Imagine a digital system that doesn’t wait for instructions but instead, understands your business goals, learns from real-time feedback, and takes independent actions to get the job done.
Read More

Every patient conversation generates clinical value, but how much of that value gets trapped in documentation delays before it ever reaches the EHR? For many healthcare teams, the real friction begins after the consultation ends. Providers still spend valuable time organizing subjective notes, findings, assessments, and treatment plans into structured SOAP format. That delay impacts chart completion, coding readiness, and provider bandwidth across the day.
This is exactly where AI SOAP notes software development for healthcare is becoming a strategic priority for healthtech entrepreneurs, medical professionals, and healthcare administrators. As clinical workflows grow more digital, teams want documentation systems that can capture conversations, structure them into SOAP-ready notes, and route them into EHR workflows with the right compliance controls.
That demand is also reflected in market momentum, with the U.S. AI medical scribing segment moving from 397.05 million in 2024 toward 2,955.72 million by 2033, growing at 25.09% CAGR from 2025 to 2033 a clear signal that documentation automation is now tied to operational scalability.
For organizations thinking, “we are looking to develop AI SOAP notes software for our clinic, which companies can build this with EHR integration and compliance.”
Well, the answer typically lies in partnering with a custom software development company that understands healthcare workflows, secure EHR connectivity, and clinical compliance requirements from the product design stage itself.
That means the development approach should focus on:
In this guide, we’ll walk through how healthcare SOAP notes software development integrating AI should be planned, built, and scaled for 2026-ready care delivery.
AI SOAP notes software for healthcare is a clinical documentation system that captures patient-provider conversations and converts them into the standard SOAP note structure used across hospitals, clinics, and private practices. The format itself follows four essential parts: Subjective, Objective, Assessment, and Plan.
What makes the software valuable is how it turns this familiar documentation structure into a faster and more workflow-friendly process for healthcare providers and doctors. Instead of manually writing each section after the visit, the system helps structure clinical conversations into review-ready notes, which is why many clinics now look at building AI software with secure EHR workflows supported by reliable AI integration services.
To better understand what changes at the workflow level, here’s how traditional SOAP documentation differs from AI-powered SOAP notes software:
|
Workflow Area |
Traditional SOAP Notes |
AI SOAP Notes Software |
|---|---|---|
|
Note Creation |
Manually typed by provider after consultation |
Automatically generated from conversation and visit context |
|
Time Spent |
High documentation burden after every visit |
Faster draft generation with provider review |
|
Structure Accuracy |
Depends on provider consistency |
Standardized SOAP formatting every time |
|
EHR Readiness |
Requires manual copy or direct typing |
Prepared for structured EHR insertion |
|
Provider Effort |
High mental load and repetitive entry |
Lower effort with guided note review |
|
Scalability for Hospitals |
Documentation style varies across providers and departments |
Standardized note templates and automated structuring support consistent documentation across teams |
The practical takeaway is that AI SOAP notes software development for healthcare is not just about faster note writing. It is about converting the existing SOAP method into a scalable digital workflow that supports providers without disrupting how they already document care.
In the next section, we’ll break down how this workflow is architected with EHR systems and real clinical data movement.
Map the right EHR sync and note logic before scaling provider adoption
Plan Your Architecture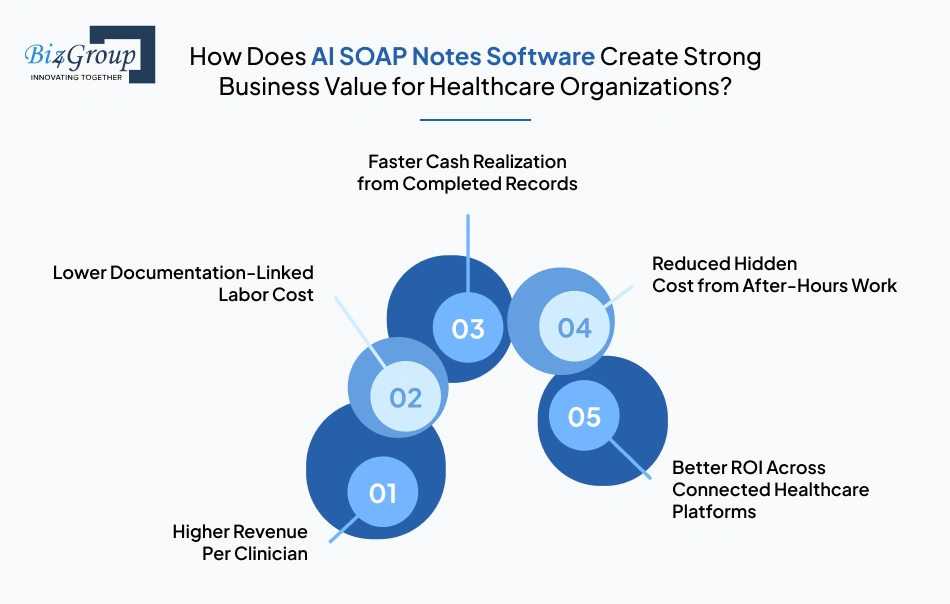
What really happens behind the screen when a doctor finishes speaking, and a structured SOAP note appears inside the patient's record? For hospitals and healthcare startups, that workflow depends on an architecture that keeps note creation fast, clinically aligned, and ready for EHR movement without interrupting provider routines.
The architecture starts by capturing the consultation through voice, typed notes, or connected visit transcripts. In most hospital workflows, this layer also maps the note to the right patient, encounter, and provider context, so the documentation starts with visit-specific accuracy.
This creates the foundation for reliable downstream note generation.
