Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

“What happens when a denial management team spends more time tracking denied claims than actually recovering reimbursement?” That question is becoming increasingly common across hospitals, multi-specialty physician groups, and revenue cycle teams struggling with rising denial volume across multiple insurance payers.
The numbers confirm what healthcare providers are already experiencing. In 2022, 30% of providers reported that at least 10% of their claims were denied. By 2024, it reached 38% and 41% in 2025. Not only this, adjudicating those claims can cost the healthcare industry a whopping $25.7 billion annually. How can this be solved?
Even businesses are puzzled and asking, “we are a large multi-specialty physician group that receives over 1500 denials monthly across 12 different insurance payers and our denial management team spends 80 percent of their time on administrative tracking tasks rather than working on appeals. So, we need an AI system that automates all the tracking and administrative work so our team can focus exclusively on building strong appeal arguments?”
Well, AI claims denial navigator software is the answer to your question.
This blog will take you through the full lifecycle of AI claims denial navigator software development from what it is to how it helps businesses in revenue generation and management. We’ll also suggest a reliable AI development company in America that can build your custom claims denial navigator software from scratch with machine learning, denial classification, automated appeal generation, and payer portal integration.
Healthcare denial volumes have increased significantly as payer rules, authorization requirements, coding standards, and reimbursement policies continue becoming more complex. Many healthcare organizations still rely on spreadsheets, disconnected billing systems, manual tracking workflows, and fragmented denial review processes that were never designed to handle modern denial workloads efficiently.
In many large healthcare organizations, clinical denials now represent a major share of total denial volume. Some academic medical centers report clinical denials reaching nearly 42% of all denied claims, where reimbursement recovery depends heavily on physician peer-to-peer review participation.
When physicians cannot prioritize denial reviews alongside patient care responsibilities, appeal deadlines begin expiring faster, and unresolved denial backlogs continue increasing.
Here’s why the traditional claims denial management fails at broader level:
Modern healthcare denial management requires more than manual tracking and fragmented workflows. Healthcare organizations now need operational systems that can organize denial activity and provide better visibility across the reimbursement recovery process, bringing AI claims denial navigator software into the picture.
What Is AI Claims Denial Navigator Software?
AI claims denial navigator software is a system that helps hospitals and healthcare providers manage insurance claims that were not paid by the insurance company. When an insurance company refuses to pay a claim, the claim becomes a denied claim. The reason could be:
The AI claims denial navigator software helps the healthcare team understand:
Instead of managing denied medical claims through spreadsheets, emails, payer portals, and manual tracking, the system keeps everything in one place. The platform usually helps teams:
The AI helps teams make faster and better decisions. It identifies denial patterns, highlights high-priority claims, estimates appeal success probability, and helps staff focus on claims with better recovery potential. In simple terms, AI claims denial navigator software helps healthcare providers track, manage, correct, appeal, and recover denied insurance claims in a more organized and efficient way.
Also Read: AI Medical Claim Processing Software Development Guide
Now before we dive deep into how the system works, let’s first make ourselves acquainted with the claim denial lifecycle and the claims that must be handled.
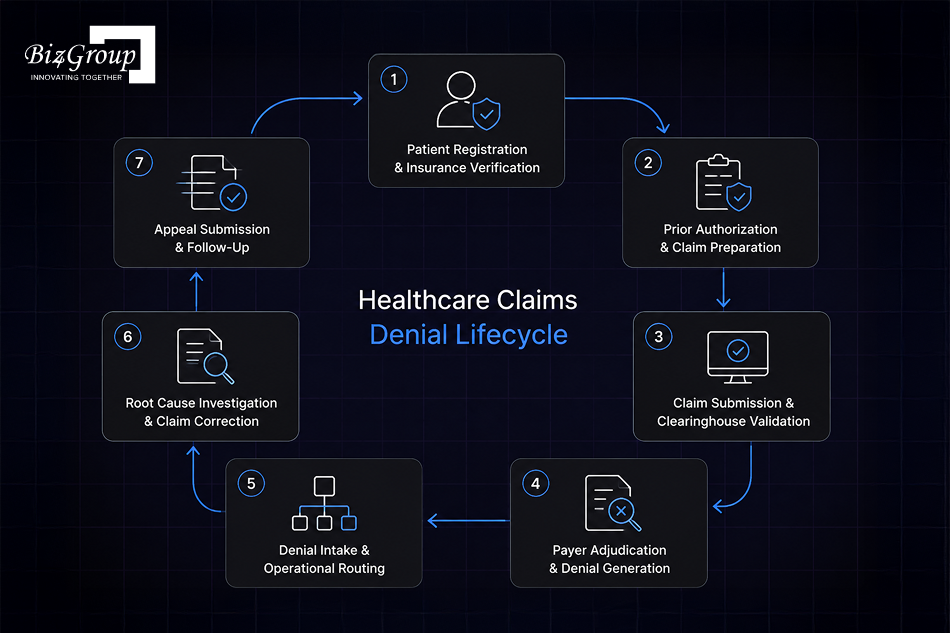
A healthcare claims denial lifecycle does not start when the insurance company refuses payment. The lifecycle actually begins much earlier during patient registration, insurance verification, and claim preparation. Problems during any of the lifecycle stages can push the claim into denial workflows later.
The AI claims denial navigator software mainly becomes operational after payer review begins, but the lifecycle it manages starts long before the denial itself happens.
The lifecycle starts when healthcare staff collect patient insurance information and verify whether the payer coverage is active and accurate. Registration teams review policy details, member information, and coordination of benefits records before treatment or billing begins.
Errors during this stage often create eligibility-related denials later in the process.
Also Read: AI Claim Scrubber Software Development
For many procedures and specialty treatments, providers must complete prior authorization checks before services are delivered. After treatment, coding and billing teams prepare the claim using diagnosis codes, procedure codes, modifiers, and clinical documentation required for payer submission.
Missing authorization records or coding inconsistencies frequently become the reason claims move into denial workflows later.
Also Read: How to Develop AI Prior Authorization Software for Mid-Size Clinics
Once the claim is ready, the provider submits it through the billing platform or clearinghouse. Before the payer reviews the claim, the clearinghouse validates whether the submission meets technical and billing requirements.
Claims with formatting problems, missing details, or coding issues are usually rejected during this stage and must be corrected before resubmission.
After the payer accepts the claim, adjudication begins. The insurance company reviews authorization status, medical necessity, coverage rules, documentation quality, and coding accuracy before deciding whether reimbursement should proceed.
Some claims are approved immediately, while others move into denial workflows because the payer identifies operational, billing, or clinical issues.
This is the stage where the AI claims denial navigator software becomes the primary operational system for denial management. The platform receives denial responses through ERA files, payer portals, or clearinghouse systems.
It then organizes claims based on denial type, payer category, urgency, financial priority, and operational ownership so the correct team can begin review.
Once the denial enters review, teams investigate why the claim failed payer approval. Staff review claim history, authorization records, coding activity, payer requirements, and supporting documentation before deciding the next action. Some claims only require correction and resubmission, while others move into formal appeal handling.
