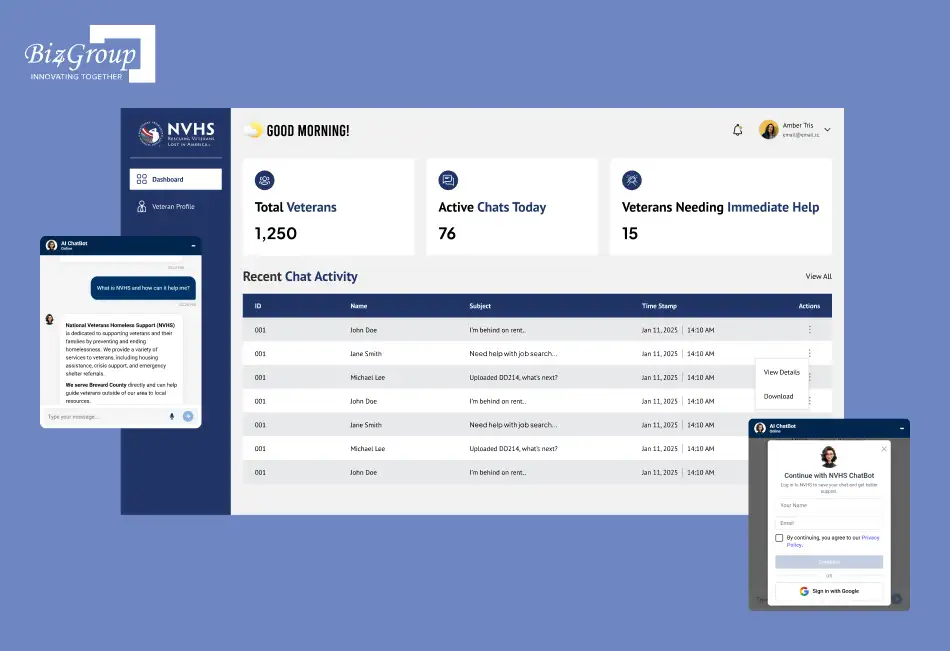
NVHS is an AI-powered virtual support assistant built to help homeless and at-risk veterans who needed fast access to healthcare and crisis assistance through voice or text.
The cost of development was controlled by aligning the process only on one conversational support journey. It focused on intent capture, crisis detection, location-based service matching, and secure case continuity through the admin dashboard. The focused chatbot architecture helped us deliver secure escalation logic and provider-side visibility without expanding the budget into broader multi-workflow healthcare systems,
Also Read: AI Virtual Assistant Development Cost
Estimated Cost: $120,000-$220,000
This use case carries higher HIPAA-compliant AI healthtech software development pricing because predictive analysis, provider dashboards, and risk scoring require stronger data pipelines and clinical transparency.
Budget is usually shaped by:
Estimated Cost: $80,000-$160,000
The pricing of building AI healthcare software with compliance increases here because continuous patient data movement, journaling, alerting, and device-linked workflows expand the compliance boundary.
Most of the budget usually flows into:
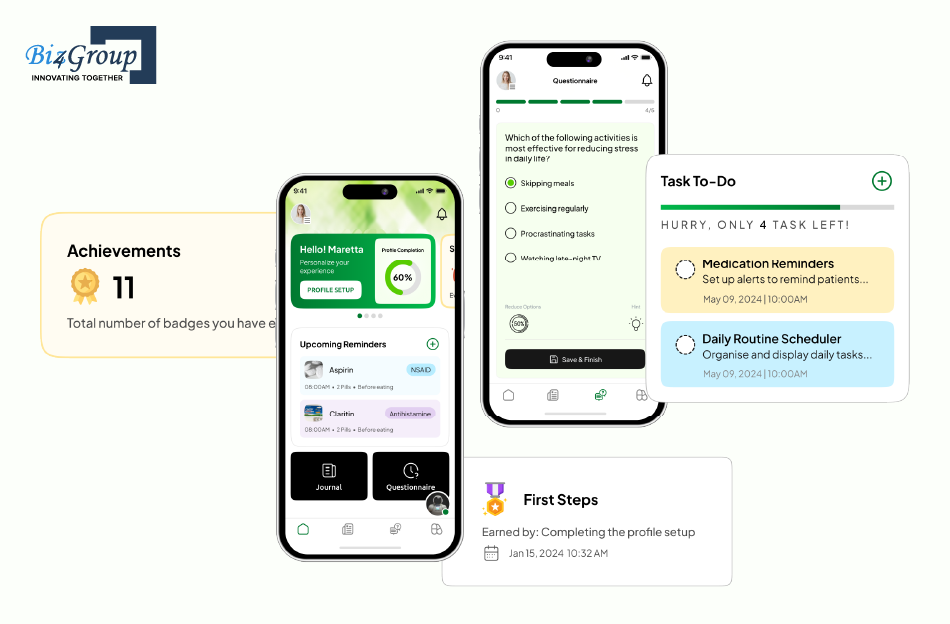
CogniHelp, is an AI-powered cognitive care app for dementia patients that supports memory reinforcement, daily journaling, emotion-aware conversations, and secure caregiver dashboards.