The captured conversation then moves through a healthcare speech recognition system that converts clinical speech into clean text. It removes filler phrases, separates speakers, and organizes fragmented discussion into medically usable note content.
This layer directly impacts how usable the final SOAP draft feels to doctors.
Also Read: AI Text to Speech App Development
Before structuring the note, the software pulls relevant patient details such as history, current medications, prior diagnoses, allergies, and recent lab data from AI EHR/EMR software workflows. This helps the system align the current visit discussion with the broader clinical picture.
This layer keeps documentation grounded in a real patient context.
Also Read: How Much Does It Cost to Develop an AI EHR Software?
This is the core intelligence layer where the system maps conversation data into subjective, objective, assessment, and plan sections. It also applies specialty-specific templates, note preferences, and care-path logic, which is critical when teams want to create AI SOAP notes software for doctors that fits real specialties.
This layer turns raw visit data into clinically meaningful documentation.
The structured note then moves into a provider-facing review screen where doctors can refine wording, verify diagnoses, and finalize the treatment plan. This keeps the workflow aligned with real clinical ownership.
This is the trust layer of the entire system.
After approval, the final note flows through middleware that helps integrate healthcare platform with AI EHR’s, linking the SOAP output with encounter records, patient charts, orders, and follow-up workflows.
This is what makes the architecture operationally useful inside hospitals.
Also Read: Your Guide on AI EHR App Development for Hospitals and Clinics
Every note edit, access event, and sync action is logged with timestamps, user roles, and version history. This layer supports compliance readiness, secure access, and audit traceability across departments.
This protects documentation integrity at scale.
The final layer tracks provider correction patterns, specialty usage, delayed note trends, and template performance. These insights help hospitals build AI SOAP notes system for hospitals that improve documentation quality over time.
The real strength of this architecture is that every layer supports both provider usability and hospital-grade governance. That is what allows AI SOAP workflows to scale from single clinics to multi-location health systems without breaking clinical routines.
When healthcare organizations invest in documentation intelligence, the real business question is not how notes get written. It is how fast that investment improves revenue, reduces cost pressure, and creates measurable ROI across provider groups.
For hospitals and clinics, the strongest value of AI SOAP notes software development for healthcare comes from better financial output per clinician, lower documentation-linked labor spend, and faster revenue realization from completed records.
When documentation delays shrink, each provider’s billable output improves within the same compensation structure. In real deployments, even a 12% increase in clinician productivity can materially improve annual revenue per physician without increasing salary cost.
That financial lift is usually reflected through:
The clearest financial gain comes from reducing paid and hidden labor spent on documentation. When organizations save 15,000 clinician hours in 1 year, the value directly converts into lower overtime exposure and better salary efficiency.
The cost savings typically appear through:
This is where documentation intelligence starts behaving like practical AI automation for healthcare investment.
Revenue delays often begin when notes remain incomplete. A 66% reduction in delayed note closures within 50 days improves how quickly completed documentation turns into financially usable records.
That monetary value grows through:
This strengthens financial control for provider organizations.
After-hours documentation creates real financial leakage through overtime, retention strain, and physician replacement costs. A 41% sustained reduction in after-hours documentation work helps organizations reduce these hidden expenses over time.
The savings become visible through:
This becomes highly valuable in developing AI SOAP notes software for clinics with secure data handling, where cost discipline directly affects profitability.
The long-term financial upside increases when SOAP documentation connects with systems such as healthcare CRM, an AI driven patient journey automation system, and AI healthcare analytic software that support payer follow-ups and revenue intelligence.
That enterprise ROI expands through:
Also Read: Artificial Intelligence in CRM
The business takeaway is clear: AI SOAP note platforms create value when they improve provider revenue output, lower documentation labor cost, reduce hidden burnout expenses, and shorten the path to realized cash flow. That is the kind of ROI healthcare organizations can justify at scale.
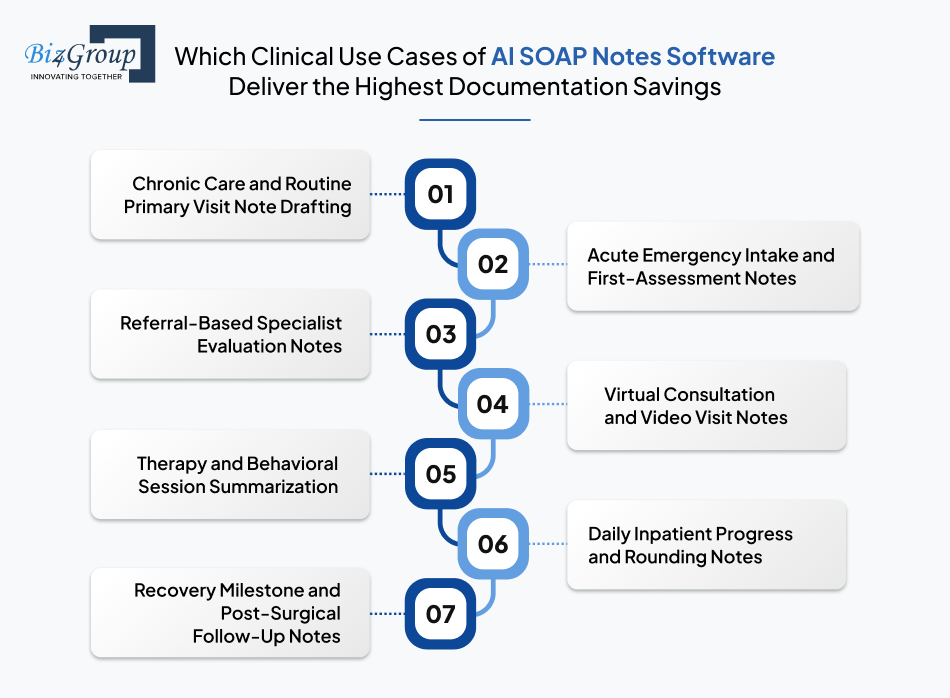
Patient documentation pressure does not look the same across every care setting, which is why the highest-value use cases come from workflows where providers repeat the same note structure across high patient volumes.
