Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

“Why is our billing team still spending hours correcting the same ICD 10 coding mistakes, modifier errors, and missing medical necessity details even after claims pass through our existing scrubber?”
That question is becoming increasingly common across hospitals, specialty clinics, and medical billing companies dealing with rising claim volumes and growing payer scrutiny. Many revenue cycle teams are now discovering that manual claim review workflows cannot keep up with changing payer requirements and recurring submission errors.
The pressure becomes harder when rejected claims continue piling up despite repeated rework efforts. Here’s something you should know:
For many organizations, the issue is no longer limited to billing inefficiency. It is directly affecting cash flow, staff productivity, and reimbursement timelines. As claim complexity increases, operational gaps start becoming more visible across revenue cycle teams:
This is where AI claim scrubber software development is gaining attention across healthcare organizations focused on improving clean claim performance through intelligent automation.
Many providers are now prioritizing building an AI claim scrubber system with real time dashboard analytics showing clean claim rates rejection patterns and financial impact. To understand why this shift is accelerating, it is important to first examine where traditional claim scrubbing workflows start breaking down. Let’s start:
Traditional claim scrubbers still depend heavily on static validation rules and predefined edit libraries. That creates serious operational gaps for healthcare organizations managing large claim volumes across:
Billing teams often discover claim issues only after submission because existing systems fail to adjust quickly to changing payer requirements. Here’s what happens:
Most traditional scrubbers require manual rule updates whenever payer policies, modifier guidelines, or documentation requirements change. As those updates fall behind:
The problem becomes more visible in organizations handling complex billing environments:
Many billing teams still depend on manual review workflows to catch errors missed during automated scrubbing. As claim volumes increase:
Traditional scrubbers provide limited visibility into recurring denial behavior. They can identify known rule violations, but they cannot learn from historical payer responses or detect growing rejection trends automatically. This leaves revenue cycle teams reacting to problems after reimbursements slow down instead of preventing those issues earlier in the workflow.
These operational limitations are pushing healthcare organizations toward AI claim scrubbing systems that can continuously analyze claim behavior, adapt validation logic dynamically, and improve submission accuracy over time.
Also Read: How to Develop a Healthcare Revenue Cycle Management Software (RCM)
The next section explains how AI claim scrubber software actually changes modern revenue cycle workflows.
AI claim scrubber software is a healthcare billing validation system that reviews medical claims before submission to identify coding inconsistencies, modifier conflicts, missing documentation, eligibility mismatches, and payer-specific submission issues automatically.
The software uses trained AI models, historical claim behavior, and continuously updated payer rules to examine claims across multiple validation layers before they are submitted to insurance payers. Instead of depending only on fixed edit libraries, the system analyzes claim patterns dynamically during the billing workflow.
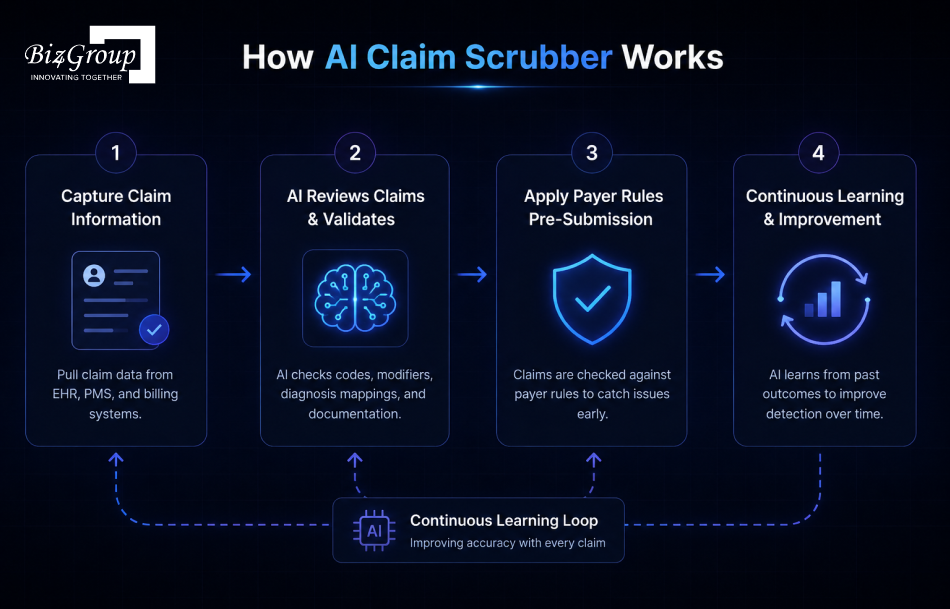
Now, let’s see how AI claim scrubber software actually works:
Also Read: How to Integrate Healthcare Platforms with AI EHRs
AI claim scrubber software brings automated intelligence into pre-submission billing workflows, helping healthcare organizations strengthen claim review processes before payer submission begins.