Claims that cannot be resolved through correction enter the appeal process. Teams prepare supporting documentation, organize payer-specific records, and submit appeals for reconsideration. Many claims continue moving through repeated payer follow-ups, escalation reviews, additional documentation requests, or secondary appeals before the organization reaches a final decision.
The lifecycle ends when the payer either overturns the denial, partially reimburses the claim, or permanently maintains the denial decision. After resolution, organizations review recurring denial patterns and move those findings back to registration, authorization, coding, billing, and documentation teams and a long manual process continues again.
Disconnected workflows keep claims moving in circles while reimbursement timelines continue slipping further
Fix The Workflow Bottleneck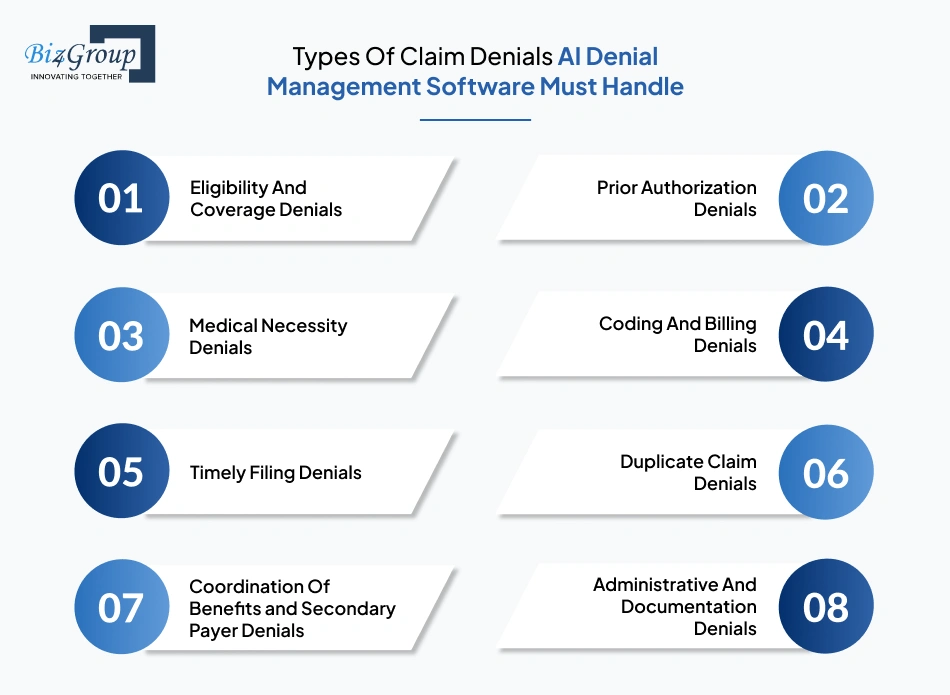
Denied claims do not follow one fixed operational pattern. Some are caused by missing authorizations, some by coding gaps, while others originate from payer filing rules or eligibility mismatches.
An AI denial management platform must recognize the operational difference between denial categories before routing the claim into review, correction, or appeal workflows.
These denials appear when patient insurance details are inactive, incorrect, expired, or mismatched with payer records at the time of billing. They are common in high-volume intake environments where coverage verification workflows move too quickly, or insurance updates are missed during registration.
Most organizations see these denials linked to:
These claims usually require insurance verification and payer validation before resubmission can happen.
Authorization denials happen when approval requirements are missing, expired, incomplete, or submitted under the wrong payer criteria. These denials are common in specialty-driven departments such as radiology, oncology, cardiology, and surgical care.
Operationally, denial teams often need to verify:
The workflow becomes more complicated when commercial payers and Medicare Advantage plans follow different approval rules for the same treatment category.
Medical necessity denials happen when the payer questions whether the treatment, admission, or procedure met clinical justification requirements. CO-50 denials commonly fall into this category and usually require extensive documentation review.
These denials often involve:
Many organizations also route these denials into peer-to-peer review workflows before formal appeal submission.
Coding denials occur when CPT, HCPCS, ICD, or modifier usage does not align with payer billing requirements. Billing denials may also happen when claim details are incomplete or submitted incorrectly.
These denials commonly involve:
Even small coding inconsistencies can create large denial backlogs when claim volume increases across multiple departments.
Also Read: AI Medical Coding Software Development
Timely filing denials happen when claims or appeals are submitted after the payer’s allowed submission window. Different payers use different filing deadlines, which creates operational risk for teams managing large denial queues simultaneously.
These denials usually happen when:
Once the filing window closes, recovery options become much harder to reopen.
Duplicate denials happen when the payer receives multiple submissions tied to the same service encounter. In many cases, this occurs because operational teams resubmit claims before earlier claim status updates become visible inside billing workflows.
These denials commonly appear during:
Without clear claim tracking visibility, duplicate denials can expand quickly in high-volume environments.
These denials happen when payer responsibility is unclear or incorrectly assigned between primary and secondary insurance plans. Staff often spend significant time verifying payer order before the claim can move back into processing.
This denial category becomes more complicated when:
These claims usually require payer coordination workflows instead of clinical correction.
Administrative denials happen when required forms, signatures, attachments, or supporting records are missing from the claim submission process. The claim itself may still be valid clinically, but incomplete documentation stops the payer from processing it properly.
Common causes include:
The denials increase manual follow-up work because staff must collect and resubmit operational documents before the claim can proceed further. Now,
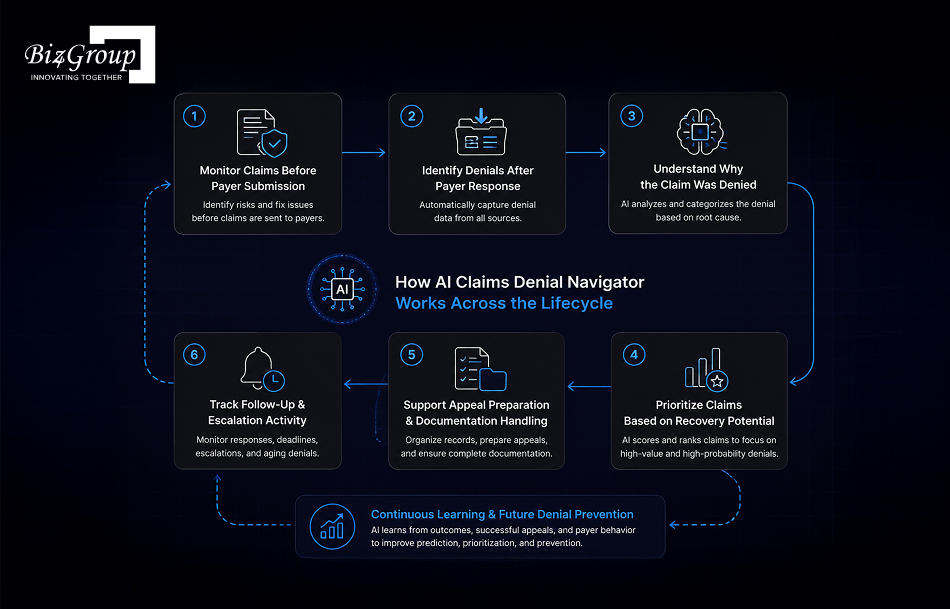
AI claims denial navigator software works across the denial lifecycle instead of becoming active only after a claim gets denied. It helps healthcare organizations manage the entire process through one connected workflow instead of relying on spreadsheets, disconnected billing systems, emails, and manual payer tracking.