When the question becomes, I want to build AI SOAP notes software that supports real-time documentation and integrates with EHR systems. What should I consider?
The right starting point is defining the exact clinical note scenarios where the software will be used every day. Take a look:
Also Read: How to Develop an AI Telehealth Automation System in 2026
The real strength of these use cases lies in how each one maps to a different clinical documentation moment across care delivery. That is why AI SOAP notes software development for healthcare should always begin with clear use-case definition before moving into feature planning.
Identify the use cases where documentation time drops fastest across specialties
Find Your Best Use CasesWhen evaluating SOAP notes software development for healthcare using AI, let us first look at how the leading platforms already solve real clinical documentation problems.
The tools below stand out because their workflows, EHR connectivity, and note-generation methods reflect what healthcare teams usually expect before they decide to develop AI SOAP notes software for healthcare with their own product vision.
Suki is an ambient clinical intelligence platform built for healthcare documentation, coding, and reasoning workflows. It captures the full patient conversation, turns it into structured clinical notes, and syncs directly with major EHRs including Epic, Oracle Health, athenahealth, and MEDITECH. Its strength lies in deep enterprise-grade interoperability and broad specialty coverage.
How It Works: It listens during the patient visit, converts the conversation into high-quality notes, allows voice-enabled edits, and sends finalized documentation directly into the EHR in real time. It also supports patient instructions and order generation.
Best For: Large health systems, multi-specialty provider groups, and hospitals that need deeply integrated ambient documentation workflows.
Freed is an AI scribe and clinician assistant focused on fast, accurate note creation with simple usability. It is widely used by individual clinicians and smaller practices that want documentation help without heavy enterprise setup. Its one-click EHR transfer makes it easy for providers to fit into existing workflows.
How It Works: The platform turns patient conversations into clear notes, prepares visit-ready documentation, and lets providers transfer finalized notes into their existing EHR with a single click.
Best For: Solo practitioners, outpatient clinics, therapists, and independent medical groups.
Heidi Health positions itself as an AI care partner for modern clinical practice, focusing on documentation support that feels lightweight and provider friendly. Its value comes from helping clinicians generate notes quickly while keeping the interaction natural and easy to review.
How It Works: It captures the clinical interaction, drafts structured notes, and supports doctor-led review before the final note is moved into the record workflow.
Best For: Growing clinics, telehealth providers, and modern digital-first care practices.
Abridge is a generative AI platform built specifically for clinical conversations. It transforms patient-clinician interactions into context-aware, clinically useful, and billable notes in real time. The platform is strongly positioned for enterprise healthcare systems that prioritize large-scale deployment.
How It Works: It listens to live clinical conversations, applies context-aware note generation, and prepares sign-off-ready documentation that can support downstream clinical and revenue workflows.
Best For: Enterprise hospitals, Epic-heavy environments, and health systems with large physician networks.
Also Read: Top Generative AI Development Companies in USA
DeepScribe focuses on specialty-specific AI medical scribe workflows. Its platform is built to transform patient conversations into fully customizable chart notes while learning provider style and specialty preferences over time. That makes it especially strong for personalized SOAP documentation.
How It Works: The provider starts the visit in the app, selects the patient from a synced schedule, and the software converts the visit into customizable specialty notes that can be refined before chart completion.
Best For: Specialty clinics, surgical groups, and providers who need deeply customizable documentation behavior.
The biggest takeaway from these tools is not just feature variety, but how each one approaches note generation, provider review, and EHR movement differently. Those product patterns become highly useful reference points when planning AI SOAP notes software development for healthcare with a differentiated workflow strategy.
A hospital-ready AI SOAP notes platform is defined by the features that directly support how doctors capture, review, finalize, and securely store clinical notes. When the focus shifts toward building an AI SOAP notes software for healthcare industry, the most practical approach is to prioritize features that improve note accuracy, preserve provider control, and protect PHI at every documentation stage.
|
Core Feature |
Purpose |
|---|---|
|
Real-Time Clinical Conversation Capture |
Captures doctor-patient conversations live during the visit and prepares the note foundation as the interaction happens, reducing the need for post-visit reconstruction. |
|
Multi-Speaker Separation Engine |
Distinguishes provider speech from patient responses so symptoms, clinical observations, and care decisions are assigned to the correct SOAP sections. |
|
Clinical Speech-to-Text and NLP Layer |
Uses AI speech recognition to convert medical conversations into structured draft text with context-aware section mapping, making it practical to create AI SOAP notes software with speech to text and NLP for real clinical use. |
|
Automatic SOAP Note Drafting |
Converts the captured visit context into subjective, objective, assessment, and plan sections in real time, so doctors review a full draft instead of starting with a blank note. |
|
Specialty-Specific Note Templates |
Applies specialty-aware documentation structures for cardiology, behavioral health, orthopedics, and other departments, so the SOAP draft matches the provider’s real note style. |
|
Provider Review, Voice Edit, and Approval |
Lets doctors refine diagnoses, update treatment plans, use voice commands for quick edits, and approve the final note before chart sync. |
|
Patient and Encounter Linking |
Connects every generated note to the correct patient, provider, visit date, and encounter type, so documentation remains traceable and EHR-ready. |
|
Provider Correction Learning Loop |
Learns from repeated provider edits and preferred wording patterns to improve future note drafts and support smarter documentation predictive analysis. |
|
Clinical Tone and Risk Signal Detection |
Uses sentiment analysis to detect distress cues, behavioral concerns, or escalation patterns inside conversations that may influence assessment and care planning. |
|
Audit Trail and HIPAA Access Governance |
Records every edit, approval, export, and access event with timestamps, role control, and version history, so note workflows stay legally traceable and HIPAA-safe. |
|
Encrypted EHR Sync and Secure PHI Storage |
Sends finalized SOAP notes into patient records through protected channels while securing transcripts, voice data, and note history during storage and transfer. |
The most effective feature sets are the ones that directly reflect how clinical notes are actually created inside hospitals and clinics. That is why AI SOAP notes software development for healthcare should begin with realistic note-generation features before moving into workflow design and compliance engineering.