Smarter claim review starts before claims ever reach payer systems
Audit Our Claim Workflow
Many healthcare organizations still lose valuable reimbursement time because small claim issues remain undetected until after submission. Some claims contain coding inconsistencies, while others fail because of missing documentation, modifier conflicts, or payer-specific validation gaps.
AI claim scrubber software helps billing teams identify these issues earlier by reviewing claims across multiple billing and payer validation layers simultaneously. Thes are:
AI claim scrubbers can identify mismatches between patient eligibility records and claim details before submission. These issues often appear when insurance coverage changes; policy information becomes outdated, or authorization requirements are missing during claim creation.
Common eligibility-related issues include:
Coding errors remain one of the most common causes of rejected healthcare claims. AI models review diagnosis codes, procedure codes, and clinical documentation together to identify unsupported or conflicting claim information.
The software can detect:
Certain payer rules require specific modifier combinations and billing sequences for reimbursement approval. AI claim scrubbers analyze these relationships during pre-submission review to identify conflicts earlier.
Common modifier-related issues include:
Claims may also fail because provider records, taxonomy information, or supporting documentation contain inconsistencies. AI claim scrubber software reviews these administrative details automatically during claim preparation workflows.
The software can identify:
Different insurance payers apply different billing and reimbursement requirements. AI claim scrubbers continuously review payer-specific validation rules during claim processing to identify submission risks before claims are sent for adjudication.
These systems can detect:
AI claim scrubber software development for healthcare helps organizations detect a wider range of billing and submission issues earlier in the revenue cycle workflow before claims reach insurance payers.
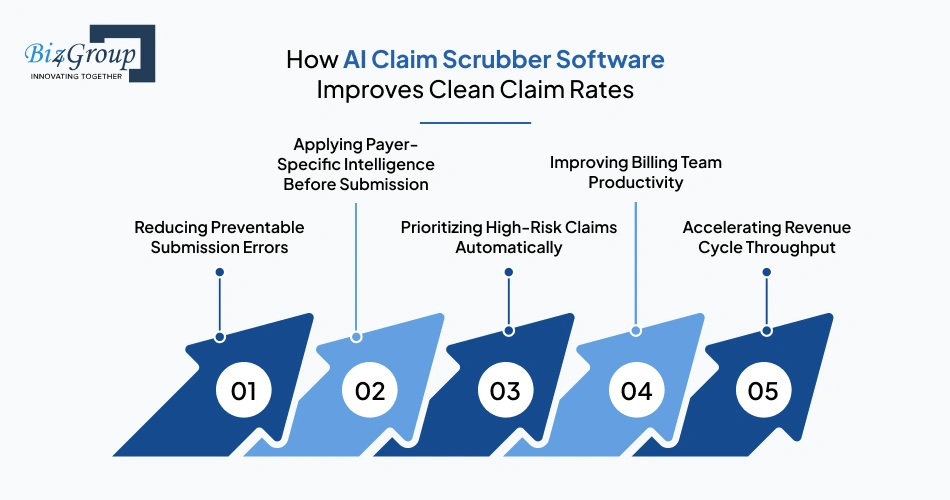
Clean claim rates depend heavily on how early billing issues are identified during the submission workflow. Creating an AI claim scrubbing software for insurance companies helps them strengthen claim quality before claims move to payers. Here’s how it helps:
AI claim scrubbers review claims across multiple validation layers before submission begins. This allows billing teams to identify incomplete claim details, coding inconsistencies, and documentation gaps earlier within the workflow.
As fewer preventable issues move into payer review stages, claim correction queues become easier to manage across billing operations.
Also Read: AI Medical Coding Software Development
Different insurance payers apply different reimbursement and validation requirements during claim adjudication. AI claim scrubbers continuously evaluate claims against payer-specific edits before submission to reduce mismatches that often trigger avoidable rejections.
This helps billing teams prepare cleaner submissions across different payer plans without relying heavily on repetitive manual review processes.
Also Read: How to Build an AI Medical Billing Software
AI models can identify claims showing patterns commonly associated with submission issues or payer review delays. Billing teams can then review higher-risk claims earlier before those claims enter rejection workflows. This creates better visibility into claim processing priorities during high-volume billing operations.
Manual correction workflows often force billing teams to spend hours reviewing recurring submission issues repeatedly. AI claim scrubbers reduce that administrative burden by flagging claim risks earlier and recommending corrective actions during review stages.