The workflow begins before the claim reaches the insurance company. The platform reviews claim details, authorization records, coding activity, documentation quality, and historical payer behavior to identify claims likely to face denial during adjudication.
At this stage, the system can identify:
This improves denial prediction because operational teams can correct high-risk claims before the payer review process begins.
Once the payer reviews the claim, denial responses enter the platform through ERA files, payer portals, clearinghouses, or billing systems. The software automatically captures denial information and organizes it inside one operational workflow.
The platform reviews:
This removes the need for denial teams to manually collect denial information from multiple systems.
After intake, trained AI models analyze the denied claim to determine what operational issue caused payment failure. Instead of forcing teams to manually review every claim, the software categorizes the denial automatically based on payer rules, claim history, authorization status, coding activity, and supporting documentation.
The system can identify:
This improves denial routing because claims move directly into the correct operational workflow after categorization.
Not every denied claim carries the same financial value or appeal probability. The AI reviews historical payer outcomes, reimbursement patterns, filing urgency, claim value, and denial trends to determine which claims should receive immediate attention.
The platform helps operational teams prioritize:
This improves prioritization by helping staff focus effort where recovery potential is higher instead of treating every denial equally.
Once the claim moves into appeal workflows, the software organizes supporting records and coordinates documentation required for reconsideration. The platform retrieves clinical records, authorization history, denial communication, and billing information directly inside the workflow.
The system supports:
This improves appeal automation because operational teams spend less time manually collecting records and managing appeal documentation.
Claims often remain active long after appeal submission. The platform therefore continues monitoring payer responses, filing deadlines, escalation timelines, and unresolved denial aging throughout the reimbursement process.
The software tracks:
This helps organizations maintain operational visibility across large denial workloads and reduces the risk of missed follow-up activity.
As more claims move through the platform, the AI continuously learns from payer decisions, successful appeals, reimbursement outcomes, and recurring operational problems. The system then uses that historical activity to improve future denial prediction, prioritization accuracy, and appeal recommendations.
Over time, this helps healthcare organizations reduce repeated denial patterns and improve broader revenue cycle operations through more informed workflow decisions.
AI-driven denial workflows help teams focus faster on appeals carrying stronger reimbursement recovery potential
Prioritize Smarter Claims FasterHealthcare providers rarely deal with one insurance payer or one fixed reimbursement workflow. Every payer follows different review standards, denial patterns, documentation requirements, and appeal processes.
That is why AI denial management software must understand payer-specific behavior instead of applying one generalized denial workflow across every claim.
Insurance payers do not operate under one standardized denial process. Every payer follows different authorization requirements, coding expectations, documentation rules, appeal timelines, and reimbursement policies. A denial workflow that works successfully for one payer may completely fail for another.
Differences usually appear in areas such as:
Because of this variation, healthcare organizations cannot rely on one generalized denial handling workflow across every payer.
Different payers generate different denial trends. Some insurance providers create higher denial volume around prior authorization, while others focus more heavily on coding accuracy, medical necessity validation, or eligibility review.
Operational teams often experience recurring issues such as:
These differences increase operational complexity when denial teams manage multiple payer contracts simultaneously.
Payer behavior also changes how appeals should be prepared and managed. Some payers require extensive clinical documentation before reconsideration begins, while others respond more effectively to corrected claims or peer-to-peer review workflows.
Variations often appear in:
Without payer-specific workflow alignment, appeal handling becomes slower and less consistent.
Payer-specific intelligence allows the healthcare denial management automation software to continuously learn from historical denial activity, reimbursement outcomes, appeal success rates, and payer response behavior. Instead of treating every denial equally, the platform understands how different payers behave operationally across the denial lifecycle.
The AI claim denial tracking system can identify:
This improves how denial teams prioritize and manage claims across different payer environments.
Therefore, payer intelligence helps maintain operational consistency.
As commercial payers, Medicare Advantage organizations, and managed care networks continue changing reimbursement policies, denial management workflows become harder to manage manually. Payer-specific intelligence helps healthcare organizations maintain more consistent denial handling processes without constantly adjusting workflows reactively. That operational visibility becomes increasingly important as healthcare providers manage larger denial volumes across complex payer ecosystems.
|
Aspect |
Traditional Denial Management Software |
AI Claims Denial Navigator Software |
|---|---|---|
|
Denial Intake |
Relies heavily on manual claim collection and review |
Automatically captures denial data from connected systems |
|
Denial Categorization |
Staff manually classify denial types |
AI categorizes denials automatically using claim and payer data |
|
Claim Prioritization |
Most claims receive similar operational attention |
AI prioritizes claims based on recovery potential and urgency |
|
Denial Prediction |
Works after denials occur |
Identifies high-risk claims before payer submission |
|
Appeal Preparation |
Manual document collection and appeal handling |
Organizes documentation and supports appeal workflow automation |
|
Root Cause Identification |
Limited visibility into recurring denial patterns |
Detects operational issues across workflows and payer activity |
|
Follow-Up Tracking |
Often managed through spreadsheets and emails |
Tracks deadlines, escalations, and payer responses centrally |
|
Payer Intelligence |
Minimal adaptation to changing payer behavior |
Continuously analyzes payer-specific denial trends |
|
Workflow Visibility |
Fragmented operational tracking across systems |
Centralized visibility across denial lifecycle stages |
|
Scalability |
Operational pressure increases with denial volume |
Supports high-volume denial management more efficiently |
|
Denial Aging Management |
Delayed follow-up often increases claim aging |
Real-time tracking improves denial aging visibility |
|
Documentation Coordination |
Staff retrieve records manually from multiple systems |
Connected workflows centralize denial-related documentation |
|
Reporting Capabilities |
Limited operational analytics and recovery visibility |
Tracks denial trends, appeal outcomes, and reimbursement activity |
|
Learning Capability |
Static workflows with limited adaptation |
AI improves recommendations using historical denial outcomes |
|
Revenue Recovery Efficiency |
Slower resolution cycles reduce recovery speed |
Faster prioritization and appeals improve reimbursement recovery |
Building an AI claims denial navigator tool that recovers maximum denied revenue by accurately predicting appeal success probability before investing staff time requires features that support different operational responsibilities across the denial lifecycle.