Also Read: AI Predictive Diagnosis and Disease Forecasting Software Development
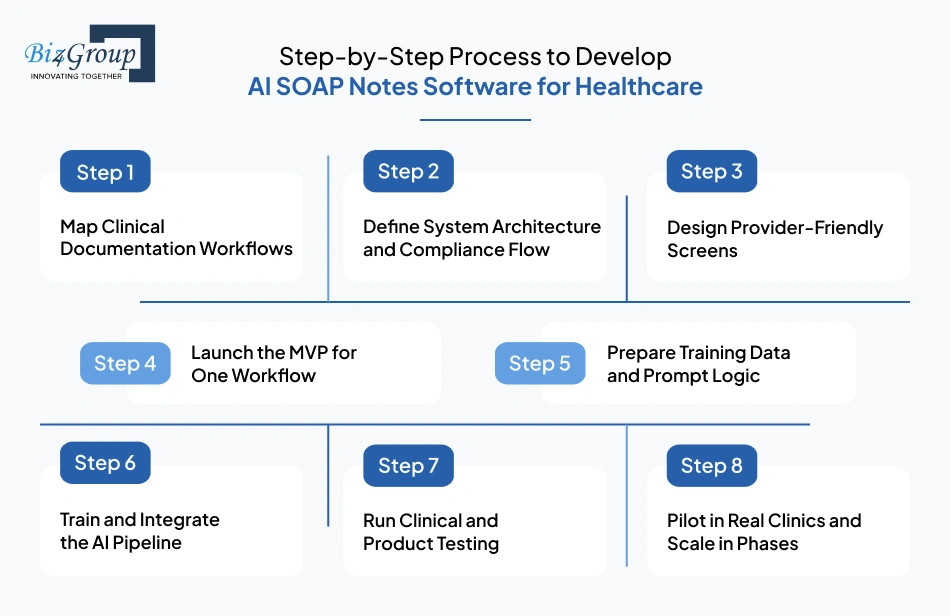
A strong product does not begin with code. It begins with clarity around how doctors document, where note friction happens, and what the first usable version must solve.
When the question becomes, how to develop AI SOAP notes software for healthcare step by step, the most practical path is a staged process that moves from workflow planning to MVP validation, model integration, and clinical-grade testing.
Start by identifying the exact care settings where the product will be used, such as outpatient visits, hospital rounds, telehealth, or specialty consultations. For teams creating AI SOAP notes solution for clinics, this step defines the first documentation journey the product should support.
Then document:
Once workflows are clear, design the full product architecture for live capture, SOAP drafting, review layers, HIPAA controls, storage, and secure API connections. This stage should also define how access control, audit history, and PHI movement will work from day one.
Then define:
Also Read: Adopt An API-First Architecture for Business Agility
The interface should feel natural for doctors who need to review notes quickly during busy schedules. Working with a reliable UI/UX design company helps shape a usable experience around transcript view, SOAP editing, voice correction, and encounter-based note approval.
Then design:
Also Read: Top UI/UX Design Companies in USA
The first release should focus on one realistic documentation scenario instead of multiple specialties. With the help of focused MVP development services, the MVP can validate whether the capture-to-note flow actually works in clinical environments.
Then include:
Also Read: Top MVP Development Companies in USA
Once the MVP workflow is stable, prepare de-identified SOAP note samples, correction examples, and specialty prompts. This is the stage where teams select AI model for your use case and define how the system should interpret symptoms, findings, assessments, and plans.
Then prepare:
Now the model layer moves into production readiness. Use this phase to train AI models on validated note structures, then integrate AI model workflows into the MVP, so real patient conversations convert into review-ready SOAP drafts.
Then connect:
Before wider rollout, validate the software in controlled care environments. Partnering with experienced software testing companies helps confirm note accuracy, approval reliability, HIPAA-safe access, and stable EHR sync under real usage.
Then test:
Also Read: Top AI Software Development Companies in USA
The final stage is a controlled pilot with real providers, followed by phased expansion across departments or partner hospitals. Use feedback from early users to improve templates, note quality, and specialty coverage before larger deployment.
Then scale through:
The strongest products follow a phased process where workflow mapping, MVP validation, AI training, and clinical testing happen in the right sequence. That is what makes AI SOAP notes software development for healthcare realistic enough for long-term hospital deployment.
Validate the right MVP path before your development timeline expands
Start Your Product RoadmapOnce the product workflow and architecture are defined, the next decision is the technology stack that keeps note generation, EHR movement, and hospital-grade reliability stable as usage grows.
When the focus turns to creating an AI SOAP notes solution for healthcare with cloud integration, the right full stack development choices decide how smoothly documentation workflows scale across clinics, departments, and hospital systems.