In fact, 69% of healthcare providers using AI solutions report reduced denials and higher resubmission success rates because billing teams can respond to claim issues more efficiently during pre-submission review workflows.
Cleaner submissions help claims move through payer processing stages with fewer interruptions caused by avoidable corrections and repeated billing reviews. This creates faster claim movement across revenue cycle workflows and reduces operational slowdowns tied to claim rework activities.
AI powered claim scrubbing software development helps healthcare organizations strengthen claim submission quality while improving billing workflow efficiency across modern revenue cycle operations.
Cleaner submissions create faster reimbursements and fewer correction cycles across billing operations
Improve Our Clean Claim RateTeams evaluating intelligent claim scrubber platform development usually care need to know where the money comes back from. Well, the value shows up when cleaner submissions reduce avoidable rework, move claims faster, and protect revenue that would otherwise get tied up in correction loops.
Every denied claim creates direct cost pressure on billing operations. Reworking a denied claim can cost between $25 and $181, depending on the claim type and the time needed to correct it. AI claim scrubber software reduces how often those claims cycle back into manual review.
When fewer claims reach denial queues, billing teams spend less time chasing payer responses and resubmission tasks. That gives denial staff more room to focus on the claims that truly need attention instead of handling repeat correction work.
Cleaner claims move through payer review with fewer interruptions. That helps shorten the time between submission and payment, especially when claims are not pushed back for avoidable corrections.
When staff are not spending hours fixing the same claim issues, the same team can handle more work without expanding headcount at the same pace. That improves labor efficiency across the revenue cycle.
A stronger clean claim rate creates steadier cash movement and less revenue stuck in correction queues. Automated transactions have also been linked to a 17% increase in administrative cost avoidance, which shows how much financial pressure can be reduced when claim handling becomes more efficient.
That is the financial case behind claim scrubbing automation software development. It is not about adding another billing layer. It is about recovering revenue faster, spending less to correct claims, and keeping more of the work inside a controlled workflow.
|
Aspect |
Traditional Claim Scrubbing Systems |
AI Claim Scrubber Software |
|---|---|---|
|
Validation Logic |
Uses predefined static rule libraries |
Uses dynamic validation models that adjust with claim behavior |
|
Payer Rule Handling |
Requires manual rule updates |
Continuously reviews payer-specific submission patterns |
|
Claim Review Process |
Reviews claims against fixed edit conditions |
Evaluates claims across multiple validation layers simultaneously |
|
Error Detection Scope |
Identifies known billing rule violations |
Detects recurring submission risks and evolving billing inconsistencies |
|
Denial Pattern Analysis |
Limited visibility into recurring rejection trends |
Reviews historical payer responses and recurring claim behavior |
|
Handling Specialty Billing |
Generic validation across different specialties |
Reviews specialty-specific billing requirements during claim processing |
|
Manual Review Dependency |
Heavy dependence on billing staff review queues |
Reduces repetitive manual correction review cycles |
|
Claim Prioritization |
Reviews claims in standard processing order |
Identifies higher-risk claims during pre-submission review |
|
Workflow Adaptability |
Slower adjustment to billing changes |
Continuously refines review logic using ongoing claim outcomes |
|
Operational Scalability |
Increased claim volume requires more manual review effort |
Handles growing submission volume with more automated review support |
Cleaner claim submissions depend heavily on how accurately the system can review billing data before claims move to insurance payers. Healthcare organizations evaluating AI claim scrubber software development often focus on features that reduce repetitive correction work, strengthen claim review workflows, and support high-volume billing operations consistently.
The following capabilities play a critical role across modern claim scrubbing environments.
These features help billing teams review claim information more accurately during pre-submission workflows.
|
Feature |
Purpose |
|---|---|
|
AI Claim Validation Engine |
Reviews claims for coding inconsistencies, missing details, and billing conflicts automatically |
|
Predictive Analysis for Claim Risk |
Identifies claims showing patterns commonly linked to submission issues |
|
Real-Time Claim Review Alerts |
Notifies billing teams about validation issues before submission |
|
Diagnosis and Procedure Matching |
Reviews CPT and ICD 10 relationships during claim preparation |
|
Modifier Validation Checks |
Detects invalid or missing modifier combinations during review workflows |
Also Read: AI Predictive Diagnosis and Disease Forecasting Software Development
Payer-specific review capabilities help billing teams manage changing reimbursement requirements across different insurance plans.