The platform structure should therefore stay practical, organized, and aligned with how denial workflows move inside healthcare environments. Let’s dive deep in to feature stack:
These features control how denied claims enter the platform and move through operational queues.
|
Feature |
Purpose |
|---|---|
|
Centralized denial intake queue |
Collects denied claims from clearinghouses, payer files, and billing systems into one workflow. |
|
Denial categorization module |
Separates denials based on type, payer, urgency, and operational handling requirements. |
|
Work queue assignment system |
Routes denial cases to the correct operational teams automatically. |
|
Filing deadline tracker |
Monitors payer appeal windows and submission timelines. |
|
Escalation management workflow |
Pushes high-priority or delayed denials into escalation review queues. |
These modules help denial teams decide where operational effort should be focused first.
|
Feature |
Purpose |
|---|---|
|
Recoverability scoring engine |
Estimates the likelihood of successful denial recovery before appeal work begins. |
|
High-risk claim prediction module |
Flags claims likely to face denial before payer submission. |
|
Financial impact prioritization |
Ranks denials based on potential revenue exposure and claim value. |
|
Payer trend monitoring |
Tracks recurring denial behavior across different payer groups. |
|
Repeat denial detection |
Identifies claims repeatedly denied for the same operational reason. |
These features organize the operational work required for denial correction and appeal submission.
|
Feature |
Purpose |
|---|---|
|
Appeal drafting module |
Generates structured appeal drafts using denial and claim details. |
|
Clinical document retrieval system |
Pulls supporting medical records into the denial workflow. |
|
Supporting file management |
Organizes attachments, referral records, and payer-required documents centrally. |
|
OCR-based denial document reader |
Converts scanned denial notices into searchable workflow records. |
|
Peer-to-peer review coordination |
Tracks physician review requests and related follow-up activity. |
These modules provide visibility into denial activity and operational movement across the organization.
|
Feature |
Purpose |
|---|---|
|
Denial operations dashboard |
Displays active denial volume, queue status, and payer distribution. |
|
Denial aging monitor |
Tracks claims remaining unresolved for extended periods. |
|
Appeal outcome reporting |
Records overturn decisions, payer responses, and appeal status history. |
|
Operational workload tracker |
Monitors denial distribution across teams and departments. |
|
Exportable reporting module |
Supports operational reviews, audits, and finance reporting workflows. |
These features support platform governance, operational control, and connected healthcare workflows.
|
Feature |
Purpose |
|---|---|
|
Role-based access controls |
Restricts system access based on operational responsibility. |
|
Audit trail logging |
Maintains records of workflow actions, edits, and claim activity history. |
|
Multi-payer configuration manager |
Supports payer-specific workflow settings and operational rules. |
|
Notification and alert engine |
Sends reminders for deadlines, escalations, and workflow updates. |
|
EHR and billing connectivity support |
Maintains synchronized claim and patient data across connected systems. |
Also Read: How to Build an AI Medical Billing Software
Strong feature planning keeps denial workflows structured without overloading teams with disconnected tools or repetitive operational steps. That balance matters because AI claims denial navigator software development should support practical denial recovery operations through clearly separated platform capabilities instead of overlapping automation layers.
Operational visibility weakens quickly when denial workflows depend on fragmented systems and manual coordination
Map The Right Feature StackDenied workflows already move across billing systems, clearinghouses, payer portals, and clinical records before an appeal even begins. A disconnected setup creates delays because denial teams keep switching between platforms to verify claim status, collect documents, and review payer responses.
That is why AI claims denial navigator software development depends heavily on integrations that keep operational data connected across the healthcare environment.
The denial platform should connect with the organization’s EHR software, so denial teams can access physician notes, treatment history, discharge summaries, and supporting records directly from the workflow. Without this connection, staff often waste time collecting documents manually before appeals move forward.
Clearinghouse integration allows the platform to receive X12 835 ERA files, denial responses, and payer acknowledgments automatically. This keeps denial queues updated in real time instead of relying on spreadsheet tracking or manual uploads from billing teams.
The denial system should stay connected with revenue cycle management platforms, so claim status updates remain aligned across billing and denial operations. This prevents mismatched records during resubmissions, payment updates, and write-off reviews.
Many payer notices still arrive through scanned letters, PDFs, or uploaded files. An OCR system helps convert those documents into searchable records, so denial data can move into the platform without manual entry from staff.
Also Read: AI Document Analysis Tool Development: A Complete Guide
The platform should connect directly with payer portals and APIs to retrieve claim updates, upload appeal documents, and track payer communication history from one centralized workflow. This becomes especially important for organizations handling denials across multiple commercial and Medicare Advantage plans.
Denial platforms should also connect with reporting systems already used by finance and administrative teams. This keeps denial records, payer activity, and operational reporting synchronized across departments instead of creating isolated data environments.
Connected integrations help denial operations stay organized across clinical systems, payer communication, and billing workflows. That structure becomes essential when creating an AI denial management system that has to support large denial volumes without disconnecting operational teams from the systems they already use.

In AI claims denial navigator software development for healthcare, the real work starts long before a model writes an appeal. The team has to understand denial volume, payer behavior, staff workflow, and the systems already in place.
Here’s how context shapes every step that follows:
Start with the real denial path inside the organization. That means tracing what happens from ERA intake to appeal submission, deadline tracking, write-off review, and prevention feedback. Do this with the people who live in the queue every day. Their process is the product boundary.
This is the point where the software scope becomes real. You are not designing for a generic hospital rather for one payer mix, one denial pattern, and one operational team with limited time.
Do not try to solve every denial on day one. A strong MVP should prove one narrow recovery path end to end. That could be medical necessity denials for one payer group or timely filing denials that keep slipping past the deadline.
This is where MVP development services become useful in a practical way. The goal is not a polished full platform. The goal is a working version that shows the organization how faster recovery will feel in daily use.
Also Read: Top MVP Development Companies in USA
The screen should match how denial teams actually think. They need to see the denial reason, the payer rule, the next action, and the supporting record without hunting through tabs. A good UI/UX design company will keep the layout simple, and task driven.
The interface should reduce fatigue, not add another system to manage. If the work takes place in a denial queue, the design should feel like a queue. If a user needs to decide in under a minute, the screen should help them do that cleanly.
Also Read: Top UI/UX Design Companies in USA
This is where AI model development starts to matter. The model should learn from the organization’s own denial history, not just generic healthcare examples. It needs to see how claims were denied, what was appealed, what was overturned, and what was written off.
The point is to make the system useful inside that specific revenue cycle environment. The team should also define how the model will improve over time. That keeps the first release grounded and makes later updates easier to trust.
Also Read: Top 10+ AI Model Development Companies in USA
The software cannot live in isolation. It must move data from the EHR, the billing system, the clearinghouse, and payer files without creating more manual work. This is where API connectivity becomes a real requirement rather than technical detail.
The team also needs to integrate AI models in a way that fits the workflow. The model should support the denial worker, not interrupt them. Data should flow in both directions so the system can read claim status and send back updated appeal actions.
Also Read: How to Select the Best AI Model for Your Use Case?
Before anyone calls the software ready, it must go through structured testing. Many teams bring in software testing companies at this stage because the platform has to prove both accuracy and usability under real denial conditions.
The testing should cover the full path a user will follow. That means checking whether the denial is classified correctly, whether the right appeal content appears, whether deadlines calculate properly, and whether status updates stay accurate after every action.
Also Read: Top AI Software Development Companies in USA
A pilot gives the organization a safe way to see how the software behaves inside daily work. Pick one denial team, one payer group, or one service line. Keep the rollout narrow enough that support stays close, and feedback stays useful.
This is the stage where the system either earns trust or exposes weak spots. The team should watch user adoption, speed of work, error patterns, and appeal handling. If the pilot is stable, launch becomes a business decision instead of a gamble.