The most practical way to evaluate the stack is by separating it into the same technology layers the product will rely on in real deployment.
|
Category |
Frameworks and Tools |
Why It Matters |
|---|---|---|
|
Speech-to-Text |
Whisper, Google Speech-to-Text, AWS Transcribe Medical |
Converts provider-patient conversations into accurate clinical transcripts |
|
NLP and SOAP Structuring |
spaCy, Hugging Face Transformers, ClinicalBERT |
Maps conversations into Subjective, Objective, Assessment, and Plan sections |
|
LLM Orchestration |
LangChain, LlamaIndex |
Manages prompt workflows, provider correction memory, and note-generation pipelines |
|
Clinical Reasoning Models |
OpenAI API, Azure OpenAI, Med-PaLM style clinical LLMs |
Supports context-aware SOAP draft generation and provider-ready summaries |
|
Category |
Frameworks and Tools |
Why It Matters |
|---|---|---|
|
Frontend |
Provider dashboards, transcript review screens, and note editing workflows through secure web development layers |
|
|
Backend |
Handles note generation logic, encounter workflows, provider review, and EHR orchestration |
|
|
APIs |
REST, GraphQL, FHIR APIs |
Moves finalized SOAP notes, encounter data, and patient context securely across hospital systems |
|
Category |
Frameworks and Tools |
Why It Matters |
|---|---|---|
|
Databases |
PostgreSQL, MongoDB |
Stores patient encounter metadata, note drafts, and provider correction history |
|
Cache Layer |
Redis |
Supports faster transcript retrieval and low latency note review screens |
|
Cloud |
AWS HealthLake, GCP Healthcare API |
Secure cloud infrastructure for PHI-safe storage, model execution, and hospital integrations |
|
Category |
Frameworks and Tools |
Why It Matters |
|---|---|---|
|
Containerization |
Docker |
Keeps environments consistent across development, staging, and hospital deployment |
|
Orchestration |
Kubernetes |
Scales documentation workloads across departments and multi-site health systems |
|
Monitoring |
Prometheus, Grafana |
Tracks note-generation latency, sync failures, and provider workflow health |
|
Category |
Frameworks and Tools |
Why It Matters |
|---|---|---|
|
Voice Workflow Layer |
WebRTC, Twilio Voice, Agora |
Supports real-time visit audio capture for live SOAP drafting |
|
Model Feedback Loop |
MLflow, Weights & Biases |
Tracks provider corrections and improves future note quality |
|
Security and PHI Controls |
Vault, AWS KMS, Azure Key Vault |
Secures PHI encryption keys, token access, and compliance-ready credential management |
A strong stack keeps hospital documentation workflows reliable under real provider demand, while also making model updates and EHR integrations easier to manage. That is why AI SOAP notes software development for healthcare depends as much on stack alignment as it does on architecture and workflow design.
Also Read: Why to Choose the Full Stack Development for Modern Business
Clinical documentation software succeeds only when providers trust that every note, transcript, and patient conversation is protected from capture to storage.
For healthcare providers asking, “we want to implement AI in our documentation workflows using SOAP notes software, what requirements should be taken into considerations for such solutions.”
The right focus shifts to compliance controls, security safeguards, and healthcare regulations that directly govern patient documentation.
Also Read: HIPAA Compliant AI App Development for Healthcare Providers
The strongest compliance strategy treats note capture, model validation, EHR sync, and long-term storage as one continuous governance flow. That is why AI SOAP notes software development for healthcare must align security engineering and regulatory controls from the earliest product stages.
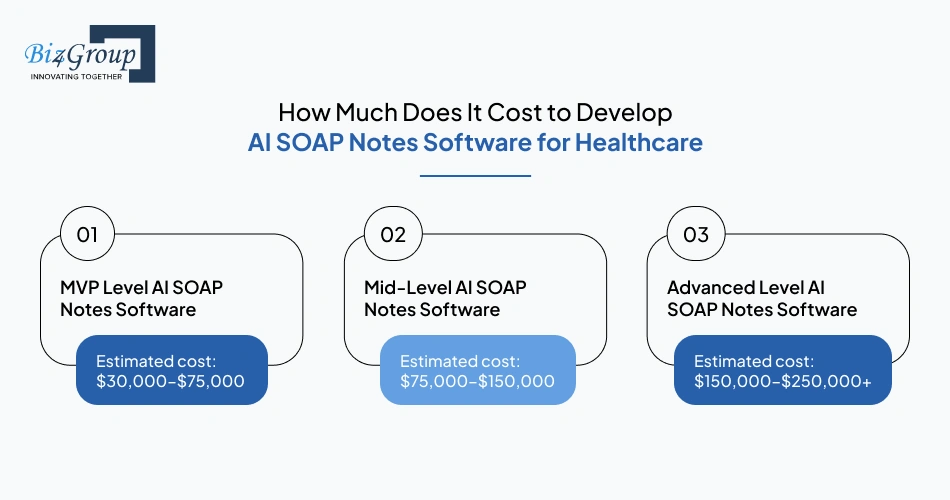
Cost planning becomes clearer when the software scope is tied to real documentation workflows, EHR connectivity, compliance controls, and AI note-generation depth. For teams focused on developing AI SOAP notes tools for healthcare, the most realistic budget range sits between $30,000–$250,000+, depending on whether the product starts as an MVP, expands into multi-specialty workflows, or scales into hospital-grade deployment.
|
Development Level |
Estimated Cost Range |
Scope |
|---|---|---|
|
MVP Level AI SOAP Notes Software |
$30,000–$75,000 |
Core speech capture, SOAP drafting, provider review, basic EHR sync, HIPAA-ready access controls |
|
Mid-Level AI SOAP Notes Software |
$75,000–$150,000 |
Multi-specialty templates, role-based workflows, advanced note editing, stronger interoperability and analytics |
|
Advanced Level AI SOAP Notes Software |
$150,000–$250,000+ |
Multi-location deployment, real-time voice workflows, provider correction learning, advanced security, compliance automation, and enterprise interoperability |
A large part of the budget depends on how intelligently the platform converts doctor-patient conversations into SOAP-ready notes. Cost of AI integration increases as software needs specialty-specific prompts, provider correction learning, and stronger clinical reasoning for assessment and plan sections.