To keep the solution under budget, we deliberately centered the roadmap on one remote cognitive care journey instead of expanding into full hospital-side patient monitoring. This helped us direct the investment only toward journaling workflows, caregiver alerts, and secure long-term activity tracking, keeping the compliance and data-storage cost aligned with the use-case budget.
Estimated Cost: $70,000-$140,000
This cost range usually increases when secure voice capture, note structuring, and compliant storage all need to work across clinician workflows. The budget rises further when systems must integrate healthcare platforms with AI EHRs for real-time record sync and provider review.
Most of the spend usually flows into:
Also Read: How to Build a Speech Recognition System With AI?
Estimated Cost: $100,000-$250,000+
This budget range expands when AI begins handling scheduling, billing, approvals, and hospital-side coordination. Costs increase faster where agentic AI development supports adaptive routing, cross-team workflows, and real-time operational decisions.
The higher budget is usually driven by:
Also Read: How to Build Agentic AI in Healthcare
This use-case view makes the cost to develop a HIPAA compliant AI healthcare software far easier to map against real healthcare outcomes. When the workflow is clearly defined, the budget stops feeling broad and starts aligning directly with the exact clinical, documentation, or operational problem you need AI to solve next.
The workflow decides the budget long before engineering hours ever begin
Get a Cost Consultation
The HIPAA-compliant AI healthcare software development cost becomes easier to estimate when you isolate the decisions that directly expand scope. For hospital administrators and healthtech entrepreneurs, these cost factors are what separate a controlled roadmap from a budget that grows unpredictably.
and healthcare AI developers
The number of workflows your platform supports directly affects budget because every added clinical path increases logic validation, user roles, and exception handling. A focused documentation workflow stays lean while triage, monitoring, and risk scoring together increase the engineering depth significantly. The broader the care journey, the more coordination layers must be secured and tested across the system.
Example: A single workflow may stay within $50,000-$80,000, while multi-workflow clinical support can exceed $180,000.
Security cost rises with the number of users, departments, and access conditions the platform must support. Role-based permissions, encryption, audit trails, and session controls all add engineering effort because every access point must be traceable and compliant. This factor becomes especially critical in provider environments where multiple teams touch the same patient workflow.
Example: Basic PHI protection may add $8,000-$15,000, while hospital-wide access governance can exceed $30,000.
The quality and variety of healthcare data used for AI directly shape data preparation costs. More records, voice inputs, images, and longitudinal patient histories increase cleaning, labeling, validation, and retraining effort. This budget expands quickly when accuracy needs to hold across specialties, age groups, and treatment patterns.
Example: Limited structured datasets may cost $10,000-$18,000, while broader patient pipelines can cross $35,000.
The more systems your software needs to connect with, the more the budget shifts toward integration engineering and workflow testing. Syncing data across EHRs, FHIR endpoints, imaging systems, and billing tools requires secure field mapping and error recovery logic. This factor often becomes one of the biggest drivers for provider-side deployments.
Example: One EHR connection may add $12,000-$20,000, while multi-system interoperability can exceed $50,000.
Costs change depending on whether you fine-tune an existing AI model or introduce custom healthcare reasoning layers. Customization adds validation depth, performance testing, and more control over outputs, which increases development hours. This is where healthcare AI developers usually influence the roadmap most.
Example: Fine-tuning may cost $10,000-$18,000, while custom clinical reasoning layers may add $35,000+.
Also Read: Cost to Hire an AI Software Developer in 2026
Healthcare interfaces must reduce user friction for clinicians, care teams, and admins. The more roles the product supports, the more user journeys, dashboards, and workflow handoffs need design and testing cycles. This factor matters heavily for hospital administrators who require visibility without slowing staff workflows.