|
Feature |
Purpose |
|---|---|
|
Payer-Specific Rule Validation |
Reviews claims against plan-level billing requirements before submission |
|
Eligibility Verification Integration |
Checks patient eligibility details during claim preparation |
|
Authorization Validation Tracking |
Reviews authorization-linked claim conditions before payer submission |
|
Timely Filing Monitoring |
Flags claims approaching payer filing deadlines |
|
LCD and NCD Rule Checks |
Reviews claims against payer medical necessity requirements |
Operational workflow features help billing teams manage submission volume and repetitive review activities more efficiently.
|
Feature |
Purpose |
|---|---|
|
Automated Claim Queue Prioritization |
Organizes higher-risk claims for earlier review |
|
Bulk Claim Review Processing |
Supports large-volume claim validation workflows |
|
Claim Correction Recommendations |
Suggests review areas requiring billing team attention |
|
Multi-Specialty Workflow Support |
Handles claim review requirements across different specialties |
|
Multi-Client Billing Management |
Supports separate workflows for billing companies managing multiple provider accounts |
Reporting capabilities help billing teams monitor submission quality and recurring billing patterns more effectively.
|
Feature |
Purpose |
|---|---|
|
Clean Claim Rate Tracking |
Monitors submission quality trends across billing workflows |
|
Rejection Pattern Reporting |
Tracks recurring payer rejection behavior |
|
Claim Review Activity Logs |
Records billing review actions across workflows |
|
Department-Level Reporting |
Reviews claim performance across specialties or provider groups |
|
Financial Impact Dashboards |
Tracks claim correction trends and reimbursement movement |
These capabilities support clean claim rate improvement software development with AI by helping healthcare organizations strengthen claim review workflows, manage submission accuracy more effectively, and maintain better visibility across complex billing operations.
Modern claim review systems require automation built around real payer behavior patterns
Show Us the Right Feature Stack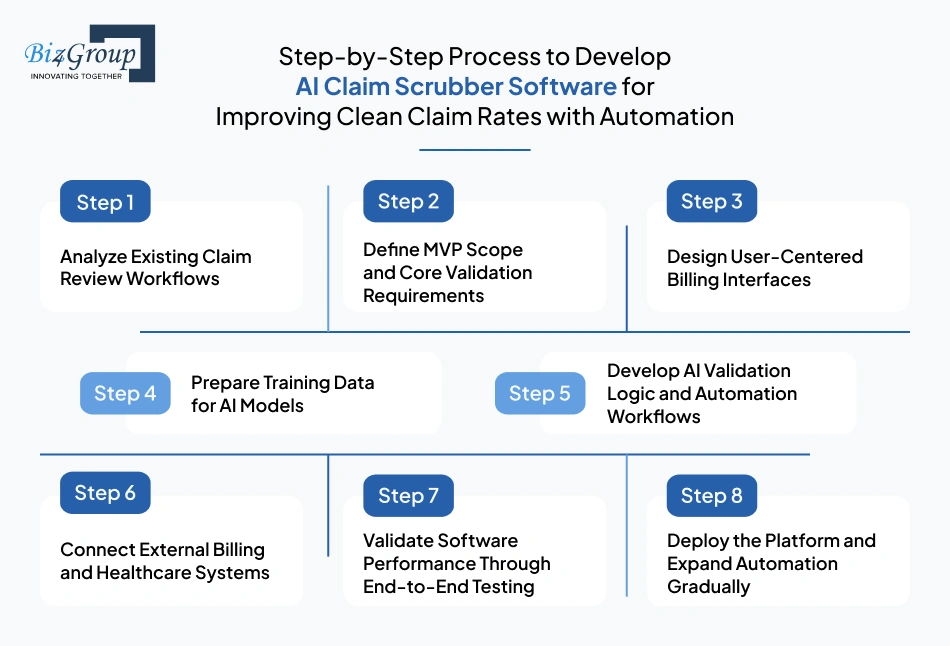
Healthcare organizations planning to create an AI claim scrubbing software with machine learning denial prediction and automated coding validation capabilities usually need more than a billing tool. They need a structured development process that aligns payer workflows, claim review operations, and AI-driven validation logic into a single operational system.
The following steps show how successful claim scrubber platforms are typically developed for real healthcare billing environments.
The development process starts with understanding how claims currently move across billing operations. This includes reviewing rejection patterns, payer workflows, coding review processes, and existing correction cycles.
Key focus areas usually include:
Also Read: How to Integrate AI with EHR/EMR Systems to Transform Healthcare Operations?
The next step focuses on identifying the minimum operational capabilities required for launch. Many healthcare organizations begin with focused validation workflows before expanding into broader automation. Teams often work with providers offering MVP development services to define initial functionality clearly.