The launch should not end the project. It should begin the performance cycle. Once the platform is live, the team needs to watch overturn rates, appeal turnaround, deadline protection, and denial patterns that keep repeating.
This is also the right time to compare the first real results against the original business case. The system should improve in small but visible ways. That may mean better appeal routing, cleaner documentation, or stronger denial prevention feedback to upstream teams.
That is the practical path for AI claims denial navigator software development. Keep the first build narrow, make the workflow clear, test it against real denials, and launch only when the team can trust it in daily revenue cycle work.
Clear development planning keeps denial workflows scalable across payer complexity operational growth and future automation needs
Plan The Platform CorrectlyA reliable technology stack matters because denial management teams work across multiple systems every day. The platform must process payer responses, review clinical records, route appeals, and surface analytics without slowing staff down.
That is why custom claims denial navigator software development should focus on stability, interoperability, and usability from the beginning.
|
Architecture layer |
Recommended tools/technologies |
Purpose |
|---|---|---|
|
User interface layer |
Next.js, React, TypeScript, React Native |
Gives denial teams a clean web and mobile experience for queues, claim details, and appeal workflows. |
|
Design system layer |
Tailwind CSS, shadcn/ui, Storybook |
Keeps screens consistent and reduces confusion during daily denial handling. |
|
Access control layer |
OAuth 2.0, SSO, Active Directory, Okta |
Controls user access and protects sensitive claim information across departments. |
|
Workflow orchestration layer |
Routes denial tasks through escalation, review, approval, and follow-up stages automatically. |
|
|
AI decision layer |
Python, PyTorch, TensorFlow, scikit-learn |
Supports denial prediction, prioritization, appeal recommendations, and recovery scoring. |
|
Document intelligence layer |
OCR tools, spaCy, Apache Tika, NLP services |
Extracts useful details from denial letters, physician notes, and supporting records. |
|
Rules and policy layer |
Decision tables, JSON or YAML policy files, business rule engines |
Manages payer rules, filing deadlines, and denial-specific workflow logic. |
|
Integration layer |
FHIR, HL7, X12 835, X12 277CA, REST APIs, Mirth Connect |
Connects the platform with EHRs, clearinghouses, billing systems, and payer portals. |
|
Data storage layer |
PostgreSQL, MongoDB, Elasticsearch, S3-compatible storage |
Stores claims data, appeal records, searchable documents, and denial history. |
|
Analytics and reporting layer |
Apache Superset, Metabase, Power BI, dbt |
Tracks overturn rates, denial trends, payer performance, and operational bottlenecks. |
|
Security and audit layer |
AES encryption, SIEM tools, audit logging, key management systems |
Protects PHI and maintains detailed activity records for compliance reviews. |
|
Deployment and monitoring layer |
Docker, Kubernetes, CI/CD pipelines, Prometheus, Grafana |
Supports stable releases, system monitoring, and controlled production updates. |
The right stack keeps denial operations practical instead of overly technical. Every layer should support faster appeals, cleaner workflows, secure data handling, and easier reporting. That approach makes claims denial navigator software development integrating AI more sustainable for provider organizations while keeping full stack development aligned with real revenue cycle operations.
Also Read: Why to Choose the Full Stack Development for Modern Business
Denied claims systems handle protected health information at every stage of the workflow. Staff review patient records, payer responses, clinical notes, appeal letters, and financial details inside the same environment. That makes compliance planning a core part of the architecture, not a late-stage checklist.
An intelligent claims denial management platform development strategy should protect data while still allowing denial teams to work quickly across appeals and payer communication workflows.
Also Read: Top 10 AI EHR Software Development Companies in USA
Also Read: HIPAA Compliant AI App Development for Healthcare Providers
Also Read: A Complete Guide to OpenAI API Integration for AI Applications
Strong compliance practices keep denial operations stable while protecting patient information across every workflow stage. That foundation matters because healthcare claims denial navigator AI development depends on secure data handling and responsible AI usage throughout the denial recovery process.
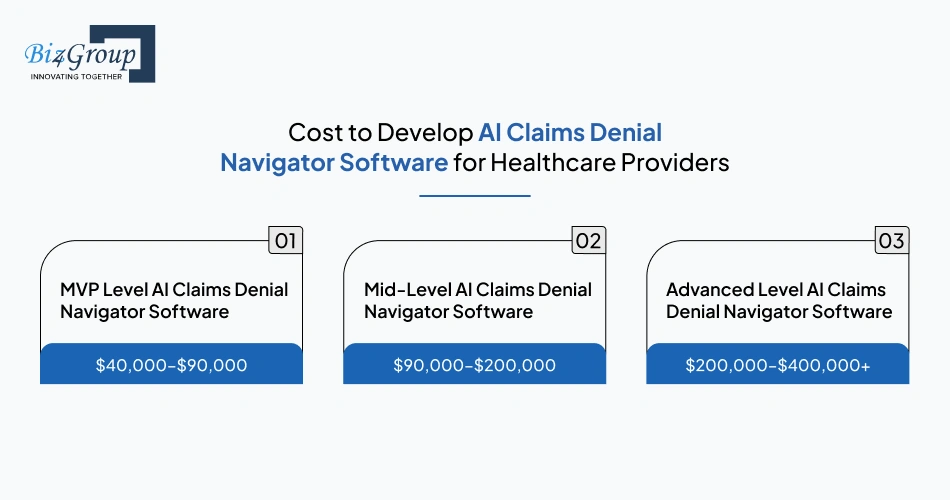
Cost depends on how deeply the platform fits into the provider’s denial workflow. Some organizations only need denial intake, appeal routing, and dashboard reporting. Others need payer-specific intelligence, clinical document extraction, EHR connectivity, and predictive recovery scoring.
That is why AI claims denial navigator software development can range from $40,000 for a focused MVP to more than $400,000 for a large enterprise platform with advanced automation and integrations.
|
Development level |
Estimated cost range |
Scope |
|---|---|---|
|
MVP Level AI Claims Denial Navigator Software |
$40,000–$90,000 |
Covers denial intake, basic work queues, simple reporting, role-based access, and limited payer workflows for pilot deployment. |
|
Mid-Level AI Claims Denial Navigator Software |
$90,000–$200,000 |
Includes AI-powered categorization, appeal workflows, analytics dashboards, clearinghouse connectivity, and multi-user operations. |
|
Advanced Level AI Claims Denial Navigator Software |
$200,000–$400,000+ |
Supports payer-specific intelligence, predictive scoring, EHR integrations, document extraction, compliance automation, and large-scale denial operations. |
Integration work becomes one of the largest budget drivers in healthcare software. Connecting with EHRs, clearinghouses, billing systems, and payer portals requires testing, validation, and secure data exchange. Enterprise AI integrations increase project time because the platform must maintain stable communication across multiple systems and denial workflows.
Some teams only need basic denial classification. Others want predictive scoring, appeal recommendations, document extraction, and payer-specific routing. The cost rises when the platform requires custom training data, historical denial analysis, and ongoing model refinement as part of building AI software for enterprise revenue cycle operations.