Example: Basic role UX may add $6,000-$10,000, while multi-role workflow design can exceed $22,000.
This layer includes penetration testing, audit readiness checks, access validation, and workflow traceability. The budget rises because HIPAA validation is not standard QA; it requires proof that every secure workflow behaves correctly under real provider usage conditions. For healthtech entrepreneurs, this often decides enterprise readiness.
Example: Standard compliance testing may cost $6,000-$10,000, while enterprise-grade validation can exceed $25,000.
The team model directly affects speed, quality, and long-term support costs. A lean external team may control short-term spending, while a healthcare-specialized delivery partner increases upfront investment but reduces compliance and rework risks. This factor changes how predictable the roadmap stays over time.
Example: A small MVP team may stay within $60,000-$80,000, while a healthcare-focused full delivery model can exceed $150,000.
These 8 cost drivers make the cost to develop a HIPAA compliant AI healthcare software much easier to justify because every budget increase now ties back to a clear product, compliance, or delivery decision.

The most practical way to understand the detailed cost to build HIPAA-compliant AI healthcare system is to follow how the budget moves across each delivery phase. This makes it easier to see where the spend stays strategic and where it starts expanding faster.
This phase budget stays focused on defining workflow boundaries, PHI scope, and early compliance assumptions. The spend remains controlled because this stage is about reducing scope mistakes before engineering starts.
Most of the budget usually goes into:
Estimated Cost: $8,000-$15,000
This phase budget increases around secure data movement, retention planning, and risk visibility. The cost expands here because future AI workflows depend heavily on how data boundaries are defined early.
Most of the spend usually flows into:
Estimated Cost: $10,000-$18,000
Also Read: Why AI Projects Fail in Companies That Lack AI Readiness?
This phase cost is driven by infrastructure layout, service boundaries, and cloud readiness. The budget grows here because system scale, access zones, and secure interoperability are decided at this stage.
Most of the cost usually covers:
Estimated Cost: $12,000-$22,000
This budget is shaped by role-based journeys, workflow screens, and provider usability depth. The spend often rises when a UI/UX design company supports complex patient and clinician workflows.
Most of the spend usually covers:
Estimated Cost: $8,000-$16,000
Also Read: Top UI/UX Design Companies in USA
This is the first major engineering phase where MVP development services validate one secure healthcare workflow. Budget stays focused on proving usability and compliance before broader expansion.
Most of the budget usually goes into:
Estimated Cost: $25,000-$50,000
Also Read: Top MVP Development Companies in USA
This is usually the largest phase because integration of AI models, dashboards, and broader building of AI softwares workflows expand the roadmap quickly. The cost rises further when care automation and AI chatbot integration enter provider workflows.
Most of the spend usually flows into:
Estimated Cost: $40,000-$90,000
This final phase budget supports secure release, environment hardening, and workflow stability improvements. The spend here protects performance and compliance confidence after rollout.
Most of the cost usually covers:
Estimated Cost: $12,000-$25,000
Also Read: Software Testing Companies in USA
|
Development Phase |
Estimated Cost |
Typical Timeline |
Budget Focus |
|---|---|---|---|
|
Discovery and Compliance Scoping |
$8,000-$15,000 |
1-2 weeks |
workflow boundaries, PHI scope, requirement clarity |
|
Data Risk Assessment and Planning |
$10,000-$18,000 |
1-2 weeks |
secure data flow, retention, risk visibility |
|
Secure Architecture Design |
$12,000-$22,000 |
2-3 weeks |
infrastructure layout, boundaries, cloud readiness |
|
UI and UX Workflow Design |
$8,000-$16,000 |
1-2 weeks |
provider journeys, patient workflows, usability |
|
MVP Engineering and Validation |
$25,000-$50,000 |
4-6 weeks |
core secure workflow, limited APIs, validation |
|
AI and Core Functionality Expansion |
$40,000-$90,000 |
6-10 weeks |
AI modules, dashboards, automation, integrations |
|
Testing, Deployment, and Continuous Optimization |
$12,000-$25,000 |
2-3 weeks |
compliance validation, release hardening, monitoring |
The phase-wise structure makes the cost to develop a HIPAA compliant AI healthcare software much easier to map because every budget layer now connects directly to a specific delivery stage.
The biggest cost leaks usually hide between roadmap phases not inside features
Discuss Your Roadmap
The budget usually feels predictable until the non-obvious cost layers begin surfacing after core development is scoped. This is where the cost to make AI healthcare software with HIPAA standards often expands unexpectedly, because legal, governance, and long-term operational controls introduce spend that rarely appears in early estimates.