The MVP scope usually includes:
Also Read: Top MVP Development Companies in USA
Billing teams work inside claim review screens for long operational hours every day. Poor workflow design slows claim handling and increases review fatigue. This is why healthcare organizations often collaborate with a specialized UI/UX design company while planning billing workflows and dashboard layouts.
This stage focuses on:
Also Read: Top UI/UX Design Companies in USA
AI validation systems require historical claim data to recognize recurring billing patterns and submission risks. Development teams organize claim records, denial histories, payer responses, and coding datasets before starting model training workflows.
This process typically includes:
Once training data is prepared, teams begin AI model development for coding validation, denial prediction, and payer-specific claim review workflows. Developers also integrate automated validation rules directly into billing operations during this stage.
Core activities usually include:
Also Read: How to Select the Best AI Model for Your Use Case?
AI claim scrubbers must exchange data with EHRs, billing systems, clearinghouses, and payer platforms continuously. Development teams establish secure API connections to support real-time claim validation workflows and external system communication.
This stage usually covers:
Also Read: A Complete Guide to OpenAI API Integration for AI Applications
Before launch, healthcare organizations must ensure claims move correctly across every review stage without creating billing interruptions. Many teams work with experienced software testing companies to validate operational stability across high-volume claim workflows.
Testing workflows commonly include:
Also Read: Top AI Software Development Companies in USA
The final stage focuses on production launch, operational monitoring, and workflow expansion. Many organizations first deploy the system within one specialty or payer environment before scaling broader automation workflows across departments. Teams also continue to integrate AI models over time as claim volume and payer complexity increase.
This stage usually includes:
Healthcare organizations following a structured custom claim scrubber software development integrating AI roadmap can manage implementation more effectively while aligning automation workflows with real billing operations.
When teams plan AI medical claim scrubber software development, the stack must keep the billing screen simple, move claim data reliably, support AI scoring, and stay manageable as the product grows.
The layers below show the parts that matter most when the platform must work inside real healthcare operations.
|
Architecture Layer |
Recommended Tool |
Purpose |
|---|---|---|
|
Frontend dashboard |
Next.js, React.js |
Supports ReactJS development and NextJS development for a billing dashboard that stays easy to use. |
|
Backend services |
Node.js, NestJS |
Supports NodeJS development for server-side requests, workflow control, and API handling. |
|
AI scoring layer |
Python, FastAPI |
Supports Python development for claim scoring and prediction APIs through a fast API framework. |
|
Data pipeline layer |
Airbyte, dbt |
Moves claim data from source systems into clean reporting inputs and turns raw warehouse data into trusted data products. |
|
Database layer |
PostgreSQL |
Stores claims, rules, users, and audit records in a relational database built for complex data workloads. |
|
Queue and cache layer |
Redis, RabbitMQ |
Keeps fast claim lookups and background work moving during heavy billing activity. |
|
Integration layer |
Mirth Connect |
Connects billing systems with external partners through a standards-based healthcare integration engine. |
|
Reporting layer |
Metabase |
Gives business users a place to ask questions about claim data and build dashboards. |
|
Security and access layer |
Keycloak |
Manages sign-in and access control with OpenID Connect and SAML support. |
|
Deployment and observability layer |
Docker, Kubernetes, Prometheus, Grafana, Sentry |
Packages the app into containers, scales it, and keeps system health and errors visible during release. |
The right stack keeps the system stable while claims move from review to release. It also gives the team a cleaner path for automated claim scrubbing system development, especially when the platform must grow without adding unnecessary complexity.
AI claim scrubber platforms handle protected health information, payer records, patient identifiers, clinical documentation, and financial data continuously. That makes governance, access control, and infrastructure security essential parts of HIPAA compliant claim scrubber AI software development.
The following areas require close attention while planning secure healthcare claim validation systems.
Also Read: HIPAA Compliant AI App Development for Healthcare Providers
Organizations planning to develop a HIPAA compliant AI claim scrubber software for medical billing companies must treat security governance and compliance controls as foundational requirements across the entire platform architecture.