Denial workflows differ across hospitals, specialties, and payer contracts. A platform handling Medicare Advantage appeals for cardiology claims will not follow the same logic as outpatient radiology denials. More workflow layers mean more configuration, testing, and operational mapping.
Compliance work adds cost because the platform must support encrypted storage, audit logs, access controls, secure APIs, and PHI protection. Healthcare organizations also require penetration testing, monitoring tools, and compliance documentation before deployment approval.
Also Read: Cost to Develop HIPAA-Compliant AI Healthcare Software
Basic reporting keeps costs controlled. Advanced analytics increase the budget because the system must track overturn rates, denial aging, payer trends, financial recovery patterns, and operational performance across departments. AI integrations cost grows when reporting includes predictive insights and automated recommendations.
Also Read: AI Healthcare Analytics Software Development for Healthcare Organizations
Denial teams work under constant time pressure. The interface must support quick decision-making and easy queue management which adds to UI/UX design cost. Clean workflow design, responsive layouts, and role-based dashboards require additional planning and testing during development.
|
Hidden costs |
Where cost goes |
Estimated cost impact |
|---|---|---|
|
Legacy system cleanup |
Preparing outdated billing or denial data before migration |
$5,000–$25,000+ |
|
Payer workflow revisions |
Updating logic when payer rules or appeal requirements change |
$4,000–$20,000+ annually |
|
Post-launch AI tuning |
Improving denial recommendations after live usage begins |
$8,000–$35,000+ |
|
Compliance reviews |
External audits, security testing, and legal validation |
$6,000–$30,000+ |
|
Staff onboarding support |
Training denial teams and operational administrators |
$3,000–$15,000+ |
|
Cloud infrastructure scaling |
Expanding storage and processing capacity as denial volume grows |
$5,000–$40,000+ annually |
Many providers reduce early investment by limiting the first release to one denial category or one payer workflow. MVP software development helps teams validate operational value before expanding into advanced automation or large-scale integrations.
Start with denial types that create the highest write-offs or workload pressure. That keeps the first release operationally valuable while avoiding unnecessary feature expansion.
Organizations already using secure cloud environments, identity systems, or reporting tools can reduce infrastructure expenses. Existing operational systems often lower integration and deployment effort.
AI automation services help reduce manual work tied to denial routing, documentation collection, and deadline tracking. Early automation also limits staffing pressure as denial volume increases.
Also Read: 10 AI Automation Use Cases for Enterprises to Scale Faster
Large integration projects increase both cost and deployment time. Many providers control spending by connecting only the systems needed for the first release, then adding additional payer or AI EHR integrations later.
A practical cost strategy keeps the platform aligned with operational priorities instead of unnecessary expansion. Teams planning to develop AI denial navigator system for healthcare providers usually see better long-term results when they focus first on denial recovery impact, workflow stability, and phased implementation rather than trying to automate every process at once.
The right architecture decisions reduce unnecessary spending before integrations workflows and automation layers become expensive
Estimate Your Real Investment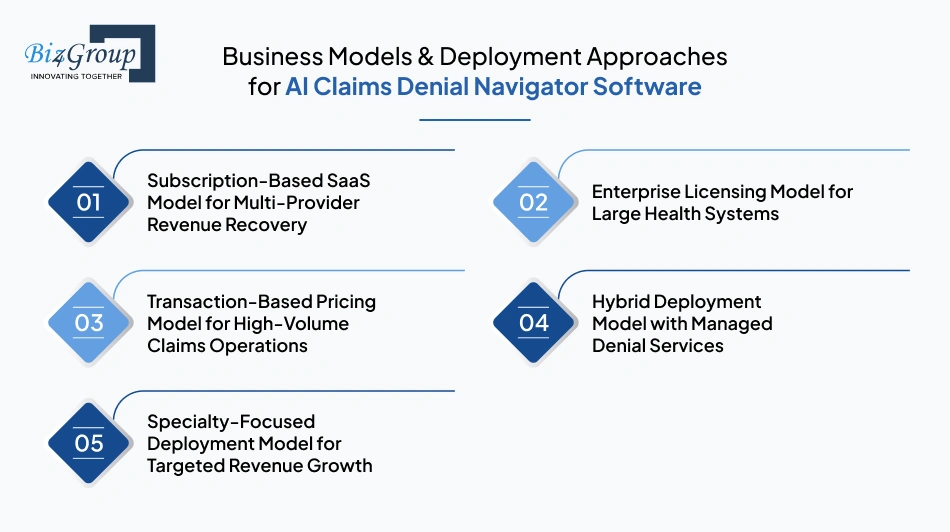
Revenue recovery goals usually shape the deployment model as much as the technology itself. Some provider organizations want tighter control over denial operations inside their own teams. Others want a scalable platform that supports multiple hospitals, physician groups, or RCM clients under one operational structure.
That is where AI claims denial navigator tool development becomes a business decision, not only a technical one.
This model works well for organizations planning to serve multiple hospitals, clinics, or physician groups from one centralized denial platform. Revenue comes through recurring monthly or annual subscriptions based on claim volume, user count, or operational modules.
The biggest financial advantage is predictable recurring income. As more provider groups join the platform, revenue scales without rebuilding the core system each time.
Illustrative Example:
A denial platform charges 12 provider groups $4,500 per month for denial workflow access and analytics support.
Total estimated yearly revenue reaches approximately $720,000 from recurring subscriptions alone.
Some hospital networks prefer complete ownership of the platform inside their internal infrastructure. In this model, the organization pays a large upfront licensing fee along with annual maintenance and support charges.
Revenue generation becomes front-loaded because enterprise deployments usually involve broader integrations, workflow customization, compliance reviews, and operational support.
Illustrative Example:
A regional health system licenses the platform for $280,000 with a yearly support contract worth $45,000.
Total project value crosses $445,000 within the first operational cycle.
This model ties revenue directly to denial activity. Organizations pay based on the number of denials processed, appeals generated, or claims reviewed through the platform.
The structure works well for RCM firms, outsourced billing companies, and high-volume denial operations because revenue grows with transaction volume.
Illustrative Example:
A platform charges $3 per processed denial and handles 45,000 denial cases monthly across multiple clients.
Additional appeal automation services for high-priority claims can further increase operational income.
Some organizations combine software licensing with managed operational support. The platform provider supplies the technology while also helping clients monitor denial queues, optimize payer workflows, or manage escalation processes.
This model creates multiple revenue streams from one deployment relationship.
Illustrative Example:
A provider network pays:
Total monthly revenue becomes $17,000 from one healthcare client. Annual value exceeds $200,000 before additional expansion work.
Some platforms focus only on denial-heavy specialties such as oncology, cardiology, behavioral health, or radiology. These specialties usually deal with complex authorization rules and higher denial rates, which increases operational value for targeted automation.
A focused deployment model often generates stronger pricing power because the workflow logic becomes more specialized.
Illustrative Example:
A radiology-focused denial platform supports 18 imaging centers at $3,800 per month.
Additional prior authorization workflow modules can further increase contract size.