This hidden cost starts showing up when security policies, workflow evidence, and access histories must be formally documented for enterprise buyers and regulated deployments. It becomes more visible when compliance managers require proof-ready artifacts beyond product delivery.
Third-party APIs, cloud vendors, and data processors often introduce extra-legal and monitoring costs after architecture decisions are finalized. These costs rise faster during custom AI healthcare software development where multiple external systems support the workflow.
Hidden spend appears after deployment when selected AI models require retraining reviews, output audits, and safe performance checks as patient workflows evolve beyond original data assumptions.
The infrastructure layer brings recurring hidden costs tied to secrets lifecycle controls, encrypted backups, and recovery readiness. These costs become more visible for healthcare IT leaders handling multi-team access.
As provider teams expand, access matrices, workflow permissions, and audit visibility begin creating operational costs that were outside the early rollout estimate.
Even secure systems need a reserve budget for escalation workflows, response playbooks, and breach simulation drills before enterprise-wide rollout.
The real budget risk is not the visible roadmap, but the costs that start surfacing after deployment, audits, and team expansion. Planning these hidden layers early keeps the cost to build secure AI healthcare software with HIPAA compliance realistic and prevents avoidable budget pressure later in the lifecycle.
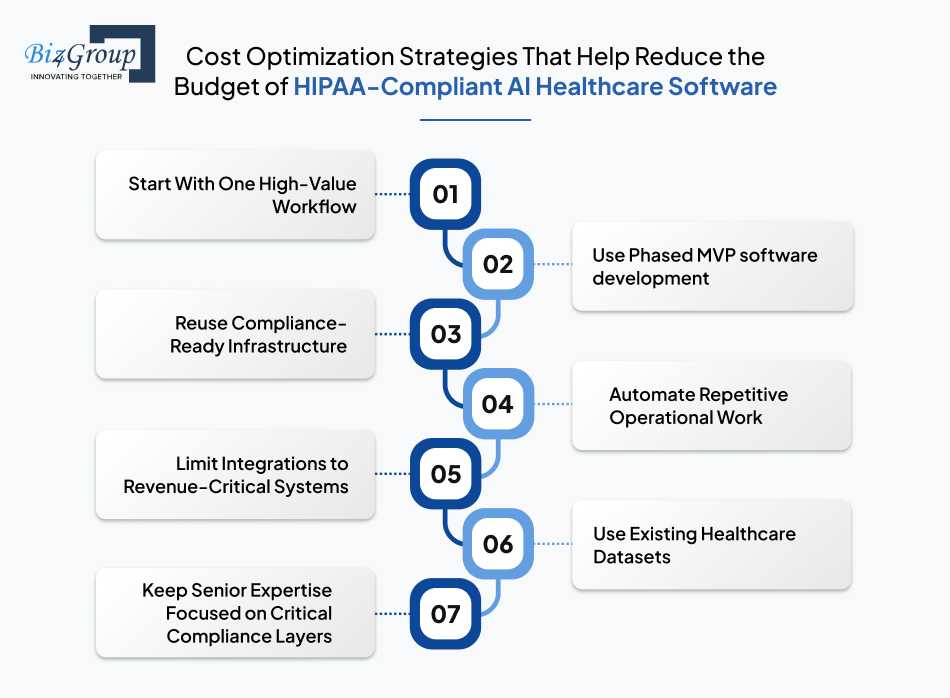
The budget becomes easier to control when cost-saving decisions are made at the roadmap level instead of after engineering begins. If you're also wondering how to reduce cost when developing HIPAA-compliant healthcare software?
Then the answer lies in reducing rework, limiting avoidable integrations, and validating the right workflow depth before the roadmap expands. Have a look:
The fastest way to reduce waste is to limit the first release to one workflow that directly proves provider value. This keeps the cost to create HIPAA-compliant AI healthcare software tied to measurable adoption instead of broad feature assumptions.
A practical way to keep the spend controlled is to focus on:
Cost Savings: This strategy usually keeps 12%–18% of avoidable spend under control, which often protects $12,000–$18,000 in a $100,000 roadmap.
A phased rollout for MVP software development prevents budget leakage caused by full-scale engineering before provider validation. This is especially effective for healthcare startup founders trying to prove workflow-market fit without overcommitting infrastructure spend.