Healthcare automation needs stronger governance before scaling across sensitive claim environments
Review Our Security Readiness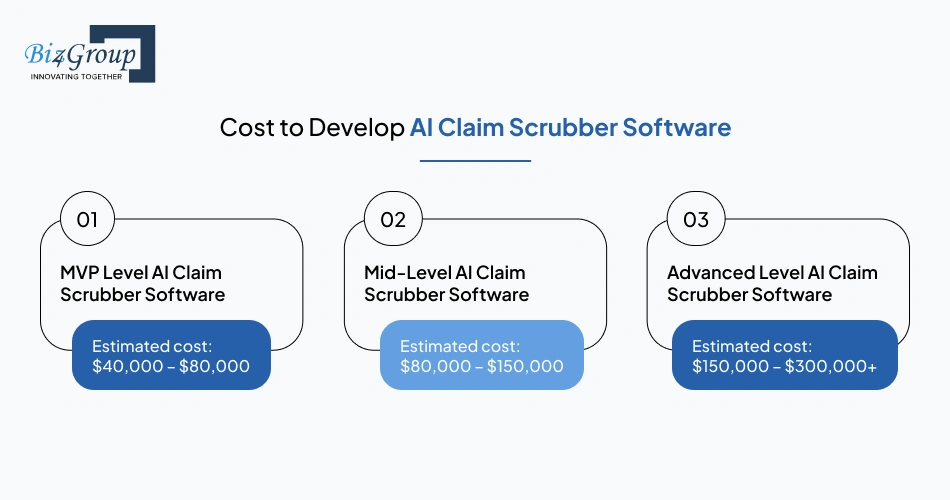
The cost to build an AI powered claim scrubbing system that catches duplicate claims coordination of benefits errors and authorization gaps usually falls between $40,000 and $300,000+. The final budget depends on how advanced the validation workflows, payer integrations, reporting systems, and automation layers become during development.
Organizations planning enterprise-scale platforms often spend more because the system must support larger claim volumes, specialty workflows, and ongoing AI refinement requirements.
|
Development Level |
Estimated Cost Range |
Scope |
|---|---|---|
|
MVP Level AI Claim Scrubber Software |
$40,000 – $80,000 |
Basic claim validation, limited payer rule checks, eligibility review workflows, dashboard visibility, essential automation support |
|
Mid-Level AI Claim Scrubber Software |
$80,000 – $150,000 |
Multi-payer support, denial prediction workflows, reporting systems, role-based access, clearinghouse integrations |
|
Advanced Level AI Claim Scrubber Software |
$150,000 – $300,000+ |
Advanced AI validation, specialty billing workflows, enterprise analytics, large-scale automation, multi-system integrations |
Estimated Cost Impact: $15,000 – $60,000
Simple claim validation workflows cost less because they mostly depend on predefined review conditions. Costs increase when the platform starts analyzing historical denials, recurring rejection behavior, and payer-specific submission patterns.
Advanced prediction models require larger datasets, repeated testing cycles, and continuous tuning before they become reliable enough for production environments. This is where AI integrations cost usually increases because the platform must support ongoing model refinement instead of static validation workflows.
Estimated Cost Impact: $10,000 – $50,000
Healthcare organizations rarely use one isolated billing system. Most platforms need secure connections with EHRs, clearinghouses, eligibility providers, payer systems, and reporting tools.
Each integration requires separate workflow mapping, testing, authentication handling, and error management. Organizations needing broader interoperability often require additional AI integration services to manage those external system dependencies correctly.
Also Read: How Much Does It Cost to Develop an AI EHR Software?
Estimated Cost Impact: $8,000 – $35,000
Basic reporting dashboards usually focus on clean claim rates and rejection visibility. Costs increase when leadership teams need payer-level analytics, operational tracking, denial trend reporting, and department-specific reporting views.
Complex dashboards also require stronger backend processing because the platform must organize large billing datasets into readable operational reports continuously.
Estimated Cost Impact: $12,000 – $45,000
Different specialties follow different billing requirements. Oncology, behavioral health, radiology, outpatient billing, and DME workflows all require separate validation conditions and payer review logic.
Development effort increases because teams must configure and test each specialty workflow independently. The review logic also becomes harder to maintain as payer variations expand across specialties.
Estimated Cost Impact: $10,000 – $40,000
Healthcare claim scrubbers process protected health information continuously. That means the platform must support HIPAA compliance, encryption controls, access restrictions, audit logging, monitoring systems, and secure infrastructure environments.
Costs rise further when organizations require penetration testing, cloud governance controls, disaster recovery planning, and external compliance reviews before production launch.
Also Read: Cost to Develop HIPAA-Compliant AI Healthcare Software
Estimated Cost Impact: $15,000 – $70,000
Some organizations only automate claim validation workflows initially. Others automate denial prediction, routing workflows, claim prioritization, payer rule updates, and operational alerts together.