Cost Impact: $8,000–$40,000
The cost changes based on how the product captures consultations. A transcript-upload workflow costs less, while live speech capture with speaker separation, medical terminology recognition, and secure audio handling increases the effort and infrastructure requirement.
Cost Impact: $5,000–$25,000
This usually becomes one of the biggest cost drivers because the software must move finalized notes into the right patient chart, encounter, and provider workflow. The more hospital systems, FHIR endpoints, and validation rules involved, the higher the implementation effort.
Cost Impact: $10,000–$45,000
Security requirements directly affect cost because the platform must support encryption, access control, audit trails, and HIPAA-ready cloud environments. For healthcare products, these safeguards are not optional and must be planned even during MVP software development
Cost Impact: $7,000–$30,000
The interface layer also impacts budget. Costs increase when the product includes live transcript views, SOAP section editing, voice-based corrections, provider approvals, and specialty-specific review workflows.
Cost Impact: $5,000–$20,000
|
Hidden Costs |
Estimated Cost Impact |
|---|---|
|
Clinical note data labeling and cleanup |
$3,000–$15,000 |
|
Post-launch specialty template expansion |
$5,000–$20,000 |
|
EHR vendor certification and testing |
$8,000–$25,000 |
|
Cloud PHI storage growth |
$2,000–$10,000 annually |
|
Compliance audits and legal reviews |
$4,000–$18,000 |
The most realistic budgets come from aligning scope, AI depth, interoperability, and compliance from day one. That is why AI SOAP notes software development for healthcare should always be budgeted as a phased product journey instead of a single fixed estimate.
Also Read: Cost to Develop HIPAA-Compliant AI Healthcare Software
Avoid hidden costs by aligning scope, AI depth, and rollout phases upfront
Talk to Our AI Experts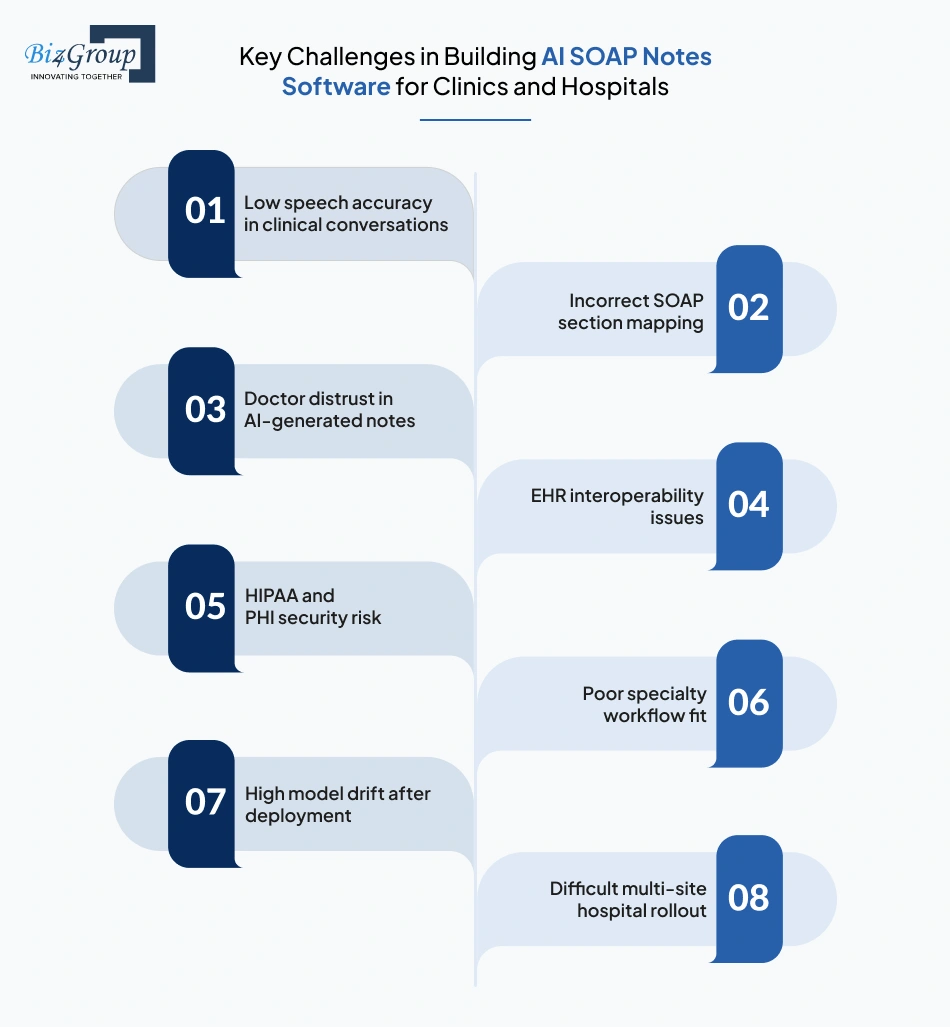
The biggest risks usually appear where clinical workflows, provider trust, and hospital interoperability meet real-world software complexity. During the development of AI SOAP notes software, product teams need to identify the challenges early so the right engineering, validation, and rollout decisions can be made before scale introduces expensive rework.