The budget stays leaner when the first release focuses on:
Cost Savings: A staged rollout generally improves budget efficiency by 15%–20%, translating to roughly $15,000–$20,000 saved on a $100,000 project.
Also Read: How to Build AI EHR MVP for Healthcare Businesses
A large portion of cost overruns comes from rebuilding security controls that can be standardized. Reusing audit trails, access controls, and encryption templates helps reduce repeated compliance engineering.
This optimization usually works best through:
Cost Savings: Reusing proven security and audit layers typically preserves 8%–12% of the budget, or nearly $8,000–$12,000 on every $100,000 implementation.
Manual operational workflows quietly increase long-term budget pressure. This is where AI automation tools reduce repeated support, routing, and internal monitoring costs.
Budget efficiency improves when you automate:
Cost Savings: Operational automation often lowers recurring engineering and support spend by 10%–14%, which can protect around $10,000–$14,000 in a $100,000 build.
AI integrations expand cost faster than most teams expect, especially during early rollout. Keeping only business-critical systems in scope helps avoid integration-heavy rework.
This usually means prioritizing:
Cost Savings: Keeping integrations tightly controlled can prevent 10%–16% of unnecessary expansion costs, equal to nearly $10,000–$16,000 on a $100,000 scope.
Also Read: Cost of Implementing AI in Healthcare
A large part of unnecessary spending comes from collecting and preparing more patient data than the first workflow actually needs. Keeping early AI model raining limited and already structured datasets helps reduce labeling, cleaning, and retraining costs.
This keeps the budget optimized by focusing on:
Cost Savings: Restricting early AI training to one workflow usually reduces data preparation and retraining costs by 9%–13%, preserving roughly $9,000–$13,000 on a $100,000 roadmap.
Budget often slips when high-cost senior resources stay involved in lower-complexity execution work. The smarter optimization is to keep senior architects and compliance specialists focused only on access controls, PHI workflows, and high-risk decision paths.
This improves cost efficiency through:
Cost Savings: Better senior resource allocation typically improves delivery efficiency by 7%–11%, which often translates into $7,000–$11,000 saved on a $100,000 engagement.
|
Optimization Strategy |
Primary Budget Benefit |
Estimated Savings |
|---|---|---|
|
Start With One High-Value Workflow |
reduces unnecessary feature scope and validation waste |
12%–18% |
|
Use Phased MVP Rollout |
prevents early overengineering and infra overspend |
15%–20% |
|
Reuse Compliance-Ready Infrastructure |
cuts repeated security and audit engineering |
8%–12% |
|
Automate Repetitive Operational Work |
lowers recurring support and workflow review costs |
10%–14% |
|
Limit Integrations to Revenue-Critical Systems |
avoids unnecessary API and sync complexity |
10%–16% |
|
Use Existing Healthcare Datasets |
controls data preparation and retraining scope |
9%–13% |
|
Focus Senior Expertise on Critical Compliance Layers |
improves specialist resource efficiency |
7%–11% |
For healthcare business owners, the real savings come from reducing unnecessary scope before it turns into engineering effort. That is how you build compliant AI healthcare software without overspending while still protecting long-term scale and compliance confidence.
Smarter rollout choices often save more than feature cuts ever can
Optimize My BudgetWhen teams ask how to create HIPAA-compliant AI healthcare software within budget, the answer usually depends on how early scope discipline, workflow focus, and reusable compliance layers enter the development roadmap. That is exactly where Biz4Group LLC defines the standards.
In our experience as a healthcare software development company, cost stays controlled when we align the product around one measurable healthcare outcome before expanding the PHI boundary. Here's the proof:
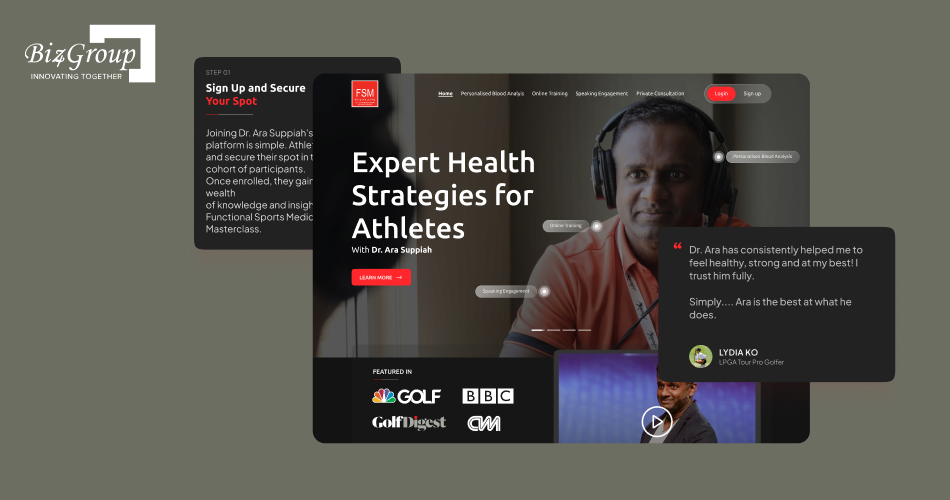
Dr. Ara is an AI-powered athletic health intelligence platform that enables users to upload blood reports, receive AI-led interpretation, and get personalized guidance around nutrition, sleep, and recovery.