Broader automation increases development effort because the system must coordinate more workflow conditions across different operational layers. Healthcare organizations implementing large-scale automation usually require extended AI automation services throughout deployment and expansion stages.
|
Hidden Costs |
Where Cost Goes |
Estimated Cost Impact |
|---|---|---|
|
Historical data preparation |
Cleaning and organizing claim records before AI training |
$5,000 – $25,000 |
|
Third-party API fees |
Eligibility systems, payer APIs, clearinghouse usage |
$3,000 – $20,000 annually |
|
Cloud infrastructure scaling |
Storage, monitoring, AI processing workloads |
$5,000 – $40,000 annually |
|
AI model retraining |
Updating validation models using new claim outcomes |
$8,000 – $30,000 annually |
|
Security audits |
Compliance reviews and penetration testing |
$7,000 – $35,000 |
|
Specialty workflow customization |
Additional payer logic and validation conditions |
$10,000 – $50,000 |
Estimated Savings: 20% – 35%
Organizations can reduce early development cost by prioritizing essential validation workflows first. Many healthcare teams use structured MVP software development planning to validate operational performance before expanding broader automation requirements.
Estimated Savings: 10% – 25%
Connecting every external system during the first release usually increases implementation timelines and testing effort significantly. Many organizations reduce early spending by integrating only the most critical payer, EHR, and clearinghouse workflows first.
Estimated Savings: 8% – 20%
Existing authentication systems, reporting environments, and billing tools can often remain operational during implementation. Reusing available infrastructure helps reduce redevelopment effort across multiple operational layers.
Estimated Savings: 15% – 30%
Organizations often control costs more effectively by automating one operational workflow at a time. Claim validation workflows usually launch first before expanding into denial prediction, automated routing, and advanced operational automation layers later.
Well-planned AI claim scrubber software development budgets help healthcare organizations align automation goals with operational priorities while avoiding unnecessary expansion costs during future scaling stages.
Also Read: How Much Does AI Software Development Cost?
Healthcare organizations planning to develop AI claim scrubbing system workflows often underestimate how much operational complexity exists behind payer validation, healthcare integrations, and AI-driven claim review logic. Many of these challenges appear during real implementation stages, especially when the platform must support large claim volumes across different healthcare environments.
The table below highlights some of the most common development challenges and practical ways to address them.
|
Challenge |
How to Solve Them |
|---|---|
|
Poor historical claim data quality |
Clean and normalize historical billing data before AI training begins. Remove duplicate records and incomplete claim information during data preparation workflows. |
|
Constant payer rule changes |
Maintain centralized payer rule management workflows with scheduled validation updates and ongoing rule monitoring processes. |
|
Inconsistent coding patterns across specialties |
Configure specialty-specific validation workflows separately instead of applying one generalized review model across all specialties. |
|
High false-positive claim alerts |
Train AI models using larger claim datasets and continuously refine validation thresholds using real operational feedback. |
|
Integration difficulties with EHRs and clearinghouses |
Use standardized healthcare interoperability frameworks and secure API structures during integration planning stages. |
|
Slow system performance during high claim volume periods |
Use scalable infrastructure environments capable of processing large validation workloads without slowing review workflows. |
|
Limited visibility into AI decision logic |
Maintain transparent validation explanations inside review workflows, so operational teams can understand why claims are flagged. |
|
User resistance during workflow transition |
Introduce automation gradually and train operational teams before expanding larger workflow changes across departments. |
|
Security and compliance risks |
Implement encryption controls, access restrictions, audit logging, and continuous infrastructure monitoring across the platform. |
|
Difficulty scaling automation workflows later |
Hire AI developers to design modular workflows early, so new payer rules, specialties, and automation layers can expand without major redevelopment. |
|
Shortage of healthcare AI engineering expertise |
Healthcare organizations should work with an experienced AI development company familiar with healthcare billing operations and AI validation systems. |
|
Balancing automation with operational oversight |
Keep human review checkpoints active for higher risk claims instead of fully automating every validation decision immediately while building AI software for healthcare workflows. |
Also Read: Cost to Hire an AI Software Developer in 2026
Strong planning, structured validation workflows, and operationally realistic AI claim scrubber software development strategies help healthcare organizations reduce implementation risks while supporting long-term scalability across evolving payer environments.
The right execution strategy prevents costly workflow breakdowns during healthcare AI implementation
Solve Our Implementation BottlenecksMany healthcare organizations reach a point where internal billing teams can no longer manage growing payer complexity, denial pressure, and automation requirements alone.
If you’re someone asking “I need a reliable US based development partner that can build our AI claim scrubber software from scratch. This includes machine learning error detection engine, the payer specific rules database, the EHR integration layer, and the real time analytics dashboard for our revenue cycle management team?”
Then Biz4Group LLC might be the answer you’re looking. We become a strong execution partner for healthcare organizations planning AI claim scrubber software development. As a HIPAA compliant AI healthcare software development company, we bring practical experience across healthcare automation, AI-driven operational systems, payer workflow integrations, and enterprise AI solutions.