|
Key Challenges |
How to Solve It |
|---|---|
|
Low speech accuracy in clinical conversations |
Use medical speech models, specialty vocabulary libraries, and provider accent tuning during training so the transcription layer performs reliably in real care environments. |
|
Incorrect SOAP section mapping |
Validate note structuring against real provider-approved SOAP samples and add specialty-specific prompt rules before production rollout. |
|
Doctor distrust in AI-generated notes |
Keep provider review mandatory, support fast inline edits, and use feedback loops that learn from repeated correction behavior. |
|
EHR interoperability issues |
Use FHIR-ready middleware, patient encounter validation, and staged integration testing with hospital sandbox environments before live sync. |
|
HIPAA and PHI security risk |
Implement encrypted storage, role-based access, vendor BAAs, and audit traceability from the first product release with guidance from experienced AI consulting service teams. |
|
Poor specialty workflow fit |
Build configurable note templates and specialty logic with support from domain-aware healthcare AI developers who understand real documentation patterns. |
|
High model drift after deployment |
Continuously retrain prompts and note-generation logic using approved provider corrections and production note feedback. |
|
Difficult multi-site hospital rollout |
Use phased deployment by department, reusable workflow modules, and centralized governance supported by a reliable AI development company delivery model. |
The most successful teams treat these challenges as product-planning inputs instead of post-launch surprises. That is why AI SOAP notes software development for healthcare becomes far more scalable when risk mitigation is built into architecture, validation, and rollout from the beginning.
When healthcare teams start asking, we are evaluating vendors to develop AI SOAP notes software, which company provides scalable and customizable solutions; the real concern usually goes beyond note generation. They want to know whether the partner understands provider workflows, HIPAA boundaries, EHR interoperability, specialty documentation logic, and how hospitals adopt new tools without slowing clinicians down.
That is exactly where Biz4Group LLC stands out. We bring practical execution depth in turning live clinical conversations into provider-trusted chart workflows while keeping the product scalable for clinics, hospitals, and multi-specialty health systems.
As an experienced AI healthcare software development company, we work closely with healthcare founders, product managers, and innovation teams to turn documentation workflows into production-ready software. Our approach stays grounded in real clinical usage, secure data movement, specialty-specific note logic, and phased rollout strategies that reduce adoption friction.
We help healthcare teams:
These are not just vague claims, here’s the proof of how we combine healthcare workflow clarity with practical delivery experience across real medical platforms.
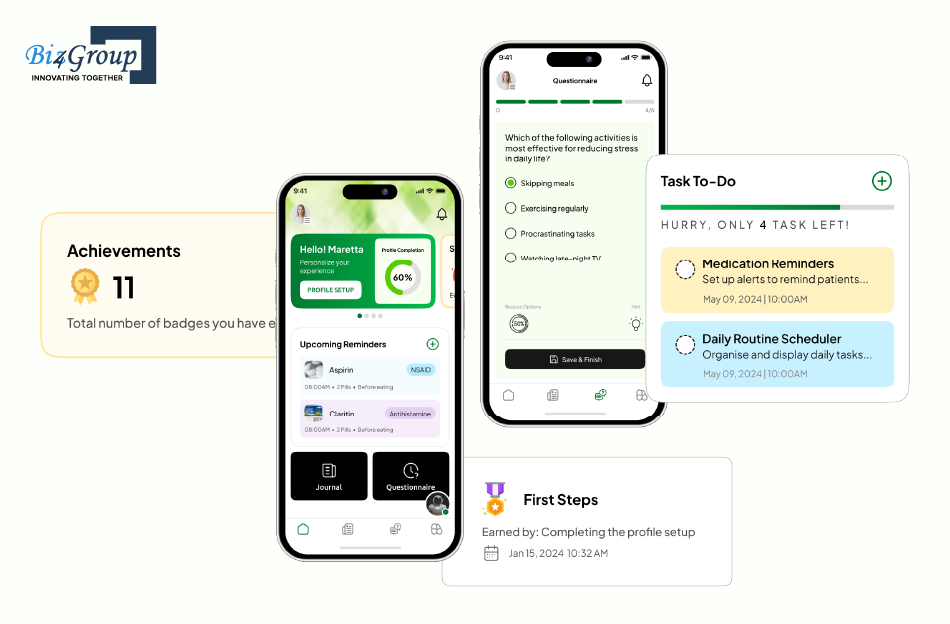
CogniHelp is an AI mobile application designed to support early- to mid-stage dementia patients with daily memory reinforcement and routine stability. The platform helps patients stay oriented by storing personal details such as family names, schedules, and important life references. It also supports journaling and guided cognitive exercises that encourage routine thought processes and help reduce confusion in everyday life.