By keeping Dr. Ara focused on one tightly scoped, high-impact workflow, we were able to keep the budget under control from the start. The PHI boundary stayed limited to uploaded reports and health tracking instead of expanding into broad hospital interoperability. This kept compliance and validation costs far more manageable while allowing the solution to scale gradually after proven returns.
Truman is an AI-powered avatar wellness platform that enables users to interact with a lifelike AI health avatar. The AI avatar delivers personalized supplement recommendations, helps users maintain a secure health history, and supports seamless membership and product transactions within one connected system.
By consolidating consultations, commerce, and user data into a shared architecture, we kept recurring engineering and maintenance costs under control. This reduced duplicated workflow logic, limited repeated validation across disconnected tools, and made long-term scaling far more budget efficient.
This is the same cost discipline we use to reduce the cost to develop HIPAA-compliant AI healthcare software. Keeping consultations, secure health data, and transactions inside one connected workflow help reduce recurring engineering effort by lowering repeated compliance checks and keeping maintenance budgets under control.
Our healthcare AI delivery model keeps compliance aligned without bloating long-term budgets
Talk to Biz4GroupWhen planning HIPAA compliant AI healthcare software, the real decision is rarely about numbers alone. It is about how confidently you can align compliance, workflow value, and long-term product growth without letting the budget drift into avoidable rework.
This pricing guide to develop HIPAA-compliant AI healthcare software in 2026 will help you think more clearly, not just as a cost estimate, but as a roadmap for making smarter product decisions with the right AI development company. At Biz4group LLC, the most successful healthcare AI products begin with a controlled scope, secure workflow boundaries, and budget discipline that supports measurable outcomes.
When those foundations are set early, compliance becomes easier to sustain, and cost stays aligned with business goals. If you are planning to create secure AI healthcare software with HIPAA and want the roadmap to stay practical from day one, talk to us for shaping the right budget around outcome you need to deliver.
Yes, but the real cost impact depends on whether the delivery partner already has healthcare workflow experience, PHI-safe engineering standards, and reusable compliance controls. For CTOs and compliance managers, outsourcing usually becomes budget-efficient when the team can reduce rework, shorten audit preparation, and avoid architecture mistakes that inflate long-term cost.
The delivery model changes both speed and budget predictability. A lean cross-functional team keeps the early roadmap efficient, while larger specialist teams increase upfront cost but reduce risk for enterprise healthcare rollouts. For healthcare startup founders, the right structure is the one that matches compliance depth with release maturity.
The first release budget is only part of the financial picture. Long-term ownership includes compliance audits, model monitoring, cloud hardening, access reviews, and workflow updates. For hospital administrators and healthcare IT leaders, this recurring layer often ranges between 15%–20% of the initial annual build cost.
Return on investment usually depends on how quickly the software reduces documentation load, operational delays, or provider-side inefficiencies. For clinic owners and enterprise decision makers, focused workflows like AI documentation or patient routing often start showing measurable ROI within 6–12 months.
Not always. The cost decision depends on whether the workflow needs healthcare-specific reasoning, explainability, or unique provider logic. For digital health companies, adapting existing secure models often keeps the HIPAA-compliant AI healthcare software development cost lower during early rollout, while custom models become more valuable after workflow validation.
Budget expands significantly when the HIPPA-compliant AI healthcare software must support multiple hospitals, care networks, or regions with different governance and infrastructure rules. Enterprise decision makers should expect higher spend around access segmentation, deployment environments, audit controls, and legal review when scaling beyond a single provider ecosystem.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.