We also understand how healthcare organizations manage operational pressure across revenue cycle environments where accuracy, compliance, and scalability must work together continuously.
Here what we bring to the table:
We work closely with healthcare and insurance-focused operational environments where payer validation logic and claim review accuracy directly affect reimbursement performance. This experience helps our team align technical implementation with real operational billing requirements instead of generic automation execution.
We have experience delivering AI insurance automation software solutions tied to workflow automation, operational intelligence, and healthcare process optimization. That practical implementation background helps healthcare organizations move beyond surface-level automation planning into scalable operational systems. Not convinced, well here’s the proof:
It is an advanced AI chatbot developed to support insurance leaders and agent teams with faster access to policy guidance, training support, and operational assistance through conversational AI workflows. The platform focused on improving training efficiency while making insurance knowledge more accessible across distributed teams.
Key capabilities included:
This AI-driven IVR and support platform is designed for healthcare third-party administrators handling large volumes of patient and insurance-related inquiries. The system automated routine call handling, supported bilingual interactions, and improved response routing through intelligent voice workflows.
Key capabilities included:
AI claim scrubber platforms require much more than isolated claim review logic. We can support payer rule systems, analytics dashboards, healthcare integrations, AI workflow automation layers, and AI validation engines within one structured ecosystem instead of fragmented development workflows.
Healthcare organizations handling protected health information require stronger governance controls across every operational layer. We approach healthcare platform engineering with close attention to HIPAA safeguards, access management, infrastructure security, auditability, and operational reliability throughout development lifecycles.
Revenue cycle automation rarely exists in isolation inside healthcare operations. Organizations modernizing claim review systems often expand into connected automation workflows later.
Our broader healthcare AI experience, including workflow-driven systems like AI prior authorization software, helps support long-term scalability planning across operational environments. Our company’s AI portfolio also reflects experience across multiple enterprise AI implementation scenarios.
Healthcare organizations looking for the best company in USA to develop AI claim scrubber software often prioritize execution reliability, healthcare domain understanding, and scalable AI implementation experience together. Biz4Group LLC brings those capabilities into one operationally focused development partnership.
Schedule a strategy call with us.
AI claim scrubber software development is becoming an important operational priority for healthcare organizations dealing with rising claim complexity, recurring submission errors, and growing payer scrutiny. Manual correction workflows and static validation systems continue creating delays that directly affect reimbursement cycles and administrative efficiency.
AI-driven claim scrubbing helps healthcare organizations strengthen claim validation through payer-specific review logic, automated claim analysis, denial pattern tracking, and scalable workflow automation. Long-term success also depends on practical implementation planning, secure healthcare infrastructure, and workflows that can adapt as payer requirements continue changing.
For organizations planning AI revenue cycle claim scrubber development, the real value comes from aligning automation with everyday billing operations instead of adding disconnected systems into existing workflows. That is where Biz4group LLC supports healthcare organizations with structured AI product development services focused on scalable healthcare automation systems. Ready to modernize your claim review workflows? Talk to us today!
Modern AI claim scrubber software can identify recurring payer-specific submission risks with significantly higher consistency than static rule-based workflows when trained on clean historical claim data. Accuracy usually improves over time because the system continuously reviews denial trends, coding behavior, and payer response patterns across live billing environments.
Yes. AI claim scrubber software development for healthcare often supports multi-specialty environments where billing workflows differ across departments like radiology, oncology, behavioral health, outpatient services, and DME processing. The system can apply separate validation logic, modifier checks, and payer conditions based on specialty-specific billing requirements.
The timeline usually depends on platform scope, integration complexity, and automation requirements. MVP-level systems generally take around 2–4 weeks, while mid-level and enterprise-scale platforms may require 6–12+ weeks. Timelines increase further when organizations need large-scale payer integrations, analytics dashboards, and advanced denial prediction workflows.
Enterprise-grade AI medical claim scrubber software development typically ranges between $150,000 and $300,000+ depending on AI complexity, specialty workflow support, reporting requirements, payer integrations, and compliance infrastructure. Smaller MVP implementations usually begin around $40,000–$80,000 before broader automation expansion begins.
Yes. Most intelligent claim scrubber platform development projects are designed to work alongside existing EHRs, clearinghouses, payer systems, and billing platforms through secure APIs and interoperability standards. This allows organizations to modernize claim validation workflows without rebuilding their entire revenue cycle infrastructure.
Healthcare organizations should evaluate practical healthcare domain expertise, payer workflow understanding, HIPAA compliance capabilities, AI implementation experience, scalability planning, and integration expertise before selecting a development partner. Teams should also review whether the company has experience handling operational healthcare automation environments instead of only generic AI projects.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.