Key Highlights:
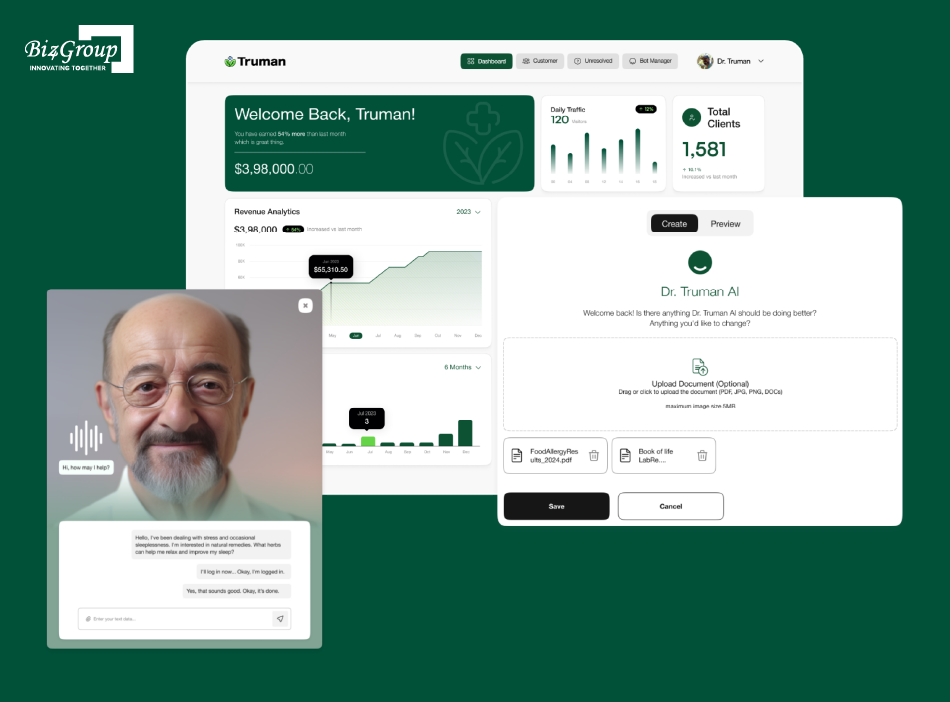
Truman is an AI-enabled avatar for personalized health advice. It delivers personalized health consultations, supplement recommendations, membership-based wellness benefits, and health history tracking in one connected experience. Users can interact with the avatar for health guidance, upload reports, and continue their wellness journey through a seamless in-app consultation-to-purchase flow.
Key Highlights:
Select Balance is an AI-powered chatbot for personalized supplement recommendations that helps users discover the right health products through guided quizzes and conversational symptom analysis. The platform uses real-time product matching and presents product cards with direct buy links. It also includes an admin-side training panel that allows live updates for keywords, product logic, and recommendation flows.
Key Highlights:
Dr. Ara is an AI-powered athletic health solution created for athletes and performance-focused users who want deeper health insights from blood reports and recovery data. The platform analyzes uploaded health reports and transforms them into personalized guidance around diet, hydration, sleep, recovery, and fitness improvement. It also supports direct consultation booking, making it a centralized performance health companion for athletic users.
Key Highlights:
These healthcare implementations reflect how Biz4Group LLC turns complex patient journeys, AI-driven recommendations, and sensitive medical data workflows into practical digital products that are easy to adopt and ready to scale.
That same execution clarity is exactly what we bring to AI SOAP notes software development, helping clinics and hospitals move from documentation pain points to secure, provider-trusted workflows with scalable AI product delivery.
Let’s discuss how we can help you shape a secure, provider-friendly, and hospital-ready AI SOAP notes platform.
The next generation of documentation platforms will not just assist with note creation. They will increasingly shape how providers prepare for visits, carry forward patient context, and manage follow-up actions across the care journey. As AI SOAP notes software development for healthcare moves beyond 2026, the product roadmap will be defined by how intelligently these systems will support continuity, anticipation, and autonomous clinical workflows.
These future shifts will most likely reshape documentation platforms in the following ways:
Together, these shifts will move documentation systems closer to intelligent clinical workflow partners rather than isolated note-generation tools. That is how the future of AI SOAP platforms will likely shape hospital documentation strategy, provider adoption, and long-term digital care continuity beyond 2026.
Shape a roadmap built for autonomous workflows and evolving provider expectations
Future-Proof Your AI PlatformThe real opportunity in healthcare documentation will come from how naturally the software fits into provider workflows while still staying scalable for hospitals, specialties, and evolving compliance needs. That is where thoughtful AI product development services make the biggest difference, helping turn documentation complexity into products that clinicians can trust, and teams can confidently scale.
When healthcare leaders reach the point of asking, I need a development partner to create AI healthcare documentation software with NLP and automation, which company should I shortlist, the decision usually comes down to who can combine workflow clarity with long-term product execution. That is where Biz4Group brings practical healthcare delivery experience, scalable AI engineering, and real product thinking that extends beyond feature development.
If you’re ready to turn your documentation vision into a provider-friendly AI platform, let’s connect and shape the right roadmap together for AI SOAP notes software development for healthcare.
Accuracy usually depends on how well the system is trained for specialty workflows such as behavioral health, cardiology, surgery, or primary care. A strong product will use specialty templates, provider correction learning, and EHR-linked patient context so the note reflects real clinical reasoning instead of generic text generation.
In hospital settings, the software should support role-based review workflows where physicians, nurses, specialists, and compliance teams can contribute to the same documentation journey. The most effective platforms maintain version history, provider attribution, and encounter-linked updates, so the final SOAP note stays clinically consistent across teams.
The most realistic overall range usually falls between $30,000 and $250,000+, depending on whether the goal is an MVP, a mid-level clinic platform, or a hospital-grade multi-specialty product. The final budget changes are based on EHR integration depth, speech-to-text accuracy requirements, compliance layers, and specialty-specific note workflows.
A focused MVP with one documentation workflow usually takes 4 to 6 weeks. A full-scale hospital-ready platform with specialty templates, cloud deployment, compliance controls, and EHR interoperability typically takes 12 to 14 weeks. The exact timeline depends on how much customization is required around provider workflows and hospital systems.
Future-ready platforms are increasingly being designed to support multilingual speech capture, translated SOAP drafting, and region-specific medical terminology. This becomes especially important for hospitals, telehealth providers, and clinics serving diverse patient populations across multiple geographies.
The most practical path starts with one clinical workflow, a secure cloud environment, and standards-based FHIR connectivity. From there, the product should expand through phased specialty templates, provider feedback learning, and scalable infrastructure, so the platform remains stable as hospital usage grows.
with Biz4Group today!
Our website require some cookies to function properly. Read our privacy policy to know more.