Strong deployment planning directly affects long-term revenue potential. Organizations that build AI claims denial management software around scalable pricing, operational efficiency, and recurring service value usually create stronger financial outcomes than teams focused only on technical delivery.
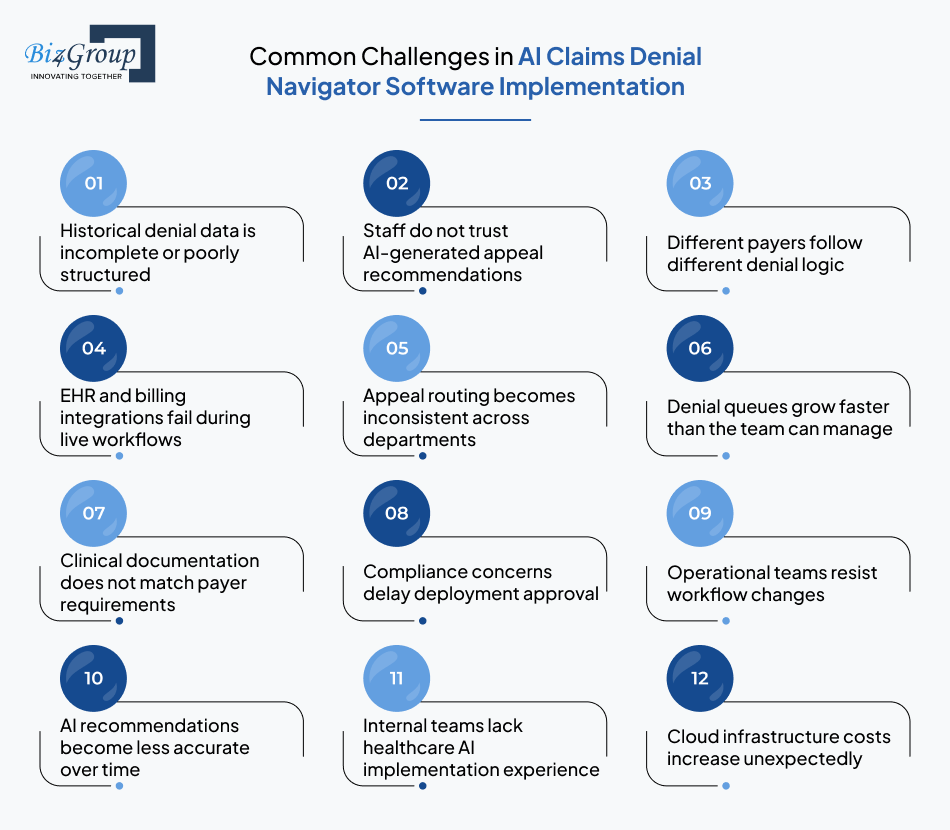
Real implementation problems usually appear after the software enters live denial operations. Teams dealing with AI claims denial navigator software development often struggle with inconsistent data, payer workflow gaps, staff adoption delays, and integration instability during rollout.
Early planning helps, but long-term stability depends on how quickly those operational issues are identified and corrected.
|
Common implementation challenge |
Practical solution |
|---|---|
|
Historical denial data is incomplete or poorly structured |
Clean denial records before model training begins. Standardize payer responses, denial categories, and appeal outcomes so the system learns from usable operational data instead of fragmented records. |
|
Staff do not trust AI-generated appeal recommendations |
Start with advisory workflows instead of fully automated decisions. Let denial teams review recommendations manually during early deployment phases so confidence builds through real usage. |
|
Different payers follow different denial logic |
Maintain separate payer rule structures instead of forcing one workflow across all denials. Teams working with AI TPA software often reduce operational errors by isolating payer-specific appeal paths early. |
|
EHR and billing integrations fail during live workflows |
Test integrations in stages before production rollout. Work with an experienced custom AI software development company that usually separates denial intake testing, claim updates, and document exchange validation to prevent workflow disruption. |
|
Appeal routing becomes inconsistent across departments |
Create standardized escalation rules for denial categories, appeal deadlines, and approval levels. This reduces dependency on individual staff judgment during high-volume denial periods. |
|
Denial queues grow faster than the team can manage |
Introduce prioritization models that rank denials by recoverability, filing urgency, and claim value. That prevents teams from spending equal effort on low-value and high-value denials. |
|
Clinical documentation does not match payer requirements |
Train the platform on real denial examples from each payer group. AI consulting services providers focus heavily on documentation mapping because poor clinical alignment weakens appeal outcomes quickly. |
|
Compliance concerns delay deployment approval |
Involve compliance and security teams during early workflow planning instead of after the platform is completed. That prevents expensive architecture changes later in the project. |
|
Operational teams resist workflow changes |
Roll out the platform in phases using one denial category or department first. Smaller pilots reduce disruption and give teams time to adjust to the new workflow structure. |
|
AI recommendations become less accurate over time |
Retrain AI models regularly using recent denial outcomes, updated payer rules, and current appeal success patterns. Static models lose reliability as payer behavior changes. |
|
Internal teams lack healthcare AI implementation experience |
Insurance provider organizations can hire AI developers with healthcare workflow knowledge as denial operations require both technical execution and revenue cycle understanding. |
|
Cloud infrastructure costs increase unexpectedly |
Monitor claim volume, document storage usage, and processing activity continuously. Teams planning to develop a cloud-based AI claims denial management system should define scaling limits early to avoid unnecessary infrastructure growth. |
Also Read: Cost to Hire an AI Software Developer in 2026
Implementation stability depends on operational discipline as much as technical execution. Teams that test workflows gradually, validate payer logic continuously, and involve denial staff early usually see smoother adoption when they create an AI claims denial software for large-scale healthcare operations.
Denied claims management becomes harder when hospitals try to force generic automation into payer-specific workflows. Instead, they need a system that can automatically capture, categorize, and prioritize denied insurance claims across their entire payer mix without increasing operational pressure on internal teams.
Businesses looking for an experienced development team that can build a custom AI powered claims denial navigator software for their hospital revenue cycle department usually reach this stage after manual denial workflows stop scaling properly. That’s exactly Biz4Group LLC steps in to ease up the process.
Biz4Group LLC is a HIPAA compliant AI healthcare software development company with experience across healthcare, insurance, workflow automation, and enterprise AI systems. Our team focuses on operationally usable software instead of feature-heavy platforms that create additional administrative work.
Here’s what we bring to the table:
Denial management software fails quickly when the development team does not understand healthcare operations. We approach denial navigation from the workflow side first. The focus stays on denial intake, payer response handling, escalation timing, appeal routing, and recovery tracking before technical architecture decisions begin.
Our background in AI insurance automation software solutions also helps address payer-specific operational complexity instead of forcing one workflow across all denial categories. Take a look at our real-world implementations:
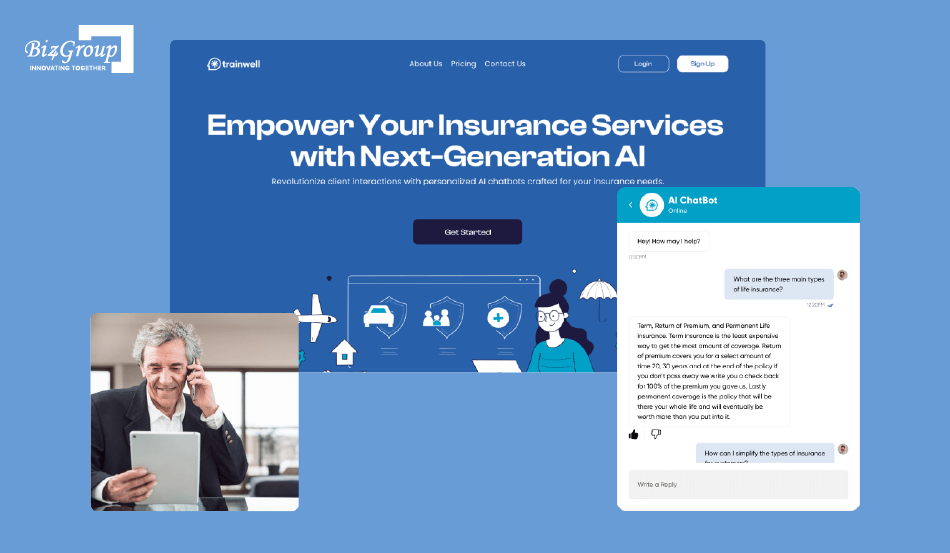
A conversational AI chatbot created for insurance organizations that needed faster internal support, smoother onboarding, and easier access to policy-related knowledge. The system helped agent teams reduce dependency on manual assistance while improving consistency across training and operational guidance.
Key capabilities included:
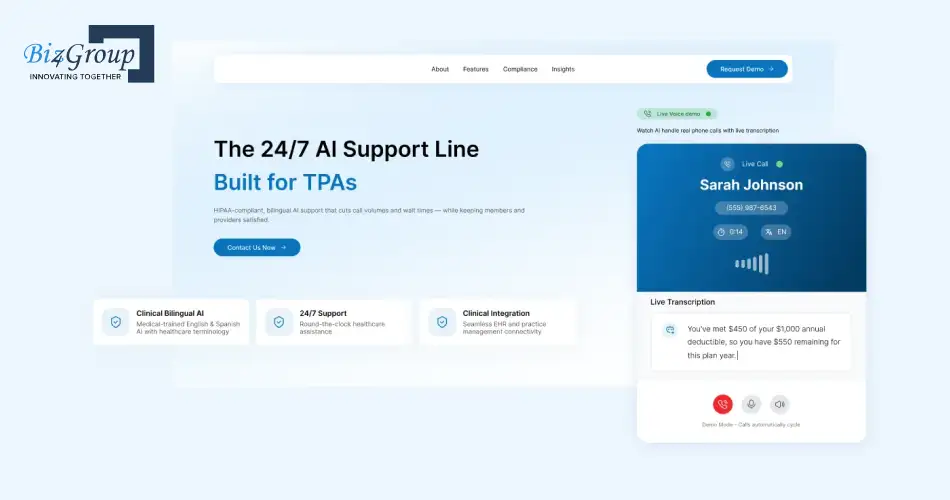
An intelligent voice support platform designed for healthcare TPAs managing frequent patient and insurance communication requests. The solution reduced manual call handling pressure by automating inquiry resolution, improving routing accuracy, and supporting multilingual interactions.
Key capabilities included:
We work on AI-driven operational systems where automation decisions directly affect revenue recovery timelines and staff workload. That becomes especially important for organizations building an AI claims denial navigator with predictive denial forecasting that identifies high risk claims before they are submitted to payers. Predictive logic only works when it stays connected to real operational patterns inside the denial lifecycle.
A technically advanced platform still fails when denial teams avoid using it. We keep the workflow structure practical for appeals teams, RCM managers, and finance operations instead of overloading the system with unnecessary process layers.
The implementation approach focuses on:
That reduces adoption resistance during live deployment.
Claims denial navigation rarely operates as a standalone environment. The software has to exchange information with EHRs, clearinghouses, billing systems, and payer portals continuously.
We approach integrations as operational dependencies rather than isolated technical tasks. That experience becomes valuable in healthcare environments where appeal workflows depend on stable payer communication and synchronized claim updates.
Healthcare organizations need visibility throughout the project lifecycle. Our AI portfolio reflects experience across enterprise automation, healthcare operations, and scalable AI-driven business systems.
We keep the process structured around workflow discovery, phased implementation, testing, compliance validation, and long-term optimization instead of treating deployment as a one-time release cycle.
Reliable denial recovery software depends on operational understanding as much as technical capability. Thus, Biz4Group LLC helps healthcare organizations align payer workflows, AI automation, and revenue cycle operations into one scalable platform through structured AI claims denial navigator software development.
Denied recovery works better when the workflow stays organized, payer-aware, and easier for teams to manage at scale. That is what this entire discussion has been centered around. The goal is not to replace denial teams with automation. The goal is to help them work with better visibility, faster decision-making, and more consistent appeal handling across the revenue cycle.
As denial volume grows, provider organizations need systems that support operational stability without adding more administrative pressure. AI claims denial navigator software development becomes far more valuable when it stays aligned with actual payer workflows, appeal timelines, and recovery priorities already discussed throughout the blog.
Teams investing in AI product development services are now focusing more on long-term operational efficiency instead of disconnected automation tools. Biz4Group LLC helps healthcare organizations move toward that transition with practical AI denial management software development tailored to real denial operations. Contact Us!
The platform separates denials by root cause instead of treating every denial the same way. Clinical denials can move through documentation-based appeal workflows, technical denials can be routed toward coding or billing corrections, and administrative denials can be escalated based on filing urgency or payer requirements. That allows denial teams to recover revenue across multiple denial categories without slowing operations with manual sorting.
Most projects require historical denial records, payer response files, appeal outcomes, ERA data, claim status history, and workflow activity from billing or EHR systems. Teams also use denial aging reports, payer rules, and appeal timelines so the platform can learn how denials move through the organization’s recovery process.
Timeline depends on workflow complexity and integration depth. A focused MVP usually takes around 3–5 weeks. Mid-level platforms with payer intelligence and analytics often require 6–10 weeks. Enterprise-scale systems with predictive denial forecasting, EHR connectivity, and large payer workflows can extend beyond 11-15 weeks.
The overall cost usually ranges from $40,000 to more than $400,000 depending on workflow complexity, AI capabilities, integrations, analytics depth, and compliance requirements.
Smaller systems focused on denial routing and work queues stay closer to MVP pricing, while enterprise healthcare denial management automation platforms require significantly larger investment because of payer logic, interoperability, and operational scale.
Yes. Multi-entity deployment is common in larger healthcare environments. The platform can separate users, payer workflows, denial queues, reporting structures, and permissions for each hospital or provider group while still operating from one centralized infrastructure. This becomes especially useful for health systems, MSOs, and RCM organizations managing denials across multiple facilities.
The platform helps denial teams focus effort where recovery potential is highest. Instead of assigning equal time to every denial, the system estimates overturn probability using historical outcomes, payer behavior, denial type, and documentation quality. That reduces time spent on low-recovery claims and helps teams prioritize denials with stronger financial recovery potential.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.